Similar to hearing aids, the market penetration of cochlear implants is surprisingly low. Many patients who fall within the current candidacy range are never referred for evaluation for a cochlear implant. And that can present problems for both the patient and for the dispensing professional. This article provides an update on the current expanded criteria for cochlear implant candidacy.

|

|
| Steve Huart, AuD, is senior marketing manager at Cochlear Americas, Centennial, Colo, and Carol A. Sammeth, PhD, is senior regulatory/clinical specialist at Cochlear Americas and is an adjunct associate professor of audiology at the University of Colorado-Boulder. | |
Hearing aids help the vast majority of hearing-impaired patients seen in audiology clinics and dispensing offices/practices. But, as the degree of sensorineural hearing loss reaches the severe-to-profound range, benefits from amplification become limited. Amplifier gain cannot be increased for greater audibility without producing feedback, and no amount of tweaking of the signal processing will result in higher speech scores because some patients simply have too much hair cell loss to stimulate acoustically. An alternative is stimulation of the nerve fibers electrically via a cochlear implant.
Unfortunately, many patients who fall within the current candidacy range are never referred for evaluation for a cochlear implant. Apparently, this is partly because some dispensing professionals believe that few, if any, patients in their own practices would actually be better candidates for cochlear implants than for high-power amplifiers or perhaps for high-to-low frequency transposition hearing aids.
This article is intended to change that perception by providing up-to-date information on the current expanded criteria for cochlear implant candidacy and performance achieved by implant recipients today.

|
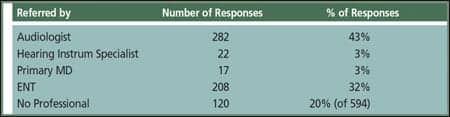
| TABLE 1. Cochlear implant recipients answering the question, “Who initially recommended that you consider a cochlear implant evaluation?” Source: Cochlear Americas Hearing Aids and Cochlear Implants Recipient Survey, December 2008; n=594. Note: The total number of responses in the table is >594 because some individuals chose more than one professional. |
The CI Under-Referral Problem
In a December 2008 survey done by Cochlear Americas, 594 cochlear implant recipients were asked what health care professional referred them for their initial evaluation (Table 1). Sadly, less than half (46%) reported being referred by audiologists or hearing aid dispensers, and 20% reported they were not referred by any professional. These latter individuals had to find out about cochlear implants from friends, family, the Internet, or other sources.
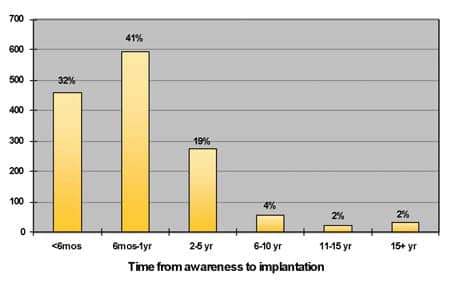
Even when patients are appropriately referred for implant evaluation, it is often only after many years of struggle with their hearing loss. In a large multicenter clinical study conducted in 2007,1 it was reported that the average time from onset of severe-to-profound hearing loss until receiving a cochlear implant was 12 years. However, once people become aware that they are a cochlear implant candidate, there is often little hesitation to proceed. In an April 2008 Cochlear Americas survey of 1,500 cochlear implant recipients, most reported that they were implanted in less than 1 year after they became aware that they were candidates (Figure 1).
|
| FIGURE 1. Time between becoming aware of being a cochlear implant candidate and actually getting implanted. Source: Cochlear Americas Recipient Survey, April 2008; n=1501. |
In another 2008 survey done at the American Academy of Audiology conference in Charlotte, NC, Cochlear Americas asked more than 400 hearing care professionals questions regarding identification and referral of patients for cochlear implant evaluation. Of these, 20% indicated that they believed they had not seen any cochlear implant candidates in the last 6 months, and 55% believed they had seen less than five candidates. Further, when asked how many patients they had referred for an implant evaluation in the past 6 months, 41% answered none, and 50% said less than five. Thus, most believed they saw few or no implant candidates on a regular basis, and they did not always refer even when they saw a candidate.
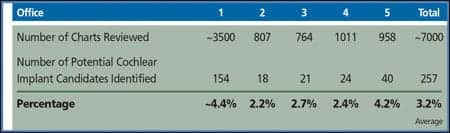
Is it reasonable to believe that there are few or no patients who are cochlear implant candidates seen in an average hearing aid practice? Some data suggest otherwise. As shown in Table 2, when five typical hearing aid dispensing offices in the United States reviewed thousands of their patient charts, they found that, on average, about 3% of the audiograms met the criteria for cochlear implantation. So, if a dispensing practice sees 100 patients in a month, it is reasonable to assume that about three of those patients might receive more help from a cochlear implant than from a hearing aid. In a long-established dispensing practice with several thousand patients in the database, there may be dozens of patients who would be eligible for cochlear implants.

