Twelve efficient screening methods for initial assessment of vestibular function
Hearing care professionals routinely encounter patients who present with problems involving balance and/or dizziness. These symptoms can lead to falls and life-threatening injury and/or severely impede their lifestyles, and thus must be treated or referred. Here are a dozen quick and effective tests that can be added to your armamentarium when screening patients for vestibular problems.
Efficiently and effectively diagnosing and treating dizziness is of paramount concern to the patient and the professional. Dizzy patients are among the most complicated and time-consuming patients seen in dispensing offices. Significant time commitments and expertise are required to obtain the case history and to document signs and symptoms, select and perform peripheral and central balance system tests, and more—all of which culminates in a comprehensive diagnosis, treatment plan, and even in-office therapeutic maneuvers.
The balance system is complex. Healthy balance systems rely on complementary and accurate sensory input from vestibular, vision, and somatosensory systems to perceive and interpret the individual’s location with regard to gravity, the horizon, and space. The balance system also indicates whether we’re moving and in which direction relative to our surroundings, and which counter-or-corrective action is required.
To maintain balance, the brain relies on equal-but-opposite (ie, paired) input from the left and right semi-circular canals (SCC). The left anterior SCC is paired with the right posterior SCC, the left posterior SCC is paired with the right anterior SCC, and the left and right horizontal SCCs are paired. In a healthy vestibular system, when the left side of the vestibular system sends excitatory information to the brain, the right side sends an equal amount of inhibitory information to the brain. If one of the vestibular organs is weak or impaired, the brain senses a mismatch, resulting in dizziness.
Dizziness is a catch-all term for numerous symptoms, ranging from subjective to objective vertiginous sensations (ie, the person feels they are spinning or senses the room is spinning, respectively), to “light-headedness” to weakness while rising from a sitting position, and everything in between. Balance problems negatively impact virtually every aspect of the patient’s life. Some patients experience a single episode of vertigo, while others may present during an acute stage of labyrinthitis; some present with positional vertigo and can be treated in the office.
Equilibrium problems reach beyond the adult population and may manifest as “balance problems” in infants and children, rather than “vertigo” or “dizziness.” Gans1 reminds us that children have “audio-vestibular systems,” not just auditory systems; congenital or acquired deficits may impact the entire audio-vestibular system. Beck, Petrak, and Bahner2 reported “Vestibular disorders in children are often under-diagnosed, and vestibular disorders are more common in children with significant hearing loss and other inner-ear abnormalities.”
To efficiently and effectively diagnose and treat dizziness, clearly the best option is to have expert audiologists and a sophisticated vestibular laboratory (ENG, VNG, VEMP, Rotary Chair, VAT, CDP and more) available. Pragmatically, experts with state-of-the-art equipment are not always available and may not be the first person to evaluate and diagnose these patients.
Therefore, this article proposes an efficient, effective, and low-cost screening protocol for the hearing care professional to consider with regard to the initial evaluation of the “dizzy” patient, and to help triage, document, and refer (as needed) these same patients.
1) Comprehensive Case History
Prior to vestibular assessment, a comprehensive case history should be obtained, including when their dizziness signs and symptoms started, how long they lasted, when the last event occurred, as well as the patient’s description of the event, and more. Dizziness questionnaires (such as Dizziness Handicap Inventory or DHI) are often useful as a “starting point” to identify and probe specific situations and concerns.
The following are some useful questions and their rationales:
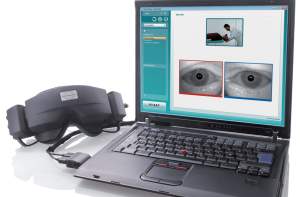
Figure 1. Frenzel Lenses (left) are shown alongside a laptop computer with a recorded image of both eyes. The image is recorded in real time and can be stored and replayed for in-depth analysis.
Q: Describe your symptoms to me without using the word “dizzy.”
Listen for terms used such as “every time,” “room spins,” “only when I turn to the left/right,” “veering to the left/right when I walk,” “this ear feels stopped up,” “unsteady,” etc.
Q: Have you recently been ill?
It is not unusual for a virus to impact the vestibular system if a patient has recently had a cold/flu or bad allergies.
Q: Have you had a recent change in medications?
Vertigo is a very common side effect of many medications.
Q: When you’re dizzy, do you experience ringing or buzzing in your ears?
“Roaring” in the ears may indicate endolymphatic hydrops or Ménière’s disease. Tinnitus in only one ear may indicate retrocochlear pathology.
Q: Do you experience symptoms every time you move your head in a certain way such as looking up, lying down, bending over, etc?
If the patient answers “yes,” it is likely their vertigo is related to head position.
Q: Do your symptoms occur only when you turn your head or lie down on one side?
This symptom is consistent with BPPV/positional vertigo.
Q: Do you experience a “stuffy” feeling in one or both ears when you are having dizziness?
This symptom may be related to endolymphatic hydrops or Ménière’s disease.
