Tests of speech perception have traditionally been used as global measures of performance, particularly in the areas of hearing aid comparison, hearing instrument success, and patient selection for cochlear implants. Unfortunately, the utility of these measures in planning individualized rehabilitation programs or measuring aural rehabilitation program success is limited.
In most cases, the results of rehabilitation are too subtle to be detected in gross measures of improvement in speech perception. New measures of speech perception are now being developed, expanding the utility of speech perception testing through examination of the use of contextual effects and a measurement of meta-linguistic proficiency. It is hoped that these new measures may assist the identification of functional goals and the measurement of program benefit.
Exploring Speech Perception Tests
One of the aims of speech perception testing is to provide some estimate of the level of difficulty that adults with a hearing impairment may have in daily communication. While closed-set perception of nonsense syllables assesses the listener’s acoustic perception, the tests require the listener only to listen for subtle differences between phonemes (eg, /aga/ vs /apa/) and do not require the organization of streams of information into recognizable words or sentences.2 Tests of word perception increase the linguistic content, allowing the listener to use further speech cues and lexical knowledge to determine the identity of the word.
Furthermore, the recognition of words in sentences depends on linguistic context and metalinguistic skills—both of which are important to the perception of speech in conversations. Open-set tests of sentence perception still lack full external generalizability. Communication, which often occurs in the form of sentences, is rarely devoid of external context. Speech is interactive and based on the context of the linguistic environment (ie, the relationship between the preceding utterance and the target utterance).
One difficulty with traditional assessments of speech perception is that they do not reflect the dynamic nature of communication.3 Typically, in a test of sentence perception, the conditions are held constant, each stimulus sentence is presented only once, the listener’s ability varies due to perceptual ability, and responses are scored as percent correct.4 While these testing conditions are reliable and easily standardized allowing for comparison and replication of procedures, they differ from true communication exchanges where sentences are not isolated events and recognition is not reliant solely on perceptual capabilities but rather on the ability to use the linguistic context and environmental cues.
Several authors5,6 recommend the development and use of speech perception tests which better estimate an individual’s communicative competence in real-life situations. Unrelated lists of sentences may underestimate a person’s speech perception capabilities because the lists do not take advantage of the dynamic exchange of information and use of context and environment.3,5 Unfortunately, the transition from open-set tests of recognition of words in sentences to speech perception in the “real world” is too large to control all of the variables influencing intelligibility.7 Hence, the task is to isolate aspects of communication which appear to be important in conversational speech perception for measurement as discrete variables.
First, we need to look at the applicability of traditional speech perception tests in measuring aural rehabilitation outcomes.
Problems in Using Speech Perception Tests for AR Outcomes
Problem 1: Construction. Tests of speech perception are designed to assess the listener’s ability to recognize speech information within the acoustic signal. Unlike other aspects of hearing measurement, such as pure-tone audiometry or tympanometry, there is no procedure or set of calibrated lists that are used universally. Speech perception materials vary in a multitude of ways, including the materials (phonemes, words, or sentences), type of responses (closed-set or open-set), presentation level (dB SPL) or presentation mode (live voice or pre-recorded). While each method has advantages and disadvantages, the objective is to select the test or battery of tests that: 1) meet the needs of the research/clinical question, and 2) are suitable for the participant.
Similarly, speech perception tests have been constructed for a number of different purposes, such as to: assess the degree of impairment caused by a hearing loss8; allow checks to determine the accuracy of the audiogram9; compare hearing aid fittings10-12; provide information about performance before and after a cochlear implant13; assist diagnosis of different types of peripheral and central pathology14; estimate age related decline in performance15,16; assess the adequacy of hearing aid fitting17,18; and provide information about different levels of auditory perception and how they relate to each other.19,20
For any investigation into the nature of speech perception, a careful analysis of the issues needs to be considered to ensure that the required tests match the purposes of the design. Unfortunately, few speech perception tests have been developed for the use of specifically measuring the outcome of an aural rehabilitation program.
