Every dispensing professional has noticed that some patients are extremely talkative while others need to be encouraged to relate anything about their hearing loss. Likewise, one patient might like a particular hearing aid, while another with an identical audiologic history/audiogram might not. Why? Could it be a difference in personalities? This article looks at personality profiling of clients (and the professional) as a means of better understanding patients and adjusting counseling/fitting approaches appropriately.
Today’s hearing instrument fittings are conducted with attention to every small detail, such as venting, dampening, compression ratios, output, insertion gain, and many other specifics with great benefit to the hearing impaired. Despite the greater capabilities afforded by digital instruments and other technological breakthroughs, there are still many patients who have difficulty utilizing amplification for reasons that appear to be related to their personal characteristics and tendencies, and/or even conflicts with the dispensing professional who is trying mightily to assist them along the path to better hearing.
Until recently, audiology literature lacked discussion of one’s personality in the diagnosis and treatment of hearing impairment.1-3 In the everyday clinic, these personal differences can be easily observed as some patients are flexible, others are rigid; some are highly logical, others are governed by feelings or intuition. These differences are not inconsequential; they can make a great difference in a fitting’s success or failure.
Personality differences have even been suggested by researchers as a likely cause of the high variability seen in the standardized measures of success, such as rehabilitative questionnaires and outcomes measures.4,5 Since it is obvious that patients react differently to their hearing loss, the responsible clinician needs to prepare for these differences and adjust his/her hearing aid fitting technique according to the specific personal differences. Although Thomas6 and Meadow-Orlans7 have indicated that the basic structure of personality is not affected by hearing loss, personality has been virtually ignored in the discussion of rehabilitative intervention.
Lately, theoretical information and specific personality testing techniques that could be utilized in hearing aid fitting have been suggested by a number of authors.1-3,9-12 While there are other personal style assessments, such as the DISC,9 being studied for possible use with the hearing impaired, the Myers Briggs Type Indicator (MBTI)11 and/or the Keirsey Temperament Sorter (KTS)12 have been studied intensively and can be easily accessed online at www.MBTI.com or at www.Keirsey.com. (Author’s Note: The www.Keirsey.com site describes assessment tests in detail and even offers clinicians and/or their patients the opportunity to take the MBTI/KTS assessment and have it scored at no charge. A more detailed discussion of these measures, as well as many of the concepts in this article, can be found in the Traynor & Holmes3 monograph in Trends in Amplification.)
Informal Assessment of Personality
Formalized assessment is, of course, the optimal situation, but computers and Internet connections are not always available and the typical clinic schedules often do not allow the luxury of taking the time for manual administration of full personality assessments, their scoring, and evaluation. Even if we are not exactly perfect in our informal assessment of personality, it is still better than treating every patient with mere adjustments according to their hearing impairment. While experienced clinicians often intuititively modify and adjust their techniques according to their experience with different personalities, many clinicians sometimes do not have the experience or personal skills from which to draw appropriate conclusions without some assessment of personal style.
An informal method of assessment can be conducted by using small-talk dialog during the case history and/or discussion of specific situations during a follow-up visit. During these sessions, the attentive dispensing professional often can get a rough estimate of the patient’s MBTI/KTS personality. By combining the clinical perception of the patient with observations and information from significant others, informal personality type judgments are often quite accurate.13,14
When attempting to observe these traits, Extraversion and Introversion are, of course, the easiest to identify as these characteristics offer the most natural cues to the observer. While there are not many natural behavioral cues identifying if patients make their decisions by logic or compassion (Thinking or Feeling), the most difficult observation remains if the patient analyzes detail or skips the specifics to analyze problems (Sensing or Intuition).15
Extraverted or Introverted?
As Jung10 discovered in the early development of personality theory, informal assessment of an extravert from an introvert is probably the easiest trait to identify. Clinicians need to ask focused questions to obtain information that can be helpful in their treatment, both initially and during their fitting.2 Studies15,16 suggest the following as a list of basic differences between Extraverts and Introverts that can be observed during clinic:
- • Extraverted (E) patients may…
- 1. Have an expressive face, voice and/or gestures;
- 2. Demonstrate a high level of enthusiasm and appreciates an energetic clinician with optimism;
- 3. Speak in a loud voice;
- 4. Be talkative and appreciate a more talkative clinician.
