A good reminder for all of us involved in hearing care is that, if hearing aid technology is effective (or ineffective) for a particular individual’s unique hearing needs, then it is our responsibility to measure it, identify it as useful or useless for that patient, and prescribe the hearing solution accordingly.
Digital hearing aids have made considerable strides in technology in the past few years, and advanced digital features are being routinely added to amplification devices to increase market penetration.1 However, it is critical for hearing care professionals not only to fit patients with the most appropriate digital technology, but also to constantly evaluate the effectiveness of such technology to ensure success in dispensing. Successful use and acceptance of digital amplification can be achieved only if we use our professional skills to fit suitable technology and evaluate real-world performance of the devices.
If digital hearing instrument features are available and recommended for individual listeners, then why are we so reluctant to measure the effectiveness of these features? Hearing aid analyzers with couplers, specialized protocols, and signals are needed to measure hearing aid effectiveness. Likewise, probe microphone equipment for real-ear measurements are often unavailable or go unused in dispensing clinics. It is amazing that many dispensing professionals—including recent audiology graduates—feel that coupler and real-ear measurements are “ancient practice” or “graduate school stuff!” The literature proves otherwise.
However, the gravest issue to consider is if we, as professionals, are unable to convince ourselves first that high technology in hearing aids is precise, accurate, and really works. If not, then how can we ever hope to convince our patients? The following illustrations are provided to show the effectiveness (or lack thereof) of some hearing aids measured in our laboratory.
Measuring Hearing Aid Performance
Multichannel compression. It is safe to conclude that all manufacturers of today’s digital hearing instruments offer some kind of multi-channel compression. Programmability of static (eg, kneepoint and ratios) and dynamic (time constants for attack and release) compression parameters provides us with solutions to deal with recruitment problems and restrict the noise in specific frequency regions for individual hearing aid wearers.2 While there is still debate on how many channels are required for compression in hearing-impaired listeners, there is little doubt that multiple frequency channels for compression can offer loudness normalization for individual listeners for soft (eg, 50 dB), medium (eg, 65 dB), and high (eg, 80 dB) inputs.
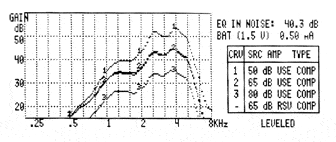
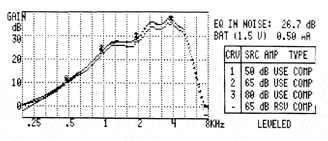
FIGURE 1. The effectiveness (top) versus the ineffectiveness (bottom) of a compression system as measured in a 2cc coupler. Curve 1 was obtained at 50 dB input, Curve 2 was obtained at 65 dB input, and Curve 3 was obtained at 80 dB input. |
A simple coupler measurement may be useful to verify the effects of compression across the frequency range for a hearing aid. As shown in Figure 1a, the compression characteristics of a hearing aid were evaluated in a 2 cc coupler of a Frye 6500 analyzer for 50 dB, 65 dB, and 80 dB inputs. Note the gain of the hearing aid adaptively decreased as the input changed from 50 dB to 65 dB to 80 dB. Figure 1b shows the ineffectiveness of compression in another hearing aid where gain remained the same regardless of input level.
Harmonic distortion. Harmonic distortion measurements are measured by pure-tone inputs into a hearing aid followed by analysis of the distortions in the output signal.3 Most standards (eg, ANSI 2003) specify that distortion be measured with a moderate (eg, 70 dB input) for a hearing aid set at reference test gain setting.4,5 Figure 2 shows the performance profile of a hearing aid measured for harmonic distortion at moderate (70 dB) and maximum output at loud (90 dB) inputs. The low distortion values have implications for good sound quality.
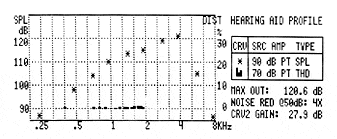
FIGURE 2. Harmonic distortion characteristics measured in a 2cc coupler.
Live speech mapping. Live speech mapping involves a real-ear measurement (probe tube placed in the ear canal) in the aided condition and can be useful as a counseling/demonstration tool to show how live speech (own voice or spouse’s voice) is perceived by the patient or influenced by the hearing instrument. Live speech mapping can be done in most probe microphone systems in the spectrum (sound level meter) mode by turning the sound source off. This setting disables the loudspeaker from being the source during real-ear measurements and makes the probe microphone live for purposes of speech mapping.