Problem 2: Practice effects. We must ensure that the material presented is novel and has not been previously presented to the client. Montgomery & Demorest21 reported that study participants were able to remember the test materials, even when a period of several weeks elapsed between presentations.
One potential solution is to use standardized lists of materials of equivalent difficulty. Despite the use of equivalent lists, a number of researchers report the occurrence of learning effects during speech perception tests.22-24 Therefore, the difference in performance may be due to improving ability rather than differences between situations or devices. Two possible solutions for this problem include randomizing the order of intervention in the design22,24 and providing sufficient training.23 Despite measures taken to reduce practice effects, it is important that measurement is conducted to ascertain if performance was confounded by practice effects. This could be through using unseen practice lists or through testing with similar material each week.
Problem 3: Possible acclimatization. While the comprehensive review of the literature by Turner et al.25 indicated that the acclimatization effect for current hearing aids varies and may not be as large as first thought26,27, it is likely that newer speech processing digital hearing aids may show similar acclimatization effects to multiple-channel cochlear implants.28 Therefore, it is possible that improvements in speech perception observed after fitting hearing instruments could be the result of acclimatization rather than aural rehabilitation.
Problem 4: Test-retest reliability. Tye-Murray29 discussed the issue of test-retest reliability and the problems posed, especially when testing children. For example, variability occurring due to different times in the day, motivational factors, and the inherent high variability within a speech perception test. While in a research setting this can be controlled for by having increased number of materials and participants, it is more difficult to control for in a clinical setting where the time for a practical assessment is usually much shorter.
Problem 5: Performance over time. Often a client’s improvement in conversational fluency over time is not an increase in access to the speech spectrum per se but an improvement in the use of conversational strategies. Therefore, we may see large improvements in conversational fluency (ie, through the participant’s improved use of conversational strategies) which do not result in an improvement in speech perception score.
Problem 6: Are we really testing communication? One of the problems of aural rehabilitation is that we are aiming to improve communication effectiveness or fluency. Unfortunately, we rarely have measures that allow us to examine this area.
Speech perception tests have three main areas that make them difficult to assess real-life communication skills in a meaningful way.30 First, materials are typically presented in unrelated lists of materials consisting often of vowels, consonants, words, or sentences. Second, the client is usually required to repeat verbatim. Third, the tests are rarely interactive. Unfortunately, this model does not resemble real-world communication whereby conversation takes place in a range of environments, speech is contextually based and results in the assembly of new information (as opposed to repetition), and is dynamic.
The remainder of this article will detail four assessments designed for adults with a hearing loss that may provide more information regarding the communication of the individual and, in particular, be suitable to for use in aural rehabilitation programs. They are contextually based, adaptive, interactive, and/or based on conversational measures.
The Effect of Context
Different tests of speech perception can be used to compare performance and gauge the influence of contextual cues. One method of comparison is through the use of probable theory, as proposed by Boothroyd31 and Boothroyd & Nittrouer19, to obtain a quantitative estimate of the facilitative effects of context. This provides more information than reporting the mean difference between scores.
A study by Flynn, Dowell & Clark32 examined the effect of context on speech perception and the interaction of context with background noise. They compared speech perception using standard CUNY sentences33 and the Connected Speech Testv2 (CSTv2)34 at different signal-to-noise levels. Thirty-four adults who had severe-to-profound hearing loss and used hearing aids were tested. As expected, the increase in context available with the CSTv2 sentences is considerable, where the sentences are related not only to a central topic but also to each other. Additionally, contextual processing increased for this population, not only as the test became increasingly based on linguistics, but also as the acoustic conditions deteriorate with background noise. It is important, however, to note that this improvement with context was not uniform. Figure 1 shows clearly that some participants demonstrated large gains in information transmitted with the addition of contextual cues, whereas other participants showed little or no improvement. This variability was independent of pure-tone average and the other speech perception tests.
