Opinion | January 2016 Hearing Review
A statistical look at the wide range of European hearing aid reimbursement systems
Among the various reimbursement schemes for hearing aids in Europe, is one system more efficient than the others? Today, we have new sources of information that may help to answer this question. This study of seven European countries based on data from EuroTrak 2012 and the Market Study of Western Europe 2011 provides a perspective by longtime industry observer and hearing aid specialist Luis Godinho.
Using the US MarkeTrak studies as a model, the European Hearing Instrument Manufacturers Association (EHIMA)1 has undertaken surveys of the hearing aids market in Europe. After an initial program in 2009 covering the three largest markets in Europe, Germany, the United Kingdom, and France, the surveys were renewed in 2012 and extended to Japan as well as four additional European countries, Norway, Switzerland, Italy, and Denmark.2 The strict methodology used for these studies, carried out by the Swiss market research firm Anovum (www.anovum.com/en), has made this information source a reference in the field, with results used by the public authorities, for example in France by the Ministry of Health in August 20143 or in Belgium by the Ministry of the Economy in December 2014.4 In addition, Tony Grant-Salmon, former chairman of the British Hearing Aid Manufacturers Association and former president of Knowles Europe, regularly publishes the Market Study of Western Europe. This study lists the different types of hearing aids and annual sales volumes in the large countries of Western Europe.5,6
Sales and Reimbursements of Hearing Aids in Several European Countries (2011)
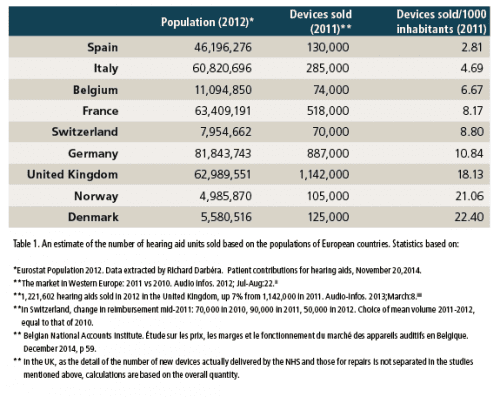
Calculating the number of devices sold per 1,000 inhabitants provides easy comparison. Table 1 and Figure 1 provide a look at hearing aid sales in three groups of countries:
- Southern Europe, with Spain and Italy, which show the lowest levels of sales, despite much higher reimbursement in Italy for certain patients,
- Continental Europe, with Belgium, France, Germany, and Switzerland, which show medium-range sales levels,
- Northern Europe, with the UK, Norway, and Denmark, where the highest levels are recorded.
It is clear that sales are not proportional to reimbursements since Belgium has an amount similar to that for Switzerland, but sales are significantly lower, and France is relatively well placed in sales despite very low healthcare system reimbursements for adults.
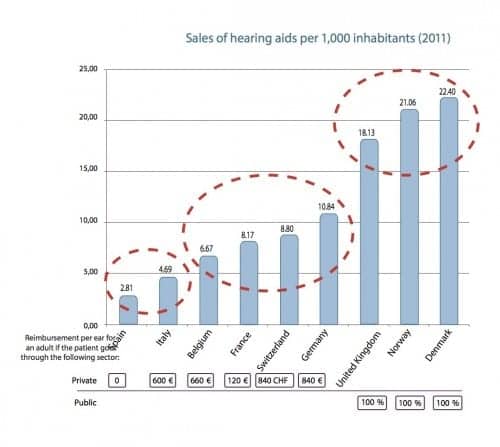
Figure 1. Number of hearing aid units sold per 1,000 people (Table 1). Private/public data on bottom show the amount of reimbursement per ear as cited in Amplifon’s 2013 Annual Report (p 35).
Number and Fitting Rate for European Countries (2011)
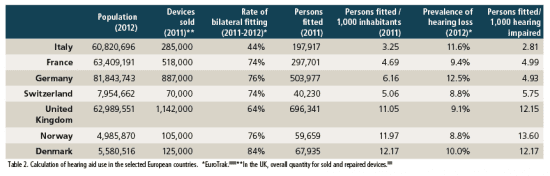
On the basis of rates for bilateral fitting and data on the prevalence of hearing loss collected by EuroTrak,1,2 we can calculate the percentage of people with hearing loss fitted in 2011 for the seven countries under study (Table 2 and Figure 2).

