Some people report ringing in their ears. Others hear crickets. And still others describe whooshing, pulsing, ocean waves, buzzing, and/or music. But in the absence of any actual noise, they are all suffering from the same thing—tinnitus.
The American Tinnitus Association (ATA) of Portland, Ore, estimates that more than 50 million Americans suffer from the condition to some degree, with 12 million of these seeking medical attention. The experience is individualized. In addition to the differing sounds, the noise may be constant or intermittent, different in pitch and tone, and mildly annoying to maddening. The ATA suggests about 2 million tinnitus patients cannot function normally as a result of the subjective noise.
|
For more on the latest |
The exact causes of tinnitus are unknown, but some conditions, such as Meniere’s disease, a vestibular disorder resulting from abnormal amounts of fluid collecting in the inner ear, have been found to be linked. “Tinnitus is not an etiology but a symptom,” says Teri Sinopoli, director of clinical services for Neuromonics USA, in Bethlehem, Pa. Sinopoli says the condition is often indicative of damage to the hearing system and, as such, may not be curable.

|
| Peter Hanley |
There is no gold standard of treatment for tinnitus, and methods are often evaluated on a trial basis. “There have been a lot of treatments developed over the years, but nothing has turned out to be efficacious for a large group of people,” says Peter Hanley, director and CEO of Neuromonics Inc, Chatswood, Australia. Hearing aids and maskers can be inadequate solutions. “Hearing aids don’t help during quiet times when tinnitus can be most disturbing, and maskers can add to hearing loss difficulties,” says Hanley. Many patients are unable to find relief.
This was true of Paul Davis, PhD, chief scientific officer of Neuromonics, and an audiologist, jazz musician, and tinnitus sufferer. “Dr Davis wanted the best treatment his profession could give him when he developed tinnitus, but found there was nothing particularly effective,” Hanley says. So Davis decided to investigate the problem and eventually developed the intellectual property upon which the Neuromonics Tinnitus Treatment is based.
The combination therapy—music, sound, and counseling—has been in development for about 15 years, with the past 5 years or so focused on commercialization. Western Australia’s Curtin University of Technology, where Davis is an adjunct associate professor, has supported the treatment’s development because of its potential benefit for large numbers of patients. “Our treatment is distinctive in that it provides bigger improvements more quickly and more consistently than other treatment,” Hanley says.
PROOF OF IMPROVEMENT
The company has proven this benefit in four clinical trials that have spanned more than a decade. The research has shown a 90% success rate in candidates eligible for the treatment (success is defined as a reduction of at least 40% in tinnitus disturbance), a mean improvement of two-thirds, and a 2-month time frame for the benefits to be felt.
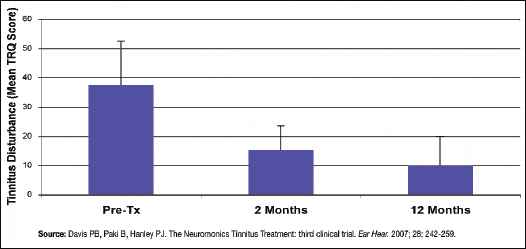
One trial found 91% of all subjects reported an improvement in tinnitus disturbance—as measured by the Tinnitus Reaction Questionnaire (TRQ)—of at least 40% at 6 months, with a mean improvement of 65%. In the same trial, 80% of subjects reported a level of tinnitus disturbance at 6 months that was no longer clinically significant.
|
| Figure 1. Mean level of tinnitus disturbance as measured by Tinnitus Reaction Questionnaire (TRQ), which assesses 26 domains of tinnitus impact on quality of life. The TRQ yields an aggregate score between 0 and 104, with a score of 17 or higher regarded as clinically significant disturbance. Solid bars denote TRQ score means for patients (n=19) receiving the standard two-stage treatment protocol, with error bars corresponding to one standard deviation. Sizable changes were evident after 2 months, with further changes continuing through to 12 months. |
Noting that these studies have proven the short-term benefit of the Neuromonics Tinnitus Treatment, Sinopoli says the next study will examine the long-term outcome. “We will be starting up the multisite CALM study—Customized Acoustic stimulus for Long-term Medical benefits—that will review patient results over 36 months in a variety of patient settings, including ENT clinics and universities,” Sinopoli says.
