In 1976, James Jerger and Deborah Hayes1 introduced the cross-check principle for pediatric audiometry. This principle can be summed up as “The results of a single test are cross-checked by an independent test measure.”1 The principle has evolved into the centerpiece for adult hearing assessment and hearing aid verification.
The cross-check principle has been utilized throughout the audiological test battery and expanded upon with the introduction of new technologies, such as otoacoustic emissions. This article looks at the use of the cross-check principle in identifying hearing loss, and then applies it to the verification of the hearing instrument fittings.
Identifying Hearing Loss
|
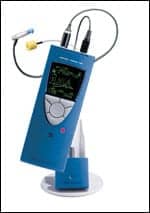
| FIGURE 1. Acoustic immittance is usually the first step in assessing the mechanical integrity of the auditory system. Shown is the MADSEN OTOflex, a full diagnostic immittance unit that includes tympanometry, acoustic reflex, reflex decay, eustachian tube, and fistula tests. |
A test battery is used in the audiological assessment to determine the type and degree of the hearing loss. The test battery assists in ruling out disorders that can be remediated by a physician, such as middle ear effusion or otosclerosis. It also helps the clinician determine if the patient is a candidate for a hearing instrument.
Acoustic immittance. Tympanometry measures the compliance of the tympanic membrane as positive and negative pressure is introduced into the ear. This measure confirms the presence or absence of a middle ear disorder. When combined with audiometry, tympanometry can confirm a conductive hearing loss.
Acoustic Reflex Thresholds measure the contraction of the stapedius muscle when a loud stimulus is introduced into the ear. The results from ipsilateral and contralateral acoustic reflex thresholds have significant diagnostic applications. The pattern of the acoustic reflex response—when combined with results from tympanometry, reflex decay, and audiometry—can assist in confirming the diagnosis of conductive hearing loss, sensorineural hearing loss, eighth nerve tumor, facial nerve disorder, or a lesion in the lower brainstem in the central portion of the reflex arc.
Reflex Decay measures the contraction of the stapedius muscle over time (10 seconds) when a constant loud stimulus is introduced into the ear. The results from ipsilateral and contralateral acoustic reflex decay assists in diagnosing the presence or absence of an eighth nerve tumor. Because of the false positive rate, the reflex decay should always be used in a battery of tests.
Audiometry
Air Conduction puretone audiometry assesses the patient’s ability to respond to stimuli at various frequencies and intensities presented via headphones, insert earphones, or soundfield speakers. This measure determines the degree, type, and configuration of the hearing loss when cross checked with acoustic immittance, bone conduction audiometry, and otoacoustic emissions. If the patient is a candidate for a hearing instrument, the information gathered from this measure also assists in determining the amount of gain needed to make speech audible.
Bone Conduction puretone audiometry assesses the patient’s ability to respond to stimuli at various frequencies and intensities presented via a bone oscillator. When the bone conduction thresholds are better than the air conduction thresholds, the hearing loss is determined to be conductive in nature. Again, the determination of a conductive hearing loss is also confirmed by cross checking these results with those obtained with the acoustic immittance measures.
Speech Threshold audiometry assesses the patient’s ability to respond to speech at various intensities and confirms that the audiometric thresholds obtained are consistent with the speech thresholds.

|
| FIGURE 2. Audiometry includes air and bone conduction testing, speech threshold, and word discrimination testing, as well as determination of UCLs and MCLs. An example is the MADSEN Itera II, a fully adaptable diagnostic audiometer. When paired with OTOsuite software, this system offers an intuitive user interface with efficient Noah interaction and quick access between diagnosis and verification software. |
Similarly, Word Discrimination audiometry assesses the patient’s ability to hear and repeat words at a level above threshold. This level can be a determined level above the speech threshold or a level the patient reports to be most comfortable, or at 65 dBHL (where speech is heard for the listener with hearing within normal limits). This measure gives the clinician an understanding of the patient’s communication performance when speech is delivered at 65 dBHL or when speech is delivered at a level the patient is comfortable listening. The word discrimination score can give some indication of hearing instrument performance.
Most Comfortable Loudness (MCL) level is the intensity at which the patient deems most comfortable for listening to sound or speech. The MCL should be determined for both puretones and speech. MCL levels can assist in setting the gain of the hearing instrument so that speech is audible and comfortable to the patient.