Q: When you lie down, do you have a brief burst of dizziness for a few seconds that goes away when you lie still?
This question will help to differentiate positional vertigo from BPPV.
Q: Is your dizziness exacerbated by loud noises or bearing down?
This question helps rule out perilymphatic fistula or semi-circular canal dehiscence.
2) Complete Audiometric Evaluation
Because the auditory and vestibular systems are contiguous and are both housed within the temporal bone, it is not surprising that, if one of these systems is affected by disease, the other may also be affected. Therefore, a complete audiometric evaluation should be obtained. The minimal audiometric test protocol should include:
- Otoscopy;
- Tympanometry;
- Ipsi- and contra-lateral acoustic reflexes;
- Pure tone thresholds (air and bone)
- Word recognition scores
- Other tests (OAEs, ABR, etc) as indicated.
3) Valsalva-Induced Nystagmus
To perform a “Valsalva,” the patient should pinch their nose and “blow”—thereby increasing intracranial pressure. However, this method cannot differentiate an increase in spinal fluid pressure from increased air pressure within the middle ear (affecting the superior canal).
A more specific means of performing this test is to ask patients to hold their breath by closing off the back of the throat (the glottis) and to “bear down” for 5 seconds in an effort to increase intracranial pressure. In both cases, the clinician would report the patient’s subjective remarks regarding whether they experienced vertigo. If the patient reports vertigo, the test should be repeated with VNG or Video Frenzel goggles.
The Valsalva-induced nystagmus test indicates whether a change in middle-ear or intracranial pressure is being relayed to the inner ear and causing vertigo. The most common disorder presenting with this symptom is superior canal dehiscence. This test also has been used in the investigation of Chiari malformation, perilymphatic fistula, and cholesteatoma.
4) Informal Spontaneous Nystagmus Examination
This test is performed by asking the patient to gently close her eyes while the clinician watches for underlying eye movement. The patient is instructed to open her eyes and visually fixate on a target. Look for three things:
- Are eye movements present? If so:
- In which direction does the eye move, and
- Does the severity of the eye movement decrease with fixation?
Spontaneous nystagmus while fixating (or any abnormal movement of the eyes while fixating) is considered a “soft sign” of central vestibular dysfunction.
While the spontaneous nystagmus test can be performed without any test equipment, recording with Video Frenzel goggles can provide added benefit to your evaluation by allowing you to physically see the patient’s eye movements, which are recorded with infrared cameras while the patient remains in a vision-denied environment. Having access to these eye recordings can, and often does, enhance the overall evaluation and can ultimately lead to a more accurate diagnosis.
5) Informal Gaze Nystagmus Examination
The clinician instructs the patient to visually follow their finger, pen, etc. Begin with the target at the patient’s center gaze. Move the target upward about 30° and maintain that position for at least 5 seconds. Repeat the procedure downward, left, and right while continually monitoring the patient’s eyes for nystagmus. Gaze nystagmus is also a soft sign of central vestibular dysfunction.
6) Informal Visual Tracking Exam
Instruct the patient to visually follow your finger while slowly and smoothly moving the target horizontally from one side of the visual field to the other. The patient should follow the target with smooth, controlled eye movement. The inability to do so is considered a soft sign of central vestibular dysfunction.
7) Dynamic Visual Acuity (DVA)
Dynamic visual acuity measures the patient’s ability to visually track a stable object while his head is in motion. It is a test of the vestibulo-ocular reflex (VOR).
This test requires a Snellen eye chart. The clinician instructs the patient to read the smallest line possible from a distance of 10 feet. The patient then turns his head from side-to-side at a rate of approximately 2-3 seconds with an arc of 20°. Visual acuity is reassessed in tandem with head motion. A significant drop in visual acuity (a change of two lines or more from the Snellen chart baseline test) implies an impairment of the patient’s VOR.
8) Dix-Hallpike
The Dix-Hallpike is used to evaluate (confirm or refute) benign paroxysmal positional vertigo (BPPV).3 The test is performed by guiding the patient through positions designed to provoke movement of otoconia within the semi-circular canals.
The patient sits lengthwise on a table with enough room behind them to support their body and shoulders. The audiologist carefully turns the patient’s head to the right (or left, depending on which ear you suspect to be affected) 30° and briskly assists the patient to a supine position with their head hanging for at least 20 seconds while the audiologist observes the patient’s eye movements. A “positive” Dix-Hallpike results in a brief burst of intense vertigo when the test is performed with the affected side downward. Additionally, “torsional” or rotary nystagmus may be observed with the top of the eye rotating geotropically (toward the earth and toward the affected ear) in tandem with a complaint of dizziness by the patient.
Patients who test positive for BPPV are generally candidates for treatment of this condition via canalith repositioning maneuvers. This test also can be enhanced by recording the patient’s nystagmus via Video Frenzel infrared cameras.
9) Past-Pointing
Past-pointing is a test of the integrity of the vestibular system. The patient extends one arm and places the index finger on the index finger of the clinician (or a static target such as a mark on a table). The patient closes her eyes, raises her arm above the head, and then quickly returns (as best she can with eyes closed) to the starting position. The procedure should be repeated several times.
