Tech Topic | May 2017 Hearing Review
Part 2: Promoting better fit-to-preference and efficiency
In Part 1 of this 2-part series (April 2017 Hearing Review),1 we discussed the changing landscape of healthcare and how it is likely to impact hearing healthcare. First, patients today tend to be better informed about their healthcare needs and services than they were in the past. They behave more like consumers, and take a more active role in their healthcare choices.
Behaving like a consumer engages the recipient of healthcare services in a different way than traditional models. Since patient engagement in healthcare has been shown to lead to improved outcomes, it makes sense to embrace this trend. And, because this consumerism trend coincides with the baby boomer generation reaching the age where hearing loss is common, it necessarily affects hearing healthcare.
Another healthcare trend is provision of services and sharing of information over distance via electronic means. Consumers are open to this trend to telehealth and teleaudiology, while hearing care professionals (HCPs) are cautious in their attitudes. One area of hearing healthcare that appears to consume a disproportionate amount of resources for both the consumer and the HCP is clinic visits for fine-tuning of hearing aids. The question is whether some aspects of telehealth can be leveraged to enhance and streamline the hearing aid fitting and adjustment process—without usurping the control of the HCP or disrupting the HCP/client relationship.
As hearing instrument technology evolves, our clinical practices also evolve. Yet as ever, user satisfaction with the hearing instruments continues to be a primary goal of our fitting protocols. How can we increase user satisfaction with today’s new technological advances?
Increased Satisfaction with Patients as Consumers
Numerous studies over the years suggest that patient satisfaction and self-perception of benefit with hearing instruments is correlated with the patient’s level of engagement in the health care process (see Hibbard and Greene2 for a review). Engagement of users in the fitting of hearing instruments includes activities that are non-passive. A non-passive, or active fitting protocol, invites the user along for the journey, and immediately places them in the driver’s seat and in a position of better ownership and understanding of what is occurring.
Active time spent with the user can include a number of procedures not directly associated with the physical act of programming hearing instrument, such as real-ear verification measures, outcome measures of benefit, satisfaction and perceived handicap reduction, and counseling. As these measures all involve the user to some degree, they tend to build on one another in the final perception of the clinical encounter.
Real-ear measures can promote engagement as well as preference. A study showed that experienced hearing instrument users preferred fitting with a real-ear verification process as compared to the hearing instrument manufacturer’s first fit.3 Shi et al4 reported validation measures resulted in higher user satisfaction rates and the need for fewer fine-tuning adjustments at 3-months post-fitting. Together, verification and validation measures have been shown to reduce the return rate of hearing instruments, while increasing user satisfaction.5 Counseling and interaction with the HCP has a positive effect on users’ self-perception of benefit6 as well as satisfaction.7 By virtue of this engagement, an active fitting procedure promotes a more open relationship between the fitter and the user, and paves the way for better outcomes. However, the actual programming or adjustment of the devices should not be overlooked as a potential opportunity for active user engagement. In fact, a survey of 100 hearing instrument users revealed that 90% of them would prefer to be more actively involved in the hearing instrument fitting process.8 In addition, hearing aid users who actively participate in fine-tuning their hearing aids using an app may initially accept gain settings that are closer to prescriptive targets than those who are fit according to a more traditional protocol where they play a more passive role (Hallenbeck S, Groth J, “Engage users and reinvent your fittings with the ReSound Smart 3D app,” white paper; 2017).
Users are increasingly technologically-savvy, and may look to online sources for hearing solutions. These may include personal sound amplification products (PSAPs) or direct-to-consumer hearing instruments via online sales. It is not difficult to acquire hearing instruments or amplifiers without much intervention, if any, from a hearing professional. The question is, can this method of service delivery compete with the clinical model, in terms of user satisfaction and fit?