Figure 2 (top). Number of people fitted with hearing aids per 100 hearing-impaired people in the population (see Table 2). Figure 3 (bottom). Percentage of hearing aid users versus the total number of hearing-impaired people in each country as measured by EuroTrak + JapanTrak 2012.2
Of note are the low level of bilateral fittings in Italy (44%) and the mid-range level of binaural fittings in the UK (64%). All the other countries have a rate between 74% to 84%.
Since the prevalence of hearing impairment increases with age, the two countries with the oldest populations, Germany and Italy, logically have the highest rates of hearing-impaired people.
Percentage of Users versus the Total Number of Hearing-impaired People Measured by EuroTrak in 2012
When looking at Figure 3, Denmark has an exceptional rate of fitting at 47.8%. This country of 5.6 million inhabitants is unique in that it is home to 3 of the 6 multinationals that manufacture hearing aids worldwide—a factor that can only promote acceptance and maximum penetration of hearing devices.
The level of fitting in Denmark is therefore the world reference and is close to the maximum level of “fittable” persons: 50% to 60% of persons who report hearing impairment. This is because not all people with hearing impairment benefit from hearing aids, for various reasons including hyperacusis, very minor deficits, certain types of tinnitus, etc.
In 2009, a European study commissioned by the public authorities in France found “a rate of fittable persons of 50% of the total hearing impaired population” in the five countries studied.7 The Swedish association for the hearing impaired, Hörselskadades Riksförbund (HRF), found that 56% of people with hearing loss could benefit from hearing aids.8 In 2013, the French Inspectorate General of Social Affairs (IGAS) worked with a similar ratio: “2.5 to 3 million fittable persons”9 in France of a total of about 6 million people with hearing loss.
The level of fitting in the United States remains moderate, on a par with rates in Italy, the lowest among the studied European countries.
Concerning satisfaction of the hearing impaired in Japan, the rate is particularly low at only 36%, while the seven European countries studied by EuroTrak show an overall satisfaction rate of between 70% and 84%.2 The level of fitting is also the lowest in Japan: 14.1%. These figures should be put into perspective given the lack of public regulation in Japan concerning supply of hearing aids, which results in high numbers of low-range products supplied without the choice, fitting, and follow-up provided by professionals: “18% of users acquired their hearing aids at an optician, and 14% through mail order or on the internet.”10 According to European Hearing Instrument Manufacturers Assn (EHIMA) Secretary General Søren Hougaard, “This shows that “non-professional” hearing health services lead to a lower customer satisfaction rate.”11
In the area of hearing impairment, it is clear that, without initial medical diagnosis and personalized care by a professional, there is no efficiency, nor patient satisfaction. This was the conclusion that the US Food and Drug Administration (FDA) came to back in 2009: “While these personal sound amplifiers may help people hear things that are at low volume or at a distance, the Food and Drug Administration (FDA) wants to ensure that consumers don’t mistake them—or use them as substitutes—for approved hearing aids.”12
The FDA’s advice is also clearly stated regarding from where to obtain hearing aids: “We recommend that patients with hearing loss go to a hearing healthcare professional (for example, an audiologist or a hearing aid dispenser), as appropriate, for a hearing assessment and hearing aid evaluation. We also recommend that a person with hearing loss have a medical evaluation by a licensed physician (preferably one who specializes in diseases of the ear, such as an otolaryngologist) when purchasing a hearing aid. The hearing healthcare professional will assess the person’s ability to hear sounds and understand others with and without a hearing aid(s) and select and fit a hearing aid(s) to the person’s individual communication needs.”13
By comparing Figures 2 and 3, the difference in the number of fitted persons in 2011 between continental Europe and the countries of Northern Europe appears to a far lesser extent in the results of the fitting levels measured by EuroTrak. This rate is for all users, regardless of the year when they were fitted. As a result, if the change in rate of fitting, an increase throughout the sample, differs from one country to the next, this could lead to variations that we will not take into account in this analysis. Nonetheless, the group Italy-France-Germany-Switzerland on the one hand, and the UK-Norway-Denmark group on the other, show consistent results. We can therefore ask why the major difference in devices supplied each year in Northern Europe versus the other countries does not show up in their levels of fitted population.
