When tinnitus becomes a constant disturbance rather than just an occasional perception, a comprehensive rehabilitation approach is required that addresses the audiological (hearing loss), neurological (adaptive response/”central gain”), and psychological (attention and reaction) aspects of the condition. By targeting all of these aspects together, a therapy is more likely to provide consistent and rapid improvements in tinnitus awareness and disturbance.
This forms the basis for the development of the Neuromonics® Tinnitus Treatment. This article describes current thinking about the causes of tinnitus and how the Neuromonics therapy works, and highlights data from current peer-reviewed studies.
Tinnitus Effects and Prevalence
Subjective tinnitus is the presence of sound heard in the absence of an external sound source, localized to either ear or throughout the head. Epidemiological studies estimate that there are 40 million Americans who experience tinnitus and, of these, 10% to 15% have tinnitus that warrants medical evaluation.1
Chronic tinnitus—or tinnitus that lasts more than 6 months—is often associated with other comorbidities, including insomnia and anxiety, which contribute to its impact on quality of life.2 Because it is most bothersome at quiet times, tinnitus can greatly disrupt sleep patterns, relaxation times, and concentration. Stress almost invariably makes tinnitus worse, but the overbearing experience of chronic tinnitus is also stress producing, so it can be a self-perpetuating problem .
Causes of Tinnitus and Central Gain
Recent research has shown that tinnitus is not simply an ear problem, but a neurological condition. Current thinking is that tinnitus involves the normal background neural activity in the hearing system—or “internal noise” —which is always present but not usually noticeable because normal hearing ensures that external sounds are louder than this internal noise. Hearing loss disturbs that natural balance, “uncovering” the internal noise.
What seems to make tinnitus disturbing is how the brain responds to the damage that has occurred with hearing loss.3 The brain automatically attempts to compensate for the hearing loss by turning up the sensitivity of the hearing system (a process referred to as central gain4). This results in the perception of this neural activity as sound; it also commonly results in decreased sound tolerance. Additionally, the brain engages a filtering mechanism that results in the tinnitus being readily detected among other signals along the auditory pathways.
Also involved is the triggering of the emotional centers of the brain—and also the fight-or-flight response that creates stress and, in turn, makes the tinnitus worse. Accordingly, the tinnitus condition involves audiological aspects (ie, the initial hearing loss that causes the auditory deprivation), neurological aspects (ie, the brain’s adaptive response to the auditory deprivation or central gain), and psychological aspects (ie, inappropriate attention to it and the emotional response or reaction to tinnitus perception and awareness).
Treatment Options for Tinnitus
Research by Hallam5 in the 1980’s and later by others, including Tyler and Babin,6 Tyler and Baker,7 Henry and Wilson,8 Coles,9 and Hazell,10 elaborated on tinnitus therapies that aimed for habituation or desensitization. These approaches seek to address the neurophysiological and psychological aspects of the condition, typically with some combination of sound therapy and counseling11 in order to reduce the disturbance associated with the patient’s reaction to his or her tinnitus perception.
The rationale behind the use of sound therapy in the treatment of tinnitus is that sound can make the tinnitus less noticeable to the patient, providing relief and thereby reducing the negative reaction to the tinnitus perception. A wide range of approaches have been used, including:
- Hearing aids. By amplifying ambient sound, aids can be helpful for people with mild tinnitus, particularly those with a marked hearing loss within the speech range, normal sound tolerance, and no difficulties sleeping, concentrating, and relaxing. The evidence that hearing aids can consistently reduce tinnitus perception for such patients is not clear.12
- Ear-level sound generators or maskers. Looking similar to hearing aids, these devices produce a constant broadband noise that serves as a distraction from the tinnitus perception. However, they have not shown consistent effectiveness and commonly have high rejection and return rates13, so they are not now commonly used.
- Musical and environmental recordings. A readily accessible option, but one that is limited in usefulness by low-frequency bias and the highly dynamic nature of ordinary music, particularly for those with decreased sound tolerance.