A recent interview-based study asked about the perceptions of internet-based hearing instrument acquisition among 18 experienced hearing aid users.9 The study participants saw some advantages to this kind of direct access to product, including the convenience of not needing to leave home to acquire devices. However, concerns were raised with respect to the lack of clinical services that would be received; specifically, participants were concerned about how their individual hearing loss would be factored into the device programming, and how adjustments to the fitting could be made. Interestingly, they thought it might be beneficial if these changes could be made in some way over the internet. Yet, despite internet fine tuning and adjustments, participants still were concerned about a lack of personal professional contact with an exclusively internet-based hearing aid delivery system. Even though there was greater convenience perceived for an at-home, purely online solution, participants in the study expressed a preference to be treated by a knowledgeable experienced expert in treating hearing loss. They felt this level of professional service could not be attained online.
Further support for the importance of professional intervention in the fitting process was revealed by Humes et al10 (see page 12), who carried out “the first-ever, placebo controlled, double-blind, randomized clinical trial of hearing aid outcomes.” In this large-scale study, participants were randomly assigned to one of three parallel groups: 1) An audiological best-practice service delivery, 2) An over-the-counter (OTC) model where participants selected and fit their own devices, and 3) A placebo condition where the audiological best-practice service delivery model was used, but the hearing aids were programmed to be acoustically transparent. The hearing aids were identical in each branch. The efficacy of the hearing aids for the groups fit according to best practice and with the OTC model was clearly established compared to the placebo group. Furthermore, there were no significant differences in speech recognition or a subjective benefit measure for the best-practice and OTC groups.
However, those fit according to the best-practice model in the Humes et al study10 showed significantly higher satisfaction scores than the OTC group. Even more telling was the fact that 81% of participants in the best-practice group chose to purchase the hearing aids, while only 55% in the OTC group did so. Interestingly, 36% of participants in the placebo group also chose to purchase the hearing aids (the price paid for purchased hearing aids was refunded at the conclusion of the study, but the participants did not know this at the time they made the purchase decision and payment). The best-practices group and the placebo group both interacted with the HCP, who performed fitting and verification using real-ear measurements, and provided hearing aid orientation and counseling. The OTC group did not experience this interaction.
For the participants in Humes et al,10 the differences in satisfaction combined with the purchase decision illustrate the great impact of the professional interaction. The OTC group received equivalent benefit from the devices as the best-practices group, but nearly half chose not to purchase and they were less satisfied. The placebo group did not benefit from the amplification, but over one-third of them decided to purchase anyway—presumably due to the professional interaction and guidance. While the results of this study support that hearing aids delivered via a do-it-yourself model can provide meaningful hearing benefit, they also strongly support that the relationship with the HCP influences outcomes to a significant degree and ultimately can make the difference in the user’s commitment to wearing the hearing aids.
Findings such as these are not surprising. Research in the context of telemedicine has shown a preference for face-to-face interactions over purely internet-based hearing care provision.11 It appears that to achieve the goal of user satisfaction, a more direct, active, human element continues to be preferred and necessary.
We can conclude from research like that of Humes et al10 that the need for active care in audiology is significant. The user is not necessarily looking for a passive experience during the fitting of hearing instruments. But how can we engage users more in the fitting process, especially if it would lead to greater satisfaction and a higher retention rate? How can we promote seamless integration of hearing aids into users’ lives without the need for multiple follow-up visits that remove them from their daily routines? How can we make the journey of fitting and adjusting as efficient as possible, while attaining the best fit-to-preference for the individual?
Efficient Professional Hearing Care and Patient-Preferred Hearing Aid Settings
Achieving efficient, professional hearing care that results in patient-preferred hearing instrument settings requires a multi-faceted approach. Improvements in technology both during and after the fitting session are crucial to the realization of these goals. Wireless fitting technology has improved dramatically over the past 10 years, evolving the hearing instrument fitting process into a quicker endeavor. Wireless fittings remove the need to manually connect hearing instruments—and the person wearing them—directly to the computer. The untethered nature of modern wireless fittings promotes a more natural interaction between the professional, the user, and the technology.
