What a Pilot’s Checklist Can Teach Us About Better Hearing
Think about an airline pilot, no matter how experienced. Before every single flight, they run through a pre-flight checklist. Not because they might forget how to fly, but because the stakes are too high to leave anything to chance. The checklist guarantees safety and performance with absolute consistency, flight after flight, regardless of how tired the pilot is or how long the day has been.
In hearing care, the stakes are just as real. Helping someone reconnect with the world around them, with their grandchildren’s laughter, with conversation at the dinner table, with the confidence to walk into a noisy room, is one of the most meaningful things a clinician can do. And yet, even the most skilled and caring professional can have an off day. The patient journey in hearing care is long and has many critical touchpoints: the first intake, the goal-setting conversation, the follow-up, the outcome check-in. Miss one, and the whole experience can unravel.
That’s the case for standardized hearing care. Not as a constraint on clinical expertise, but as the framework that makes expertise reliable, at every stage, for every patient.
It’s Not Just About the Fitting. It’s About the Whole Journey.
When most people think about hearing care quality, they think about the fitting itself. But the fitting is just one moment in what should be a carefully structured relationship between clinician and patient.
Consider how many things have to go right before a patient even arrives at that moment. Did the intake capture the right information? Did the clinician understand where hearing loss is truly affecting this person’s life, not just their audiogram, but their relationships, their work, their confidence? Were their goals documented in a way that can actually guide the care plan?
And consider what happens after. Was there a follow-up survey to catch early dissatisfaction before it became a return? Were outcomes tracked in a way that demonstrates genuine value to the patient and to the practice? Did the patient feel supported throughout, or did they feel like they were on their own after walking out the door?
Each of these touchpoints is an opportunity to either build trust or lose it. A standardized approach to the entire care journey ensures that none of them are left to chance.
From Guesswork to Guarantee: What Consistency Actually Means for Patients
Without a structured process, even experienced clinicians are working from intuition, and intuition, however well-honed, is inconsistent by nature. One patient gets a thorough goal-setting conversation; the next gets a rushed one. Follow-up happens for some patients but slips for others. Outcome data exists in some files but not across the practice as a whole.
The result is a patient experience that varies not just between clinics, but within the same clinic, even with the same clinician, depending on the day.
Standardization replaces that variability with reliability. It means every patient goes through the same carefully designed journey, from the first intake question to the last outcome survey, because the process itself ensures nothing is missed. The clinician’s expertise shapes how each step is delivered; the structure ensures every step is delivered.
This is what transforms good intentions into guaranteed outcomes. And for patients navigating a confusing and often emotional process, that consistency is more than a quality metric, it’s a form of trust.
What Does a “Gold Standard” Appointment Actually Look Like?
So what does it mean in practice to standardize the full care journey? It’s less about rigid scripts and more about ensuring the right things happen at the right time, consistently.
It starts with truly understanding the patient. A structured intake captures not just clinical information, but the human context, where hearing loss is affecting daily life, what the patient’s goals are, what success will actually look like for them. This isn’t a checkbox; it’s the foundation everything else is built on.
It continues with structured follow-up. Timely surveys after fitting catch problems early, before frustration sets in. They also capture positive outcomes, data that builds the case for the value of care and fuels ongoing trust.
It’s supported by efficient, accurate clinical documentation. When note-taking is streamlined, clinicians spend less time on administration and more time with patients. The record of each appointment becomes a reliable thread running through the entire patient relationship.
It ends, and begins again with outcomes. Tracking outcomes systematically across a practice doesn’t just improve individual care. It reveals patterns, highlights what’s working, and builds the kind of evidence base that sets a clinic apart.
When these elements work together, the patient journey stops being a series of disconnected appointments and becomes a coherent, supported experience. That’s the difference between a practice patients tolerate and one they recommend.
How the Right Tools Make Consistency Effortless
The rise of audiology practice management software is changing what’s possible for hearing care clinics. Rather than relying on individual memory or disconnected systems, the right platform can guide clinicians through a consistent, evidence-based workflow at every stage of the patient journey, from intake to outcome, ensuring that nothing is missed, and that the standard of care doesn’t vary with the day or the clinician.