“Compliance Index” and Rate of Overall Satisfaction
Therapeutic compliance is “the way in which a person complies with medical prescriptions or rules in a treatment program.”14 In the area of hearing devices, this could be defined as actual use of the hearing device effectively supplied. By dividing the rate of users measured by EuroTrak by the percentage of devices supplied, on the basis of data in the Market Study of Western Europe and Eurostat demographic data, it is possible to determine a “compliance index” concerning hearing aids. The higher the compliance index, the more the devices supplied will promote effective use of hearing aids in a higher number of people (Table 3).
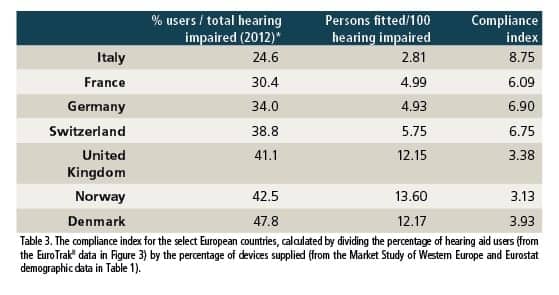
Considering the data in Table 1 and the differences between the UK and France—in terms of prevalence, bilateral fitting levels, and population—if the UK had a compliance index like that of France (6.09), it would have been enough to supply 634,422 devices in 2011 to reach its rate of users of 41.1%.* However, we can see that 1,142,000 devices were dispensed in 2011 in the UK. (*41.1 ÷ 6.09 = 6.75% of fitted hearing impaired; ie, 6.75 × 62,989,551 × 0.091 ÷ 100 = 386,843 fitted persons.)
Is the Compliance Index Proportional to User Satisfaction?
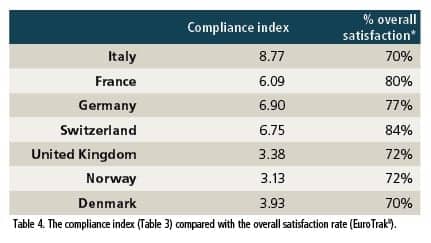
We have overall satisfaction rates for the seven countries through EuroTrak 2012 data (Table 4 and Figure 4). With the exception of Italy, Figure 4 shows the considerable correlation between the compliance index and overall satisfaction.
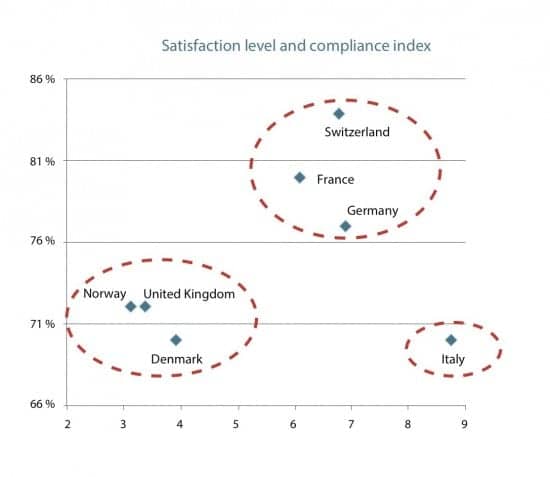
Figure 4. The seven European countries graphed as a function of the compliance index (x-axis) and overall satisfaction rate with hearing aids (y-axis).
As with the level of fitting, the rate of overall satisfaction measured by EuroTrak is that of all the users, regardless of the year of fitting, with a level of satisfaction that increases for more recent devices. The increase in the satisfaction rate found in all countries indicates that the margin of error is low, with the consistency of results for the studied countries supporting this conclusion.
Author’s note: Median renewal times are concentrated around 5 years (Italy and Denmark: 4 years; Switzerland, France and UK: 5 years; Germany and Norway: 6 years), and concern less than half the users for all countries. The effect on the results is therefore limited.
Italy. The high compliance index goes hand-in-hand with a low level of bilateral fitting (44% versus 75% as a mean for the six other countries studied), as mentioned above. The result is a lower rate of satisfaction (70%) compared to the seven countries and on a par with Denmark—confirming the need for bilateral fitting when necessary, as demonstrated in many studies.
Denmark, Norway, and the United Kingdom. These three countries have very similar results: the low compliance index may indicate that a large number of devices supplied with no patient contribution are not actually used by the patients. They also have a relatively low satisfaction level, between 70%-72%.