QUALITY OVER CURE
The study will reflect the treatment’s potential use. Currently, there are more than 100 locations in the United States providing Neuromonics Tinnitus Treatment, according to Sinopoli. The company aims to expand that number to 200 or more over the next few months.
The goal of the treatment, no matter the setting, is to reduce the physical, mental, and emotional disturbance perceived by the patient as a result of tinnitus. Neuromonics measures this experience using the 26-item TRQ. “About 90% of patients have at least a 40% reduction in their TRQ score,” Hanley says.

|
| The Neuromonics Oasis is a Class II wired device for treating tinnitus. |
The score does not necessarily reflect a change in the symptoms of the tinnitus, but in the patient’s quality of life. Neuromonics does not claim to cure tinnitus with its treatment, but rather to reduce the distraction tinnitus causes by making the sufferer less aware of the noise.
The treatment addresses the audiological, psychological, and neurological aspects of tinnitus, incorporating five stages: comprehensive personalized assessment, processor configuration, preconditioning stage, active treatment stage, and maintenance stage.
During the assessment phase, a comprehensive profile of the patient’s hearing loss and tinnitus is compiled. This information is used to develop a customized audio profile—comprising music and a neural stimulus—that is programmed into the patient’s Neuromonics processor. Similar in size to an MP3 player, the device delivers the acoustic portion of the treatment in stereo through headphones; its frequency range is 100 Hz to 12.5 kHz.
During the preconditioning phase, the audio program includes an acoustic neural stimulus with varied intermittent intensity, designed to provide relief from the tinnitus symptoms by masking them. The interaction with this stimulus is then reduced during the active treatment stage so that the brain is exposed to the tinnitus sounds intermittently and is trained to filter them out.
The company offers a 4-hour selection of different types of music to combine with the stimulus to give patients some choice, control, and consistency. “It needs to be familiar to fit into the background of the conscious mind rather than requiring the active listening process,” Hanley says.
|
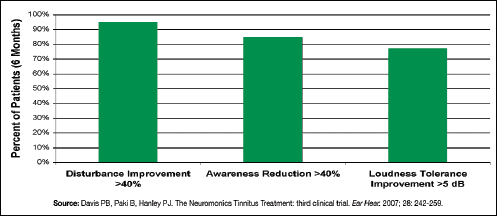
| Figure 2. Consistency of benefit reported for tinnitus disturbance, for which a successful outcome is defined as an improvement of at least 40%, is measured by TRQ, as well as for tinnitus awareness (a reduction of at least 40%) and loudness tolerance (an improvement of at least 5 dB as measured by Loudness Discomfort Levels (LDLs), among those whose pretreatment LDLs were averaged less than 85 dB). |
This happens naturally as patients listen to the device for at least 2 hours every day. The audio program is intended for use while completing other tasks, but does not need to be worn for extended periods. Hanley contrasts this to the 10 to 12 hours required for hearing aids and maskers.
Once patients are desensitized to the disturbances, they have entered the maintenance phase—typically about 6 months into therapy. They can reduce listening sessions to suit their needs. Some patients will not need to use the device at all; others may continue to listen for abbreviated periods daily.