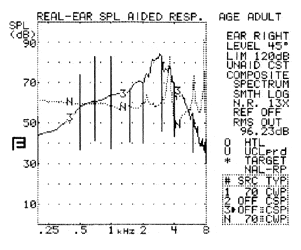
FIGURE 3. Live speech mapping using real-ear.
Figure 3 shows live speech mapping conducted with the high frequency speech sound /sh/. The significant gain in the high frequencies in the aided (see “Curve 3”) condition verifies that the hearing aid is amplifying the high frequencies needed for audibility of this sound. Similar gains in the lower frequencies for the vowel /a/ can be seen in Figure 4 (see “Curve 2”). Such live speech measurements can also serve as a patient demonstration tool.
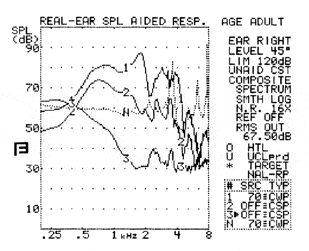
FIGURE 4. Occlusion effect measured using real-ear, where “N” is the unaided condition. Curve 1 represents the aided composite, Curve 2 is aided live speech, and Curve 3 represents the occlusion effect.
Occlusion effects. Occlusion effects are characterized by descriptions of people with low frequency thresholds less than 40 dBHL who complain that, when their ear canal is occluded by an earmold or shell, their voice sounds like it is hollow, boomy, echoic, or coming from inside a tunnel.3 The occlusion effect can be measured by placing a probe microphone in the ear canal and having the user vocalize a vowel (eg, /i/) with their hearing aid in the ear canal but turned off.6,7
Figure 4 shows the occlusion effects of a tight-fitting earmold (see “Curve 3”). Real ear measurements can be useful measures of not only the occlusion effect in patients but also useful measures of the effectiveness of solutions used to overcome this problem (eg, venting, open ear canal fitting, etc). For example, the occlusion effect measured in Figure 5 could be replaced by an open-ear instrument or a vented earmold to compare the possible benefits.
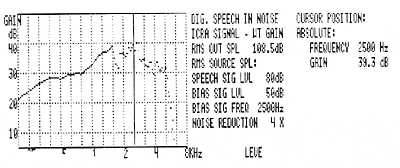
FIGURE 5. Digital noise reduction measured in a 2cc coupler.
Digital noise reduction. Modern digital aids use modulation detection strategies to attempt to differentiate modulated (speech-like) from unmodulated (noise-like) signals. Figure 5 shows the gain of a digital hearing aid measured in a 2cc coupler for concurrent signals—a modulated (interrupted digital speech) signal and an unmodulated (steady bias tone) on a Frye hearing aid analyzer. Such measurements are useful to measure adaptive gain changes in the output of digital instruments to simulate approximate “speech in noise” performance.
| Sridhar Krishnamurti, PhD, is an associate professor of audiology at Auburn University, Auburn, Ala. |
Acknowledgments
The author acknowledges the equipment support provided by Frye Electronics Inc for measurements reported in this study.
Correspondence can be addressed to HR or Sridhar Krishnamurti, Auburn University, Dept of Communication Disorders, 1199 Haley Center, Auburn, AL 36849; email: [email protected].
References
1. Kochkin S. MarkeTrak VII: Hearing loss population tops 31 million people. The Hearing Review. 2005;12(7):16-29.
2. Sweetow R. Selection considerations for digital signal processing hearing aids. Hear Jour. 1999;51(11):35-42.
3. Dillon H. Hearing aid earmolds, earshells, and coupling systems. Hearing Aids. New York: Thieme; 2001.
4. Frye Electronics Inc. Workbook for ANSI measurements. Available at: http://frye.com/manuals/ansi03workbook.pdf; Accessed: Dec 2005.
5. Frye GJ. Understanding the ANSI standard as a tool for assessing hearing instrument functionality. The Hearing Review. 2005;12(5):22-27,79.
6. Chung K. Feedback and occlusion effect reduction strategies. Trends Amplif. 2004;8(4):147-150.
7. Mueller HG. There’s less talking in barrels but the occlusion effect is still with us. Hear Jour. 2003;56(8):10-16.