Germany, France, and Switzerland. For this group, the results are also consistent: the compliance index is high (6.09-6.90), as is the satisfaction rate (77%-84%). Logically, when most patients use their devices, satisfaction is high. This results in a virtual circle enabling fitting of a larger proportion of the population with a lower number of hearing aids. These countries appear to have a system that is more efficient.
Inelastic Demand to Price, and an Operator-dependent Satisfaction Rate
It may appear surprising that the best results are obtained in the countries where the cost is only partially covered by the system, leaving some patient contribution (including the system in France that requires almost 1,000 Euros per ear for an adult).15
In short, demand for hearing aids is relatively inelastic to price.16 The General Inspectorate for Social Affairs in France (IGAS), responsible for evaluating public policies for the Ministry of Health, indicates that hearing aids are not “a consumer item…but a device aimed at compensating and also preventing loss of autonomy.”9 The report “Hearing aids in Belgium” points out that “it is important to understand that demand is relatively inelastic to price, since hearing aids are seen as a basic necessity.”17
Also in the United States, it has been found that “simply lowering the cost of hearing aids—even by as much as 40%—does not improve hearing aid purchase…Even the best hearing aid on the market won’t help if it is not fitted properly by an expert.”18
Hearing care professionals must adapt to “complex” patients and provide devices that patients are reluctant to obtain as a result of psychological obstacles, fear of stigma, etc, and for which the benefits may not be fully perceived until several days or even weeks after the start of use. The distribution phase cannot only be considered as a simple distribution process; it is more a question of adapted and personalized service. Fitting hearing aids involves a number of appointments with the patient (eg, hearing tests, manufacture of the earmold or shell, adjustments) then, after supplying the device, follow-up over several years to ensure an appropriate fitting and to perform regular personalized adjustment throughout the lifetime of the device.
France’s Inspection Générale des Affaires Sociales (IGAS) states that “no professionals other than hearing aid specialists are competent to carry out these recommendations, testing, and support steps. The choice of the device is therefore left in the hands of the hearing aid specialist and can only be checked by a professional with the same skills.”9
Links between hearing impairment and loss of autonomy
- Hearing loss is associated with cognitive decline.19 For mild hearing loss (25 dB), the decrease in cognitive performance is equivalent to that of a person 6.8 years older.20
- The risk of dementia is multiplied by 1.89 for moderate hearing loss, by 3.00 for mild loss, and by 4.94 for severe loss.21 Elderly people with hearing loss have an acceleration of cognitive decline greater than 30% to 40%.22 Non-compensated hearing loss causes a decrease in quality of life related to isolation, a reduced social life, and a feeling of exclusion, leading to increased prevalence of depression.23,24
- Even a moderate degree of hearing loss almost triples the risk of falls in elderly patients.25
- At the 37th Congress of French hearing care professionals in Paris (April 10-12, 2015), Prof Hélène Amieva from the French National Institute for Health and Medical Research (INSERM) in Bordeaux, France, made an exclusive presentation of her ongoing study. Her findings26 show that cognitive decline is clearly accelerated in people with hearing impairment versus a control group, while cognitive decline in people with hearing aids is slowed and is similar to that of people with normal hearing. “These results support diagnosis and rehabilitation of hearing deficits,” according to Dr Amieva.
- A moderate hearing loss (25 dB) is therefore sufficient to double the risk of cognitive decline and to triple the risk of falls in elderly subjects. These results speak in favor of rehabilitation starting from a moderate hearing loss of 25 dB. Health economics studies show that the cost of non-treated hearing loss is much higher than the cost of hearing aids.27,28
With an aging population in Europe, good quality management of hearing loss is a public health priority in order to limit the increasing number of dependent individuals.
Highly “Operator-dependent”
Fitting hearing aids is a highly “operator-dependent” profession in which hearing aid specialists do not “sell the devices” but charge for their expertise for selection and fitting, and for their time to train the patient on use of the device and regular personalized follow-up, as often as the user deems necessary. This leads to better functioning in countries where patients can freely choose a professional who will select and adjust the device, and ensure all necessary follow-up.
This is the case in Germany, Switzerland, and France. Professionals are in competition with one another, and users more often turn to those who have the best reputation, often based on advice from medical practitioners or other patients. Thus, specialists are driven to follow up with patients, helping improve overall satisfaction due to “competition through quality.”