- • Introverted (I) patients may…
- 1. Express insecurity or sensitivity and is comfortable with silence;
- 2. Demonstrate an awkward interpersonal style;
- 3. Behave in a fearful or timid manner;
- 4. Be reserved or unexpressive, and be less comfortable with action;
- 5. Keep their partner at a distance;
- 6. Show a general lack of interest in clinical interaction.
Sensing or Intuition?
The most difficult personal style component to informally assess is if the patient uses Sensing (S) or Intuition (N) strategies to gather information.15,16 Generally, Sensing patients tend to look for specifics and examine all the components of issues, focusing more on the process than the overall outcome, while their Intuitive counterparts gather information randomly then seek its meaning. Clinically, patients may present the following clues to disclose their preference for either Sensing or Intuition.14,17-20
- • Sensor patients may…
- 1. Gesture very little;
- 2. Keep his/her hands in pockets or behind their backs;
- 3. Tend to read more realistic books and remember specific plots and details of the story;
- 4. Relate stories, case histories, and experiences with hearing aids in great detail;
- 5. Appreciate a step-by-step, concrete and detailed approach to situation;
- 6. Be uncomfortable with novel and imaginative approaches.
- • Intuitor patients may…
- 1. Tend to look toward the possibilities of “what might be”;
- 2. Overemphasize the benefits;
- 3. Jump from topic to topic;
- 4. See unrealistic possibilities with amplification and/or audiologic treatment;
- 5. Often overlook facts and be unrealistic about their hearing loss, the technological capabilities of their hearing aid, etc;
- 6. Appreciate novel or imaginative approaches to treatment.
Thinkers or Feelers?
The identification of Thinkers (T) from Feelers (F) is often not overtly observable, but does not take as much experience and skill as looking for other traits. When looking for cues to the Thinking/Feeling continuum, there are some specifics that clinicians should easily observe14,17-20:
- • Thinker patients may…
- 1. Act or appear to be “irritable”;
- 2. Express skepticism or cynicism and avoid emotions—especially in the early sessions;
- 3. Draw diagrams with their hands and innumerate points using their fingers;
- 4. Need the rationale and logic behind the treatment approach and/or hearing aid selection;
- 5. Talk at their partner.
- • Feeler patients may…
- 1. Probably behave in a cheerful manner;
- 2. Laugh frequently;
- 3. Gesture with open hands in flowing movements;
- 4. Want to be an easy, good case that is remembered and appreciated.
Judging or Perceiving?
As with the observation of Extroversion/Introversion, the Judging (J)/Perceiving (P) continuum is also fairly easy to identify. Some helpful clues to Judging/Perceiving patients are14,17-20:
- • Judger patients may…
- 1. Fear losing control;
- 2. Want to have options in difficult situations;
- 3. Find change stressful;
- 4. Work hard on projects and tolerate discomfort;
- 5. Need an organized, structured, step by step approach.
- • Perceiver patients may…
- 1. Be very likely to avoid decision-making;
- 2. Like to have lots of options and they do not like organized group programs;
- 3. Like to have lots of flexibility in the rehabilitative program;
- 4. Not be tolerant of discomfort;
- 5. Be great time-wasters.
Clinical Implications
Although the MBTI presents a lot of detail in the analysis of personality, it offers too many categories to be clinically useful. No matter the method of assessment, patients seem to fall into four general categories,8,9 offering audiologists the opportunity to design four different treatment techniques for the major personality differences observed.
The Keirsey Temperament Sorter (KTS) offers a method for reducing the MBTI assessment into a clinically useful tool. Theoretically, Kiersian theory suggests that the MBTI’s Thinking (T)/Feeling (F) continuum has the most effect on those individuals that are the non-detail oriented Intuitors (N), while the detail-oriented Sensors (S) are most affected by the Judging (J)/Perceiving (P) continuum.12 Thus, the KTS facilitates the digestion of personal style into four Kiersian groups (Table 1) of Sensing-Judging (SJ), Sensing-Perceiving (SP), Intuitive-Feeling (NF), and Intuitive-Thinking (NT).
