
|
| 3-year-old Zuri Boucad contracted bacterial meningitis in May 2008, leaving both cochlea severely damaged. |
It all started with a sniffle. “It looked like a little cold,” recalls Nicole Boucad, a native of the Republic of Trinidad and Tobago, and the mother of 3-year old Zuri, who awoke one morning this past May with a runny nose.
A lively, charming, and irrepressible child, Zuri soon developed a high fever, became somnolent and droopy-eyed, and 2 days later was rushed to the hospital, where she was diagnosed with bacterial meningitis. A week later, while she was still hospitalized, Zuri’s father, Dion, noticed that she was not responding to loud noises. An audiologist determined that there was severe hearing loss and that both cochlea had been damaged, a characteristic result of the disease.
“In the space of a week,” says Nicole, “Zuri’s world went silent.”
The Boucads could not have imagined the dramatic odyssey that would ensue from that little sniffle. Although they received excellent care for Zuri at the public hospital at Mt Hope, Trinidad, and they are extremely grateful that she suffered no other long-term effects from the infection, there was little treatment available in their country for damaged cochlea and profound hearing loss.
“Both the audiologist and ENT specialist agreed that she would do well with cochlear implants,” recounts Nicole. The implants would allow Zuri to hear again—not the same way as before, but she would be able to recognize sounds, speech, and music. Hearing aids would not help because the deafness was too profound, the degree of amplification needed too great.
But the Boucads were faced with some major obstacles. The procedure was not only unavailable in their homeland, but also very expensive. The implant device itself costs $65,000 for each ear (more than $300,000 Trinidad-Tobago dollars), and surgical, hospital, and required follow-up care for 1 year would run the bill to about $90,000 per ear.
“The cost boggled our minds,” said Nicole, not to mention the added expense of having to travel to another country. A publications manager at the University of the West Indies Trinidad campus, she and Dion, a freelance videographer, couldn’t come near to affording the procedure, and as she had only recently begun her new position, there was as yet no health insurance. Even with insurance, cochlear implants are not covered in that Caribbean nation.
Also, there was the time factor. Meningitis produces ossification in the inner ear, and an MRI confirmed that bone was starting to grow. Obstructive calcification generally takes place within 2 months of the infection, and the procedure then becomes virtually impossible.
Yet, despite the daunting circumstances, the Boucads had faith that things would somehow work out. It was time for a miracle, and they were ready to do whatever they could to make that miracle happen for their beloved daughter.
It started with an e-mail about Zuri that they put out to everyone they knew on the island. One of their friends, Sonja Dumas, responded that she knew a doctor in the United States, someone she had once worked with in Trinidad, who was now at the New York University Medical Center, and she believed he worked in the area of cochlea implants. As it turned out, that doctor, Devon John, MD, did not specialize in hearing, but he knew another doctor at NYU who did.

|
| J. Thomas Roland, Jr, MD |
That physician, J. Thomas Roland, Jr, MD, became a pivotal figure in the dramatic course of events that was to follow. Director of otology/neurotology at the NYU Medical Center, as well as associate professor of otolaryngology and neurosurgery and co-director of the NYU Cochlear Implant Program, Roland was highly qualified from a medical standpoint, but it was other qualities he possessed—namely, concern and compassion for those unable to afford such costly procedures—which brought about the eventual culmination of what had appeared to be an impossible dream.
Roland’s philosophy is simple and compelling: “If there’s a need, it’s hard to deny care. I felt in this and other similar situations that it was the right thing to do.”
Roland donated his services as Zuri’s surgeon—just as he had done before for a Palestinian boy, a Guatemalan girl, a young man in Uganda, and a woman in Guam. But in this case he went further, contacting Advanced Bionics, the only American company pursuing the development and manufacturing of cochlear implants. With the cooperation of CEO Al Mann (founder of the philanthropic Mannkind Foundation) and president and co-CEO Jeff Greiner, and with the further assistance of Advanced Bionics’ Ethics and Donations Committee, Roland was able to have one of their Harmony cochlear implant devices donated free of charge.
Roland also worked with the Special Cases Committee at NYU Medical Center, under the leadership of director Maria Corbo, to drastically reduce hospital charges to a level that the Boucads, as a result of a grassroots fund-raising campaign they had undertaken, were able to manage.
The procedure, says Roland, is “an example of a new era of providing this kind of high-technology care in places where the supportive infrastructure doesn’t exist. These smart and active kids will have a chance to be mainstreamed, get a full education, and have careers of their own some day, which might not have happened if they had stayed in the world of deafness.”
