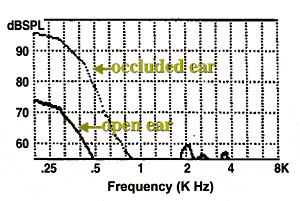
The aided sound-field threshold (ASFT) represents the softest sound that the wearer can hear inside the audiometric test booth when using a hearing aid. For a wide dynamic range compression (WDRC) hearing aid without a volume control (VC), the aided threshold approximates the softest sound that the wearer hears in real-life listening situations.1 This perceptual index reflects the “audibility of sounds” to the hearing aid user.
Especially for children, the audibility of sounds is the foundation for language acquisition and all learning. This unique property makes the ASFT one of the most commonly used measures in cochlear implant and middle-ear implant evaluations. In hearing aids, nearly 80% of audiologists who work in an educational setting routinely measure this index to verify/validate their hearing aid fittings.2 It is important that this index be obtained as reliably as possible and the results interpreted as accurately as possible for its maximum utility. Kuk & Ludvigsen1 provided a description of the meaning of this index. In this article, we examine the reliability of this index as ASFTs are measured on nonlinear hearing aids.
Reliability refers to the changes or fluctuations in threshold responses within a test session or between test sessions. A good clinical tool must be reliable to be useful. Unfortunately, previous reports on the reliability of the ASFTs have been unfavorable. Hawkins et al.3 showed that the between-session standard deviation (SD) of the ASFTs measured on linear hearing aids was about 6-8 dB. This suggests that the “true” measured ASFT may differ from the measured value by 12-16 dB (ie, 2 times standard deviation at 95% confidence interval). Another general interpretation is that any two ASFT measurements must be 12-16 dB different from each other in order to consider them statistically significant (with a 5% error rate). On the other hand, Humes & Kirn4 reported a standard deviation of 4-6 dB. In their study, more variation was reported in the high frequencies than in the low frequencies. With the advent of nonlinear hearing aids—which could potentially introduce more variability in the measured ASFT—it is no surprise that the utility of this index as a validation/verification tool has been questioned.5
A Second Look at ASFTs
Despite the potential questions surrounding the reliability of ASFT measures, there is no evidence supporting the speculation that the ASFTs obtained on nonlinear hearing aids are more variable than those obtained on linear hearing aids. In addition, precautions may be exercised to minimize variability. For example, Kuk6 recommended that, in measuring the ASFT, one should use a modulated sinusoid that is longer than the attack time of the compression hearing aid (which is typically less than 1 s in duration) and an inter-stimulus interval that is longer than the duration of the release time (which is typically less than 1-2 s, but in some hearing aids, may be as long as 20 s).
In order to prevent abrupt changes in gain characteristics, a 5-dB step ascending approach was recommended instead of the typical bracketing approach set forth in ASHA’s 1978 guidelines for manual puretone threshold audiometry.7 In the following study, the validity of this approach in minimizing the variability in ASFT was evaluated by comparing the standard deviation of the unaided sound-field thresholds (USFT) and the ASFT. Presumably, this approach may be considered acceptable if the reliability of the USFT and ASFT is similar.
Methods
Study Participants. A total of 12 listeners who had participated in previous studies at our research office were recruited. These participants varied in age from 32-82 years with a mean of 61.3 years. Eight of these participants had worn hearing aids for 1-21 years, while 4 were first-time wearers. However, all participants had worn the study hearing aids for at least one month prior to the study. All were native speakers of English. The hearing loss in all the listeners was sensorineural and symmetrical (±10 dB) in nature. Figure 1 shows the audiograms averaged between the left and right ears of each listener.
Hearing Aids. The 12 subjects were fit binaurally with Widex Senso Diva hearing aids. In order to generalize the findings to all hearing aid styles, behind-the-ear (BTE), in-the-canal (ITC), and completely-in-the-canal (CIC) styles of hearing aids were each used by 4 subjects. The aids were fit with a vent diameter based on the degree of hearing loss at 500 Hz. A vent diameter of 2 mm was used for those with less than 30 dB HL at 500 Hz. Every 10 dB increase in hearing loss resulted in a 0.5 mm decrease in vent diameter.