In the United Kingdom, there also appears to be a willingness to increase patient freedom. This policy is known as Any Qualified Provider (AQP) and broadens the choice for patients. It will be interesting to monitor changes in the compliance index and overall satisfaction over time in view of this new possibility offered to patients.
What is the Most Efficient Reimbursement System in Europe?
The IGAS studied the various management systems in Europe and found that “Two analysis criteria make it possible to understand the various systems for payment of technical devices in Europe: the higher the amount remaining as a patient contribution to acquire hearing aids, the higher their level of choice; on the contrary, the higher the public level of reimbursement, the more restricted patients are in their choice.”9
In our sample, the countries of Northern Europe (Denmark, Norway, and the National Health Service in the UK) opted for a system of controlled supply, with a limited choice of devices and of professionals, and no contribution left to the patient. In Switzerland and France, the authorities placed a ceiling on the amount of reimbursement but allowed complete freedom for the patient to choose their healthcare professional and the characteristics of their hearing aids.
Germany is in an intermediate situation where the patient’s contribution and freedom to choose a professional are in the middle of the range, since patients can opt for a basic hearing aid with limited possibilities and no patient contribution, or choose higher-level devices while paying the difference.
Analysis of the overall satisfaction rate and the compliance index are in favor of the model that provides for the greatest freedom for patients—both for the type and technical level of the hearing aid—and for the healthcare professional who will fit the device and provide patient training and regular follow-up over time. This remains true even if the patients need to assume part of the cost (with the exception of the population that has the lowest income and requires specific offers, depending on income, with no patient contribution).
It would appear the most efficient scheme therefore needs to include:
- Rehabilitation starting from moderate hearing loss of 25 dB;
- The same amount of reimbursement irrespective of the patient’s age or cause of hearing loss (congenital, acquired, accidental, occupational, etc);
- Complete freedom for the patient to choose their professional to promote “competition by quality”;
- Choice by the patient of their hearing solution, taking into account their hearing loss, their wishes, the financial contribution they wish to make, with the expertise and advice of a specialist in hearing solutions;
- Independence of the professional in the choice of the best solution for their patient in terms of private funders and manufacturers;
- Systematic choice, adjustment, supply, and follow-up by the same professional;
- Flat-rate reimbursement by the public healthcare system with known periodicity, facilitating access to a quality hearing solution, enabling the patient to select more sophisticated devices if desired, and leaving the price difference to the patient (except for patients with the lowest income);
- Reliable patient information, from a public source, so that the patient can promote “competition by quality.”
Areas for Improvement in Hearing Aid Reimbursement in Select Countries
Italy. One of the priorities for Italy would be to bring the rate of bilateral fitting (44% in 2012) up to the mean of the other countries (75%). It would also be beneficial to implement a flat-rate for hearing aids from 25 dB of hearing loss irrespective of the cause (occupational deafness, presbycusis, etc).
Denmark, Norway, and the United Kingdom. With AQP, the United Kingdom has broadened possibilities for patients (see above). More generally, enabling the patient to choose their hearing care professional and their hearing solution should be promoted in these three countries.
Reimbursement of a flat-rate to the patient (including for care through retail in the United Kingdom), with the freedom to choose a more sophisticated device and to pay the difference in price, should also be considered in order to improve the compliance index and overall satisfaction.
Germany. The obligation for professionals to offer patients a solution with a cost between 685-800 Euros per ear covered by insurance, with no contribution from the patient—meaning a flat-rate twice as high as it was before 2014—could lead to lower satisfaction levels than those found in Switzerland and France. (Studies by GfK show that less than 5% of devices cost less than 800 Euros per ear in France; Switzerland has a product mix that is similar to that found in France.) The fact that this obligation exists may lead patients to believe that this offer is sufficient for satisfactory results. We should remember that about one-third of patients choose this solution despite the results obtained with devices that have very limited capabilities. Abandoning this obligation would enable patients to use their flat-rate reimbursement for solutions that are more qualitative, with the aim of achieving greater satisfaction.