|
| TABLE 2. Cochlear implant candidates found in a random chart review done by five typical US hearing aid dispensing practices (2008). |
Why then does it appear that the hearing care profession is dropping the ball on appropriate referrals for cochlear implants? In many cases, we believe it is due to a lack of awareness about how cochlear implant technology has advanced over time. Many dispensing professionals were trained at a time when cochlear implant candidacy was limited and subsequent performance of implanted patients was, frankly, unimpressive.
These same professionals may not now have any contact with modern cochlear implant users, and thus may not realize that, over the past 25 years, there have been dramatic improvements in the performances of implant recipients, and a corresponding expansion of the criteria for candidacy. Most clinics very likely have a number of patients in their practices who are, in fact, excellent cochlear implant candidates and poor performers with amplification.
How Many Implant Candidates Are There?
According to Kochkin,2,3 in 2005 there were about 7.4 million hearing aid owners in the United States, but only 6.2 million were “active users” who wore their hearing aids at least once a year. More than 21% of hearing aid owners were not satisfied, with satisfaction defined by Kochkin as hearing better in 70% of their listening environments (aided versus unaided). Of the active users, 7% reported that their hearing aids did not improve hearing in any situation. Further, the 20% of hearing aid users with the greatest degree of hearing loss rated benefit from amplification lower than did those with less severe hearing loss.4
While overall customer satisfaction with hearing aids and the professionals who fit them is relatively high, clearly some patients are not doing well. It may be that some of these dissatisfied users are people who have reached a degree of hearing loss where hearing aids are just no longer adequate and referral for an implant evaluation is indicated.
The number of people who could benefit from a cochlear implant but have not yet been referred can only be estimated. While a number of sources report prevalence of hearing loss in the United States, only a few have reported prevalence by degree of loss and estimates vary depending on the definitions used. The US Centers for Disease Control and Prevention5 reports that there are a total of 37 million people with hearing loss. Of these, 3.5% report having “a lot of trouble hearing or totally deaf.” The Gallaudet Research Institute6 reports that there are 1 million people over age 5 who are “functionally deaf.” Blanchfield et al7 estimated there were between 500,000 and 1.2 million people with severe-to-profound hearing loss in the United States in 2001. ASHA reports there are between 250,000 and 1 million potential US cochlear implant candidates.8
Let’s assume that there are about 1 million people with severe-to-profound hearing loss who, by virtue of their degree of hearing loss, might be considered potential candidates for cochlear implants. The industry estimates a population of about 50,000 to 60,000 cochlear implant recipients in the United States, meaning only about 10% of the people who could benefit from a cochlear implant have received one. This leads one to conclude that there is a need for more information relative to who, when, and where to refer potential cochlear implant candidates.
Cochlear Implant Candidacy Criteria
Good dispensing professionals know that hearing aid candidacy is as much a function of lifestyle and motivation as it is of the audiogram. A 45 dBHL high frequency hearing loss might not bother a retired lumberjack, but could be devastating to an elementary school teacher who cannot understand his young students’ questions in the noisy classroom. Although determining candidacy for, selecting, and fitting an appropriate hearing aid do require substantial scientific background, there is also a considerable “art” to successful dispensing. The history and counseling of a patient can sometimes make as much difference as details in the fitting of the amplifier.
Similarly, patient selection for and success with cochlear implant candidacy is multifaceted. When determining potential candidacy for a cochlear implant, beyond the audiologic indicators, the cochlear implant team (surgeon, audiologist, and others) will discuss the individual’s lifestyle, motivation, and family support network. Counseling for appropriate expectations for performance with the implant will include factors such as age at onset, etiology of the loss, duration of profound deafness, previous hearing aid use, and any ossification in the cochlea. Patients need to be aware that success with an implant will require a period of time in a post-surgical habilitation/rehabilitation program.
With those considerations in mind, however, the referral criteria for cochlear implant evaluation are actually quite well defined for the dispenser confronted with a patient who is not successful with hearing aids. Referral criteria are simply based on the degree of hearing loss shown on the audiogram and aided speech recognition test scores—both factors that can initially be evaluated by the hearing aid dispensing clinic in deciding whether a patient should be referred to a cochlear implant clinic.