The study hearing aid is a 15-channel WDRC hearing aid that uses in-situ threshold measures (sensogram) at 500 Hz, 1000 Hz, 2000 Hz, and 4000 Hz to determine the wearer’s unaided thresholds. An expanded sensogram which allows in-situ threshold measures at 14 of the 15 channels may be conducted for listeners with atypical audiometric configurations. Channels covering the speech frequencies (500 Hz to 4000 Hz) were approximately 1/3 octave in bandwidth, while the lower and higher frequencies were broader in bandwidth (about 2/3-octave wide). Unaided in-situ threshold (sensogram) values were used to specify gain settings on the study hearing aids.
The Senso Diva has several adaptive processes that may introduce variability in the measured ASFTs. This includes the adaptive active feedback cancellation system, the automatic adaptive directional microphone, and the adaptive noise reduction algorithm. In addition, the slow-acting compression used by the hearing aid may also introduce measurement errors if care is not taken during threshold measurement. Consequently, during the ASFT measurements, the Senso Diva hearing aid was put in one of its four possible test modes (Test Mode 2) in which the noise reduction and the active feedback cancellation algorithms were deactivated, an omnidirectional microphone was used, and fast attack and release times were used. This test mode is recommended for measuring the frequency-output characteristics or determining the ASFTs of the study hearing aid. Effectively, this changed the Senso Diva into a fast-acting WDRC hearing aid.
Procedure. All testing was conducted in a double-wall sound-treated booth (Industrial Acoustics) that measured 10’ x 10’ x 6’6”. In addition, fabric-wrapped panels were installed on the upper half of the internal walls for acoustic and cosmetic purposes. The reverberation time of the booth was less than 0.1 s above 500 Hz. Participants were seated one meter directly in front of the test loudspeaker (Cerwin-Vega). The measured ambient noise was lower than 55 dB-C and less than 10 dB SPL in all 1/3-octave bands above 200 Hz throughout the course of the study.
During a session, the participants’ sensogram was first measured along with the unaided sound-field thresholds (USFT) and aided sound-field thresholds (ASFT). Thresholds were measured at 500 Hz, 1000 Hz, 2000 Hz, and 4000 Hz each three times within a session. The sequence in which the sound-field threshold measures were conducted was counterbalanced. In addition, the test frequencies were also counterbalanced.
Unaided sound-field thresholds were measured using the GSI-61 clinical audiometer and Cerwin-Vega loudspeakers. Warble tones (5%) with a modulation rate of 5 Hz were used as stimuli. The audiometer/sound-field system was calibrated at the 0° azimuth following ANSI (1996) recommendations.8 To minimize listener movement, a loudspeaker stand was modified so that a piece of foam that measured 3 inches by 6 inches was placed behind the listener’s head as a stabilizer. Study participants were instructed to keep their heads in contact with the foam stabilizer during the sound-field threshold measure. Walker et al.9 recommended fixing the head during sound-field measures to minimize variability. A modified method of limits (ASHA 1978 guidelines7) was used to bracket the USFT. USFTs were determined one ear at a time. The non-test ear was occluded with an EAR foam plug and then covered with the supra-aural headphone to ensure non-participation of that ear. All study participants were given the same instructions:
The purpose of this study is to determine how soft you can hear some beeping sounds of different pitches. As an example, these are the sounds that I am talking about (demonstrate), except that they will be very soft. Raise your hand when you hear them, even though it may be very faint and barely audible. Lower your hand when you don’t hear the beeps. Try not to move your head or your body at any time during the test. We will start with the right ear, followed by the left ear (when appropriate).
Aided sound-field thresholds were measured using the same equipment, set-up, and instructions as in the USFT measurement. The mean sensogram measured from the average of 3 trials within a session was used to specify the hearing aid setting. The hearing aids were set to Test Mode 2 during ASFT measurement.
Three special precautions were taken in order to minimize any variability in ASFTs that may originate from the attack/release time of the hearing aids6:
1) For a stable output, the duration of the warble stimuli was fixed between 1-2 s to ensure that it exceeded the attack time of the hearing aid.
