Inside the Research | April 2018 Hearing Review
Todd Ricketts, PhD, is a professor and vice chair of Graduate Studies at Vanderbilt University Medical Center and director of the Dan Maddox Hearing Aid Research Laboratory. Prior to his work at Vanderbilt, he spent 3 years as an assistant professor at Purdue University. He is also the past-editor of Trends in Amplification, and the current associate editor for the Journal of Speech, Language and Hearing Research. Although his research interests are wide-ranging, they usually involve aspects of amplification and how we can improve the overall listening experience of individuals with hearing loss. Ricketts, along with co-authors Ruth Bentler, PhD, and H. Gustav Mueller, PhD, published in January the textbook Essentials of Modern Hearing Aids: Selection, Fitting, and Verification.1 We thought this would be a good time to catch up with him.
Beck: Good morning, Todd. I have to say congratulations on publishing what is very likely to become the most prominent textbook in audiology and hearing aid dispensing. Seriously, this is an excellent text. I would recommend this book for all doctoral students in audiology, and it would be an excellent book for any hearing care professional (HCP) to get in sync with 2018 hearing aid-fitting protocols, concepts, and what is needed to know to excel in an increasingly competitive marketplace.
Ricketts: Thanks Doug, that’s very kind of you. Speaking on behalf of my co-authors and friends Drs Bentler and Mueller, we appreciate your endorsement!
Beck: My pleasure. Now, the ground rules for this interview are sort of loose. I intend to jump around quite a bit, going from topic to topic at the speed of sound.
So let’s start with an unfortunate and uncomfortable reality—by which I mean our profession’s lack of compliance with AAA or ASHA best-practice protocols.2,3 I recently interviewed our mutual friend and your co-author Dr Mueller (July 2017 Hearing Review),4 and he suggested that perhaps only one-third of all HCPs bother to perform verification, validation, and probe-mic measures, all of which are critically important components of best practices. So then, what are your thoughts on this pivotal issue?
Ricketts: You’ll recall the paper Sergei Kochkin, you, and about a dozen well-respected co-authors published almost 10 years ago (April 2010 Hearing Review),5 which stated that whether the dispenser was an audiologist or not was often more-or-less irrelevant with regard to outcomes and hearing aid fitting practices. What mattered most—as measured by patient satisfaction—was adherence to best practices; the more closely the HCP aligned with best-practice protocols, the higher the patient satisfaction level, regardless of the HCP’s clinical knowledge or degree. The fact that someone is highly trained and may know quite a lot about hearing aid dispensing, doesn’t mean they do everything they were supposed to do in the real world with real patients, and that’s a huge problem.
Beck: Yes. I recall many of our colleagues being quite upset by those findings, but if you look at the authors and read the article in detail, those were not lightly drawn conclusions.
Ricketts: Right, and so it’s clear to me that we need to implement best practices based on evidence-based outcomes. We all understand that it’s a personal choice. One can do a great job or a mediocre job dispensing; there’s usually nobody looking over your shoulder…but isn’t that the definition of integrity? What you do when nobody’s looking?
Nonetheless, I have to question the decision-making of those who choose to dispense based on first fits and tweak the fitting based on “how does that sound?” Our text references a number of studies that demonstrate weak protocols lead to inferior patient outcomes.
Beck: I wonder if you would review one of the pragmatic examples from the book, as to why we need to always acquire probe-mic measures.
Ricketts: Sure. This isn’t verbatim, but Dr Mueller offered a scenario which goes something like this. Imagine Mr and Mrs Smith come to see you. She’s a tiny woman, just under 5 feet tall and about 96 pounds. Her husband is quite the opposite: 6’8” and 265 pounds. They each get a hearing test and, amazingly, they have exactly the same audiogram.
If we place the same thresholds in the first-fit software, we’ll get the same prescribed gain and output. However, her ear canal volume might be less than half of his. For example, his could be 2.7 cc and her’s 1.1 cc, and if that’s the case—and going back to Boyle’s Law in undergraduate physics—the SPL in his ear canal will be much less because his ear canal volume is so much larger. Conversely, the SPL in her ear will be much higher because her ear canal is relatively tiny. So, given the same audiogram and the same first-fit recommendation, he may lose audibility for soft speech, and she may be more likely to perceive high-level sounds as uncomfortably loud.
Beck: Let’s totally change topics and take a look at the demographics in 2018, because you seem to have the most current numbers. So, how many hearing-impaired people are there in the United States, and what percentage of them acquire hearing aids and are binaurally fit?