Approaches aimed at achieving better fit-to-user-preference have emerged in recent years. Trainable hearing instruments were introduced as a user-driven alternative to fitting with traditional, non-learning hearing instruments. In a trainable hearing instrument, the device analyzes the acoustic environment while noting user-driven changes to parameters, such as volume. Over time, when the user encounters similar acoustic environments, the device applies these adjustments.12,13 The potential advantages of this type of learning hearing instrument are reduced need for follow-up visits, greater personalization, and better engagement of the user in the fitting process.14
The downside of trainable hearing instruments is that it may take time for a hearing instrument to accurately and consistently apply the desired changes. The onus is on the user to make these adjustments consistently and often, while in that particular listening environment. Further, if mistakes are made, it takes time for the hearing instrument to “unlearn” them. And if the concern is major, such as feedback, the time it takes for trainable hearing instruments to effect a solution such as high-frequency gain reduction can be unacceptable.
A newer development with the same goal as trainable hearing instruments was the introduction of user-controlled apps with “favorite” settings. A user saves a “favorite” setting in a certain listening environment or even a particular geo-tagged location, and this setting can be selected or automatically applied when the user returns to that setting.
Today’s wireless and hearing instrument technology affords HCPs even more opportunities to quickly meet hearing needs. The obvious solution to the “user fit-to-preference versus time constraints for both users and professionals” dilemma is a hearing fitting protocol that marries the personal and professional interactions so important for user satisfaction with the convenience of user-driven services, such as apps or secure cloud connections. Through technological innovations, we are now able to meet the needs and preferences of users who increasingly use internet-based services, yet still value professional attention.
For the participants in Humes et al, the differences in satisfaction combined with the purchase decision illustrate the great impact of professional interaction.
Combining Personal Hearing Care with Efficiency and Convenience
ReSound SmartFit is a new fitting software platform that provides HCPs with the tools to meet the needs of today’s users. Two goals are paramount in the design and implementation of this new technology. The first goal is to engage the user more directly, to achieve a better fit-to-preference and increased user satisfaction. The second goal is to maximize the efficiency of the fitting process, by reducing the time spent on passive activities such as connecting to hearing instruments and programming. The time gained from a faster fitting process can then be used to engage the user in activities that research shows are better correlated with satisfaction and benefit from the hearing instruments, as well as a better relationship with the professional.
Direct user engagement is achieved both during the fitting and afterwards, when the user is wearing the devices in daily life. Clinical demonstrations of how the hearing aids sound in simulated environments can be helpful, but often it is only when wearing the hearing aids in actual daily activities that fine tuning needs emerge. Imagine if a user could send a secure message to their HCP describing an issue with the hearing aids or the fitting at their own convenience—even in the situation where they are experiencing it—and the fitter could resolve the issue at their convenience as well, without the user having to return the clinic for a follow-up visit.
ReSound SmartFit with ReSound Assist is designed for this level of flexibility and personalization with an asynchronous model of teleaudiology. By asynchronous, we mean that the HCP and the user do not need to be present simultaneously to interact in real time, but can instead both carry out the communication and actions when it best suits each of them. Here’s an example of how it works:
- A patient is fitted with ReSound LiNX3D hearing instruments and ReSound SmartFit wireless fitting software. The fitting may include personalization and engagement activities, such as real-ear measures, speech in noise testing, counseling, and relationship-building between the professional and the user.
- Once home and using the hearing aids, the patient may notice issues in certain listening environments. She may be uncertain as to whether these might be solved by an adjustment or some other means. A solution might be looked for using the ReSound Smart 3D app, but ultimately she may want to consult the HCP. She sends a request to the HCP via the secure cloud. Her request includes a questionnaire that helps her formulate the issues in a way that is easily decoded by the HCP. Furthermore, the HCP receives a weekly update of the datalogging in the hearing aids, so that information on usage patterns and environments can inform clinical decisions.
