Observations and RH measurements on patients
The basic components of hearing devices are the microphone, receiver, amplifier, and power source. As hearing amplification systems have progressed, many of these components have become smaller and more complex. We have learned that the receiver is the component that is most prone to malfunction. We also touch upon some of the remedies that have been proposed to ameliorate or eliminate receiver failure.

|

|
| C. Mike Hall, AuD, is a clinical audiologist who lives in Walnut Creek, Calif, and is now retired from private practice. Carl Croutch, AuD, is an audiologist at Kaiser Permanente Hearing Center in Daly City, Calif. | |
Based on observations, articles, and discussions with colleagues, there appears to be a correlation between the amount of relative humidity (RH) and proximity of the hearing aid receiver to the tympanic membrane with the incidence of receiver problems. This is true with custom devices such as the in-the-ear (ITE), in-the-canal (ITC), completely-in-the-canal (CIC), and the newer types of devices that are positioned adjacent to the tympanic membrane. As hearing devices have decreased in size, receiver fragility has become an issue.
Previous research. To date, there have been relatively few studies regarding RH measurements of the ear in general, or that specifically examined the RH in a patient’s ear as it would apply to hearing aids.1-4 Bailey and Valente,4 with the help of three assistants, collected data on temperature and RH data occurring inside the shells of ITEs and ITCs they wore. They found that most (77%) of the temperature readings were between 80 and 99°F and most (63%) of the RH readings were between 30% and 49%. Smaller hearing aids (with a smaller mass) like ITCs tended to be slightly warmer, and they noted that exercise and even head gear worn can have some influence on both temperature and RH.
|
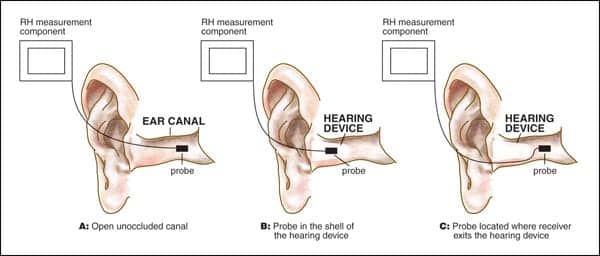
| FIGURE 1. Schematic showing three different methods for placement of a probe for measuring relative humidity (RH). |
Agnew2 reported similar findings wearing a custom ITE with the temperature and RH measured inside the shell of the device. He found that the RH inside the shell closely tracked the RH of the ambient environment (usually between 40% and 50% RH).
Gray et al3 conducted a study of RH on a group of patients, including those with no history of pathological middle ears including no perforations, otitis media, or middle ear drainage. Those with negative histories of middle-ear pathology had RHs of around 40%, whereas a separate group who had positive histories of past and current middle ear problems had RHs of around 70%. This problematic subgroup is that which had a well-documented history of moisture on the canal portion of the device when it was taken out of the ear or had frequent episodes of middle-ear pathology with possible surgical intervention.
However, all of these studies were conducted with the RH probe placed in an open ear3 or in the middle of the hearing aid case2,4 (Figures 1a-b). We feel a more valid method to assess the relationship of RH and receiver problems would be to place the humidity probe where the receiver normally exits the shell (Figure 1c).
|
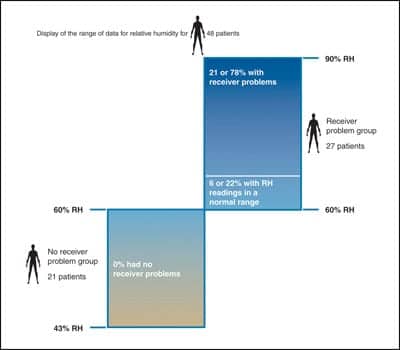
| FIGURE 2. Display of the range of data for relative humidity for the 48 patients in this field study. |
Other factors for consideration. Many professionals in the hearing industry have argued that cerumen is produced in the medial part of the ear canal, and that deeper placement of the receiver in the ear canal reduces the likelihood of cerumen and moisture. However, our clinical experience suggests the deeper the receiver is located, the more likely cerumen and moisture problems will occur.
Another factor that might play a critical role in RH is ambient (external) humidity. For example, a patient in a hot or humid area, such as Houston or Florida, might be expected to have a higher humidity reading in their ear canal.
Field Study
In order to determine if there is a relationship between RH and receiver problems, RH was measured on a group of 48 patients wearing ITC hearing aids. These patients had a negative history of chronic or recent middle-ear problems. In order to focus on RH, we excluded patients who we previously knew had problems with cerumen, debris, or dead skin accumulation.
Questionnaire and patient history. We used a brief questionnaire to obtain a history of the patient’s middle-ear and cerumen problems. The questionnaire asked:
- Do you notice a great deal of wax accumulating in your ears?
- Do you notice moisture on the canal part of your hearing device or do you notice a great deal of moisture when you take your device off?
- Do you feel that you have had an inordinate amount of repairs for your hearing device?
Anyone who indicated a high probability of receiver problems as a result of cerumen and moisture were placed in the Receiver Problem Group (RPG). There were 27 subjects in this group.
The subjects who did not have problems with receiver repairs or did not have any accumulation of moisture and/or cerumen were identified as members of the No Receiver Problem Group (NRPG). There were 21 subjects in this group.