France. The main problem is the very low level of reimbursement: 120 Euros for the public system and 350 Euros on average for optional complementary healthcare insurance. About 1,000 Euros per ear on average remain to be paid by adult patients, and this amount prevents patients with low income from accessing hearing aids. As a result, people with hearing impairment in France are left with a disability that has unknown and underestimated consequences, and leaves the country with an imbalanced system of access to hearing rehabilitation.
This low level of reimbursement may even suggest to patients that it is not particularly useful or important to rehabilitate hearing loss. Improving public healthcare reimbursement is a priority and should make it possible to move closer to the fitting levels found in the countries that have satisfactory reimbursement in place.
Switzerland. With the highest satisfaction levels of the studied countries, excellent results in fitting levels and the compliance index, Switzerland has the best overall results.
The Swiss public authorities must be made aware of the major public health impact of hearing impairment, the fact that it is impossible for competition law to be the only regulator of the sector, and the significant operator-dependent nature of hearing care professionals who fit hearing aids. Fitting of hearing aids must therefore be strictly limited to qualified professionals to avoid a decrease in the overall satisfaction among patients. (Author’s note: Initial results of the EuroTrak 2015 studies were presented on April 10, 2015 at the Congress of Hearing Professionals held in Paris. They concern only Switzerland and France. The overall level of satisfaction in Switzerland changed from 84% to 81% between 2012 and 2015.)
European Competition Law in Health and Public Payment of Care
“The specificity of healthcare prohibits competition law from becoming the only regulator.”29
In 1963, Kenneth Arrow established the economic nature of healthcare activities and drew attention to “the asymmetry of information between the consumer of services and the professional offering these services.”29 This implies demand that is “not very sensitive to changes in price,” even when these markets are open. “Since determining state of health is difficult and subjective…care is considered to be credence goods…The relationship of trust that develops between the supplier and customer prevents behaviors of pure negotiation, and adjustment through prices.”29
Asymmetry of information, reputation, trust, and inelastic demand to prices are all criteria that are found in the area of rehabilitation of hearing impairment. “Competition through prices” translates into a reduction of the time spent with the patient. Therefore, “diminished” personal support leads directly to lower satisfaction. Satisfaction is correlated with support time, needed for initial patient training and follow-up by a professional.30 “Mechanisms of competition cannot function as in other markets without running the risk of altering the quality of products and healthcare services. This is why competition law, if it is to govern this area, cannot do it alone. State intervention remains the rule in a sector that is poorly harmonized across the European Union.”29
High concentration of the need for hearing aids among persons over age 65 (in France, 75% of costs are concentrated on people ages 65+)31 and the proven role of rehabilitation of hearing loss in the prevention of loss of autonomy further reinforce the need to include payment of hearing aids in the range of care reimbursed by public healthcare systems in Europe.
Moving to the Next Level
Through the EuroTrak studies, EHIMA provides data that improves our understanding of the hearing aid sector. It would be useful to extend these studies to other countries, particularly Spain, the Netherlands, and Belgium. Hopefully, all the countries scrutinized by EuroTrak in 2012, will be included in the 2015 study! Learning more about the product mix in the various countries would also help improve analysis of the various sectors.
Once all the data are available from the EuroTrak 2015 studies and the Market Study of Western Europe 2014, it will be possible to study changes in the compliance index and level of satisfaction since this study. The results, both in terms of compliance and satisfaction rates, are extremely close in Denmark, Norway, and the UK. However, important differences in the share between the public and private markets can be observed from one country to another. Specific data should be collected in order to perform an in-depth analysis of each type of reimbursement system in these three countries. Also, consideration should be given to the possibility of refining results by accounting for differences between the existing coverage and prescription habits in said countries.
Acknowledgements
A version of this article originally appeared in the November 2015 edition of Audio infos and is republished here with permission.32 The author thanks Brice Jantzem, hearing instrument specialist, and Richard Darbéra, chairman of the Bucodes-Serdi France Association for the Hearing Impaired for their review and contributions to this article.