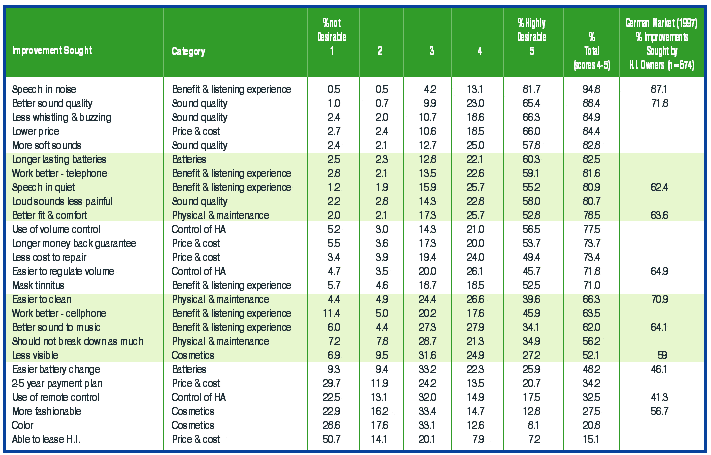
Table 1. The four primary Kiersian Temperaments and MBTI Types.2
Although there needs to be much research into specific treatment and/or hearing aid fitting protocols for these four different personal styles, the following represents initial considerations for the four different personal style presentations.
Tendencies of Sensing-Judging (SJ) Clients: The SJ temperament consists of the MBTI types ESTJ, ISTJ, ESFJ and ISFJ. Estimates for the incidence of this personality type in the adult hearing-impaired population range from 63% in private practice clinics to 86% in public/VA hospitals.3
The following are issues to consider when working with SJ patients.
- Intense need for the clinician to maintain control of situation;
- Usually very cooperative, active participant in A/R process;
- Values and appreciates authority, but has high expectations;
- If adjustment is slow, can get very bored with the process;
- Easily follows detailed instructions and will organize priorities;
- Take responsibility for their own rehabilitative program;
- Prefer a detailed, practical, step-by-step approach (ie, “nitpicker”);
- Prefer specific objectives, but over analyze minor details;
- Need to be on time for appointments; fear of losing control.
Tendencies of Sensing-Perceiving (SP) Clients: SP personalities make up about 15% of our patient population and, as a group, generally are very tolerant of their own difficulties and shortcomings. This tolerance of imperfection makes accuracy (ie, in the hearing aid fitting) not of particular importance to the person with an SP personality. SPs are comprised of the ESTP, ISTP, ESFP, and ISFP MBTI types, and clinicians should consider the following points when working with patients that are SP personalities16,17:
- They want short explanations, and have a “please fix me” attitude;
- No time for the hearing impairment;
- Just jumps into the process and may not follow your directions;
- If it appears to be not successful, these patients will give up;
- No time concept, distractible, avoid discomfort and decisions;
- Easily follow detailed instructions and will organize priorities;
- Constant drive to fix their “broken” hearing;
- Must consider the program a valuable use of time;
- May not read any of the materials unless absolutely necessary;
- Prefer a detailed, practical, step-by-step approach (ie, “nitpicker”);
- Intense need for the “spotlight,” communication is essential;
- Very prone to denial of the severity/impact of the hearing loss;
- No real long-term satisfaction, more likely to say “this never worked”;
- A/R program (fittings) must be immediately relevant;
- Pragmatic, concrete program—not interested in theory;
- Do not prepare, and prefer to just see what happens.
Tendencies of Intuitive-Feeling (NF) Clients: NFs are the abstract cooperators of the world. Also making up about 15% of our clinical population, NFs have difficulty staying on task and usually have several projects going at the same time. These individuals are often very diplomatic in their interactions and have an intense need for harmony in their world. Keirsey12 characterizes the signature of the NF as a person harboring a theoretically impossible need to keep everyone happy. Specifically, the NF consists of the ENFJ, INFJ, ENFP, and INFP MBTI types and, clinically, audiologists should consider the following when working with the NF patient.3,18
- Respond best to positive reinforcement;
- Intense need for communication with others;
- Set clear goals and expectations, do not oversell benefits;
- Feeling of obligation to others to do well in the A/R process;
- Are doing this for someone else, but want to be “good clients”;
- When unsuccessful, patients can become rigid and demanding;
- They will not give much positive feedback;
- Talk is cheap, just give them results;
- Usually very cooperative in A/R process and work very hard;
- Often have well-developed coping behaviors;
- Worry that they could have done a better job. Prone to self criticism;
- Never quite satisfied, always want a bit more;
- If unsuccessful, it will be their fault.