- The HCP downloads and accesses her request, and decides on the best course of action. Perhaps the issue is resolved with a return message that answers or reassures the user. Or perhaps a face-to-face visit seems in order, as might be the case with a physical comfort issue. It is also possible that the issue is one that can be resolved remotely, as would be the case with a fitting software-based fine-tuning of settings. In this case, the HCP can make the programming change and send it as a data package via the cloud to the user. The user receives a message that an update to her hearing aids is available. At her convenience, she can download the data package to her mobile device and apply the changes wirelessly to the hearing instruments. All adjustments can also be rejected or ignored if she desires to return to or keep her previous settings.
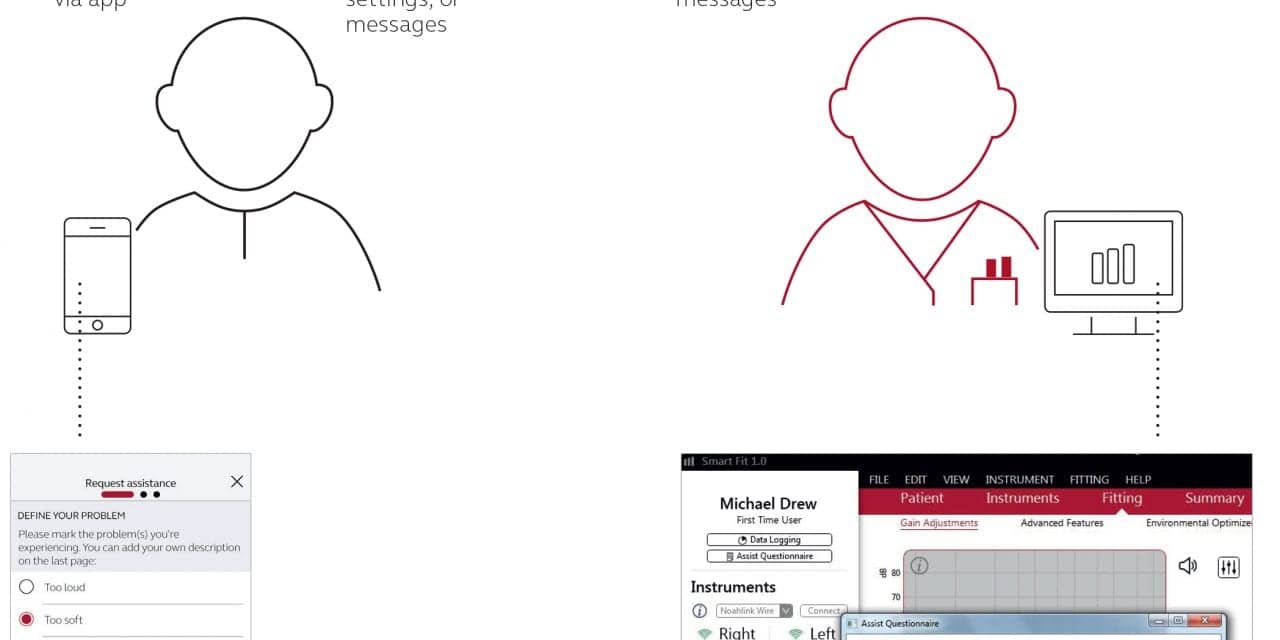
The ReSound Assist process is illustrated in Figure 1. With the opportunities for this “remote fine tuning” available via ReSound SmartFit and ReSound Assist, users are able to report issues and express their preference for different hearing instrument settings, such as volume changes and program settings.

Figure 1. ReSound Assist lets the user send a message to the HCP, who can respond at their convenience with information or updated settings for the hearing aids. Because ReSound Assist and ReSound Smart Fit form an integrated system, the full range of settings are available to the HCP, and all fitting information will be stored with the client data. The HCP also receives status updates including a weekly datalog from the hearing aids, as well as information on whether the user updated their hearing aids if an update was sent.