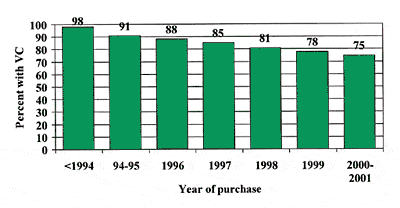
Figure 1. Comparison between CUNY sentences and CSTv2
sentences at +5 dB SNR showing the wide degree of variability
in performance between participants. Participants are ordered
in respect to decreasing PTA. From Flynn & Dowell, 1999.38
The reported variability in performance may reflect differing metalinguistic skills between listeners, which are not assessed using conventional speech perception measures. The difference between traditional and context laden tests of speech perception may be predictive of this ability to adapt and/or cope with a substantial hearing loss. Additionally, this may assist the dispensing professional in determining how well a person will adapt to an amplification device. It may be that people who show a larger no-context/context test difference may be quicker at acclimatizing to a new device. Conversely, people who show little difference between conditions may need extra time allocated in the clinic for acclimatization.
While the addition of context and the evaluation of contextual information provided by different speech perception tests is a move forward in the evaluation of people with a hearing impairment, the test is still not adaptive. It tells us about contextual information but does not tell us what information/cues the person may require in order to fully understand a message.
Adaptive Testing Procedures
The Sent-Ident procedure35 demonstrates the minimum set of cues that a hearing-impaired listener requires for understanding. The utility of this procedure is in the adaptive methodology of the assessment. Over the five different conditions, the sentences are made progressively clearer with more visual cues, allowing a measurement of what level of cues the adult with a hearing loss requires.
In this way, Sent-Indent holds at least four advantages over tests of word and sentence perception.
1. It allows the results to be presented in a way that is more meaningful than a speech perception score, for the participant, family member and care-giving staff. It is not an abstract score. For example, for a patient to obtain 100% of the message when wearing hearing aids, repetition of the sentence may be required. Without hearing aids, the message may need to be presented with audio-visual cues.
2. The assessment and presentation of results in this manner relates directly to aural rehabilitation goals.
3. Sent-Ident can be conducted in the rest home by an audiologist and/or trained staff. It could be possible for trained staff to use Sent-Ident as a method of objectively identifying people who may be in need of aural rehabilitation services. Patients could then be classified according to this information, and then staff could be aware of the minimum amount of cues required to communicate effectively with a resident.
4. The procedures can be adapted to demonstrate other important concepts such as the importance of distance and background noise.
Sent-Ident, therefore, provides one method of assessment of performance of the adult with a hearing impairment that may provide more information than the traditional assessment of word and sentence perception— without losing objectivity. Despite this considerable advantage, Sent-Ident does not take the interactive and contextual nature of conversation into account.
Conversational Interaction within Speech Perception Tests
The majority of communication in the real world involves conversations. Conversations are the way that language is exchanged in a systematic and reciprocal manner.36 It represents the flow of ideas and interaction between two or more people, and as such, is subject to rules and maxims in order to ensure efficiency. Contextual control comes through the use of adjacency pairs.
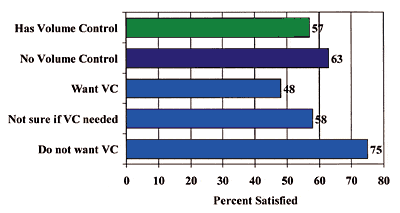
Figure 2. Example scores from the Sent-Ident procedures
for 40 residents of a retirement home, demonstrating the
improvement of performance obtained through hearing
aids. From Flynn et al, 2002.40
An adjacency pair consists of an utterance produced by one speaker that is intended to result in a specific type of response by the listener. Therefore, these utterances have a high degree of facilitative context because the listener gains access to context not just through the sentence form (as in open-set tests of sentence perception), but also through apriori knowledge of the grammatical shape, pragmatic function, and semantic intent of the target utterance. Adjacency pairs may therefore offer great potential in speech perception testing and aural rehabilitation.