If the patient successfully returns her index finger to the target (ie, a “negative” result), no abnormalities are indicated. Conversely, if her index finger misses the target substantially (ie, “drifts”), a “positive” result is noted, which may indicate vestibulo-cerebellar abnormalities.
Alternatively, the subject is seated in a revolving chair with eyes closed and is rotated to the right 10 times. The right arm is extended horizontally and the right index finger is brought to touch the examiner’s finger; the arm is then raised vertically and the subject is instructed to touch the examiner’s finger while again placing the arm horizontal. If the vestibular apparatus is normal, the finger will be brought down several inches to the right of the examiner’s finger or may touch the target. The same is true with left rotations and the same left-based challenges.
10) Romberg
The Romberg can occasionally be used to help establish whether vestibular dysfunction exists. The patient is instructed to stand with feet together and arms to the side with eyes closed. The examiner should watch the patient closely for 1 minute to see if the patient begins to sway (positive Romberg). If the patient sways with eyes closed, the test is considered positive. This test is non-specific regarding site-of-lesion.
11) Fukuda Stepping Test
The Fukuda Stepping Test (“Fukuda”) screens for asymmetry of the peripheral vestibular systems. The patient stands with eyes closed and arms extended to the front and “steps in place” (ie, marches) for 50 steps while the clinician observes and documents whether the patient rotates. A rotation greater than 30 degrees is considered a positive Fukuda, indicating peripheral vestibular dysfunction likely consistent with the side to which the patient has rotated.
12) Screening for Lower Extremity Weakness
If the musculature of the lower body and/or legs is impaired, the patient is at greater risk for imbalance and falling. To screen for lower extremity weakness, simply ask the patient to get up from a chair without using their hands or arms. If the patient is unable to perform this task, the examiner notes the patient is likely at greater risk for falling due to lower extremity weakness. This weakness may also be linked to the common patient complaint of “imbalance.”
Summary
When dizzy patients present to the clinician, it is of paramount concern to quickly evaluate, treat, and/or refer the patient. The screening protocols mentioned above highlight useful “bedside” tests, which may be used individually or collectively. These tests do not involve expensive equipment, but may be enhanced with Video Frenzel goggles to allow for video recordings of eye movements.
These screening tools may be useful with regard to identifying the etiology and may serve as the foundation for referral to other professionals (otolaryngologist, neurologist, or audiologist) with sophisticated balance equipment. In the next installment of “In the Trenches,” we’ll review contemporary balance equipment and the contributions each component offers.
Correspondence can be addressed to HR or Douglas Beck, AuD, at .
References
- Gans R. Equilibrium-vestibular assessment for infants. Audiology Today. January/February 2012:25-31. PDF at: preview.tinyurl.com/83f9tzx
- Beck DL, Petrak MR, Bahner CL. Advances in pediatric vestibular diagnosis and rehabilitation. Hearing Review. 2010;17(11):12-16. At: tinyurl.com/6u6w8vy
- Agrawal, Y., Carey, JP., Hoffman, HJ, Sklare, DA and Schubert, MC. (2011): The Modified Romberg Balance Test: Normative Data in U.S. Adults. Otol Neurotol. 2011 Oct; 32(8):1309-11.
- Casqueiro, JC., Ayala, A & Monedero, G. (2008): No More Postural Restrictions in Posterior Canal Benign Paroxysmal Positional Vertigo. Otology and Neurotology. Vol 29, No 5. August. Pgs 706-709
- Herdman, SJ., Schubert, MC & Tusa, RJ. (2001): Role of Central Preprogramming in Dynamic Visual Acuity with Vestibular Loss. Arch Oto HNS 2001:127:1205-1210
- Jacobson GP, Shepard NT. (2008): Balance Function Assessment and Management. San Diego; Plural Publishing.
- Management of BPPV (2008 ): Interview with Alan Desmond, Au.D. www.audiology.org/news/interviews/Pages/20081113a.aspx
- O’Reilly RC, Morlet T, Nicholas BD, Josephson G, Horlbeck D, Lundy L, Mercado A. (2010): Prevalence of Vestibular and Balance Disorders in Children. Otology & Neurotology 31(9):1441-1444.
- Parnes LS, Nabi S. (2009): The Diagnosis and Management of Benign Paroxysmal Positional Vertigo. Seminars in Hearing 30(4):287-303.
- Gans R. Overview of BPPV: Pathophysiology & diagnosis. Hearing Review. 2000;7(8):38-43,72. At: tinyurl.com/8798dpc4.
- Overview of BPPV: Treatment Methodologiesby Richard E. Gans, PhD At: tinyurl.com/7sdduk3
Citation for this article:
Smith A., Petrak M., Bahner C., Beck D. In the Trenches, Part 1: Screening Tests for Patients with Dizziness Hearing Review. 2012;19(04):12-23.