The reasonable question arises: How well are users able to discern their preferred settings? Dreschler et al15 found that the selection of a closed set of hearing instrument settings by users is both reliable and reproducible. This suggests that user-driven fine-tuning adjustments could be a viable alternative to more traditional fine-tuning adjustments performed in the clinic, as long as the hearing instruments are initially programmed appropriately by the hearing professional. Clinical professional programming is crucial to approximate the user’s preferred settings, and tends to limit the need for dramatic adjustments following the fitting. For this reason, the option for ReSound Assist requires that the hearing instruments are initially programmed by the HCP in the more traditional clinic encounter.
ReSound SmartFit introduces highly secure cloud-based services to the hearing instrument industry. This technology does not significantly change existing procedures and processes in the interactions between HCPs and hearing aid users; instead, it provides an optional method to allow both parties to share information or hearing aid settings remotely. This offers efficiencies for both the HCP and the user that can enrich the hearing aid fitting experience.
Angley et al16 investigated the practicalities of a synchronous model of teleaudiology for hearing aid fitting and follow-up. They revealed satisfaction with the process on the part of both the HCPs and the users who participated. They also reported that the most frequently cited reason for users wanting remote appointments was time savings, despite that fact that 86% of them lived within 50 minutes’ travel time from the clinic.
The advantages of this technology are ground-breaking. Instead of having to wait for trainable hearing instruments to “learn” a user-driven remote control change, or the user needing to set desired changes as a “favorite” via the user app, adjustments can be immediately applied by the user after the hearing professional sends the secure data package. These adjustments can also be “undone” if the user so desires. Moreover, because ReSound Assist is part of an integrated fitting system, a complete range of changes can be made via ReSound SmartFit. The benefits of user-controlled changes—personalization, reduced need for clinical follow-up visits, and better user engagement—are maintained in a more efficient manner.
With secure cloud capabilities, other timesaving options are possible as well. One added functionality of ReSound Assist is the ability to update the hearing instrument firmware remotely, and at the convenience of the user. Firmware updates are useful for keeping a hearing instrument working as well as possible in the face of evolving technology. This could include compatibility updates for operations as new versions of mobile device operating systems are released, as well as general updates to the current hearing system the user purchased. Just as smartphone or iPhone users can download and update their devices’ apps, a hearing instrument user can now update their devices to enjoy optimal performance.
The ReSound SmartFit Remote Firmware Update feature allows a user to download firmware changes without an otherwise unnecessary clinical visit. ReSound sends firmware releases to the secure ReSound cloud, and makes them available for download via the hearing instrument user’s mobile device(s). A step-by-step process guides the user through the required steps for updating the firmware in the hearing instruments.

Figure 2. While hearing aids provide benefit in terms of better hearing, interaction with the HCP helps engage the user and leads to better outcomes. The addition of convenient ways to communicate and make hearing aid adjustments via the secure cloud accommodate the trend toward consumerism in hearing healthcare, and can enhance the professional relationship.
The functionalities provided by ReSound Assist help to resolve the issue of providing personal, professional care amidst time constraints in the clinic. At the same time, this technology accommodates trends in hearing healthcare including the rise in consumerism, increasing acceptance of telehealth, and the widespread adoption of mobile smart devices. Innovations like ReSound Assist that let the user take charge of their hearing instruments can also lead to a greater sense of ownership and improved outcomes. Harnessing secure cloud technology, both users and HCPs can reach a greater level of satisfaction and device performance without the typical logistical inconveniences of clinical visits for minor concerns or updates. When more time is freed up in a busy clinic from these activities, more time is available to do what really counts: meeting users’ hearing needs, serving new clients, counseling, and building strong relationships between the HCP and the hearing aid user.
About the Authors
Tammara Stender, AuD, is Director of Global Audiology, and Jennifer Groth, MA, is Director of Audiology Communications at ReSound in Glenview, Ill; David Fabry, PhD, is VP of Global Medical Affairs at ReSound in Bloomington, Minn.
