Cooling the sensitive tissues of the inner ear before and during a cochlear implant surgery may lead to better hearing outcomes, according to a University of Miami Health System and College of Engineering researcher who is leading a collaborative team developing this therapeutic approach. An article detailing the research appears on the University of Miami Health System website.
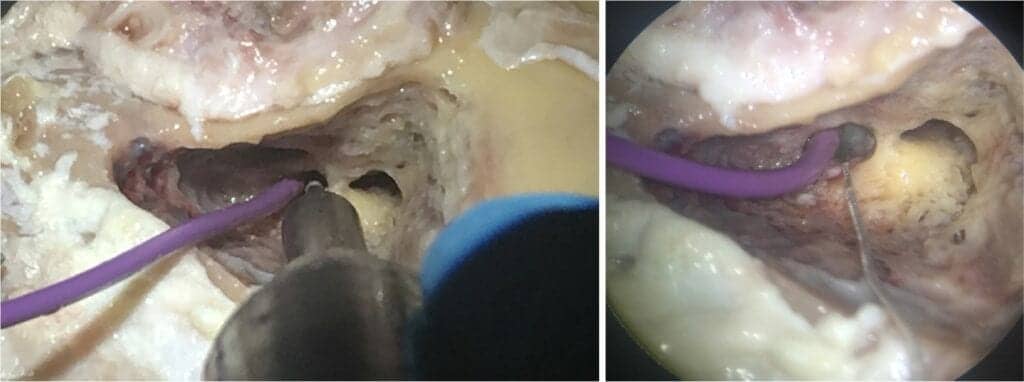
“We are studying how delivering localized hypothermia can support the survival of hair cells and neural structures in the cochlea against this surgical trauma to the inner ear, leading to improved speech perception outcomes,” said Suhrud Rajguru, PhD, associate professor at the Miller School of Medicine, biomedical engineering and otolaryngology, co-director, Institute for Neural Engineering; and assistant director, Miami Clinical and Translational Science Institute (CTSI) Team Science.
Dr Rajguru is the principal investigator of a new five-year, $2 million grant from the National Institute on Deafness and Other Communication Disorders (NIDCD) for “Application of Mild Therapeutic Hypothermia for Hearing Conservation During Cochlear Implant Surgeries.” It follows a pilot grant from the CTSI, a small business innovation grant from the National Institutes of Health (NIH), and industry funding to Dr Rajguru and his laboratory.
“This grant to Dr Rajguru demonstrates the power of the UM engineering-medical collaborations over many years,” said Fred F. Telischi, MEE, MD, chairman of otolaryngology; professor of neurological surgery and biomedical engineering; and the James R. Chandler Chair in Otolaryngology. “Internal seed funding, such as that from CTSI and other sources, has been invaluable to our young investigators and hopefully will continue to grow in magnitude.”
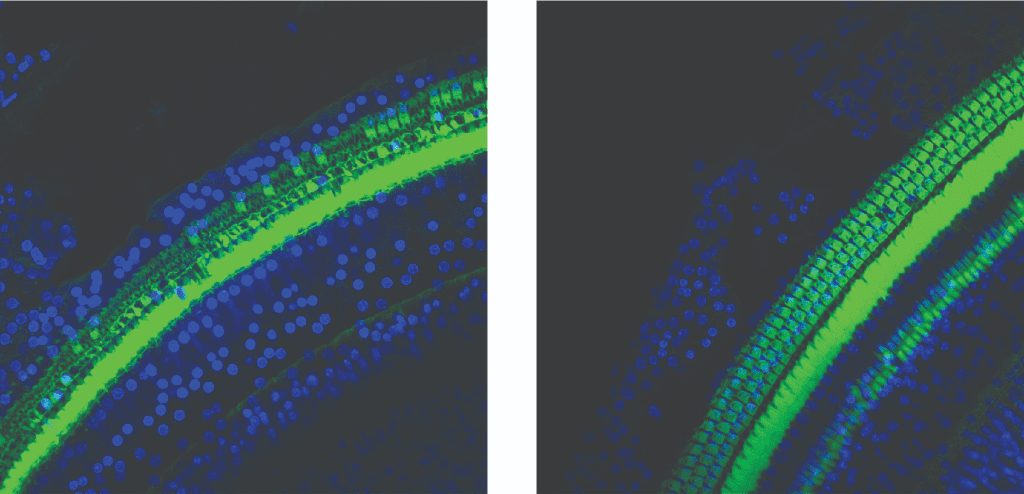
Dr Rajguru has been collaborating with W. Dalton Dietrich, scientific director at The Miami Project to Cure Paralysis and the Kinetic Concepts Distinguished Chair in Neurosurgery; and Michael Hoffer, MD, professor of otolaryngology at the Miller School of Medicine, in studying the delivery of mild hypothermia to the cochlear structures. “Our work would not have been possible without an excellent team of scientists and doctoral students, led by Rachele Sangaletti, PhD, assistant scientist,” said Dr Rajguru. “I am fortunate to get to work with them.”
In the US, more than 500,000 adult and pediatric patients have benefitted from cochlear implants, according to Dr Rajguru. Many have some level of residual hearing that can be affected by the trauma from implantation. “Our preliminary data shows that localized, mild hypothermia delivered to the cochlea is highly effective and safe, preserving residual hearing long-term after implantation,” he said.
The new NIDCD grant will allow the UM researchers to test the safety and effectiveness of cooling the cochlea, and develop an optimal protocol for improved long-term outcomes. “We will also study the neuroprotective mechanisms underlying hypothermia and develop a device and system for patient application,” said Dr Rajguru. “Based on these results, we are also extending the applications of this therapy to other inner ear-related trauma, such as ototoxicity, and noise- and blast-induced hearing loss.”
That research has led to the formation of a start-up by Dr Rajguru and Curtis King, RestorEar Devices LLC, that is developing a prototype device for clinical care.
Working with RestorEar Devices, Dr Rajguru and the UM team are planning to extend these preclinical results to clinical studies with adult patients. However, Dr Rajguru says that the application of mild hypothermia could eventually be extended to children receiving cochlear implants, as well. “Being able to preserve the structures of the inner ear could have an even bigger long-term impact in young pediatric patients,” he added.
A biomedical engineer, Dr Rajguru has been studying the application of hypothermia to the cochlea since 2014 in collaboration with Miller School of Medicine scientists and clinicians. “I truly believe that an interdisciplinary approach can accelerate the translation of laboratory findings to clinical therapies,” he said. “This is a great example and UM has been a leader in supporting this collaborative approach to science.”
Source: University of Miami Health System
Images: University of Miami Health System