Ricketts: I suspect that if we use the audiogram by itself and estimate that there are 325 million people in the USA, we could guess a hearing loss prevalence of about 10-12%, giving a total of some 35-38 million people who have hearing loss. The numbers are hard to nail down because the criteria changes over time and multiple scales have been used. Further, when we speak about hearing loss per an audiogram, we’re probably leaving out many people with auditory neuropathy spectrum disorder (ANSD), synaptopathy, and multiple other listening disorders.
But let’s go with 35 million. From there, we state that research indicates only about one-third of those perceive their hearing loss as troublesome enough to seek a diagnosis or a solution. So that means only about 10-12 million people might attempt to seek a solution via an HCP, and this might represent the “actual total population pool.”
Of course there are new people who join the pool, and people who exit the pool, but for now, it seems about 3.75 million hearing aids are dispensed professionally in the USA. Of those, some 700,000 hearing aids are dispensed through the VA, and given that perhaps 80% of all fittings are bilateral, we only have about 1.6 or 1.7 million people who buy hearing aids annually.
Beck: Which, at first blush, seems remarkably low. Yet, if we have 35 million people with hearing loss, and only about one-third of them believe their problem is substantial enough to seek a solution, that gets us to 12 million people. So then, given that well-maintained, high-quality hearing aids often last 5 to 6 years or more (and those not well-maintained may only last 2 or 3 years) it seems reasonable that, of the 12 million people in the “actual total population pool” who replace or acquire hearing aids every 5 or 6 years, about 2 million people buy hearing aids annually—which pretty much agrees with your numbers.
All of which speaks to the issue that simply having hearing loss as demonstrated on an audiogram does not mean you want or need hearing aids. Likewise, having a “normal” audiogram also doesn’t necessarily mean you wouldn’t benefit from an increased signal-to-noise ratio to make it easier to focus on the primary signal.
Ricketts: Exactly. The go or no-go decision to get a hearing aid is based on multiple factors including a listening needs’ assessment and a complete audiometric evaluation—and it all starts with the patient accepting they might have a real hearing problem. Enhancing hearing aid success for patients requires a professional hearing aid evaluation, probe-mic measures, pre- and post-fitting assessments, troubleshooting, appropriate counseling throughout the entire process, and much more. You recently covered many of these same issues with Michael Valente, PhD (December 2017 Hearing Review),6 so we don’t need to revisit all of it. However, the point is pure-tone thresholds are important, but optimized hearing aid fittings are based on many factors beyond the audiogram, such as the patient’s speech recognition-in-noise ability, their acceptable noise limits, and more—which are not predicted by, or correlated with, the pure-tone audiogram.
Beck: Todd, let’s change the subject again. What can you tell me about the relationship between hearing impairment and cognition?
Ricketts: I think that if we consider untreated hearing loss in an older adult, there is real opportunity for it to exacerbate cognitive and dementia issues. The relationship between hearing loss and cognitive decline is significant in many people—this has been demonstrated across multiple studies. However, one has to be careful to recognize correlation, which does exist between hearing loss and cognitive decline and dementia, versus causation. There is a statistically significant correlation, but that does not mean every person with hearing loss develops dementia or suffers cognitive decline due to untreated hearing loss.
So we have to be careful when we interpret the science and when we talk to patients about these issues. Of course, in addition to talking about the negatives associated with untreated hearing loss, we should also address the benefits associated with amplification: increased social interactions, higher income levels, increased overall health, enhanced relationships and intimacy, better control over life’s events, and more, all of which we review in detail in the book.
Beck: Fair enough. New topic…As a musician, I can recall looking at the specs on the old TDK, Maxell, and BASF cassette tapes, and I recall so many of my colleagues paying more for the better tapes because they had a flat response out to 40,000 Hz. But as an audiologist, it occurs to me that humans can only perceive 20-20,000 Hz. Further, at either end of the spectrum, we’re talking about more than 120 dB SPL to perceive the sounds. And so, at normal conversational levels, the real useful speech and music spectrum (if faithfully reproduced) is maybe 40-12,000 Hz. Is that correct?

Beck: My musician friends are usually whacko about this, and I’ve stopped trying to convince them. Some say they can hear the difference in recordings which go out to 15 or 20 kHz. I say “Pepsi Challenge.”
Nonetheless, some readers will be relieved to learn that modern hearing aids have a bandwidth of 10 to 12,000 Hz. In fact, I might point out that middle C on a piano is about 256 Hz, and given an 88-key piano, some 70% of all fundamental frequencies are below 1,000 Hz, whereas with speech sounds, about 70% of all speech sounds are above 1,000 Hz.7 So, in general, one could actually say that music is a low-frequency event, whereas speech is more or less a high-frequency event.