- Fans and general sound enrichment. These can be helpful in specific quiet locations (eg, at bedtime).
A New Tinnitus Treatment Method
Australian audiologist Paul B. Davis, PhD, developed the Neuromonics technology as a consequence of his own experience with tinnitus nearly 15 years ago. While recognizing the merit of approaches that combined sound therapy with counseling, Davis discovered that the available options were characterized by a lack of consistent clinical efficacy, efficiency, and/or user acceptability. He investigated ways to make sound-based treatment more efficient and pleasant to use by addressing the audiological, neurological, and psychological aspects of the condition.
Neuromonics Tinnitus Treatment uses a spectrally modified and customized broadband acoustic stimulus. The acoustic customization takes into account each patient’s unique hearing and tinnitus profile, allowing stimulation of a broad range of auditory pathways at a comfortable listening level. The customization is performed separately for each ear to allow a broad frequency stimulus (up to 12.5 kHz) at a low-volume overall listening level, allowing for any asymmetry in hearing thresholds.
The treatment also takes into account loudness sensitivity considerations so that the listening experience is both pleasant and comfortable. The use of relaxing music as part of the acoustic stimulus—spectrally modified to account for individual hearing loss in each ear—positively engages the limbic system, facilitating a beneficial emotional response and compliance with treatment.
The effectiveness of the customization process can be seen when measuring the listening volume required to cover up the tinnitus, which averaged 16 dB lower for the customized stimulus than an equivalent noncustomized stimulus.14 This is a large difference because 6 dB represents an approximate doubling of loudness. This is a key aspect of this treatment and distinguishes it from the use of broadband noise generators and noncustomized music. With these latter approaches, patients commonly report that the volume becomes uncomfortably loud before they can achieve any appreciable interaction with their tinnitus perception.
The dynamic nature of music used as part of the Neuromonics stimulus also allows the patient to experience intermittent exposure to his or her tinnitus perception. Experiencing repeated, momentary exposure to the tinnitus perception in the context of a relaxing and pleasant listening experience is a key objective of the treatment because this facilitates the desensitization process.

|
| FIGURE 1. Neuromonics Oasis is a Class II medical device for treating tinnitus that uses individually customized signals for each ear to allow a broad frequency stimulus (up to 12.5 KHz) at a low-volume level. |
The use of the customized acoustic treatment is combined with a collaborative counseling program that involves education, support, and monitoring over a typical 6-month period, while the total clinical time required is modest at around 5 to 6 hours per patient.
Integrating Treatment for Everyday Use
Patients are recommended to use the treatment for at least 2 hours per day for approximately 6 months. The acoustic stimulus is administered using a completely digital, Class II medical device called the Neuromonics Oasis (Figure 1). The portable device is designed to allow the patient to easily and conveniently integrate treatment into his or her day-to-day routine. It incorporates a usage log to allow patients to monitor their daily dosage, and to allow hearing care professionals to easily track patient use at regularly scheduled appointments.
Patient Indications
Adults with a clinically significant degree of tinnitus disturbance and hearing thresholds that are no worse than moderate across the speech range in at least one ear are considered the best candidates for Neuromonics treatment. Patients with more extensive hearing loss—including those with usable hearing in only one ear—also respond well to treatment, albeit treatment usually requires a longer duration to appreciate full benefits.
The treatment has also been shown to be effective in improving loudness tolerance levels among patients with decreased sound tolerance, in addition to reducing their tinnitus disturbance and awareness.14 Such patients are commonly very challenging to treat effectively using other forms of sound therapy.
Patient Outcomes
Neuromonics Tinnitus Treatment has been the subject of evaluation over a series of controlled clinical studies over the past 15 years. These studies have shown that the approach yields consistently positive results for tinnitus sufferers. One was a randomized, controlled study15 that compared the effectiveness of the Neuromonics Tinnitus Treatment to a counseling-only control group and a group that received bilateral broadband noise (set at the “mixing point”), plus counseling. It revealed superior clinical outcomes for the Neuromonics system relative to the other approaches.