References
-
Hougaard S, Ruf S. EuroTrak I: A consumer survey about hearing aids. Hearing Review. 2011;18(2)[Feb]:12-28. Available at: https://hearingreview.com/2011/10/eurotrak
-
Hougaard S, Ruf S, Egger C. E EuroTrak + JapanTrak 2012: Societal and personal benefits of hearing rehabilitation with hearing aids. Hearing Review. 2012;20(3):16-26. Available at: https://hearingreview.com/2013/03/eurotrak-japantrak-2012-societal-and-personal-benefits-of-hearing-rehabilitation-with-hearing-aids
-
Haeusler L, De Laval T, Millot C. Étude quantitative sur le handicap auditif à partir de l’enquête «Handicap-Santé». Apr 29, 2014:59. Available at: http://www.drees.sante.gouv.fr/etude-quantitative-sur-le-handicap-auditif-a-partir-de-l,11341.html
-
Belgian National Accounts Institute. Étude sur les prix, les marges et le fonctionnement du marché des appareils auditifs en Belgique. December 2014. Available at: http://economie.fgov.be/fr/binaries/Etude_Appareils_auditifs_tcm326-261094.pdf
-
Grant-Salmon T. The market in Western Europe 2011 vs 2010. Audio infos. 2012;July-Aug.
-
Grant-Salmon T. The European hearing aid market. Audio infos. 2013;81[Sept]:20-23.
-
Caisse nationale de solidatité pur l’autonomie (CNSA). Étude européenne sur le marché et les prix des aides techniques. Synthèse Aides Auditives. 2009;Dec:4. Available at: http://www.cnsa.fr/documentation/synthese_transversale.pdf
-
Strömgren J-P. Høorselskadades Riksførbund. Available at: http://www.csc.kth.se/utbildning/kth/kurser/DH2625/itfunk-h07/schema/hrf.pdf
-
Blanchard P, Strohl-Maffesoli H, Vincent B. Évaluation de la prise en charge des aides techniques pour les personnes âgées dépendantes et les personnes handicapées [report of the Inspection Générale des Affaires Sociales (IGAS)]. April 2013. Available at: http://www.igas.gouv.fr/spip.php?article331
-
Anovum. JapanTrak 2012. Available at: http://ivo.ehima.dev02.accedo.dk/wp-content/uploads/2014/03/JapanTrak_2012.pdf
-
FranceEuroTrack 2012 Japan: a very mixed picture. Audio infos. 2013;No 181[Mar].
-
US Food and Drug Administration (FDA). Hearing Aids and Personal Sound Amplifiers: Know the Difference, October 20, 2009. Available at: http://www.fda.gov/ForConsumers/ConsumerUpdates/ucm185459.htm
-
US Food and Drug Administration (FDA). How to get hearing Aids. June 11, 2014. Available at: http://www.fda.gov/MedicalDevices/ProductsandMedicalProcedures/HomeHealthandConsumer/ConsumerProducts/HearingAids/ucm181479.htm
-
Académie de Médecine. Medical Dictionary. Available at: http://dictionnaire.academie-medecine.fr/?q=Observance
-
Syndicat Natinoal des Audioprothésistes (UNSAF). Les synthèses de l’Unsaf. Available at: http://www.unsaf.org/site/l-unsaf/les-syntheses-de-l-unsaf.html
-
Amlani AM. How patient demand impacts pricing and revenue. Hearing Review. 2008;15(3):16,18-19. Available at: https://hearingreview.com/2008/03/how-patient-demand-impacts-pricing-and-revenue
-
Federaal Kenniscentrum voor de Gezondheidszorg (KCE). Hearing aids in Belgium: Health technology assessment [KCE reports 91C]. 2008:iv. Available at: https://kce.fgov.be/sites/default/files/page_documents/d20081027369.pdf
-
Ramachandran V, Stach B, Becker E. Reducing hearing aid cost does not influence device acquisition for milder hearing loss, but eliminating it does. Hear Jour. 2011;64(5):10-18. Available at: http://journals.lww.com/thehearingjournal/Fulltext/2011/05000/Reducing_hearing_aid_cost_does_not_influence.3.aspx
-
Uhlmann RF, Larson EB, Rees TS, Koepsell TD, Duckert LG. Relationship of hearing impairment to dementia and cognitive dysfunction in older adults. JAMA. 1989;261(13):1916-1919.
-
Lin FR, Ferrucci L, Metter EJ, An Y, Zonderman AB, Resnick SM. Hearing loss and cognition in the Baltimore Longitudinal Study of Aging. Neuropsychol. 2011;25(6):763-270.
-
Lin F, Metter E, O’Brien R, Resnick S, Zonderman A, Ferrucci L. Hearing loss and incident dementia. Arch Neurol. 2011;68(2):214-220.