Ricketts: I agree that once you get past 10 kHz, there’s not a lot of sound energy to be had—even if you are listening to live symphony orchestra performances. Consequently, it is not that surprising that audible output bandwidth for hearing aid wearers with significant hearing loss is commonly limited to below 8 kHz or less (sometimes much less).
Beck: And, although I clearly recall the Bell Labs’ studies8 from Murray Hill, New Jersey, which determined the bandwidths for telephones should be about 300 to 3,400 Hz, I was kind of shocked to read in your book that smartphones have roughly the same spectral response?
Ricketts: Yeah, that’s pretty interesting, right? But then again, there’s “HD Audio” too, which is voice over IP (VoIP) frequency extension; so, there are smartphones that, when connected to other capable smartphones, offer an enhanced high-frequency (VoIP) response. These can be found in newer smartphones from Samsung, iPhone, and other high-end brands. For me, this extended bandwidth greatly improves sound quality. But I have normal hearing. If you have hearing loss which prevents you from perceiving the available and transmitted high frequencies, it may not sound that different at all! However, the extended low frequencies (below 300 Hz) can have an even greater effect on sound quality than extended high frequencies.
Beck: So these particular HD phones have a wider bandwidth available, via your data package, to capture and transmit more spectral information?
Ricketts: Yes, and if you can perceive it, it might be worth it. But keep in mind that low-energy Bluetooth and other wireless systems, including telecoil, limit your bandwidth. Typically, those systems have bandwidths that are less than 6-8 kHz, but they often sound great to patients with the right coupling!
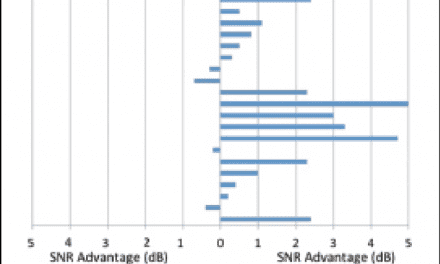
Beck: OK, and oddly enough, in my mind this is analogous to real-world measures from directional microphones. That is, although the directivity index (DI) may be 5 or 6 dB—which is derived with a closed-canal fitting in an anechoic chamber using a KEMAR [mannequin] listening to pure tones—in the real world, the directional benefit is often only 1 or 2 dB, or maybe 3 dB in an excellent fitting, as some 85% of all hearing-aid fittings are open-canal fittings.
Ricketts: Yes, I have to agree, 1-3 dB is fairly typical, and your numbers are reasonable approximations of reality. In general, you might expect half the DI to be realized in the real world, although variability is vast across technologies, patients, coupling, and fitting strategies. However, it should be emphasized that those 1-3 dBs can make a big difference in speech understanding.
Beck: Let’s move on to the issue of word recognition score (WRS). This very basic measure of hearing is often grossly misunderstood, and you and your co-authors did a fantastic job reviewing the numbers in the new book. Specifically, please explain the statistically significant differences which need to occur for one WRS to be significantly different from another. I know many people have written about this,9 and the first reference I recall was the binomial model by Thornton and Raffin10 in the late 70s. But you’ve got a few other references—all of which agree that WRS’, for the purpose of hearing-aid fittings, are simply not a very good measure.
Ricketts: Exactly. Relative to the clinic, this is a very interesting issue, and I think many HCPs are glossing over some things when it comes to WRS. If you’re using recorded 25-item word lists, (please don’t tell me if you’re using live voice!) the hearing loss is symmetric, and if the first score is 48% correct, anything between 24-72% is the same score statistically. Likewise, given a first score of 68%, anything between 44-88% correct is statistically the same, and finally, given 92% correct score on the first ear, anything between 72-100% is the same. And, of course, using the 50-word lists would reduce the range of “same scores” across all data points.
Beck: What are your thoughts on real-ear-to-coupler-difference (RECD) measures for adults and children?
Ricketts: Well, nobody would argue that RECD measures would decrease fitting accuracy or make fittings less acceptable. RECDs also allow for accurate verification of prescriptive gain and output targets in children and uncooperative adults. An additional use of the RECD is for the calculation of an actual threshold in an individual’s ear, rather than one based on a RETSPL. This improves accuracy of threshold estimates and, in turn, prescriptive gain targets.
The primary issue for the typical adult patient is that RECD measures take time, but generally not more than a few minutes for experienced clinicians familiar with the software and the protocol. The DSL advocates in Western Ontario have sometimes argued for this RECD use in adults.11 Of course, one can build a rational argument, but I’m not sure I see that happening as a regular part of clinical practice in the foreseeable future.