Cochlear implants are “Class III” regulated medical devices according to the US FDA classification system, and thus the “indications for use” (ie, candidacy criteria) for each cochlear implant model must be approved by the FDA before the device is introduced to the market. Approval is based on results from clinical trials of the device showing safety and efficacy for the intended population, and approved criteria do differ across manufacturers and implant models.
The first multichannel cochlear implant was approved for use in the United States in 1985. At that time, the only candidates were adults with post-lingual deafness (after obtaining speech and language ability), bilaterally profound sensorineural hearing loss (all thresholds >90 dBHL), and 0% aided speech recognition scores. Cochlear implants were subsequently approved for children in 1990, but they too had to be profoundly deaf in both ears at that time.
Since then, however, the FDA-approved criteria for cochlear implantation have changed substantially. Today, the approved criteria for implantation also include pre-lingual hearing loss (before development of speech and language skills), and approved candidates span the age range from infants (>12 months old) to geriatric patients (no upper age limit barring medical contraindications). Research shows that the earlier the intervention (before the critical language acquisition stage), the better the outcome for children.9 Further, older adults show no increase in operative time or length of stay in the hospital,10 with performance outcomes comparable to those of younger implant recipients.11
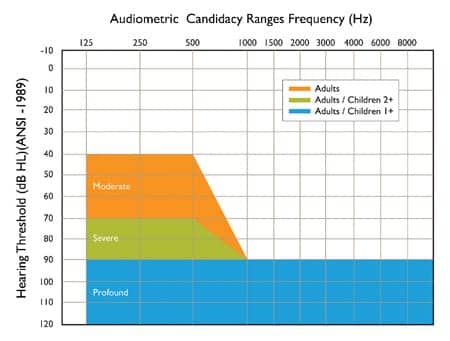
Also, candidacy criteria now include lesser degrees of hearing loss than in the past. For example, the approved criteria for the Nucleus® cochlear implant manufactured by Cochlear Ltd now include audiograms with some residual low-frequency hearing, as shown in Figure 2. As illustrated, adult candidates can have low-frequency hearing thresholds as low as in the moderate hearing loss range (>40 dBHL) as long as they have profound hearing loss (>90 dBHL) at the mid-to-high frequencies. Children between ages 2 and 18 years can have low-frequency thresholds in the severe hearing loss range (>70 dBHL). Infants ages 1 to 2 years must show profound hearing loss across the audiometric range.
|
| FIGURE 2. Current FDA-approved speech recognition criteria and audiogram ranges by age group for candidacy for Cochlear™ Nucleus® cochlear implants (graph courtesy of Aaron Parkinson). |
Before a patient is considered a cochlear implant candidate, he or she must have been given the opportunity to try well-fit amplification. Especially for young children, there should be a demonstrable lack of auditory progress with bilateral hearing aids after 3 to 6 months of aural habilitation.
However, people who receive some limited benefit from hearing aids are still implant candidates. The current FDA-approved candidacy criteria for speech recognition in adults and children for the Nucleus implant are also shown in Figure 2. For adults, aided sentence recognition (using recorded materials) must be 50% or less in the ear to be implanted and 60% or less in the “best-aided” condition (either the contralateral ear alone or bilateral hearing aids) to meet the criteria.
The sentence-level test material most commonly used today for cochlear implant evaluations in adults is the HINT sentence test in quiet,12 which evaluates key word recognition with contextual cues provided. Some hearing aid dispensing clinics may not have access to these sentence test materials, however, so it is reasonable to examine the patient’s aided scores using monosyllabic word test materials (CNCs13 or PB word scores) as an additional screening tool beyond the audiogram. Although there will be differences across patients in terms of their ability to utilize contextual cues in sentences, and candidacy ultimately must be decided based on recorded sentence test scores, aided word recognition scores of about 30% or less would suggest the need for referral for further evaluation at a cochlear implant center.
Candidacy criteria for the Nucleus implant in children include best aided sentence performance that is <30% specifically using the Multisyllabic Lexical Neighborhood Test (MLNT) or the Lexical Neighborhood Test (LNT)14 (the latter for older children or those with higher ability level).
Although these tests would not likely be found in a hearing aid dispensing clinic, it is not necessary that speech recognition testing be done in children prior to referral for cochlear implant evaluation. Due to the importance to development of speech and language, and the negative impact of the hearing loss on learning ability, all severe-to-profoundly impaired children falling within the audiogram candidacy range should be referred for full evaluation at a cochlear implant center.
Cochlear Implant Surgery and Reimbursement
Cochlear implantation has become a routine procedure in the hands of a skilled ENT surgeon. Most people tolerate the surgery very well and go home from the surgical suite or outpatient clinic the same day.