Adjacency pairs had been used previously in speech perception tests by Gagne, Tugby & Michaud37 and Erber.5 Both studies showed a clear advantage in the use of the initiating sentence and the use of context. The research of Flynn & Dowell38 expanded the paradigm of Erber5, taking into consideration the effects of related context, disruptive context and neutral context. Flynn & Dowell38 used four different question types: 1) no question, as in a standard speech perception paradigm; 2) a related question; 3) an unrelated question, and 4) a neutral question as shown in the following paradigm:
Reply (target sentence): “He twisted his ankle playing tennis last night.”
- No Question (ie, a standard speech perception sentence paradigm)
- Related: “Why is your brother limping today?”
- Neutral: “Why?”
- Unrelated: “Why didn’t you buy a dog?”
The results demonstrated that in all conditions where there was a preceding question, speech perception significantly improved (p<.05), and increasing the cohesion between the question and the reply further improved speech perception scores.
The potential uses of such a form of assessment include using it as a measure of contextual processing. A gross measurement could be made of a person’s ability to process contextual information and the effects of negative context.
Another perhaps more interesting use was reported by Flynn & Dowell38 in that they showed that adjacency pairs were extracting differences in terms of semantic, grammatical, pragmatics, and auditory priming. Therefore, if perception of adjacency pairs relates to the four aspects of linguistic functioning as suggested, then the assessment and comparison between these different situations may provide important information for aural rehabilitation.
The difference between a good communicator and a poor communicator may relate to one particular aspect, such as the ability to recognize the pragmatic aspects of adjacency pairs. Consequently, aural rehabilitation could focus on this one area of deficiency to provide improvement. Therefore, a speech perception test could provide specific goals for aural rehabilitation instead of the general aim of conversational fluency.
A final use of adjacency pairs could be in the aural rehabilitation program itself. There may be some adults with a hearing loss who do not fully understand or use the facilitative benefit of contextual information in their communication. Adjacency pairs could be used as a method to improve contextual skills and as a practice task to demonstrate the importance of context versus no context.
Despite the benefits of using an interactive test of speech perception, the task is still removed from conversation or real-life speech perception; the listener is required to repeat back exactly what they heard and the nature of the question/answer pair are structured. In this way the participant still does not have control over the fluency of the conversation or access to conversational repair strategies.
Conversational Fluency
In the quest for developing speech perception tests that better represent “real-life” communication, we have focused on how much of the grammatical and syntactic information is received rather than on if the communication exchange was effective. This is ignoring the whole area of conversational fluency. A fluent conversation involves minimal periods of time spent repairing conversation breakdowns, exchange of information and ideas, as well as shared speaking time.
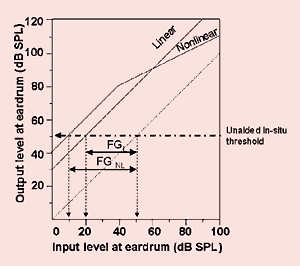
Figure 3. Example of the information provided
by Dyalog software, demonstrating the
information provided.
The difficulty has been how to measure conversational fluency in a way that is robust and representative of real-life experience. For example, tracking success in a task of conversational fluency may vary with the ability of the communication partner, and baseline measures depend on the nature of the material (ie, the topic of conversation). Additionally, how do we measure performance in the clinic? Rarely do communication problems arise in the clinic, because these settings are usually relatively quiet, have low reverberation communication environments, and involve a cooperative communication partner.
Additionally we might be interested in how to define conversation time clinically. Erber39 provided an excellent outline for the types of behaviors that may be of interest. These were:
- Time spent repairing communication breakdown,
- The exchange of information and ideas, and
- Shared speaking time.