As for the effectiveness of a cochlear implant, Roland explains that “Normal hearing is very complex—implants can’t reproduce all the subtleties and complexities. You’re essentially replacing 28,000 neuron cells, each with multiple neuron connections, with 16 electronic contacts.”
However, while not reproducing normal hearing entirely, the implant does improve hearing well enough to allow the patient to develop language and speech skills that would otherwise be difficult, if not impossible, to achieve. “Also, the device can create up to 120 additional virtual channels through complicated paradigms that will stimulate 10 to 1,000 neurons, still not nearly as much as the normal ear, but progress in the right direction.”
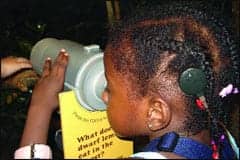
|
| Shortly following her successful cochlear implant surgery in New York, Zuri enjoyed a visit to the Bronx Zoo. |
As for the surgery itself, in Zuri’s case, Roland recounts, “We had to be prepared in case there was fibrosis inside the cochlea. Fortunately, Zuri wasn’t born deaf, so the inner ear structure was normal, and there was no problem inserting the implant.” As a precaution, the surgical team did have backup devices ready in case the cochlear was obstructed, but the operation, involving a small incision at the back of the ear, went smoothly and was completed in 75 minutes.
The cochlear device, which consists of a processor/microphone that rests above the ear, a transmitting telecoil that is affixed to the scalp, and the inner ear implant, was then tested with the help of an off-site audiologist utilizing the Internet. Neuro-response imaging shows if the brain and central nervous system are responding to the device, and once correct functionality was established, the incision was closed. After a few more hours in the hospital, Zuri went home that evening.
Nearly as challenging as the surgery is the fine tuning of the device, which is accomplished by the audiologist.
“Every single electrode has to be mapped to give total dynamic range,” explains Roland. “The patient should be able to hear but at a comfortable level that is not too loud. It’s a tedious process for the audiologist to determine how much energy actually goes into the electrodes to perceive sound at an acceptable level.” The tuning process, accomplished in this case by William Shapiro, AuD, continues intermittently for months after the initial setup, because “the environment inside the cochlea changes with time, and “we have to make sure the map is still good for her.” Once Zuri and her parents have returned to their homeland, the audiologist continues to work with them remotely online.
“The mother will be given programs (the device can hold three programs), each one louder and more complex than the previous. The audiologist has to make sure that the parents are properly educated in understanding maintenance.”
Thus far, Zuri has received the one left-ear implant, which is functioning properly. It is possible for a patient to do well with just one implant, Roland notes, but with only one there is no directionality, and since the patient doesn’t know where sounds are coming from, there is difficulty interpreting speech in a noisy environment, among other possible hazards. Also, should there be a failure or some kind of problem causing interruption in a single device, the patient would revert to deafness. And, Roland points out, “With both ears working, the overall auditory process is better. The person doesn’t have to work as hard to hear.”
Zuri and her parents are awaiting further funding through their ongoing efforts in order to have the second implant. With all the donations received so far from family, friends, and respondents worldwide, as well as the free device, services of Dr Roland, and reduced hospital costs, the Boucads need to raise about another $30,000 to complete the procedure. Fortunately, the remaining right ear does not show signs of advancing fibrosis, so treatment is not as urgent, and it is hoped that the second operation will take place by the end of 2008 or the beginning of 2009.
The future for cochlear implants is bright, as progress toward increased capacities of the device, as well as miniaturization, is steadily ongoing. “There may come a day,” Roland believes, “when we can not only have greater ability to reproduce sound more naturally, but also place most, if not all, of the apparatus inside the ear.” This would not only result in the cosmetic advance of “invisible” hearing, but would also allow the individual to utilize the device at all times, rather than having to remove the processor and coil while sleeping, bathing, and swimming, as is now the case.
Statistics reveal that four to six out of a 1,000 live births have hearing defects that can lead to profound deafness, and approximately 10% to 15% of those cases would benefit from cochlear implants.
“I think overall the industry and scientists in this area have done a wonderful job in allowing patients to learn to perceive and speak language,” Roland says. “But now they’re going even further, heading into the finer qualities of sound such as music appreciation and understanding speech better in noisy environments. We’re seeing a lot of advancement.”
Patti Trautwein, AuD, director of education at Advanced Bionics, agrees. “Cochlear implants are going in the direction of making the parts smaller and smaller and fully implantable, and the software more and more upgradeable. The technology is leapfrogging into dimensions once thought impossible.” Today, the potential field of candidates for implants has expanded considerably to include those with moderate to severe as well as profound hearing loss. Trautwein says that about 50% of all hearing aid users are now candidates for cochlear implants, as well as children as young as 1 year.
