By Mona Dworsack-Dodge, AuD
I still remember participating in my first Mayo Clinic Audiology Conference some 15 years ago. As a graduate student, I thought our profession was so forward thinking, even futuristic. I was proud to participate as a student and was even more proud when I later found myself doing my clinical fellowship year at a host site. Little did I know then how far we would progress over a relatively short period. Flash forward to 2013, a time when video-conferencing, web-conferencing, and distance learning in general have become standard means for audiology education.
As for audiology and dispensing practices, we now live in a world where a hearing care professional sitting in one location can log onto a remote computer and hardware to deliver calibrated speech to a patient sitting hundreds (or even thousands) of miles away. While this may sound exotic, or even irrelevant, when compared to the day-to-day needs of your practice, it is important to think about ways in which this new reality can be leveraged to better serve your patient population—and make you more efficient.
The Department of Veterans Affairs and Teleaudiology
Teleaudiology has been defined as the use of electronic information and telecommunications technologies to support remote and distance clinical hearing healthcare, professional and public education, public health matters, and health administration.1 The Department of Veterans Affairs (VA), a leader in delivery of telehealth services, describes three discrete areas of telepractice:
- Clinical video telehealth (CVT): Real-time video-conferencing to assess, treat, and provide care to patients at a distant location.
- Home telehealth (HT): Video and mobile devices to monitor and manage patients (at home) with acute and chronic disease.
- Store and forward telehealth (SFT): Uses technologies to acquire and store clinical information (eg, data, image, sound, and video) that is then forwarded to or retrieved by a provider at another location for clinical evaluation or interpretation.
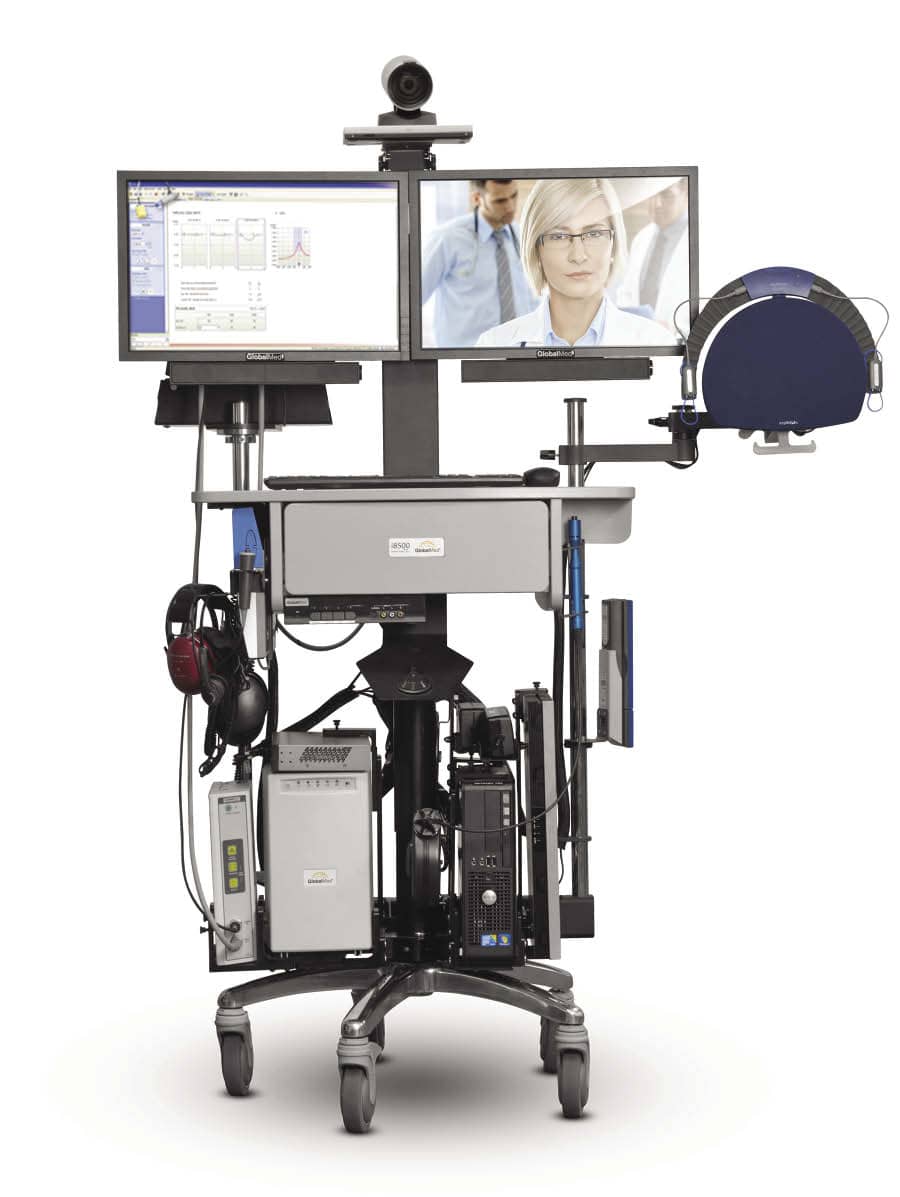
Borne from a need to provide better access to care for veterans in rural areas, the VA established over 800 community-based outpatient clinics (CBOCs) to alleviate long travel times and provide veterans closer care to their homes.2 In 2011, the VA initiated a pilot program to establish the feasibility of remote hearing instrument programming and verification at 10 CBOC locations (Figure 1). Details regarding challenges and opportunities identified in this pilot program are outlined by Dennis et al2 in the October 2012 special edition of The Hearing Review guest-edited by Jerry Northern, PhD.
