A patient-driven/adjusted, interactive fitting method for binaurally balanced intensity information
A computer-based, patient-driven, interactive fitting method is described that uses patient-adjusted, binaurally balanced intensity information. The goal is to 1) increase the accuracy and benefit of multi-channel hearing aid fittings; 2) reduce the time of involvement of professionals whose expertise can be focused in more meaningful areas; and 3) reduce reliance on iterative processes that require extraneous equipment, time, and expense. Fittings with the new method were accomplished with an off-the-shelf multi-channel hearing aid and compared to conventional fittings previously completed on a variety of hearing aids. Objective tests of speech audibility show improved performance using the new fitting method, as do subjective reports of aided benefit.
The role of binaural hearing in sound localization has been known for centuries.1 Binaural localization phenomena are the bases for the “cocktail party effect,” release from masking,2 binaural squelch,3 and other advantageous listening strategies. The advantages of binaural hearing among hearing-impaired individuals are more fully realized if hearing aid fittings minimize distortions in binaural timing and intensity information across the frequency spectrum.
Hearing and Fitting Variables
Accurate delivery of amplified sound minimizes disturbances to binaural information. Reducing variation is the key to accuracy. Much variation occurs in the fitting of hearing aids—from audiograms to patient responses to the amplified sound and corresponding adjustments in response to the question, “How does that sound?”
Guidelines have been developed to mitigate variation in the assessment of audiometric thresholds.4 These guidelines assume an audiometer that is capable of tolerances no worse than ±3% of target frequency and ±3 to 5 dB of target intensity.5 These tolerances are greater than the test-retest variation in thresholds exhibited among patients and greater still than the capabilities of current instrumentation.6 Yet, despite these wide tolerances, there is additional variation among clinicians in the measurement of audiometric thresholds.7,8
Prescriptive fitting algorithms also introduce variation. They differ philosophically as to how much gain to prescribe. Then, once a prescriptive algorithm is chosen, it is possible that the fitting system will not deliver the prescribed gain accurately.9 Additionally, the specifications for hearing aid performance10 allow wider tolerances than the range necessary for accurate fittings. For these reasons, post-fitting verification via real-ear measurements has become the standard for best practice in an effort to reduce variation from all of these sources.11 However, even when the prescription is accurately delivered, the patient’s preferred use-gain may end up being different from their prescription,12 which may be why Kochkin’s research13 suggests that subjective validation may carry more weight than verification.
Kochkin et al11 have summarized clinicians’ reasons for their reluctance to adopt verification and validation procedures in their practices. Whether these reasons are real or perceived, we acknowledge that objections nevertheless exist. They are an impediment to the adoption of accepted best practices by many hearing health providers. At risk is what Kochkin et al have termed “quality control at the point of dispensing.”11
Quality Control and Dispensing
The essence of quality control theory is to reduce variability, thereby increasing accuracy. Modern quality control techniques aim to reduce variability by controlling the processes that produce an end product. This is accomplished through measurement of process parameters rather than measurement of attributes of the end product. Quality is achieved when several milestones are reached. These include:
- The process runs unfettered and intervention to “correct” the process is minimized;
- Variation due to “assignable causes” (ie, process errors) is eliminated;
- Remaining variation in key metrics is random and maintained within rigorous control limits (ie, variation is small); and
- Measurement of attributes of the finished product no longer contributes to improvements in quality.
These same quality philosophies can be applied to activities other than bricks-and-mortar manufacturing, including the fitting of hearing aids. In the case of fitting hearing aids, there is variation among patients over which the clinician has no control. However, a process that can accommodate this type of variation achieves quality by removing (or accounting for) the influence of the variation. In the case of the interactive fitting process described herein, direct patient input is in response to a stimulus controlled by the process. Individual patient variation is accounted for because it is, in effect, measured and “neutralized” by the patient.
Measurement of a product’s attributes as a means to ensure quality—whether calipers on a manufactured widget or sound pressure in a real ear canal—requires additional physical, intellectual, and human resources. Additional procedures also increase patient “chair time,” which is cumulative over several visits. The length of an initial patient visit may be in line with the clinic’s productivity plan, but this may not deliver a fulfilling experience for the patient. The patient may require several subsequent visits in order to experience a modicum of satisfaction, whereas the most satisfied patients achieve satisfaction with fewer visits.11,13
A Fitting System Designed For Real-World Dispensing
Because there is so much resistance to adding equipment, iterative steps, professional resources, and other expense in the name of best practices—even in the face of compelling reasons to do so—we looked at a fitting process designed to reduce variability and deliver a hearing aid fitting that provides exceptional benefit, and does not, in most cases, require additional verification, validation, and adjustment.