“For a child like Zuri, it makes the difference in learning how to talk. Whereas someone like her used to have to go exclusively to sign language, she now can do both, sign and oral.”
Making a difference is what it’s all about. It takes people to make that difference, and no one appreciates that more than Zuri’s parents, whose hearts are filled with gratitude for all the help they’ve received.
“Zuri loves music, singing, and dancing,” says Nicole. “And those things were just taken away. In our homeland, there are very few hearing loss facilities and the deaf community is not well served. Now, because of all these wonderful people, she has a fighting chance to live up to her fullest potential.”
Dion concurs, “I am extremely grateful for the opportunities given to us. At first we thought there was little hope, that the only choice would be a school for the deaf.”
Their friends, kind strangers, Advanced Bionics, NYU Medical Center, and especially Dr Roland changed all that, loudly and clearly.
Alan Ruskin is staff writer for Hearing Products Report. He can be reached at [email protected].

|
The Big Three
ADVANCED BIONICS
Sylmar, Calif-based Advanced Bionics’ new Harmony HiResolution Bionic Ear System is designed to “help cochlear implant recipients maximize their hearing potential beyond words and experience as much of the full spectrum of natural sound as possible.” The system is comprised of “revolutionary high resolution sound processing with the new Harmony Sound Processor with optional HiRes Fidelity 120 programming,” and the HiRes 90K implant that “enhances music appreciation and improves hearing performance in a variety of difficult listening environments.”
Some of the benefits of the New Harmony BTE Sound Processor include “the fastest stimulation rate available, up to 83,000 signals to the hearing nerve per second, plus CD-quality 16-bit sound processing, programmable wide input dynamic range, and dual–loop automatic gain control for unmatched fidelity and clarity.” The system facilitates using the telephone, listening in classrooms, and enables the hearing of loud and soft sounds without having to use a switch. With a 50% greater battery life than the previous generation BTE, a single charge allows a full day of listening. The processor is also water tolerant and impact resistant, and has a built-in LED for monitoring of system status. (800) 678-2575 ext 2101; TTY: (800) 678-3575; www.advancedbionics.com.

|
COCHLEAR
With world headquarters in New South Wales, Australia, Cochlear introduced cochlear implants more than 20 years ago; 120,000 cochlear milestones later, the company offers two implant systems today. The fifth-generation standard system is the Nucleus Freedom, which the company says is “designed to mimic the path of natural hearing, automatically distinguishing important sounds from everything else.” The system consists of the typical apparatus—processor, telecoil, and implant with electrode array. High on the list of claims for the Nucleus Freedom is its reliability, which Cochlear claims is 99.70%, or only one failure in 333 within a 3-year period. The implant is equipped with the Smart Sound digital microchip, which is designed to handle a broad range of future upgrades and enhancements.
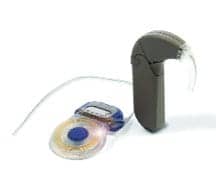
Cochlear’s second offering is the Baha bone-anchored system, which uses direct bone conduction to transmit sound to a functioning cochlea, bypassing the middle ear. This type of implant can be utilized by those whose middle ear has been damaged, blocked, or occluded. The design, says the company, is simple—an abutment connects the processor to a small titanium implant placed behind the ear. The implant fuses with living bone through osseointegration. Cochlear says Baha is the only system of its kind cleared by the FDA, and “recipients report a wide range of advantages over other hearing devices.” Cochlear Americas is based in Centennial, Colo. (800) 523 5798; www.cochlear.com.
|
MED-EL
At Med-El (global headquarters in Austria), the latest offerings are the Maestro implant system and the Opus 2 speech processor. The Maestro features “hearing in high-definition with FineHearing (Fine Structure Processing),” and offers the smallest internal transplant on the market. Also, the company reports that “A clinical investigation demonstrated remarkable improvements in music enjoyment and statistically significant improvements in hearing in noisy environments—two areas of hearing that have been challenging for cochlear implant users.” The Maestro system can be used with either of two Med-El internal cochlear implants (Sonata 100 or Pulsar 100) and either of two speech processors (Opus 1 or Opus 2).
The Opus2, Med-El’s latest speech processor, is “the only processor with a fine tuning remote control (Fine Tuner), which allows adjustments of settings without having to remove the processor from the ear or interrupting hearing.” The company also says that it is “the thinnest and lightest processor available today, with a new ergonomic design for maximum comfort and cosmetic appeal.” Med-El’s North American base is located in Durham, NC. (888) 633-3524; www.medel.com.