A peer-reviewed study14 that appeared in the April 2007 edition of Ear and Hearing compared stage-related variants of the Neuromonics approach. The most consistently positive outcomes were reported with a two-stage protocol in which subjects had their tinnitus completely covered up while using the treatment for the first 2 months, then experienced intermittent exposure for the remaining 4 months of treatment. As a consequence, it is this protocol that is now being offered by specialist clinics around the country. Some highlights of the results for this protocol are described below.
|
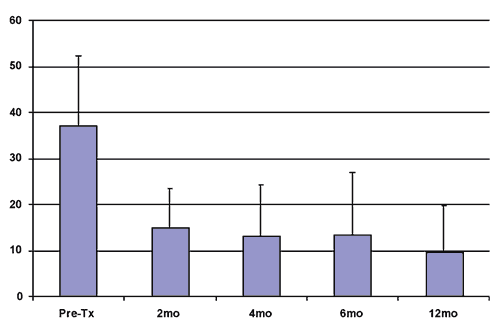
| FIGURE 2. Mean level of tinnitus disturbance as measured by the Tinnitus Reaction Questionnaire (TRQ), which assesses 26 aspects of tinnitus on quality of life (n = 35). The TRQ yields a score of 0 to 104, with a score of 17 considered clinically significant. Solid bars represent group TRQ score means, with error bars corresponding to one standard deviation. Sizable changes were reported quickly (within 2 months), and 95% of subjects reported an improvement in level of tinnitus disturbance of at least 40% after 6 months.14 |
Improvement in TRQ scores. Figure 2 shows improvement in the mean level of tinnitus disturbance for this group, as measured by the Tinnitus Reaction Questionnaire (TRQ).16 The TRQ evaluates 26 aspects of the impact of tinnitus on quality of life, yielding a score between 0 and 104, whereby a score of greater than 16 is considered clinically significant. The data demonstrate that sizeable changes were reported quickly—after 2 months. After 6 months, 95% of subjects reported an improvement in tinnitus disturbance of at least 40%, and 79% reported a level of tinnitus disturbance that was no longer clinically significant (a TRQ score of less than 17). Mean percent improvement on this measure was 64% after 6 months, rising to 74% after 12 months.
A significant finding in this study was a clear dosage relationship between clinical outcomes and average device usage. Figure 3 displays the clinical outcomes achieved after 4 months for low users (whose reported usage was 0 to 1.5 hours per day), moderate users (1.6 to 2 hours per day), and high users (>2 hours per day).
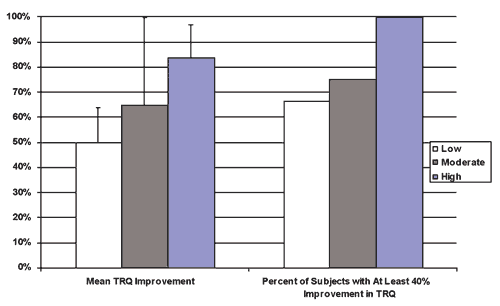 |
| FIGURE 3. Relationship between reported treatment usage (low, moderate, and high) and clinical improvement after 4 months. |
Improvement in LDLs. Improvements in loudness discomfort levels (LDL) were also reported in this study. After 12 months, mean LDL improvement exceeded 10 dB. This is a significant result in light of the high prevalence of decreased sound tolerance among tinnitus sufferers, and the debilitating impact this condition can have on overall quality of life. As a result of this finding, further study is planned to evaluate treatment in patients with hyperacusis, or hearing sensitivity, who do not have clinically significant tinnitus.