Tendencies of Intuitive-Thinking (NT) Clients: Clinicians should be grateful that NTs make up only about 4-5% of the general clinical population as they are the proverbial “engineer type.” The NTs have very high standards and are unimpressed with authority, preferring complexity, strategic thinking, and they want to be considered both logical and ingenious. NT’s consist of the ENTJ, INTJ, ENTP, AND INTP MBTI types.16,17 The following are clinical considerations when working with an NT patient.3,16
- Likes detailed explanations, not impressed with credentials;
- Over analyzes everything, but once convinced works very hard;
- Can present as aloof, intimidating, argumentative, and arrogant;
- Often impatient with the A/R (fitting) process;
- Sometimes complains about very small problems;
- Does not respect authority and pursues self improvement;
- When unsuccessful, may change program on their own;
- Most particular and independent of all types;
- Constantly thinking of how they can improve the procedure and your A/R program;
- Skeptical and often require lots of references and rationale for a fitting or A/R program;
- Tend to over-analyze the problem and try to fix it themselves.
The Clinician’s Personal Style: Tendencies and Implications
Hearing care professionals should also be aware that they have their own personal style which may reflect how they perceive and conduct the fitting process. Personal style interaction may explain why certain patients do better with some clinicians than with others or why some clinicians become frustrated with certain types of patients.
Recently, studies have been conducted to obtain information as to the personal styles of audiologists to better understand their interactions with patients. One study3 is that of 94 audiologists attending the 2000 Academy of Dispensing Audiologists (ADA) Convention in San Diego. In this study, each subject was screened to ensure that they were involved in diagnostic and rehabilitative treatment each day. Subsequently they were administered the MBTI/KTS which was scored via an Internet connection. Sensing-Judging (SJ) personalities made up 56% of the audiologists participating in the study, 16% were Sensing-Perceiving (SP), 21% presented Intuitive-Feeling (NF) styles, and 7% were Intuitive-Thinking (NT)3,7 (Figure 1a).
|
||
| Figure 1a-B. Personal styles of audiologists as reported by Traynor & Holmes3 (top, 1a) and Carmen20 (bottom, 1b). |
Carmen21 has also reported the personal style of audiologists from his study conducted by Audiology Online utilizing the MBTI/KTS assessment. The research finds a substantially different stratification of personal style among audiologists than that of the San Diego study. However, he suggests that it is possible the respondents were a special group of people (ie, a certain personality type that may have been more prone to respond over the Internet because of its easy access, privacy, less-threatening approach, etc). Carmen’s data on 217 subjects indicated that Sensing-Judging (SJ) audiologists were 38.7% of the group, while Sensing-Perceiving (SP) were 2.8%; 35.5% were Intuitive-Feeling (NF) and 23% demonstrated Intuitive-Thinking (NT) (Figure 1b). Although the number of NTs in this study was 4 times the national average, he indicates it is quite possible that a high number of audiologists online are NTs, and those online tend not be SPs—thus skewing the survey toward those that are computer-minded clinicians.
Obviously, there are some differences in the data regarding the prevalence of the various MBTI/KTS personalities among audiologists. It is, however, reasonable to assume that such variability exists and can cause some confusion in the fitting and/or treatment program. Thus, based upon the personal style literature and clinical experience, the following are some procedural recommendations for personal style variations among clinicians:
- Considerations for SJ Clinicians
- 1. Do not expect every patient to be on time.
- 2. All patients do not want an organized step-by-step program.
- 3. Do not be practical for everyone, especially the NT Patients.
- 4. Do not focus on the procedure, especially for SPs and NFs.
- 5. Do give clear objectives and prepare for situations.
- 6. Have options when one treatment program (or hearing aid) does not work.
- Considerations for SP Clinicians
- 1. Do put up with long procedures when they are necessary.
- 2. Try to focus more on the overall outcome rather than the process.