|
| Figure 1. Example of a teleaudiology solution (as configured for VA pilot sites) featuring front of Otometrics’ Madsen Astera, Madsen Otoflex, AURICAL PMM, and AURICAL HIT. |
This multi-phased project was designed to take teleaudiology practice using clinical video telehealth from concept to routine care delivery, with the goal of achieving similar outcomes obtained through teleaudiology versus traditional care delivery models.
Dennis et al2 point out that, despite the complexities of implementing such a program, making hearing care accessible with equivalent outcomes outweighs associated challenges.
But What’s in It for Me?
I can hear readers saying “It all sounds great, but why and how do I translate these remote services into my daily work?” This is especially true if you do not have access to all the resources marshaled by the Department of Veterans Affairs.
The “why” is simple. Teleaudiology is the way forward for our profession. We are challenged to find ways to differentiate ourselves and to draw consumers into our practices. Northern1 points out that embracing technology to provide hearing healthcare from a distance may be the saving grace for the future of our profession. He cites the demand for convenience for delivery of services of all kinds and routine application of face to face electronic conversations as driving forces.
Furthermore, Swanepoel et al3 explain that the need for audiology services worldwide exceeds our current capacity to deliver these services. They highlight various opportunities in the areas of education/training, screening, diagnosis, and intervention.
The solutions for “how” are also surprisingly accessible. Store and forward teleaudiology is already in play for most of us, as electronic health/medical records (EHR/EMR) become required for billing and reimbursement. Computer-based, integrated instrument solutions (video-otoscopy, acoustic immittance, audiometry, otoacoustic emissions, counseling and simulations, probe microphone measurements, hearing instrument test devices) that communicate with EMR are also standard of care.
When considering professional issues surrounding teleaudiology, one can reference the basic guidelines from the American Academy of Audiology4 and American Speech-Language-Hearing Association.5
The following are a few opportunities to put teleaudiology into your hands and clinic.
1) Skype and FaceTime: Good for More Than Letting Grandma Visit with the Grandkids
Instrument manufacturers have used tools like PC Anywhere, Log-me-in Rescue, WebX, and Office Communicator for clinical and technical support for years. As mobile devices become prevalent, Skype and FaceTime have become meaningful tools that add tremendous value and enhance customer support.
Skype and FaceTime in particular are widely used by and easily accessible to our patient populations. One of these or a similar platform can serve as a simple medium for you to get started. Routine follow-up to new hearing instrument fittings and basic aural rehabilitation can easily be delivered through these means. Doing so saves the patient a trip and your waiting room is freed up for in-person encounters.
It’s worthwhile to seek not only your patient’s e-mail address, but also their Skype handle or other mode of contact. Initiate the dialogue by asking how they would like to receive follow-up services, and consider making video chat one option. Using remote media (even e-mail!) as a means to provide routine care frees up your clinic schedule, yet still allows you to deliver a high level of patient care.
2) Video Otoscopy (VO): Thinking Outside the Ear Canal
|
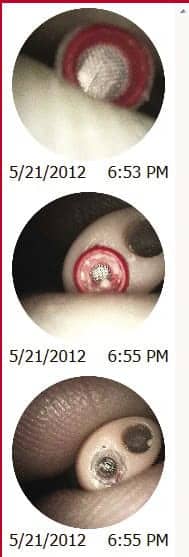
| Figure 2. Still images taken with a video otoscope to show inspection of HI receivers for cerumen. |
Traditional use of VO has been well documented as a store and forward tool, which is comparable to in-person examination.6 It’s worth noting that VO is also a versatile tool that lends itself to counseling on the use and placement of hearing instruments, battery, inspection of receivers or wax guard replacement, etc (Figure 2). All of these topics and more can be conducted using VO, either in-person or via remote sessions.