2) Rather than using a bracketing approach, a 5-dB ascending approach was used to reach the threshold estimate once the vicinity of the listeners’ thresholds were known. For example, testing would start at 25 dB HL in 5 dB steps if it was known that the listeners’ aided thresholds were around 30 dB HL. The attenuator dial would be increased in 5 dB step until a threshold response was indicated. This dial setting was recorded. This was followed by the dial being decreased in 5-dB steps until no response was indicated; then the dial was increased until a reliable response was indicated again. The dial settings where thresholds were first indicated were averaged to yield the ASFT.
3) The inter-stimulus interval was timed to be around 30 s for complete gain recovery on the hearing aid before the next stimulus presentation. This minimized variability resulting from the release time of the nonlinear hearing aids. ASFT was measured one ear at a time and three times for each frequency. The non-test ear was occluded by the hearing aid in the “off” position. A supra-aural headphone was also placed over this ear to provide additional sound insulation.
Study participants returned in approximately 2 weeks with the study hearing aids to have their sound-field thresholds measured at each of the four frequencies. Prior to the measurements, the listeners’ ears were examined otoscopically and they were asked if they noticed any changes in their hearing sensitivity during the past 2 weeks. The listener would be disqualified for the study if they indicated changes in their hearing or that their sensogram thresholds deviated by more than 10 dB from the previous session. None of the listeners were disqualified.
The clinical audiometer and the associated transducers (including headphones, sound-field loudspeakers) were calibrated on a monthly basis following ANSI 1996 guidelines.8 The audiometer was calibrated between the first and second session. A listening check was performed daily prior to the experimental session. The integrity of the listeners’ study hearing aids were also confirmed with electroacoustic evaluation according to ANSI standards10 prior to each session.
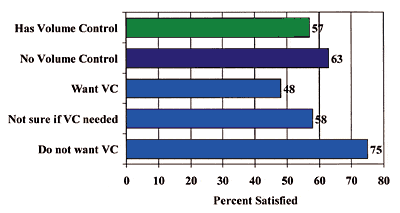

Figure 2. Within-session reliability of unaided (USFT) and aided (ASFT) sound-field thresholds estimated by the percentage of responses showing a criterion within-trial deviation in threshold (threshold difference of 0 dB and 5 dB between largest and smallest threshold estimates). |
Results
Within-Session Reliability. In order to assess the within-session reliability, we counted the number of instances in which the largest and smallest threshold estimates within a trial deviated by a specific criteria (0 dB, 5 dB, or 10 dB). The number of instances for each criterion deviation was summed for both ears and for both visits since there was no statistical difference between ears or between visits. Finally, the proportion of time each criterion deviation occurred was calculated by dividing the frequency of a criterion deviation by the total number of counts for all deviations.
Figure 2 summarizes the proportion of each deviation for each test frequency for the unaided and aided sound-field thresholds. It shows that the majority of listeners were consistent in their within-session threshold responses. Between 60% and 70% of listeners showed no difference (ie, 0 dB difference) in their threshold estimates. All subjects showed a 5 dB within-session variation. A similar conclusion can be drawn from the ASFT measurement results. No deviation in threshold estimates was seen in 60%-70% of the listeners. Only 1 person showed more than a 5 dB difference. This suggests that the within-session reliability of the sound-field thresholds is comparable to the step size (5 dB) used during threshold estimation. Furthermore, it suggests that the within-session reliability of the USFTs is similar to that of the ASFTs.
Between-Session Reliability. The between-session reliability can be estimated by comparing the absolute difference in thresholds between Visits 1 and 2 and the standard deviation of the difference between sessions. Figure 3 shows the averaged absolute threshold difference between sessions among listeners averaged between ears for both the aided and the USFT measures. Figure 4 shows the standard deviation of the threshold difference between sessions for the same measures. For the unaided sound-field threshold, the absolute difference in threshold between sessions was between 1.9 dB and 2.3 dB, with a standard deviation between 2.55 dB and 3.28 dB across frequencies. This suggests that 95% of listeners will show a test-retest difference of less than 5 dB-6.5 dB.