Uncomfortable Loudness (UCL) level is the intensity at which the patient deems uncomfortable or intolerable for listening to sound or speech. The UCL should also be determined for both puretones and speech. UCL levels assist in setting the maximum output of the hearing instrument so that loud sounds are not uncomfortable to the patient.
Otoacoustic Emissions
Distortion Product Otoacoustic Emissions (DPOAEs) and Transient Evoked Otoacoustic Emissions (TEOAEs) assess outer hair cell function of the cochlea by measuring the response produced when a tone or click stimulus is presented to the ear. Otoacoustic emissions should be absent if significant hearing loss is present.

|
| FIGURE 3. Otoacoustic emissions (OAEs) provide dispensing professionals with an analysis of outer hair cell function. The determination of the type of hearing loss is confirmed by cross checking these results with results obtained with the acoustic immittance measures and puretone audiometry. Shown is the MADSEN Capella, which includes screening and diagnostic TEOAE, DPOAE, spontaneous OAEs and screening tympanometry. |
Otoacoustic emissions can be an indicator of auditory neuropathy/neural dysynchrony if present when all other measures indicate a significant hearing loss. It is advisable to rule out the presence of normal outer hair cell function before fitting a patient with amplification. Again, the determination of the type of hearing loss is confirmed by cross checking these results with results obtained with the acoustic immittance measures and puretone audiometry.
Verification of Hearing Instrument Fitting
Once candidacy for a hearing instrument is determined appropriate based on the results of the audiological assessment and a hearing instrument is selected for the patient, verification of the hearing instrument fitting should follow. There are three main goals in hearing instrument verification:
1. Soft speech should be audible.
2. Conversational speech should be comfortable.
3. Loud sounds should be tolerable.
These three goals are at the core of most hearing instrument sound processing strategies; therefore, they should be methodically verified in the hearing instrument by using objective measures.
Modern hearing instruments offer many dynamic features, such as noise suppression, feedback cancellation, and directionality. These features should also be verified and determined to be functioning properly, so that they are offering benefit to the patient.
Surprisingly, the following statistics were reported in 2006 by George Lindley2 of PCO School of Audiology, and similar findings were reported by Gus Mueller3 in a survey conducted in 2003:
1. Informal measures to verify hearing instrument fitting are used by 80% of audiologists.
2. Aided speech recognition to verify the hearing instrument fitting is used by 40% of audiologists (44% in quiet and 56% with background noise).
3. Real-ear measurements are used by 41% of audiologists.
Why aided soundfield testing should always be cross checked. Aided soundfield testing is performed using some of the same measures that were used in the initial audiological assessment, but with the hearing aids on the patient and the stimuli presented in soundfield.
Word Discrimination is often used in several different ways to demonstrate the benefit of amplification. First, the unaided word discrimination score is obtained at 65 dB HL in soundfield and then again at the same level with the patient wearing the hearing instrument(s). In most cases, the patient’s word discrimination score should improve with amplification and the improvement exhibits to the patient that there is a benefit to the amplification. This gives the clinician a general idea that the patient is hearing speech at 65 dBHL and in quiet. Adults can often determine what is being said by making inferences from their language skills to assist them in deciphering the word being presented.
This is a good measure but does not ensure that the patient is hearing all frequencies needed to understand speech and a quiet booth is not the same as the typical listening environment. To address the issue of listening in quiet versus listening in noise, some clinicians will perform word discrimination while presenting background noise and using live speech to deliver the words. This gives the clinician an idea of how the patient will hear in a noisier environment.
It is important to know how the patient responds to speech and other sounds. It is also important to obtain feedback regarding if speech is audible and comfortable. These measures are somewhat subjective and, when used alone, do not give enough information to ensure that the hearing aid is properly fit for the patient. “Can you hear me now?” or “How does that sound?” are not the most reliable, state-of-the-art approaches for hearing aid fittings. When fitting a hearing instrument, the clinician should verify exactly how much dB SPL is being delivered to the ear for various frequencies and intensities. While the soundfield measures are useful in informing the clinician about how the patient is using their hearing, they should be cross checked with other objective verification methods such as Real Ear Measurements and Visible Speech Mapping.