Some professionals and consumers may think that, since Medicare and most insurance companies will not pay for hearing aids, they will not pay for more costly cochlear implantation. In fact, Medicare does cover cochlear implants, as do many private insurance carriers. Some insurers even cover bilateral cochlear implants for qualified candidates.
Modern-Day Performance with Cochlear Implants
Dispensing professionals who are not aware of the changes in candidacy criteria for cochlear implants also may be surprised by the improvements that have occurred in the performance of cochlear implant recipients.15 Over the years, cochlear implant technology has advanced in much the same manner as hearing aid technology. Some cochlear implant speech processor models now have the capability of multiple user-selectable programs and directional microphones to provide recipients with greater comfort and higher performance across diverse listening environments. Advanced signal processing strategies and speech coding enhancements now enable many implant users to achieve high open-set (no visual cues) word recognition scores and the ability to talk on the telephone—achievements that would have been inconceivable just a few years ago.
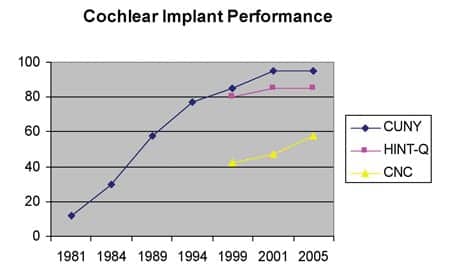
In the early 1980s, the best one could hope for after implantation was low double-digit open-set sentence test scores. Currently, open-set speech recognition performances for implant patients (listening with the cochlear implant ear alone) average about 80% to 90% correct on sentence-level materials and 55% to 60% correct for monosyllabic word tests,1 as illustrated in Figure 3.
|
| FIGURE 3. Advances in technology and signal processing in cochlear implants have resulted in improved performance outcomes over time. Shown are group mean percent correct scores for CUNY and HINT sentences in quiet, and for CNC monosyllabic words. Source: Internal data from Cochlear Americas clinical trials. |
Referral Benefits for the Dispensing Practice
For those who own a dispensing practice or get paid a commission on the sale of hearing aids, the prospect of referring a patient to another clinic might not initially seem very appealing. Consider the following, however: the No. 1 driver of customer satisfaction in the dispensing office is when you are able to provide solutions to the patient’s hearing problem. When hearing aids do not solve the problem and you recommend a cochlear implant, you become the driver of that patient’s satisfaction, and satisfied patients tell their hearing-impaired friends about your office/practice.
Only a small percentage of the people you see will actually be cochlear implant candidates, and some of these may even return after evaluation if the implant team determines that they are, in fact, not good candidates. The bottom line is that, in addition to the great service you have performed for the individual, any goodwill you generate by referring a patient for something as life-changing as a cochlear implant is likely to result in more traffic to your office instead of less.
Further, about 90% of those who have a cochlear implant are unilaterally rather than bilaterally implanted. As cochlear implant candidacy criteria have expanded so that patients with more usable residual hearing are being implanted, many will continue to wear a hearing aid in the nonimplanted ear—a configuration called “bimodal devices.”16 Not every patient wants or needs bilateral cochlear implants, and some authors have argued that bimodal fittings provide “complementary cues” to hearing.17 Many cochlear implant clinics do not have the time, equipment, or inclination to fit hearing aids, so the audiologist/dispenser who is proficient in both cochlear implant criteria and the specifics of bimodal fittings may well have an advantage in the competitive hearing aid market. For a review of factors to consider when fitting bimodal devices, see Huart and Sammeth.16
Finally, it is important to keep in mind that patients who get the least benefit from hearing aids often take up the most time. Multiple reprogramming visits might still end up in a return for credit. Even if someone does not return a hearing aid for credit but ends up putting it in their drawer, the result is negative word of mouth about the practice and statements that hearing aids do not help. There is just no incentive for a dispenser not to refer when the patient might be better served by a cochlear implant.

|
|
Fitting and Evaluating a Hearing Aid for Recipients of a Unilateral Cochlear Implant: The NAL approach—Part 2. Bimodal hearing should be standard for most cochlear implant users. By Therese Ching, PhD, et al. Aug 2004 HR. Cochlear Implants and Education of the Deaf Child. By Ann Geers, PhD. May 2003 HR. A Model Program for Children with Cochlear Implants. By Carolyn Brown, MS. July 2008 HR. Cochlear Implants and Hearing Instruments: Do They Mix? By Marsha McCandless, MA, & Clough Shelton, MD. Nov 2000 HR. |
We are, of course, not suggesting that a well-satisfied adult hearing aid patient be sent to a cochlear implant center just because he or she meets the candidacy criteria. Imagine a new customer who walks into your clinic wearing a hearing aid purchased on eBay. Your evaluation reveals hearing thresholds falling within the adult shaded area on the audiogram in Figure 2. Aided HINT sentence recognition scores in quiet are only 15% using his second-hand aid, so you fit new high-quality bilateral hearing aids, and now his bilateral aided sentence recognition score reaches 56%. You are disappointed that the results are not better, but the patient is ecstatic. He reports that his quality of life and communication ability have been greatly improved. This patient may have no desire to even consider a cochlear implant at this point in time.