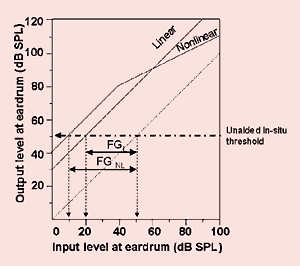
A similar observation was also seen with the ASFTs. The absolute between-session threshold difference was between 1.7 dB and 2.8 dB across frequencies, with a standard deviation between 2.8 dB and 3.6 dB across frequencies. This suggests that 95% of listeners will show a test-retest difference of 5.6 dB to 7.2 dB. These results showed that there is no difference in test-retest threshold difference between the USFT and ASFT at any of the test frequencies.

Comparisons to Other Studies
This study compared the within-session and between-session reliability of the unaided sound-field thresholds (USFT) with the aided sound-field thresholds (ASFT) measured with a nonlinear hearing aid. The results showed similar reliability between the two sound-field threshold measures. Under the present test conditions, the reliability of the aided sound-field thresholds was not affected by the processing of the nonlinear hearing aids.
Compared to previous studies, the findings from this study showed higher reliability for both the unaided and aided sound-field threshold measures. For example, Byrne & Dillon11 reported a test-retest standard deviation of 4.6 dB on the USFTs when their subjects were tested again in 24 hours. Humes & Kirn4 reported a test-retest standard deviation of 4-6 dB on the USFTs when subjects were retested in 10 minutes and in 2 weeks. Higher variability was seen at 4000 Hz than at 250 Hz. Both studies reported a higher standard deviation than that seen in this study, which varied between 2.5 dB and 3.3 dB across frequencies upon a 2-week retest.
Large variability was also reported on the ASFTs even with linear hearing aids. Hawkins et al.3 instructed their subjects to listen to a 70 dB SPL discourse passage and adjust the VC on the hearing aids to a comfortable listening level prior to ASFTs. These authors showed a between-session standard deviation of 6-8 dB. This magnitude of standard deviation would suggest that two aided thresholds must be different by 12-16 dB to be considered statistically different (p < 0.05). On the other hand, Humes & Kirn4 reported a lower standard deviation of 4-6 dB when their subjects were not allowed to adjust the VCW on the linear hearing aid. These researchers concluded that the variability seen in the use and processing of the linear hearing aids resulted in the higher SD with the ASFT measure than with the USFT measure.4 Similarly, Stuart et al.12 showed test-retest standard deviation of 3-5 dB across frequencies when measuring the ASFT in children 5-14 years of age.
The present study showed a standard deviation of 2.8 to 3.6 dB in the ASFT measures. This means that 95% of the test-retest variation of the ASFT will be 5.6 dB-7.2 dB (around 1 step size), significantly smaller than what had been reported. It is noteworthy that this magnitude of variability was obtained with a nonlinear hearing aid, and that this deviation is not significantly different from that of the USFTs. In other words, despite the potential increase in variability with the use of a hearing aid—and especially a nonlinear hearing aid—the variability may be circumvented.
Factors Affecting ASFTs
One of the main reasons for the higher reliability in the sound-field thresholds measured in this study is that many factors that affect them were circumvented by the study design. In other words, the present finding should be regarded as the “best case scenario” and may not be typical of clinical experience. However, with a little extra care (as was shown in this study), it is possible to minimize the variability and achieve relatively reliable ASFTs.
The following is a list of factors that could affect the reliability/validity of sound-field thresholds and what we did in the present study to minimize its impact.
• Noise. Ambient noise in the test environments may act as maskers, raising the level of the aided and/or unaided thresholds, especially for signals below 500 Hz. This becomes more problematic for fluctuating noise. Furthermore, Macrae & Frazier13 and Hawkins14 also pointed out that circuit noise from hearing aids could impose a floor effect on the aided threshold. Listeners with normal hearing or a mild hearing loss in the low frequencies would be most susceptible to this masking. The aided thresholds measured in these frequency regions should be interpreted carefully. Test rooms for conducting sound-field testing must be free from any extraneous noise sources. In the current study, the overall ambient noise floor was measured at 50 dB SPL-C with each 1/3-octave band measuring lower than 10 dB SPL above 200 Hz.
• Standing waves. Because most test environments are enclosed, standing waves will likely develop from reflections off the walls of the test booth. To overcome such an occurrence, frequency modulated (5% at 5 Hz) pure-tones (or warble tones) were used as the test stimuli because they cover a narrow frequency region and are less susceptible to room resonance. Furthermore, in the present study, fabric-wrapped panels were used in the test booth to minimize reflections.