Objective verification of the hearing instrument fitting has two stages, as reported by Brian Moore, PhD,5 at the University of Cambridge. “The first stage involves setting the parameters of the hearing aid using a ‘formula’ or computer-based procedure, usually using information from the audiogram, which may be combined with information on loudness discomfort levels. The second stage involves ‘fine tuning’ to suit the acoustic and auditory characteristics of individual ears and to suit individual needs and preferences.” It is important to verify the gain or output delivered because of the unique characteristics of the patient’s ear(s). What we think we are delivering and what is actually being delivered may not be the same.

|
| FIGURE 4. Real ear measurement using a formula-based approach is performed to verify that the hearing instrument is appropriately fit for the patient’s hearing loss. Shown is the AURICAL Plus, which offers a comprehensive, modular diagnostic and fitting system that includes audiometry, real ear measurements, and hearing instrument test box. |
Real Ear Measurements: A formula-based approach for fitting verification. Real Ear Measurements are performed to verify that the hearing instrument is appropriately fit for the patient’s hearing loss by measuring the sound pressure level (SPL) in the ear canal utilizing a probe microphone. There are at least four widely used measurements related to real-ear testing.
1. Real Ear Unaided Response (REUR) measures the natural resonance of the ear canal without a hearing instrument in the ear. The open ear naturally provides amplification of 17 dB on average between 2000-4000 Hz. When a hearing instrument is placed in the ear, this natural amplification is lost and therefore must be compensated for in the hearing instrument fitting. This measure is used to determine the Real Ear Insertion Gain (REIG).
2. Real Ear to Coupler Difference (RECD) measures the difference in the resonance of the patient’s ear in comparison to the resonance of a 2cc coupler. This is a very important measure because many fitting targets are based on the 2cc coupler and adjustments need to be made to compensate for peaks or troughs caused by the resonance of the patient’s own ear. Obviously, this is very important for infants and young children whose ear canal is considerably smaller than 2cc. It must also be mentioned that RECD is valuable for the adult population as well. Many adults have ear canals that vary from the average 2cc coupler.
3. Real Ear Aided Response (REAR) measures the sound pressure level in the ear when the hearing instrument is in the ear and turned on. REAR is an output measure and is currently becoming the most valued measurement. REAR is used to verify that the output of the hearing instrument will meet the three main goals in hearing instrument verification, or namely:
Soft speech (50-55 dB SPL) should be audible.
Conversational speech (65-70 dB SPL) should be comfortable.
Loud sounds (>90 dB SPL) should be tolerable.
4. Real Ear Insertion Gain (REIG) displays the amount of gain provided by the hearing aid minus the amount of gain lost by occluding the ear as determined by the REUR measure.
Traditional real-ear measurements use a prescriptive target to assist in the hearing aid fitting, such as NAL-NL1 or Desired Sensation Level (DSL). These targets utilize information documented in the commercial equipment, such as the audiogram, monaural or binaural fitting, age of the patient, UCLs, and RECD (measured or average), producing a fitting target for the frequencies related to the speech region. DSL is one of the only targets developed for infants and children. While measuring the patients RECD is the best approach, some patients will not cooperate, and DSL provides the clinician with age-related average RECD values.

|
| FIGURE 5. Visible speech mapping has become a valuable part of the modern test battery. Like REM, visible speech verifies if the hearing aid is appropriately fit for the patient’s individual hearing loss by measuring the SPL in the ear canal with a probe mic, but instead of the formula-based approach, it uses speech over the range of frequencies that constitute the speech banana. For example, AURICAL Visible Speech uses the binaural, wireless SpeechLink, and includes the Hearing Loss Simulator, Hearing Instrument Simulator, and Visible Speech Mapping. |
Real ear measurements often use frequency sweep, noise, or tone bursts as the stimuli for assessing if the hearing aid is appropriately fit. The problem with some of these stimuli types is that, with the new hearing instruments that feature noise suppression or feedback cancellation, the hearing instrument accepts the stimulus as being noise and then automatically reduces the gain. Then the clinician has to disable the noise suppression or feedback cancellation feature in order to utilize these stimuli. It is best if the features the patient is going to be using remain on during the verification process so that they are taken into account and evaluated during the fitting.
The other problem with these stimuli is the gain needed to amplify them may not be the gain needed to amplify speech. The optimal approach is to use a dynamic stimulus, like speech, to verify hearing instruments that utilizes dynamic features. Prescriptive fittings are a starting point to ensure that speech is audible, but they do not account for listening conditions.