-
- According to an article in the March 2007 JAAA, and reported on in the April 26, 2007 HR Insider, almost 25% of the population has tinnitus, with 9.4% reporting moderate to severe tinnitus. The researchers concluded that “quality of life is diminished in participants with tinnitus, and the effect increases with severity.”
Overall outcomes. Achieving the above clinical end points translated into important quality-of-life benefits. Large improvements in sleep, relaxation, and general well-being were also reported by a high number of subjects. Furthermore, nearly all subjects found the treatment pleasant and convenient to use, and would recommend it to others.
Conclusion
Neuromonics Tinnitus Treatment is an effective, innovative, noninvasive treatment for adults with moderate to severe tinnitus disturbance. It features a convenient-to-use Class II medical device that provides customized acoustic stimulation in conjunction with a collaborative counseling program. It has been clinically proven to reduce both disturbance from and awareness of tinnitus over a relatively short period of time, doing so consistently for a very high number of suitable patients.
References
- Heller AJ. Classification and epidemiology of tinnitus. Otolaryngol Clin North Am. 2003; 36,239-248.
- Langenbach M, Olderog M, Michel O, Albus C, Kohle K. Psychosocial and personality predictors of tinnitus-related distress. Gen Hosp Psychiatry. 2005;27; 73-77.
- Jastreboff PJ. The neurophysiological model of tinnitus. In Snow JB Jr, ed. Tinnitus: Theory and Management. Hamilton, Ontario: BC Decker Inc; 2004:96-106.
- Eggermont JJ. Tinnitus: some thoughts about its origin. J Laryngol Otol. 1984;(suppl 9): 31–7.
- Hallam RS. Tinnitus: Living with the Ringing in Your Ears. New York: Harper Collins;1989.
- Tyler RS, Babin RW. Tinnitus. In: Cummings CW, Fredrickson J-M, Harker L, Krause CJ, Schuller DE, eds. Otolaryngology–Head and Neck Surgery. St. Louis: CV Mosby Co; 1986:3210-3217.
- Tyler RS, Baker LJ. Difficulties experienced by tinnitus sufferers. J Speech Hear Disord. 1983; 48:150-154.
- Henry JH, Wilson PH. The Psychological Management of Chronic Tinnitus: A Cognitive–Behavioral Approach. Boston: Allyn & Bacon; 2001.
- Coles RRA. Tinnitus and its management. In: Stevens SDG, Kerr AG, eds. Scott–Brown’s Otolaryngology. 5th ed. Boston: Butterworth Publishers Inc; 1987:368-414.
- Hazell JWP. Tinnitus. London: Churchill Livingstone; 1987.
- Tyler RS. Neurophysiological models, psychological models, and treatments for tinnitus. In Tyler RS, ed. Tinnitus Treatments: Clinical Protocols. New York: Thieme Medical Publishers; 2005:1-22.
- Surr RK, Montgomery AA, Mueller HG. Effect of amplification on tinnitus among new hearing aid users. J Am Acad Audiol. 1999; 10:489-495.
- Henry JA, Schecthter MA, Nagler SM, Fausti SA. Tinnitus retraining therapy and masking; how do they compare? In Patuzzi R, ed. Proceedings of the Seventh International Tinnitus Seminar. Perth: University of Western Australia; 2002:247-254.
- Davis PB, Paki B, Hanley PJ. The neuromonics tinnitus treatment: third clinical trial. Ear Hear. 2007;28: 242-259.
- Davis PB, Wilde RA, Steed L. Clinical trial findings of a neurophysiologically-based tinnitus rehabilitation technique using tinnitus desensitization music. In: Patuzzi R, ed. Proceedings of the Seventh International Tinnitus Seminar. Perth: University of Western Australia; 2002:74-77.
- Wilson PH, Henry J, Bowen M, Haralambous G. Tinnitus reaction questionnaire: psychometric properties of a measure of distress associated with tinnitus. J Speech Hear Res. 1991; 34:197-201.