• Head and body movement. Any movement by the test subjects during sound-field measure would change the acoustic input to the ear and result in threshold shifts. The effect is more significant in the higher frequencies because of their shorter wavelengths. In this study, we asked subjects to keep the back of their heads in contact with a head-pad to reduce any head or body movements. This minimized variability in the high frequencies. Indeed, in this study, the test-retest reliability at 4000 Hz was not significantly different from the lower frequencies. Higher variability in USFT and ASFT in the high frequencies was frequently reported in previous studies.4
• Nonlinear hearing aids. ASFTs may have higher variability than USFTs because a difference in positioning of the hearing aid between trials could add to variability. Nonlinear hearing aids may add even more variability between trials because of their changing gain characteristics over time. Consequently, the attack and release times of such hearing aids could interact with the stimuli and affect the measured aided thresholds. Some nonlinear hearing aids have test modes in which many of the adaptive/digital features are scaled down or disabled. This may reduce variability.
The typical bracketing approach (ie, ASHA guidelines)7 used in threshold estimation may yield more variable results in a nonlinear hearing aid with long time constants and low compression thresholds (CT). This is because the recommended bracketing approach involves relatively large intensity change (and thus potential gain change) between stimulus presentations (eg, up 10 dB and down 5 dB, or 15 dB in each “bracket”). While stimulus levels that are below the CT may not introduce output uncertainty (ie, because compression is not activated), those at or above the CT of the hearing aid may introduce output uncertainty, depending on the time constants of the hearing aids and the temporal characteristics of the stimuli. To minimize the impact of the fluctuation in the input, one may present stimuli in an ascending manner in 5-dB steps once the vicinity of the aided threshold is known. This minimizes unpredictable gain swing and the associated variability in the ASFT measure. This step was used in the current study.
The duration of the stimulus (above the CT) could interact with the attack time of the nonlinear hearing aid and affect the aided threshold. Kuk & Ludvigsen1 illustrated that a nonlinear hearing aid with a short attack time may result in a higher (or poorer) aided threshold than one using a longer attack time when the duration of the stimulus is longer than the attack time of the hearing aids. Thus, two hearing aids with identical I/O characteristics could yield different aided thresholds if they are significantly different in their attack times. Given that most WDRC hearing aids use a relatively short attack time (less than 10 ms), a stimulus that is about 1-2 s in duration is more than sufficient to obtain a consistent aided threshold. The present study set the hearing aids in a “fast-acting” mode in which a fast attack time was used (2 ms). Nonetheless, the duration of the stimulus was purposely set to 1 to 1.5 s for consistency.
The interval between stimulus presentations could interact with the release time of the nonlinear hearing aid to affect the reliability of the aided thresholds. Consecutive stimuli may be presented at different stages of the gain-recovery phase of the hearing aid. This means that two stimuli presented close to each other may potentially receive different gain. This could lead to variable aided thresholds. To minimize this source of variability, one should wait for the duration of the release time before presenting the next stimulus. In this study, the inter-stimulus interval was 30 sec—longer than the longest release time of the hearing aid in order to minimize any incomplete gain recovery.
Any extraneous sounds in the test-booth, or even the subjects’ verbal response to the test stimulus could decrease the gain on the hearing aid and lead to an elevated threshold. A non-verbal task, such as hand-raising (or pressing a button) is preferred.
Suggestions for Measuring ASFTs
The present study showed that the reliability of the ASFTs in nonlinear hearing aids may be better than what one anticipates—if care is taken to measure them. One should remember the following precautions in order to ensure maximum reliability of the ASFTs:
1. Always conduct sound-field measurements in a quiet, minimally reflective sound-booth.
2. Use standardized instructions for all listeners.
3. If a VC is present on the hearing aid, make sure that its position is marked so it may not be intentionally or unintentionally changed during testing.
4. Minimize any potential head and/or body movements of the listeners during threshold determination. Walker et al.15 suggested that keeping the subject’s head in a fixed position would improve the reliability of sound-field measurement.
