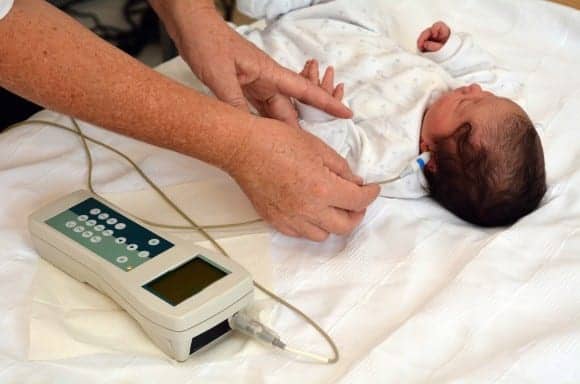
The August 24 version of the Morbidity & Mortality Weekly Report (MMWR) from the US Centers for Disease Control and Prevention (CDC) highlights the benefits of and gaps in assessing point-of-care newborn screening for hearing loss (HL) and critical congenital heart disease (CCHD), the CDC announced on its website. The CDC believes that these critical gaps need to be closed to help all children have a better chance to reach their full potential.
About 1 in 500 infants are born with CCHD, which includes the more severe forms of congenital heart disease (CHD). According to the CDC, CHD is the most common type of birth defect and accounts for more than 30 percent of all infant deaths from birth defects. Point-of-care screening can help identify many infants with CCHD before they go home.
Newborn screening, a public health program that benefits 4 million US infants every year, identifies conditions that can affect a child’s long-term health or even survival. Besides laboratory testing of dried bloodspots for dozens of conditions, which has been in place since the 1970s, national guidelines now call for newborns to be screened for hearing loss and CCHD while at the birth facility.
“Newborn screening at birth is crucial to quickly identify infants at risk of hearing loss and congenital heart disease so they can receive early intervention and follow-up care,” said CDC Director Brenda Fitzgerald, MD. “Finding these conditions early can give infants the best chance to properly develop and lead healthy lives.”
CDC estimates that without newborn screening, each year about 875 US newborns with a CCHD were not diagnosed before discharge from birth facilities. However, most of these babies can now be identified using a non-invasive and painless test referred to as “pulse oximetry testing.” For every 200 infants with CCHD, at least one death due to an undiagnosed CCHD can be avoided if all birth facilities screen newborn babies using pulse oximetry testing.
Similarly, permanent hearing loss present at birth affects nearly 2 infants per 1,000 in the United States. According to the CDC, most children with hearing loss are considered to have or be at risk for a developmental delay. Infants who are diagnosed before 3 months and receive intervention services before 6 months have significantly better language development than children who are not.
Federally-funded, state-based Early Hearing Detection and Intervention (EHDI) programs help ensure infants receive recommended diagnostic and intervention services. In short, EHDI focuses on nationally recognized “1-3-6” guidelines: children are screened for hearing loss before 1 month of age, and, if needed, diagnosed for hearing loss before 3 months and enrolled in early intervention programs before 6 months.
In contrast to EHDI, there is no federal support for state-based CCHD screening programs. Not detecting heart-related birth defects early can pose a significant increase in risk for permanent disability and even death.
“The collaboration between EHDI programs, health professionals, and parents has led to great progress on hearing loss screening and follow-up,” said Stuart K. Shapira, MD, PhD, chief medical officer and associate director for science at CDC’s National Center on Birth Defects and Developmental Disabilities. “We must apply the same effort and resources to CCHD screening to help prevent infant deaths and offer children the greatest chance to thrive.”
This MMWR complements the September 2016 Public Health Grand Rounds forum Beyond the Blood Spot: Newborn Screening for Hearing Loss and Critical Congenital Heart Disease.
To read the article, visit MMWR homepage.
Visit CDC’s website to learn more about hearing loss in children and birth defects of the heart.
For a video summary of the MMWR findings:
Beyond the Blood Spot: Newborn Screening for Hearing Loss and Critical Congenital Heart Disease
Original Paper: Grosse SD, Riehle-Colarusso T, Gaffney M, et al. CDC grand rounds: newborn screening for hearing loss and critical congenital heart disease. Morbidity and Mortality Weekly Report. August 25, 2017; 66(33):888–890.DOI: dx.doi.org/10.15585/mmwr.mm6633a4
Source: CDC, Morbidity and Mortality Weekly Report