Essentially, Erber39 considered a fluent conversation to be one in which clarification time was minimal, ideas were easily exchanged, and speaking time was shared. Tye-Murray29 built upon this framework and suggested that we might want to measure the mean length turn ratio (MLT ratio) whereby a comparison is made between the talker’s mean length of speaking turn (MLT). If these ratios are equal, then it can be said that speaking time was shared. Difficulty arises in how might these be measured in a clinical context. One method might be through the use of the Dyalog computer software developed by Erber.39
Dyalog is one way in which we could objectively measure conversational fluency. The software is relatively simple and can be easily included into the clinical context. The clinician has a conversation, which can be controlled using the TOPICON procedure30, and records the occurrences and time of conversation breakdown and repair by pressing the space bar. Additional variables, such as background noise and speaker type, can also be controlled. Dyalog can then measure (over a set conversation time) the duration of conversation (in seconds) taken by clarification, the proportion of conversation time consumed by clarification, the number of occurrences of clarification, the average time per occurrence of clarification, and the overall duration of the conversation.
Dyalog can then be used to track/create the goals of aural rehabilitation. For example, if the goal of the program is conversational fluency, then one can objectively measure the components of conversational fluency—the amount of time in clarification can be tracked and measured. Presumably the goal of intervention would be to reduce the occurrence of communication breakdowns and the amount of time spent in each episode of communication breakdown.
Alternatively, the goal could, in fact, be the opposite: to increase the amount of time in clarification. For people who bluff and nod their way through conversations, the aim could be for them to use more clarification strategies that are effective and efficient, ensuring that the important information is transferred.
The Future of Speech Perception Tests
Four potential advances or developments in speech perception tests have been explained above: 1) the evaluation of contextual skills in adults with a hearing loss; 2) the use of adaptive measures that manipulate the speech perception task and adjust the difficulty for each person; 3) the use of interactive measures such as the adjacency pairs speech perception test, and 4) the use of software that measure conversational fluency itself in an objective and robust manner.
Speech perception tests still have a valuable and important role to play in any assessment of the client. However, the limitations should be recognized, and valuable effort should be made to ensure that we establish measures that provide an improved assessment in terms of aural rehabilitation. The measurement of assessment and performance in an aural rehabilitation program should ideally consist of a quality-of-life measure, a well-selected measure of speech perception, and a measure that is conversationally based. The overall aim should be to develop a communication profile rather than a speech perception score.
One crucial part omitted from the discussion of speech perception tests is that they should be selected with reference to an overall model of speech perception. There should be a firm clinical and theoretical rationale for why a test needs to focus at the phoneme, syllable, word, or sentence level. It is hoped that, in the future, tests could be selected from a battery of assessments that allow the clinician to target specific areas of auditory processing that can lead directly to amplification solutions or rehabilitation outcomes and/or goals. There has been relatively little discussion on the area of the receptive meta-linguistic skills needed for speech perception.
It should be noted that these measures have not been sufficiently researched, and that these are ideas as to where assessments of communication performance in the hearing impaired should be heading. We are in desperate need to develop tests that are:
- Highly correlated with real-life speech perception capabilities.
- Provide direction in the aims and goals of aural rehabilitation programs;
- Measure the outcomes of aural rehabilitation programs and
- Can predict performance post-implant or hearing aid fitting.
We are on the way to achieving these goals. More than 30 years ago, James Jerger made a call to action: “…we are, at the moment, becalmed in a windless sea of monosyllables. We can only sail further on the fresh winds of imagination.”1 Hopefully, we will soon be able to answer this call.
Acknowledgments
The information in this article was originally presented at the International Adult Aural Rehabilitation Conference held in Portland, Maine, in May 2001. (The Second Intl. Adult Aural Rehabilitation Conference will be held in Portland, Maine, on May 5-8; for information, contact Geoff Plant at the Hearing Rehabilitation Foundation: (617) 628-4537.) The ideas presented here are based on the assistance and help of a variety of many people, including Professor Richard Dowell and Dr. Norm Erber. Traci Schmidtke of Oticon A/S provided valuable feedback on an earlier copy of this paper.