5. Make sure that the measured aided thresholds are meaningful. The measured aided threshold should be related to the insertion gain for soft sounds on the hearing aid. Likewise, the measured aided thresholds may be elevated (due to the circuit noise of the hearing aid) if:
- The hearing aid has a high circuit-noise level;
- The listener has little or no hearing loss especially in the low frequencies;
- The hearing aid is in a fixed directional microphone mode.
6. Understand the processing of the nonlinear hearing aids in order to circumvent its influence:
- Compression time constants. Use modulated sinusoids that are 1-2 seconds in duration and an inter-stimulus interval that is longer than the release time of the nonlinear hearing aid.
- Noise reduction. Use modulated sinusoids that are shorter than the activation time of the noise reduction algorithm. Typically, stimuli that are 1-2 seconds in duration are short enough for most noise reduction algorithms to remain inactive.
- Active feedback cancellation. Use modulated sinusoids that are shorter than the time required for the feedback system to estimate the feedback path. Typically, a 1-2 second stimulus duration is acceptable. In addition, random inter-stimulus intervals should be used to avoid patterning.
- Directional microphones. The azimuth of the loudspeaker where the test stimuli are presented could affect the magnitude of the aided thresholds. In general, stimulus presented at 0° azimuth will yield better and more consistent aided thresholds in both fixed and adaptive directional microphones. For stimuli presented at other angles, the duration of the stimulus may interact with the adaptation time of the microphone to yield variable results. It is important to check with the manufacturer of the specific adaptive microphones to appraise how the adaptation time of the specific microphone may affect the accuracy and reliability of the ASFT.
A modulated sinusoid that is 1-2 seconds in duration, when coupled with sufficiently long and randomly spaced inter-stimulus intervals, is sufficient to achieve reliable ASFT results in many nonlinear hearing aids today. In addition, it is also possible to set the nonlinear hearing aid in a non-adaptive state in which the noise reduction, feedback cancellation system, and adaptive directional microphones are deactivated. This would also produce reliable results.




|
References
1. Kuk F, Ludvigsen C. Reconsidering the concept of the aided threshold for nonlinear hearing aids. Trends Amplif. 2003;7(3):77-97.
2. Tharpe A, Fino-Szumski M, Bess F. Survey of hearing aid fitting practices for children with multiple impairments. Am J Audiol. 2001;10:32-40.
3. Hawkins D, Montgomery A, Prosek R, Walden B. Examination of two issues concerning functional gain measurements. J Speech Hear Dis. 1987;52:52-63.
4. Humes L, Kirn E. The reliability of functional gain. J Speech Hear Dis. 1990;55:193-197.
5. Stelmachowicz P, Hoover B, Lewis D, Brennan M. Is functional gain really functional? Hear Jour. 2002;51(11):38-42.
6. Kuk F. Considerations in verifying modern nonlinear hearing aids. In: Valente M, ed. Hearing Aids: Standards, Options and Limitations. Second edition. New York: Thieme Medical Publishing; 2002.
7. American Speech-Language Hearing Association. Guidelines for manual pure-tone threshold audiometry. Asha. 1978;20:297-300.
8. American National Standards Institute. American National Standard: Specification for Audiometers. ANSI S3.6-1996. New York: ANSI; 1996.
9. Walker G. Technical Considerations for Sound Field Audiometry. In: Sandlin R, ed. Handbook of Hearing Aid Amplification. Vol. I. San Diego: Singular Publishing Group; 1995:147-164.
10. American National Standards Institute. American National Standard: Testing Hearing Aids with a Broad-Band Noise Signal. ANSI S3.22-1992. New York: ANSI; 1992.
11. Byrne D, Dillon H. Comparative reliability of warble tone thresholds under earphones and in sound-field. Austr J Audiol. 1981;3:12-14.
12. Stuart A, Durieux-Smith A, Strenstrom R. Critical differences in aided sound-field thresholds in children. J Speech Hear Res. 1990;33:612-615.
13. Macrae J, Frazer G. An investigation of variables affecting aided thresholds. Austr J Audiol. 1980;2:56-62.
14. Hawkins D. Limitations and uses of the aided audiogram. Sem Hear. 2004;25(1):51-62.
15. Walker G, Dillon H, Byrne D. Sound-field audiometry: recommended stimuli and procedures. Ear Hear. 1984;5:13-21.