In fact, video otoscopes today are often designed with teleaudiology in mind. Some devices use standard Windows drivers, which allow for the use of the VO camera using virtually any web-conferencing software.
3) Remote HI Programming
Much attention has been given to remote programming of hearing instruments both in the literature2,7 as well as in audiology blogs.8 In fact, practical step-by-step instructions can be found on blog sites for remote programming of hearing instruments and mapping of cochlear implants.9
While this may not be suited for all programming demands, consider some of your more routine sessions that are resolved with minimal adjustments. Routine and easy for sure, but they eat up valuable appointment time. Freeing up this time is beneficial for not only professionals but also for patients who may not be freely and independently mobile—and may well serve to promote consistent amplification use. Ask your patients; you might be surprised to hear the answer.
4) Participate in the Progress
The formation of the Tele-Audiology Network (http://tan.geoaxon.co.za) has created opportunities for clinicians to volunteer time to conduct and evaluate hearing tests remotely.3 Seeking out opportunities to volunteer your professional services provides an easy way for you to try it out. Perhaps you might even be inspired with new ways to differentiate your clinic from others.
A Glimpse at the Future of Dispensing…
Ear scanning technology is poised to transform the way we deliver hearing aid services, custom swim plugs, and hearing protection, rendering most silicone ear impressions obsolete. Dispensing professionals will be able to capture a full digital 3D image of both the ear canal and the concha, then transmit the electronic image to the appropriate instrument manufacturer as easily as sending an e-mail (Figure 3). The transmission time for this is less than 2 minutes. In addition to time savings, this process will eliminate shipping costs and the margin of error involved in generating silicone impressions today.

|
| Figure 3. Workflow diagram for digital imaging of the ear to custom mold production and delivery. (click to enlarge) |
3D ear scanning technology will become a standard of care, and represents another breakthrough in store-and-share telehealth technology. In the same way that Hi-Pro standardized the way we program hearing aids in the 1990s, ear scanning technology has the potential to revolutionize the way thousands of impressions are made every day. Once the 3D scan is made, it is available on file. If a remake is needed, the clinician and earmold lab or hearing aid manufacturer can review the file simultaneously to identify areas of modification required, without the need to redo the scan.
Ear scanning technology is forecast to become commercially available in 2014. Enthusiasm at AudiologyNOW 2013 indicates that attendees would like to use this technology within the next 2 years. If this is any indication of adoption rates, most readers of this article will likely make use of 3D ear scanning technology, and thus become active participants in the next wave of telehealth in audiology.
Are You Ready?
Technology will continue to advance. How ready are you to incorporate these changes for better patient care? Making your services more accessible will increase the visibility of our industry and your practice to those who need you.
As you can see from the examples above, present and future tools offered by telehealth do not replace the unique care provided by competent and dedicated hearing care professionals. Rather, with informed and careful implementation, these methods allow us to expand our reach and supplement our capacity to provide that care for people seeking our services. They also provide a tool for us to address the impending shortage of hearing healthcare professionals. In light of these factors, it seems that there is little not to like about telehealth finding its way into your daily practice.

|
Mona Dworsack-Dodge, AuD, is Director of Audiology Services for GN Otometrics North America in Schaumburg, Ill.CORRESPONDENCE can be addressed to Dr Dworsack-Dodge at: [email protected] |
References
1. Northern JL. Extending hearing healthcare: Tele-audiology. Hearing Review. 2012;19(10):12-16.
2. Dennis KC, Gladden CF, Noe CM. Telepractice in the Department of Veterans Affairs. Hearing Review. 2012;19(10):44-50.
3. Swanepoel D, Clark JL, Koekemoer D, et al. Telehealth in audiology–The need and potential to reach underserved communities. Int J Audiol. 2010;49:195-202.
4. American Academy of Audiology (AAA). The use of telehealth/telemedicine to provide audiology services [2008]. Available at: http://www.audiology.org/advocacy/ publicpolicyresolutions/Documents/TelehealthResolution200806.pdf
5. American Speech-Language-Hearing Association (ASHA). Audiologists Providing Clinical Services via Telepractice: Technical Report [2005]. Available at: www.asha.org/policy
6. Kokesh J, Ferguson AS, Patricoski C, et al. Digital images for postsurgical follow-up of tympanostomy tubes in remote Alaska. Otolaryngol Head Neck Surg. 2008;139:87-93.
7. Galster J, Abrams H. Are you ready for remote hearing aid programming? Hearing Review. 2012;19(10):26-28.
8. Cooling G. Tele-Audiology: A threat or an opportunity? Available at: http://justaudiologystuff.com/index.php/tele-audiology-a-threat-or-an-opportunity
9. Schwartz D. Telehealth for programming hearing aids and MAPping CI’s [2013]. Available at: http://thehearingblog.com/archives/1274#Step-by-step instructions