References
-
Fabry D, Groth J. Teleaudiology: Friend or foe in the consumerism of hearing healthcare? Hearing Review. 2017;24(4):16-19. Available at: https://hearingreview.com/2017/04/teleaudiology-friend-foe-consumerism-hearing-healthcare
-
Hibbard JH, Greene J. What the evidence shows about patient activation: Better outcomes and care experiences; fewer data on costs. Health Affairs. 2013;32(2):207-214.
-
Abrams HB, Chisolm TH, McManus M, McArdle R. Initial-fit approach versus verified prescription: comparing self-perceived hearing aid benefit. J Am Acad Audiol. 2012;23:768-778.
-
Shi L, Doherty KA, Kordas TM, Pellegrino JT. Short-term and long-term hearing aid benefit and user satisfaction: A comparison between two fitting protocols. J Am Acad Audiol. 2007; 18(6):482-495.
-
Valente M, Potts LG, Valente M. Signal testing approaches; clinical procedures to improve user satisfaction with hearing aids. In: Tobin H, ed. Practical Hearing Aid Selection and Fitting. Baltimore: Department of Veterans Affairs. Chapter 6;1995.
-
Street RL, Makoul G, Arora NK, Epstein RM. How does communication heal? Pathways linking clinician-patient communication to health outcomes. Patient Education and Counseling. 2009;74(3):295-301.
-
Strom K. HR interviews Sergei Kochkin, PhD. Hearing Review. 2005;12(11)[Oct]:24-32,82. Available at: https://hearingreview.com/2005/10/hr-interviews-sergei-kochkin-phd
-
Schweitzer C, Mortz M, Vaughan N. Perhaps not by prescription–but by perception. In: Kochkin S, Strom KE, eds. High Performance Hearing Solutions. Hearing Review. 1999; 3[Suppl]:58-62.
-
Chandra N, Searchfield GD. Perceptions toward internet-based delivery of hearing aids among older hearing-impaired adults. J Am Acad Audiol. 2016;27: 441-457.
-
Humes LE, Rogers SE, Quigley TM, Main AK, Kinney DL, Herring C. The effects of service-delivery model and purchase price on hearing aid outcomes in older adults: A factorial randomized double-blind placebo-controlled clinical trial. Am J Audiol. 2017 Mar 1;26(1):53-79. doi: 10.1044/2017_AJA-16-0111.
-
Eikelboom RH, Atlas MD. Attitude to telemedicine, and willingness to use it, in audiology patients. J Telemed Telecare. 2005;11[2: Suppl]:S22-S25.
-
Dijkstra TMH, Ypma A, De Vries B, Leenen JRGM. The learning hearing aid: Common-sense reasoning in hearing aid circuits. Hearing Review. 2007;14(110[Oct]:34-51. Available at: https://hearingreview.com/2007/10/the-learning-hearing-aid-common-sense-reasoning-in-hearing-aid-circuits
-
Taylor B. Listener preferences and trainable hearing aids: Historical perspectives, current trends and practical considerations. Oct 19, 2009. Available at: http://www.audiologyonline.com/articles/listener-preferences-and-trainable-hearing-873.
-
Dillon H, Zakis JA, McDermott H, Keidser G, Dreschler W, Convery E. The trainable hearing aid: What will it do for clients and clinicians? Hear Jour. 2006; 56(4): 1-6.
-
Drechsler WA, Keidser G, Convery E, Dillon H. Client-based adjustments of hearing aid gain: The effect of different control configurations. Ear Hear. 2008; 29(2): 214-227.
-
Angley GP, Schnittker JA, Tharpe AM. Remote hearing aid support: The next frontier. J Am Acad Audiol. 2017; 00:1-8.
CORRESPONDENCE can be addressed to HR or Dr Stender at: [email protected]