The fitting system and method under investigation, called Personal Sound Perception™, was developed by Pixation Corporation and is currently used with hearing aids that are similarly branded. However, the system could be adapted for use with any programmable, multi-channel, wide-dynamic range compression (WDRC) hearing aid. Inherent to the success of the process is its interactive patient interface, which includes a method for binaurally balancing hearing aid gain. The instrumentation is PC-based and performs the functions of an ANSI/ASA S3.6 Type 5 audiometer5 integrated with the hearing aid fitting algorithm. The patient can be prepped and the process attended by nonprofessional technical personnel, freeing professional staff for more cost-appropriate activities.
This first of several planned studies was undertaken to evaluate initial design goals as outlined in this article’s abstract. The intent was to ascertain the basic benefit intrinsic to the overall fitting process by comparing fittings completed with the new process to conventional hearing aid fittings on two performance metrics: 1) word recognition in quiet, and 2) subjective ratings of benefit.
Methods
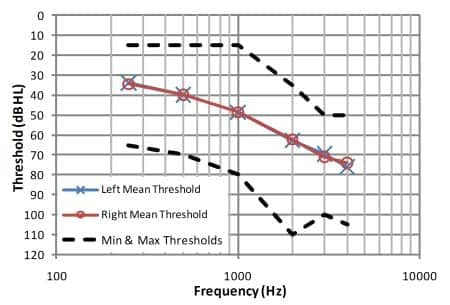
Figure 1. Minimum, maximum, and mean right and left audiometric thresholds
(N = 11).
Research design. A two-way analysis of variance (ANOVA) with repeated measures design was used to compare word recognition scores (WRSs) as the dependent variable, obtained on the same subjects under three aided conditions at five speech levels. The WRSs were collected using phonemically scored monosyllabic words. Five speech levels were used in order to generate performance-intensity (P-I) function curves for each aided condition. Post hoc analyses were conducted to parse out statistically significant findings.
Subjects. A power analysis of the intended research design was accomplished a priori using PiFace Java script software for power analysis.14 The power analysis yielded a minimum sample size of 10 subjects for P > .994 at a significance level of .05. The 10 initial subjects consisted of 8 males and 2 females. An additional female subject was included in order to offset the gender imbalance somewhat. The final subject pool had a mean age of 74 years, ranging from 56 to 90 years. All of the subjects were enrolled in the study under informed consent.
The 11 subjects were current hearing aid wearers and had been wearing hearing aids binaurally for at least 6 months prior to the current study. All subjects had bilateral, generally symmetrical, sensorineural hearing loss of mild-to-severe degree below 1 kHz, and moderate-to-profound degree above 1 kHz. Mean right and left thresholds (with minimum and maximum thresholds) for the 11 subjects are shown in Figure 1.
Materials. The subjects were each fit binaurally with new receiver-in-the-canal (RIC) devices or conventional behind-the-ear (BTE) devices, depending on the severity of the hearing loss. All of the new hearing aids were constructed with omnidirectional microphones. The signal processing technology within the hearing aids (ON Semiconductor® Ezario™ 5900 with IntriCon Ethos™ firmware) was identical for both the RIC and BTE devices. The only difference between the RIC and BTE devices was compensation for earmold plumbing, where appropriate.
Target speech for WRSs consisted of recorded lists of monosyllabic words scored phonemically and presented in a soundfield from audio compact disc (CD).15 The soundfield was constructed within a single-walled test room with target speech originating from a JBL Control-1 loudspeaker mounted on a stand located at 0º azimuth and 1 meter distant from the center of the listening position.
Procedures. The fittings of the new hearing aids were completed using a procedure wherein sensitivity thresholds were obtained using a descending amplitude-modulated tone presented from a computer via calibrated headphones. These thresholds were used to determine a starting point for obtaining binaural balance data at comfortable and loud levels.
While the method for obtaining the subjects’ behavioral binaural balance response is unique, the classical Method of Adjustment may serve as a point of orientation (see Gelfand,16 Chapter 7, for review). The subject is asked to adjust an unmarked, non-detented control until the stimulus, also presented under headphones, is determined to be the same level in both ears or fused as a single image in the center of the head. The metric is the virtual angle, representing the level difference between the two ears.