Visible speech mapping: Using speech to fine tune the fitting. Visible Speech Mapping, like real ear measurements, is performed to verify if the hearing instrument is appropriately fit for the patient’s hearing loss by measuring the sound pressure level in the ear canal utilizing a probe microphone. The main differences are the stimulus is speech and there is not a prescriptive target, but rather a fitting range based on the speech banana. Speech is a dynamic signal and is preferred so that the dynamic features of the hearing aid can be left on during the verification process.
The Customized Speech Banana is based on the Articulation Index4 and is customized based on the patient’s audiogram. The speech banana is increased in intensity to make it audible and then compressed to fit into the patient’s dynamic range (between the patient’s thresholds and UCLs). An important benefit from the AURICAL Visible Speech, offered by GN Otometrics, is the ability to collect verification binaurally using the AURICAL SpeechLink because both probe microphones are live simultaneously.

|
| FIGURE 6. The “OnTop” mode in the AURICAL Plus and Visible Speech allows the clinician to modify the hearing instrument settings and immediately see the ramifications of changes. This feature makes verification of changes quick and easy and also assists in counseling the patient. |
The greatest benefits to combining Visible Speech Mapping into the verification process are that the hearing instrument fitting can be verified with all dynamic features turned on and with a speech signal which is realistic of what the patient will typically be listening to in their daily environment. The speech signal can be one that is provided in the software, live speech of the clinician or relative, or a music compact disk.
If the peaks of the speech signal cover without exceeding the customized speech banana, then the clinician has verified that speech is audible. The speech signal can be delivered at a soft level (50-55 dB) and at a moderate level (65-70 dB). The gain settings of the hearing instrument can easily be modified using “OnTop mode,” and the changes in audibility are instantly displayed in the Visible Speech Mapping software. The clinician can simultaneously program and hearing instrument and verify the patient’s audibility of the stimulus.
The Visible Speech Mapping software gives the patients visual and auditory feedback on their fitting, making them an active participant in the process. Counseling and having appropriate expectations are also important to having a satisfied patient who wears hearing instruments. As stated by Quilter6 in a past Hearing Review article, “the AURICAL Visible Speech is designed to enhance patient counseling by providing innovative features that make the fitting/ verification process more meaningful to the patient, it engages the patient as a partner in their rehabilitation, encourages ownership of the problem (as well as the solution), and involves family members in decision making.” If the degree of configuration of the hearing loss does not allow for full audibility of speech, this helps the patient understand what modifications in the fitting can be performed and the outcomes that will be provided.
Moore5 states that Visible Speech Mapping: “…allows markedly improved accuracy in the verification and fitting of hearing aids, it provides an immediate indication of the audibility of important, everyday signal such as speech, including the speech of relatives; it makes it possible to adjust the parameters of hearing aids to optimize the audibility of speech while avoiding loudness discomfort; it involves the client and their relatives in the fitting process, leading to greater understanding and satisfaction, and it is likely to reduce the number of post-fitting visits, saving time and money.”
There are three components of the hearing instrument fitting, with each component cross checking the other and verifying that the patient leaves the office with the best fit ensuring that the three goals are met:
1. Soft speech should be audible.
2. Conversational speech should be comfortable.
3. Loud sounds should be tolerable.
The best fit is possible by setting the hearing aid initially using a “formula,” fine tuning the fitting using a speech signal, and if possible, reconfirming audibility and patient satisfaction using soundfield testing.
References
- Jerger JF, Hayes D. The cross-check principle in pediatric audiometry. Arch Otolaryngol. 1976;102:614-620.
- Lindley G. Current hearing aid fitting protocols: Results from an online survey. Audiology Today. 2006:18(3):19-22.
- Mueller G. Fitting test protocols are “more honored in the breach than the observance.” Hear Jour. 2003:56(10):19-26.
- Mueller HG, Killion MC. An easy method for calculating the articulation index. Hear Jour. 1990:43(9):1-4.
- Moore BCJ. Speech mapping is a valuable tool for fitting and counseling patients. Hear Jour. 2006:59(8):26-30.
- Quilter M. Taking the guesswork out of hearing instrument fittings. The Hearing Review. 2006;13(6):56-60.