On the other hand, consider a different patient, one whom you have taken care of for more than 10 years. When you met her, she had CICs that were no help and whistled all the time. You fit her with directional microphone BTEs and she could not believe the improved performance. She has purchased three sets of hearing aids from you in the past decade. Unfortunately, now her audiogram has progressed into the adult shaded area of Figure 2, and despite your best efforts, her aided bilateral HINT sentence recognition scores are only about 40%. You fit an FM system, which only helps a little. She reports that she is afraid she will probably have to quit her job because it is just too hard to hear what is going on around her, and she is very frustrated that she can no longer understand her grandchildren and must rely on her husband to answer the phone. When she stops by the dispensing office to drop off a gift basket to thank you for all you have tried to do, she tells you, “I just wish there was something else you could do to help me.” You can. You can refer this patient for evaluation for a cochlear implant.
References
- Balkany T, Hodges A, Menapace C, et al. Otolaryngol-Head Neck Surg. 2007;136(5):757-762.
- Kochkin S. MarkeTrak VII: Hearing Loss Populations Tops 31 Million. Hearing Review. 2005;12(7):16-29.
- Kochkin S. MarkeTrak VII: Obstacles to adult non-user adoption of hearing aids. Hear Jour. 2005;60(4):27-43.
- Kochkin S. MarkeTrak VII: Customer satisfaction with hearing aids in the digital age. Hear Jour. 2005;58(9):30-37.
- US Centers for Disease Control and Prevention. Available at: nidcd.nih.gov/hearth/statistics/quick.htm
- Gallaudet Univ. Can you tell me how many deaf people there are in the US? Available at: gri.gallaudet.edu/Demographics/deaf-US.php. Accessed April 23, 2009.
- Blanchfield B, Feldman J, Dunbar J, Gardner E. The severely to profoundly hearing-impaired population in the United States: prevalence estimates and demographics. J Am Acad Audiol. 2001;12(4):183-9.
- American Speech Language Hearing Assn. Incidence and Prevalence of Hearing Loss and Hearing Aid Use in the United States – 2008 Edition. Available at: www.asha.org/research/reports/hearing.htm. Accessed April 27, 2009.
- Geers AE. Factors influencing spoken language outcomes in children following early cochlear implantation. Adv Otorhinolaryngol. 2006;64:50-65.
- Labadie R, Carrasco V, Gilmer C, Pillsbury H. Cochlear implant performance in senior citizens. Otolaryngol-Head Neck Surg. 2000;123(4):419-424.
- Kelsall D, Shallop J, Burnelli T. Cochlear implantation in the elderly. Am J Otol. 1995;16(5):609-615.
- Nilsson M, Soli SD, Sullivan J. Development of the Hearing In Noise Test for the measurement of speech reception thresholds in quiet and in noise. J Acoust Soc Amer. 1994;95:1085-1099.
- Peterson FE, Lehiste I. Revised CNC lists for auditory tests. J Speech Hearing Dis. 1962;27(1):62-70.
- MLNT/LNT materials (developed by Kirk et al at Indiana University). Available from Auditec of St Louis at www.auditec.com.
- Krueger B, Joseph G, Rost U, Strauss-Schier A, Lenarz T, Buechner A. Performance groups in adult cochlear implant users: speech perception results from 1984 until today. Otol Neurotol. 2008;29(4):509-512.
- Huart S, Sammeth C. Hearing aids plus cochlear implants: Optimizing the bimodal pediatric fitting. Hear Jour. 2008;11(61):54-58.
- Ching T, van Wanrooy E, Hill M, Dillon H. Binaural redundancy and inter-aural time difference cues for patients wearing a cochlear implant and a hearing aid in opposite ears. Int J Audiol. 2005;44:513-521.
Correspondence can be addressed to HR at [email protected] or Steve Huart, PhD, at .
Citation for this article:
Huart S, Sammeth C. Identifying Cochlear Implant Candidates in the Hearing Aid Dispensing Practice Hearing Review. 2009;16(5):24-32.