This process is replicated at octave frequencies below 1 kHz and at half-octave frequencies above 1 kHz (the virtual starting angle of the stimulus is randomized), for both comfortable and loud levels, and the measurements at each test frequency are averaged as long as the difference between the two measurements is within a predetermined range. Measurements outside this range are repeated until the replication falls within the acceptable range. Measurements at a specific frequency and intensity are aborted if the subject cannot replicate the measurement within several attempts. The entire fitting process takes approximately 20 minutes.
At the initial clinical visit, each subject received a comprehensive audiological evaluation and WRSs in quiet were obtained in the soundfield, unaided (No HAs condition), at 40, 50, 60, 70, and 80 dBHL, in order to construct a performance-intensity (P-I) function curve. If the subject was in possession of their own previously fit hearing aids at the time of the initial visit, WRSs were obtained in this aided condition as well (Previous HAs condition). WRSs were obtained on the new hearing aids (New HAs condition) at 7 to 10 days post-fitting on average.
Subjects were seated facing the loudspeaker and asked to repeat the words heard. They were also instructed to guess at words or repeat any speech sounds heard when only partially audible since phonemic scoring was used. Phonemic scoring of monosyllables is an established means of generating comprehensive word recognition data with fewer test items, in less time, and with greater sensitivity than whole word scoring.17,18 The word lists used were developed by Olsen et al18 and are included among the test items on the CD.15
P-I function curves were analyzed as the dependent variable because they provide performance data over a range of hearing losses and intensities that are unavailable with a single score,19 and may be more predictive of differences in performance among different types of amplification.20 Lists and conditions were randomized using a hyper Latin-square to establish administration order for speech levels, word lists, and aided conditions.
Subjective ratings of benefit were collected using the Abbreviated Profile of Hearing Aid Benefit (APHAB).21 An APHAB form was either mailed to the subjects along with a self-addressed, postage prepaid return envelope, or completed by the subject in the clinic 10 days to 2 weeks post-fitting with the New HAs. Administration and scoring followed the recommended procedure.22 As the sample size for this study is not sufficient to determine significance using statistical methods or APHAB difference scores,23 APHAB data are interpreted in terms of normative data for wearers of WDRC hearing aids.24
A note on the hearing aids in this study. All of the subjects in this study are patients of the second author, a medical physician. New HAs evaluated in this study were purchased by the patients in the normal course of their care under the physician. These patients were given no additional incentive (financial or otherwise) to purchase the hearing aids or participate in this study, so there is no bias in this regard.
The second author performed all of the New HA fittings using the new fitting system and method. These fittings were not optimized or adjusted using any secondary objective verification process (eg, real ear measurements). Prior fittings of the patients’ own hearing aids were performed by various hearing care providers in the community. The first author is an independent consultant contracted to perform conventional audiometry, collect the objective and subjective data reported herein, and perform the data analyses. The first author did not participate in the fitting or sale of any hearing aids evaluated in this study, and holds no financial interest in the physician’s practice or in Pixation Corporation. The second author has no direct financial interest in Pixation Corporation, but is related to the president of Pixation Corporation, hence the necessity of contracting an independent third party to design and conduct this experiment.
As a physician, the second author fits hearing aids as permitted under the laws of the State of Utah. This point is made to highlight the fact that a trained person without professional credentials specific to audiology or hearing aid dispensing can perform the tasks necessary to achieve beneficial hearing aid fittings using the process described in this paper.
Results
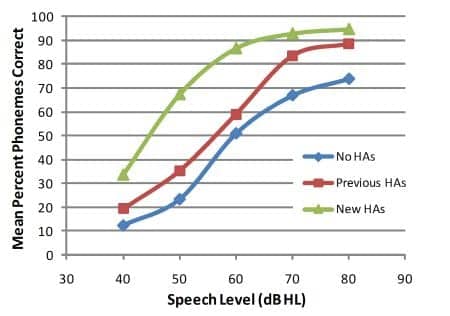
Figure 2. P-I function curves for hearing-impaired listeners (N = 11). Curves are given for three Aided Conditions (No HAs, Previous HAs, and New HAs).
Objective measures. P-I function curves of the experimental data are displayed in Figure 2. Improved audibility is indicated by several hallmarks of a P-I function curve:
- Higher percent-correct scores at a given speech level (ie, achieving 50% correct at a lower speech level);
- Functions with steeper slopes; and
- No evidence of “rollover” at higher speech levels (rollover may be an indication of distortion when testing with amplification).
A two-way ANOVA on the P-I function data yielded two significant main effects and a significant interaction. The factor Speech Level is significant (F[4, 164] = 79.31, P < .001), simply because increasing the presentation level is expected to produce higher WRSs. Aided Condition was also a significant factor (F(2, 164) = 26.73, P < .001).