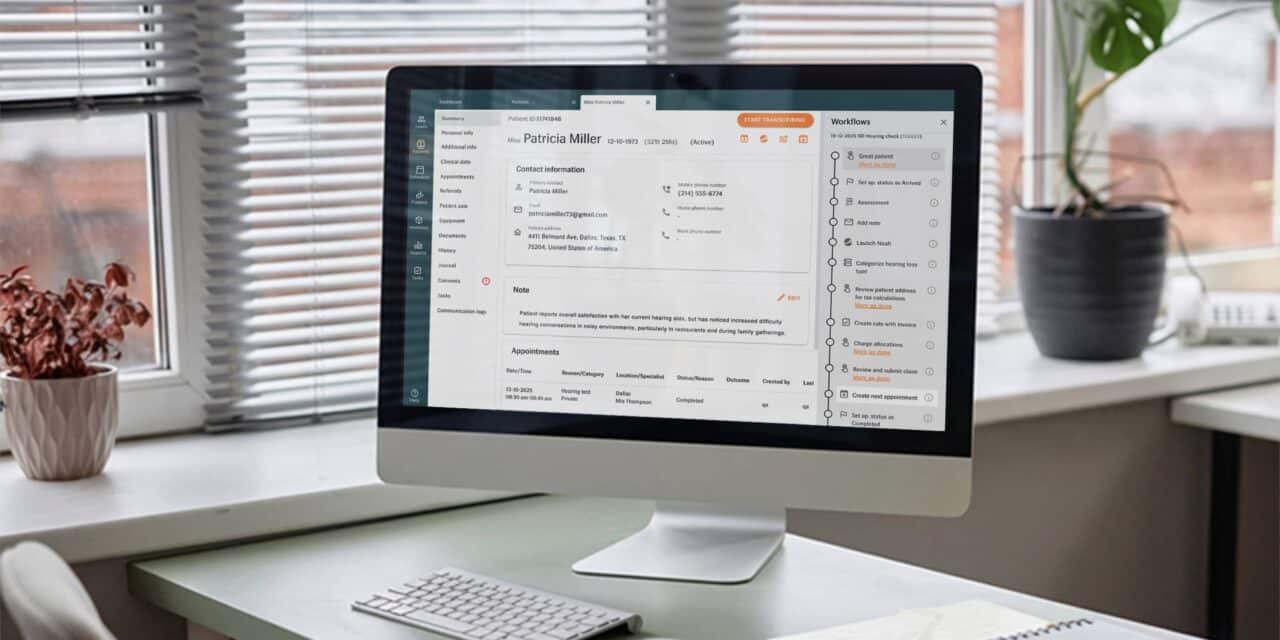
This is precisely what Auditdata, Practice Management Software, Manage was built to do.
Manage is a software designed specifically for hearing care, built around the principle that consistency shouldn’t be hard. It structures the patient journey from first contact to long-term follow-up, supports clinicians with AI-assisted note-taking so less time is spent on administration and more on care, and captures outcome data through integrated surveys that flag problems early and demonstrate value over time.
For clinic owners, that consistency translates directly into fewer returns, higher patient satisfaction, and a practice built on outcomes rather than transactions. For clinicians, it means less cognitive load, more time for the human side of care, and the quiet confidence of knowing that nothing has been missed.
The Standard Every Patient Deserves
The best clinicians have always known that process isn’t the enemy of care, it’s the foundation of it. A structured approach doesn’t make the experience less human. It frees the clinician to be more present, more focused, and more effective, because the important things are taken care of.
Every patient who walks through the door deserves a consistent, high-quality experience, not because they happened to come in on a good day, but because the practice is built that way.
If you’re ready to make that the standard in your clinic, we’d love to show you what Manage can do. Book a demo today! → https://www.auditdata.com/get-started-with-auditdata/
Read the other posts in this series:
Smarter Online Booking for Multi-Location Hearing Clinics
Audiology Practice Management Software: Choosing the Right Fit
How Multi-Location Hearing Clinics Scale Successfully, and Why Practice Management is the Foundation
More Connection, Fewer Clicks: AI Notes That Put Patients First
SPONSORED BY

Medqor is committed to protecting and respecting your privacy. We may contact you about our products and services or share information with sponsorship partners, as well as other content that may be of interest to you. For further information, please check out our privacy policy here