Patient charts were reviewed following the collection of this data to verify the answers on the questionnaires. We found there were varying degrees of cerumen accumulation over a period of time. Some patients who had large accumulations of cerumen were seen approximately every month, while others had no visible cerumen. Additionally, there was a “middle group” of patients who did not appear to accumulate much cerumen, but when the hearing aid was removed and examined, a thin film of cerumen could be seen in the receiver. Patients in this last category can be the most problematic because they will often complain that their device “is not as strong” as when they first received it. If they are wearing a device with a screen or damped receiver, small amounts of cerumen can accumulate without them or the clinician being aware of it.
|
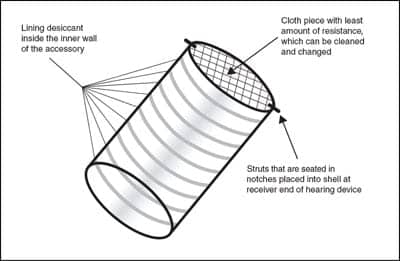
| FIGURE 3. Example of a moisture-reducing accessory. |
RH measurements. We measured the RH for all 48 patients in the study at the point indicated in Figure 1c. In the NRPG group (21 patients), none had RH measurements exceeding 60%, as shown in Figure 2.
However, within the RPG group, only 6 of the 27 patients (22%) had RH measurements in the normal range (50-60% RH), while 21 patients (78%) in this group had measurements above 60% RH.
Discussion and Conclusions
There were a few differences in our data collection compared to previous investigations:
- We placed the measurement probe at the point where the receiver in a custom or deep-canal device would normally be located.
- We excluded patients as subjects if they had ongoing cerumen, debris, or dead skin accumulation.
Additionally, the previous studies2,4 were conducted to observe whether the RH inside the hearing devices varied and/or what the RH values were. Our field study concentrated on what effect RH had, if any, upon the functioning of receivers in relatively deep-seated devices.
As stated earlier, while the RPG did not have a history of heavy cerumen accumulation, in our opinion, they were susceptible to receiver problems because of the consistent collection of small amounts of cerumen visible with an otoscope. We observed that even large vents in the shell had no effect upon the RH measurement, although it should be noted that Agnew2 found higher RHs (by 17% to 23%) in what may have been similar venting. The RPG patients, who did not appear to have high amounts of cerumen, did have a persistent film of wax. Very possibly, humidity and atmospheric conditions contributed to the persistent film of wax that was exhibited by these patients. Over time, this could lead to an amount of wax that dampens the sound output.
A useful indicator that a patient may have this kind of problem is if they inform the clinician that they hear well in the morning when they put their devices on, but after a few hours the aids seem to get weaker. In the past, when only analog devices with a volume control were available, the patient merely turned their volume control up if the loudness decreased. Many newer digital hearing aids do not have this capability.
Discussion and Summary
This study may help clarify the role of RH and its relationship to receiver failure. In summary, subjects with RH values greater than 60% were found most likely to have receiver failures as a result of moisture, whereas subjects with 40% or less have dramatically fewer problems relative to receiver problems.
Manufacturers have tried to deal with this issue; dry-aid kits, ultrasonic, vacuum and centrifuge cleaners, and other similar types of devices are available to the client to mitigate moisture problems. However, our clinical experience and findings from this study indicate that there is no device that is 100% effective in solving receiver-moisture problems.
Our suggestion would be to consider the development of insertable and removable devices that look similar to the Knowles metal impedance cylinders in various sizes. This type of device would be the structural size of a Knowles receiver that was originally designed for use in BTE devices and used on occasion in other styles of devices, as shown in Figure 3.
Although these filters are typically used for modifying gain, output, or smoothing the frequency response of the sound coming out of the ear hook, the device we are proposing is one with a desiccant moisture absorbing material where the impedance filter would usually fit. The size of the receiver openings exiting many of the hearing devices today is smaller than in BTE hearing aids. The type of moisture control sleeve would consist not only of a changeable receiver sleeve but more importantly, an insert device lined with desiccant or water absorbing material. This moisture control device could be easily changed by the patient without affecting the proper functioning of the receiver.
Further, a low-cost RH measurement device could prove helpful in identifying patients with abnormally high RH values. This would assist the clinician in counseling regarding potential receiver moisture problems. If RH measuring devices were made and sold in bulk, they could be reasonably priced.
Our data suggests that patients identified for high RH and, hence, moisture and receiver problems should be counseled as to the importance of taking proactive measures to reduce potential frustrations with the device. Our hope is that these findings will lead to additional research and possibly the development of better equipment to deal with this problem, and if necessary, that RH assessment will become a part of the selection and fitting process.
References
- Bruener RC, House L. Thermodynamics of the external auditory canal. Temperature and relative humidity inside an ITE hearing instrument. Ann Otol Rhinol Laryngol. 1967;76(2):409-13.
- Agnew J. Temperature and RH inside an ITE hearing instrument. Hearing Review. 1999;6(8):28-73.
- Gray RF, Sharma A, Vowler SL. Relative humidity of the external ear canal in normal and abnormal ears, and its pathogenic effect. Audio Clin Otolaryngol. 2005;30(2):105-114
- Bailey JW, Valente M. Measurements of relative humidity and temperature in hearing aids. Hear Jour. 1996;49(10):59-63.
Correspondence can be addressed to HR or C. Mike Hall at , or Carl Croutch, AuD, at .
Citation for this article:
Hall CM, Croutch C. A Field Study on the Effect of Relative Humidity on Hearing Aid Receivers. Hearing Review. 2010;17(1):32-35.