|
Correspondence can be addressed to Mark C. Flynn, PhD, Oticon A/S, Strandvejen 58, 2900 Hellerup, Denmark; email: [email protected].
References
1. Jerger J. Research—Present status and needs. In: Proceedings of the Inst. Aural Rehab, University of Denver, 1968.
2. Tye-Murray N, Witt S, & Castelloe J. Initial evaluation of an interactive test of sentence gist recognition. Jour Amer Acad Audiol. 1996; 7:396-405.
3. Erber NP, Lind C. Communication therapy: Theory and practice. In: Gagne JP, Tye-Murray N, eds. Research in Audiological Rehabilitation: Current Trends and Future Directions. Jour Acad Rehab Audiol. 1994; [Monograph] 27:47-66.
4. Erber NP. Communication Therapy for Hearing Impaired Adults. Melbourne, Australia: Clavis Publishing; 1988.
5. Erber NP. Adaptive assessment of adult sentence perception. Ear and Hear. 1992;13:58-60.
6. Gagne JP. Visual and audiovisual speech perception training: Basic and applied research needs. In: Gagne JP, Tye-Murray N, eds. Research in Audiological Rehabilitation: Current Trends and Future Directions. Jour Acad Rehab Audiol. 1994; [Monograph] 27:133-159.
7. Pollack I, Pickett JM. Intelligibility of excerpts from fluent speech: Auditory versus structural content. Jour Verbal Learning and Verbal Behavior. 1964;3:79-84.
8. Mendel LL, Danhauer JL. Audiological evaluation and management and speech perception assessment. San Diego: Singular Publishing Group;1997.
9. Lloyd LL, Kaplan H. Audiometric interpretation: A manual of basic audiometry. Austin, TX: Pro-Ed;1978.
10. Feeney MP, Franks JR. Test-retest reliability of a distinctive feature difference test for hearing aid evaluation. Ear and Hear. 1982; 3:59-65.
11. McDaniel M, Cox RM. Evaluation of the speech intelligibility rating (SIR) test for hearing aid comparisons. Jour Speech and Hear Res. 1992;35:686-693.
12. Walden BE, Schwartz DM, Williams DL, Holum-Hardegen LL, Crowley JM. Test of the assumptions underlying comparative hearing aid evaluations. Jour Speech Hear Disorders. 1983;48:264-273.
13. Waltzman S, Hochberg I. Perception of speech pattern contrasts using a multichannel cochlear implant. Ear and Hear. 1990;11:50-55.
14. Olsen WO, Noffsinger D, Kurdziel S. Speech discrimination in quiet and in white nose by patients with peripheral and central lesions. Acta Otolaryngol. 1975;80:375-382.
15. Gordon-Salant S. Age-related differences in speech recognition performance as a function of test format and paradigm. Ear and Hear. 1987;8:277-282.
16. Humes LE, Watson BU, Christensen LA, Cokey CG, Halling DC, Lee L. Factors associated with individual differences in clinical measures of speech recognition among the elderly. Jour Speech Hear Res. 1994;37:465-474.
17. Byrne D, Parkinson A, Newall P. Hearing aid gain and frequency response requirements for the severely/profoundly hearing-impaired. Ear and Hear. 1990;11:40-49.
18. Byrne D, Parkinson A, Newall P. Modified hearing aid selection procedures for severely/profound hearing losses. In: Studebaker GA, Bess FH, and Beck LB, eds. Vanderbilt Hearing-Aid Report II. Parkton: York Press; 1990.
19. Boothroyd A, Nittrouer S. Mathematical treatment of context effects in phonemes and word recognition. Jour Acoust Soc Amer. 1988; 84:101-114.
20. Rabinowitz WM, Eddington DK, Delhorne LA, Cuneo PA. Relations among different measures of speech reception in subjects using a cochlear implant. Jour Acoust Soc Amer. 1992;92,1869-1881.