However, for me, it’s a simple matter of how accurate do you want to be? Probe-mic measures and adjustments take just a few minutes, and some adjustments are automatic and probably the same can be said for RECD. But in the final analysis, if a patient is paying several thousands of dollars for an excellent product dispensed by an expert—a device they will wear 10 to 14 hours daily for many years—the 5-15 minutes added to the protocol to assure the most accurate fitting possible seems like a good investment.
We believe this is important, even though we will often make minor adjustments based on patient input. As many studies looking at prescriptive gain have shown, the starting point matters!
Beck: Do you believe that speech-in-noise (SIN) tests are useful clinically?
Ricketts: Yes, I think this is pretty clear by the amount of ink we spend on this topic in the textbook! SIN tests need to be incorporated in the test battery because SIN results may very clearly impact the fitting, the choice of technology, realistic expectations of the patient and the HCP, the counseling and aural rehabilitation approach, and more.
However, it is important to understand that these tests and how they are given are not all equivalent. So the HCP using these measures has to be cautious and ensure they are comparing apples to apples, and to make sure the protocol they’re using has the desired clinical and day-to-day life applicability.
Beck: OK, Todd. Although I could ask your thoughts and opinions all day, I know I need to let you run. Thanks very much for the work you, Ruth, and Gus did on this book—again, I believe it is among the very best textbooks written on audiology and hearing aids.
Ricketts: Thanks Doug. I’ll look forward to seeing you at the AAA Convention in Nashville.
References
-
Ricketts TA, Bentler R, Mueller HG. Essentials of Modern Hearing Aids Selection, Fitting, and Verification. San Diego: Plural Publishing;2018.
-
Valente M. Guideline for audiologic management of the adult patient. October 30, 2006. Available at: https://www.audiologyonline.com/articles/guideline-for-audiologic-management-adult-966
-
American Speech-Language-Hearing Association. Guidelines for hearing aid fitting for adults. 1998. Available at: https://www.asha.org/policy/GL1998-00012/
-
Beck DL. Speech mapping and probe microphone measurements: An interview with Gus Mueller, PhD. Hearing Review. 2017;24(8):38-39. Available at: https://hearingreview.com/2017/07/speech-mapping-probe-microphone-measurements-interview-gus-mueller-phd
-
Kochkin S, Beck DL, Christensen LA, et al. MarkeTrak VIII: The impact of the hearing healthcare professional on hearing aid user success. Hearing Review. 2010;17(4):12-34. Available at: https://hearingreview.com/2010/04/marketrak-viii-the-impact-of-the-hearing-healthcare-professional-on-hearing-aid-user-success
-
Beck DL. Best practices in hearing aid dispensing: An interview with Michael Valente, PhD. Hearing Review. 2017;24(12):39-41. Available at: https://hearingreview.com/2017/11/best-practices-hearing-aid-dispensing-interview-michael-valente-phd/
-
Revit L. What’s so special about music? Hearing Review. 2009;16(2):12-19. Available at: https://hearingreview.com/2009/02/whats-so-special-about-music
-
Miller GA, Licklider JCR. The intelligibility of interrupted speech. J Acoust Soc Am. 1950;22(2):167–173.
-
Chasin M, Chasin C. Cutting short a word list: What are the chances for error? Hearing Review. 2007;14(10)[Sept]:52-56. Available at: https://hearingreview.com/2007/09/cutting-short-a-word-list-what-are-the-chances-for-error/
-
Thornton AR, Raffin MJM. Speech-discrimination scores modeled as a binomial variable. J Sp Hear Res. 1978;21(3):507-518.
-
Glista D, Hawkins M, Moodie S, Scollie S. Understanding how RECDs fit into the “big picture” of hearing aid fitting. Hearing Review. 2016;23(3):26-31. Available at: https://hearingreview.com/2016/02/understanding-recds-fit-big-picture-hearing-aid-fitting/
Original citation for this article: Beck DL. Real-ear, cognition, speech-in-noise, and more: An interview with Todd Ricketts, PhD. Hearing Review. 2018;25(4):24-26.
Correspondence can be addressed to Dr Beck at:
[email protected]
About the author: Douglas L. Beck, AuD, is Executive Director of Academic Sciences at Oticon Inc, Somerset, NJ. He has served as Editor In Chief at AudiologyOnline, and Web Content Editor for the American Academy of Audiology (AAA). Dr Beck is an Adjunct Clinical Professor of Communication Disorders and Sciences at State University of New York, Buffalo. He also serves as Senior Editor of Clinical Research for the Hearing Review’s Inside the Research column.




![An Evidence-Based Systematic Review on Cognitive Interventions for Individuals With Dementia [Review]](https://hearingreview.com/wp-content/themes/Extra/images/post-format-thumb-text.svg)