Figure 2 shows all Aided Conditions to be different from each other. A Tukey-Kramer post hoc comparison of Aided Condition reveals that Previous HAs is significantly better than No HAs, and New HAs is significantly better than both Previous HAs and No HAs. The interaction between Speech Level and Aided Condition was significant, F(8, 164) = 2.63, P < .014, because amounts of separation among the three P-I function curves vary as a function of speech level. In other words, the Previous HAs curve is closer to No HAs except at the highest speech levels, where it is closer to the New HAs curve.
Subjective measures. Eight of the 11 subjects returned completed APHAB profiles (Figure 3). When viewing Figure 3, keep in mind that lower is better, suggesting that fewer problems are being reported. Also note that the first three subscales are pertinent to listening performance, whereas the Aversiveness subscale reports on problems with sound annoyance.
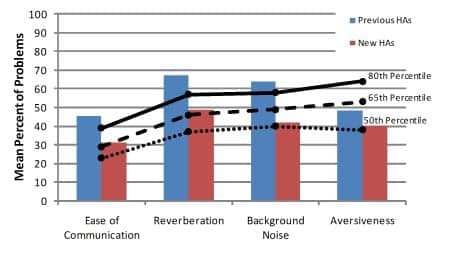
Figure 3. Mean percent of problems reported on the APHAB for both conventionally fit Previous HAs and New HAs fit with the interactive fitting method (N = 8), compared to the 50th (dotted line), 65th (dashed line), and 80th (solid line) percentile norms of wearers of WDRC hearing aids.
The APHAB scores for Previous HAs and New HAs are compared with the normative data for wearers of well-fit WDRC hearing aids reported by Johnson et al,24 as well as to each other. The lines in Figure 3 represent the 50th (dotted), 65th (dashed), and 80th (solid) percentiles for the WDRC norms. Figure 3 implies that the subjects in the present study, while wearing their own, previously fit hearing aids, reported more listening problems on the first three subscales than 80% of the individuals comprising the normative data. Conversely, while wearing the new hearing aids fit with the new fitting process, these same subjects reported fewer problems, on par with about 65% of their peers on the Ease of Communication and Reverberation subscales, and 50% of their peers on the Background Noise subscale.
Data from the Aversiveness subscale suggest that the subjects in this study found that sound amplified by New HAs was less bothersome than sound amplified by Previous HAs. Aversiveness problems with New HAs were reported at about the same rate as that experienced by 50% of WDRC wearers.
Conclusions
This study reports on a new fitting process that relies on patient interaction in a unique binaural balancing paradigm to arrive at prescriptive fitting parameters for multi-channel WDRC hearing aids. The design intents are to increase the accuracy, and therefore the benefit, of multi-channel hearing aid fittings while reducing the temporal and fiscal costs associated with the oversight of credentialed professionals, additional and iterative processes, extraneous equipment, and additional patient visits. The results of the present study show that the Personal Sound Perception method meets these design goals. The objective and subjective outcome measures presented herein demonstrate that the hearing aid fittings completed with the new process are capable of providing greater benefit than conventional hearing aid fitting methods.
By relying on a process-control model of quality assurance, wherein process variation is small and relatively insensitive to external influences, this fitting system may be able to deliver improved performance without the constant need for additional verification and validation steps. The number of additional patient visits may also likely be reduced. The average number of visits to complete the Personal Sound Perception fittings among the subjects participating in the present study is on par with the 2.41 visits reported by Kochkin13 for the most satisfied hearing aid wearers.
Although the Personal Sound Perception system meets the requirements for an ANSI/ASA S3.6 Type 5 audiometer,5 the thresholds obtained by the system are air-conduction only. The measured thresholds are used exclusively in the prescriptive algorithm for fitting hearing aids. Conventional audiometry is still necessary for diagnostic work-ups and comprehensive baseline data. Audiometric thresholds generated by conventional audiometry are not accurate enough to be used in the Personal Sound Perception prescriptive algorithm. The 5-dB step size for conventional audiometric thresholds yields a test-retest reliability of ±5 dB. Test-retest reliability of the thresholds obtained by the Personal Sound Perception system appears to be smaller than ±1.5 dB averaged across test frequencies in preliminary evaluations. Data are currently being collected in order to assess this fully in a future publication.
In this initial report on a new fitting system and method, we have discussed objective functional test results using a basic metric of the audibility of speech obtained at various intensities in quiet and compared them to similar results obtained on hearing aids fit using conventional methods.