21. Montgomery A, Demorest M. Issues and developments in the evaluation of speech reading. Volta Review. 1998;90:119-148.
22. Skinner MW, Clark GM, Whitford LA, Seligman PM, Staller SJ, Shipp DB, Shallop JK, Everingham C, Menapace CM, Arndt PL, Antogenelli BA, Brimacomb JA, Pijl S, Daniels P, George CR, McDermott HJ, Beiter AL. Evaluation of a new spectral peak coding strategy for the Nucleus 22 channel cochlear implant system. Amer Jour Otology. 1994;15 (Suppl 2):15-27.
23. Theodoridis GC, Schoeny ZG. Procedure learning effects in speech perception tests. Audiology. 1990;29: 228-239.
24. Whitford LA, Seligman PM, Everingham CE, Antogenelli T, Skok MC, Hollow RD, Plant KL, Gerin ES, Staller SJ, McDermott HJ, Gibson WR, Clark GM. Evaluation of the Nucleus Spectra 22 processor and new speech processing strategy (SPEAK) in postlingually deafened adults. Acta Otolaryngol (Stockh). 1995;115, 629-637.
25. Turner CW, Humes LE, Bentler RA, Cox RM. A review of past research on changes in hearing aid benefit over time, Ear and Hear. 1996;17:14s-28s.
26. Gatehouse S. The time course and magnitude of perceptual acclimatization to frequency responses: Evidence from monaural fitting of hearing aids. Jour Acoust Soc Amer. 1992;92:1258-1268.
27. Gatehouse S. Role of perceptual acclimatization in the selection of frequency responses for hearing aids. Jour Amer Acad Audiol. 1993; 4:296-306.
28. Tyler RS, Summerfield AQ. Cochlear Implantation: Relationships with research on auditory deprivation and acclimatisation. Ear and Hear. 1996;17:38s-50s.
29. Tye-Murray N. Foundations of Aural Rehabilitation. San Deigo: Singular Press; 1998.
30. Erber NP. Communication therapy for Hearing-impaired Adults. Melbourne: Clavis; 1996.
31. Boothroyd A. Measurement of speech production in hearing-impaired children: Some benefits of forced choice testing. Jour Speech Hear Res. 1985;28:185-196.
32. Flynn MC, Dowell RC, Clark GM. Adults with a severe-to-profound hearing impairment. Investigating the effects of linguistic context on speech perception. Proceedings of the 5th International Conference of Spoken Language Processing, 1985: SL980121:1-4.
33. Boothroyd A, Hanin L, Hnath T. A sentence test of speech perception: reliability, set equivalence, and short term learning. In: Internal report RCI 10. New York: City University of New York;1985.
34. Cox RM, Alexander GC, Gilmore C, Pusakulich KM. Use of the connected speech test (CST) with hearing-impaired listeners. Ear and Hear. 1988;9:198-207.
35. Erber NP. Effects of a question-answer format on visual perception of sentences, Jour Acad Rehab Audiol. 1992;25:113-122.
36. Myllyniemi R. Conversation as a system of social interaction. Language & Communication. 1986;6:147-169.
37. Gagne JP, Tugby KG, Michaud J. Development of a speechreading test on the utilization of contextual cues (STUCC): Preliminary findings with normal hearing subject. Jour Acad Rehab Audiol. 1991;24: 157-170.
38. Flynn MC, Dowell RC. Speech perception in a communicative context: An investigation using question/answer pairs. Jour Speech, Lang Hear Res. 1999;42:540-552.
39. Erber NP. Dyalog Computer Program. Available at: http://parrotsoftware.com. Accessed: March 18, 2003. Parrot Software, 1996.
40. Flynn MC, Kennedy EK, Johns J, Stanbridge R. Hearing and vision loss within residential care facilities – the need for improved service delivery. Australasian Jour Ageing. 2002;21:142-145.