- 3. Accuracy of a particular adjustment or procedure may be more accurate than you think.
- 4. Be tolerating of patient difficulties.
- Considerations for NF Clinicians
- 1. Be aware that you will never make all of your patients happy.
- 2. Good clinicians need to disagree with their patients sometimes.
- 3. Focus and concentrate on boring rehabilitative treatment tasks.
- 4. Do not expect everyone to care as much as you do.
- Considerations for NT Clinicians
- 1. Perfection is not always necessary.
- 2. Most patients need to have things simplified.
- 3. Most patients do not require long presentations including the background for each procedure.
Summary
This discussion presents methods of informal assessment to arrive at some components of patient personal style for use in hearing aid fitting sessions. It further suggests some considerations when conducting sessions for patients and clinicians of particular personal styles. It is hoped that the strategies presented here can be modified by hearing care professionals into specific treatment methods for patients of different personalities.

|
Correspondence can be addressed to HR or Robert M. Traynor, EdD, Audiology Asociates of Greeley, Inc, 2528 16th Street #100, Greeley, CO 80634; email: [email protected].
References
1. Traynor RM, Buckles KM. Personality typing: Audiology’s new crystal ball. In: Kochkin S, Strom KE, eds. High Performance Hearing Solutions, Vol 1. Hearing Review. 1997; 4(1)[Suppl]:28-31.
2. Traynor RM. Relating to Patients. In: Sweetow RW, ed. Counseling for Hearing Aid Fitting. San Diego: Singular Publications;1999.
3. Traynor R, Holmes A. Personal style and hearing aid fitting, Trends in Amplif. 2002;6(1):1-31.
4. Humes, L, Dimensions in hearing aid outcome. J Am Acad Audiol. 1999;10:26-39.
5. Cox R, Alexander GC, Gray G. Personality and the subjective assessment of hearing aids. J Am Acad Audiol. 1999;10(1):1-13.
6. Thomas AJ. Acquired Hearing Loss: Psychological and Psychosocial Implications. London: Academic Press;1984.
7. Meadow-Orlans KP. Social Psychological effects of hearing loss in adulthood: A literature review. In: H. Orlans, ed. Adjustment to Adult Hearing Loss. San Diego: College-Hill Press;1985.
8. McCarthy P, Traynor R, Huart S, Holmes A. Personality Influences on attitudes and expectations in hearing aid fittings. Paper presented at: American Academy of Audiology annual convention, San Antonio, Texas, April 2003.
9. Huart S, Weber J, Cheverette M. The use of the DISC to determine return rates of hearing aids. Paper presented at: American Academy of Audiology annual convention, Philadelphia, PA, April 2002.
10. Jung CG. Psychological types. Princeton, NJ: Princeton University Press Inc, 1920.
11. Briggs KC, Myers IB. Myers-Briggs Type Indicator. Palo Alto, CA: Consulting Psychologists Press, 1943, 1976.
12. Kiersey D, Bates M. Please Understand Me. Delmar, Calif;1984.
13. Kendrick D, Funder DC. Profiting from controversy: Lessons from the person-situation debate. Am Psychol. 1988;43 (1):23-34.
14. Funder DC, Sneed CD. Behavioral manifestations of personality: An ecological approach to judgmental accuracy. J Pers Social Psych. 1993;64:479-490.
15. Thorne A. The press of personality: a study of conversations between introverts and extraverts. J Pers Social Psych. 1987; 53: 718-726.
16. Kroeger O, Thuesen JM, Type Talk. New York: Dell Publishing;1988.
17. Bayne R. The Myers-Briggs Type Indicator: A Critical Review and Practical Guide. New York: Chapman and Hall;1995.
18. Myers IB, McCaulley M. Manual: A Guide to the Development and use of the Myers-Briggs Type Indicator. Palo Alto, Calif: Consulting Psychologists Press; 1985.
19. McCaulley M. Asking the right questions. Bull Psych Type. 1992; [Monogr] 15(2):1,5-6.
20. Scanlon S. Gestures. Type Reporter. 1988; 3(8):1-4.
21. Carmen R. Personality types as measured by the Myers-Briggs Type Indicator. Audiol Today. 2003;15(4).14-18.