An expanded report on results from extensions of this study is planned for future publication. Future performance measures will include tests of speech in noise and the influence of digital noise reduction and directional microphones on the binaural balancing process using signal processing algorithms and firmware currently under development by Pixation Corporation. Experimental populations will include individuals new to hearing aid use and those with asymmetrical hearing losses.
Correspondence can be addressed to HR or Dean G. Anderson, MD, at .
REFERENCES
- Libby ER. In search of the two-eared man. In: Libby ER, ed. Binaural Hearing and Amplification: Volume 1. Binaural Hearing Contents. Chicago: Zenetron Inc; 1980:1-36. Reprinted from Etymotic research library, Vol 1 [CD-ROM]. DE Rose, ed. Elk Grove Village, Ill: Etymotic Research; 1998.
- Licklider J. The influence of interaural phase relations upon the masking of speech by white noise. J Acoust Soc Am. 1948;20:150-159.
- Koenig W. Subjective effects of binaural hearing. J Acoust Soc Am. 1950;22:61-62.
- American Speech-Language-Hearing Association. Guidelines for manual pure-tone threshold audiometry. ASHA. 1978;20:297-301.
- American National Standards Institute (ANSI)/Acoustical Society of America. Specification for audiometers (ANSI/ASA S3.6-2004). New York: ANSI/ASA; 2004.
- Stuart A, Stenstrom R, Tompkins C, Vandenhoff S. Test-retest variability in audiometric threshold with supraaural and insert earphones among children and adults. Audiology. 1991;30:82-90.
- Howell RW, Hartley BP. Variability in audiometric recording. Br J Ind Med. 1972;29:432-435.
- Mowrer DE, Stearns C. Threshold measurement variability among hearing aid dispensers. Hearing Instruments. 1992;42(4):26-27.
- Aarts NL, Caffee CS. Manufacturer predicted and measured REAR values in adult hearing aid fitting: accuracy and clinical usefulness. Int J Audiol. 2005;44:293-301.
- American National Standards Institute/Acoustical Society of America. Specification of hearing aid characteristics (ANSI/ASA S3.22-2009). New York: ANSI/ASA; 2009.
- Kochkin S, Beck DL, Christensen LA, et al. MarkeTrak VIII: The impact of the hearing healthcare professional on hearing aid user success. Hearing Review. 2010;17(4):12-34.
- Stelmachowicz PG, Dalzell S, Peterson D, Kopun J, Lewis DA, Hoover BE. Comparison of threshold-based fitting strategies for nonlinear hearing aids. Ear Hear. 1998;19:131-138.
- Kochkin S. MarkeTrak VIII: Reducing patient visits through verification and validation. Hearing Review. 2011;18(6):10-12.
- Lenth RV. Java Applets for Power and Sample Size [computer software download]. 2006-9. Available at: www.stat.uiowa.edu/~rlenth/Power. Accessed May 27, 2011.
- Harris RW. Speech Audiometry Materials (compact disc recording). Provo, Utah: Hearing and Speech Sciences Laboratory, Brigham Young University; 1991.
- Gelfand SA. Hearing: An Introduction to Psychological and Physiological Acoustics. 4th ed. New York: Informa Healthcare; 2007.
- Markides A. Whole-word scoring versus phoneme scoring in speech audiometry. Br J Audiol. 1978;12:40-46.
- Olsen WO, Van Tasell DJ, Speaks CE. Phoneme and word recognition for words in isolation and in sentences. Ear Hear. 1997;18:175-188.
- Boothroyd A. The performance-intensity function: an underused resource. Ear Hear. 2008;29:479-491.
- Jerger J, Malmquist C, Speaks C. Comparison of some speech intelligibility tests in the evaluation of hearing aid performance. J Speech Hear Res. 1966;9:253-258.
- Cox RM, Alexander GC. The Abbreviated Profile of Hearing Aid Benefit (APHAB). Ear Hear. 1995;16:176-186.
- Cox RM. Administration and application of the APHAB. Hear Jour. 1997;50(4):32-48.
- Paul RG, Cox RM. Measuring hearing aid benefit with the APHAB: is this as good as it gets? Am J Audiol. 1995;4:10-13.
- Johnson JA, Cox RM, Alexander GC. Development of APHAB norms for WDRC hearing aids and comparisons with original norms. Ear Hear. 2010;31:47-55.
Citation for this article:
Ghent RM Jr, Anderson DG, Rose DE, Chabries DM. Interactive Binaurally Balanced Fittings for Improved Audibility, Reduced Costs, and Fewer Return Visits. Hearing Review. 2011;18(12):36-43,55.