The device can help patients to regain a sense of control as well as help relax them. “The emotional response can be the most significant driver behind tinnitus response, and the music used in the program can contribute relaxation benefits in addition to the auditory retraining. This in turn can drive acceptability as well as compliance,” Hanley says.
|
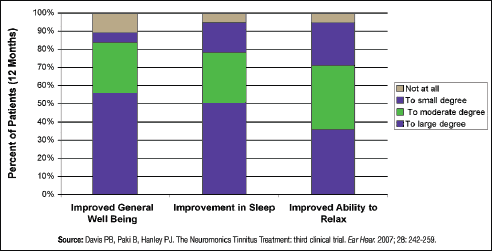
| Figure 3. Consistency of benefit reported for general well-being, sleep, and relaxation. On each dimension, at 12 months after commencing treatment, patients (n=19) rated the degree to which each benefit applied to them. These are displayed as percentages of all respondents. |
THE BALANCING ACT
Patients without the ability to meet the 2-hour listening requirement would not be recommended for Neuromonics Tinnitus Treatment. Other contraindications include fluctuating hearing loss (“We can’t tailor treatment to a moving target,” Hanley says), severe hearing loss, and inability to self-administer the treatment. It is also not advised for patients who cannot eliminate exacerbating factors “such as working in loud environments without proper ear protection,” Hanley says. “We’ve also seen poor responses in patients with unrealistic expectations,” Hanley adds.
The ideal patients are adults with a moderate to significant level of tinnitus disturbance who can organize themselves for daily treatment, Hanley says. Patients must purchase the Neuromonics device, but because it is a medical treatment, it may be covered by insurance, at least in part. Hanley compares the cost of treatment cost to that of a high-level hearing aid.
Audiologists who offer the treatment must attend a 2-day training workshop that reviews the known facts about tinnitus and its treatment as well as the techniques and procedures for using the Neuromonics system. The company also provides support for clinicians treating their first few patients.
Most patients are monitored for the first couple of weeks or months after beginning treatment to assure proper use. The device features data usage logs that can record whether the patient is using the treatment properly.
One challenge has been to balance the high degree of customization with the need to keep the program easy to administer. “The acoustics and counseling approach is tailored to the patient, but the number of clinical hours required to administer [Neuromonics] treatment is fewer than that for programs with more intensive counseling aspects,” Hanley says.
Hanley notes that development of the treatment has sought to address the limitation of other methods, and it has succeeded in many aspects. The Neuromonics Tinnitus Treatment has found a more effective way into patients’ heads than has been achieved through more traditional methods.
Tin Ear
Tinnitus is not a cause but a symptom, and a potentially debilitating one. Often, treatment focuses on reducing the disturbance caused by the sound the sufferer hears, but in some cases the origin of the problem may be alleviated, reducing the tinnitus complications.
|
For more information |
Potential causes of tinnitus include noise-induced hearing loss; wax buildup in the ear canal; toxins, including medications and chemotherapy; ear and/or sinus infections; jaw misalignment; cardiovascular disease—often experienced as pulsatile tinnitus; tumors; head and neck trauma; hypo- and hyper-thyroidism; Lyme disease; fibromyalgia; thoracic outlet syndrome; and Meniere’s disease.
“There can be any number of causes, but tinnitus is a fairly consistent series of neurological events that lead to perceptions of sounds and the potential associated mental and emotional disturbances,” says Peter Hanley, director and CEO of Neuromonics Inc, Chatswood, Australia.
When the sound is enough of a disturbance, patients will seek help, typically seeing an ENT or otolaryngologist first. Once medical conditions have been ruled out, the patient is referred to an audiologist for treatment.
According to the American Tinnitus Association (ATA), Portland, Ore, treatment options include amplification (hearing aids), biofeedback, cochlear implants/electrical stimulation, cognitive therapy, drug therapy, sound therapy, temporomandibular joint treatment, and alternative options such as acupuncture, craniosacral therapy, herbal preparations (eg, ginkgo biloba), hyperbaric oxygen, hypnosis, magnets, minerals (magnesium or zinc), and vitamins in the B family. The ATA does not recommend any particular method.
—RD
Renee Diiulio is a contributing writer for Hearing Products Report. For more information, contact [email protected]