-
Lin FR, Yaffe K, Xia J, Xue QL, Harris TB, Purchase-Helzner E, Satterfield S, Ayonayon HN, Ferrucci L, Simonsick EM. Hearing loss and cognitive decline on older adults. JAMA Intern Med. 2013 Feb 25;173(4):293-9. doi: 10.1001/jamainternmed.2013.1868
-
Mener DJ, Betz J, Genther DJ, Chen D, Lin FR. Hearing loss and depression in older adults. J Am Geriatr Soc. 2013 Sep;61(9):1627-1629. doi: 10.1111/jgs.12429
-
Arlinger S. Negative consequences of uncorrected hearing loss–a review. Int J of Audiol. 2003; 42:2S17–2S20. Available at: http://www.ncbi.nlm.nih.gov/pubmed/12918624
-
Lin FR, Ferrucci L. Hearing loss and falls among older adults in the United States. Arch Intern Med. 2012;172:369-371.
-
Viljanen A, Kaprio J, Pyykkö I, et al. Hearing as a predictor of falls and postural balance in older female twins. J Gerontol A Biol Sci Med Sci. 2009; 64(2):312-317.
-
Shield B. Evaluation of the social and economic costs of hearing impairment. A report for HEAR-IT. October 2006. Available at: http://www.hear-it.org/sites/default/files/multimedia/documents/Hear_It_Report_October_2006.pdf
-
Ciorba A, Bianchini C, Pelucchi S, Pastore A. The impact of hearing loss on the quality of life of elderly adults. Clin Interv Aging. 2012;7(6):159–63. doi: 10.2147/CIA.S26059
-
L’Autorité de la Concurrence. Droit de la concurrence et santé. 2008 Annual report. Available at: http://www.ladocumentationfrancaise.fr/rapports-publics/094000296
-
Kochkin S. Reducing hearing instrument returns with consumer education. Hearing Review. 1999;6(10)[Oct]:18-20.
-
Syndicat Natinoal des Audioprothésistes (UNSAF). Hearing impaired primarily among the elderly. Available at: http://www.unsaf.org/site/l-unsaf/les-syntheses-de-l-unsaf.html
-
Godinho L. What is the most efficient reimbursement scheme in Europe? Audio infos. 2015; Oct [EUHA issue]:19-26. Available at: http://www.unsaf.org/doc/What_is_the_most_efficient_reimbursement_scheme_in_europe.pdf
Luis Godinho is a hearing aid specialist in Paris, President of the French Union of Hearing Aid Professionals (UNSAF), and member of the Haut Conseil pour l’Avenir de l’Assurance Maladie (HCAAM).
Correspondence can be addressed to Hearing Review or Luis Godinho at: [email protected]
Original citation for this article: Godinho L. What Is the Most Efficient Reimbursement System in Europe? A statistical look at the wide range of European hearing aid reimbursement systems. Hearing Review. 2016;23(1):16.?






A very interesting article. I’m in the UK and wear a pair of Oticon NHS hearing aids for mild/moderate hearing loss (at 47 my audiogram looks like that of the average 80-year-old for reasons unknown.)
My thoughts on increasing hearingaid uptake and satisfaction.
1) The NHS must blow its own trumpet – every GP’s surgery needs a poster encouraging people of all ages to get their hearing tested and showing pictures of the modern, small colorful hearing aids they actually supply today. Mine are cute and purple (having a choice was weirdly important) and in no way resemble the things my grandmother needed, but never had.
2) NHS needs to continue working with private suppliers so we do not have to go to large, very busy, County hospitals for hearing aid fittings and follow up appointments.
3) Hearing screening, everyone should be offered a hearing test from 60 years old, if not before. When people are aged 75 or 80 and have stopped going to many of their outside interests, it’s way too late.
I had no choice, but to do something. I need to hear in meetings and I get grief for the TV deafening my teen daughters. If you’re 80 and live alone or with a elderly partner whose hearing is a bit ropey too, there’s much less motivation.
Sadly, although I love the idea, reimbursement towards private aids would not work in the UK.
It’s rumored the NHS bulk buys hearing aids for ~£90 and I can’t conceive the Government parting with more than £100-200, which is off a £1000+ totally pointless.