How cochlear dead regions can be identified, what kinds of hearing losses are often associated with them, and why
Editor’s Note: This article1 and the interview that follows2 were originally published in the July/August 2003 (Vol 52, No 4) and March/April 2004 (vol 53, No 2) editions of The Hearing Professional, the official journal of The International Hearing Society (IHS). The articles are adapted and reprinted here with permission.
The cochlea is the “retina of the ear.” It changes sound into electrical impulses, and those impulses are the language the brain understands. Just as dead areas of the retina can create holes in one’s field of vision, dead hair cell areas of the cochlea can produce audiometrically useless frequencies. At these frequencies, hearing aid amplification does little or no good.
Brian Moore, PhD, a Cambridge University researcher in areas of psychoacoustics, has developed a protocol, called the Threshold Equalizing Noise (TEN) test, to clinically identify cochlear dead spots. The most interesting thing about this test is not its clinical utility and how well and consistently it identifies cochlear dead spots. Instead, the best thing about this test is that, in order to understand its rationale and how it works, one is forced to understand how the cochlea works.
Outer and Inner Hair Cell Basics
By way of a brief overview, each cochlea contains one row of approximately 3,000 inner hair cells and 3-5 rows of about 12,000 outer hair cells (Figure 1).
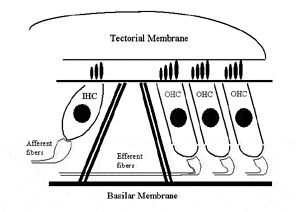
Figure 1. The hairs or stereocilia of the outer hair cells are jammed into the underside of the tectorial membrane, while those of the inner hair cells are not. When soft sounds enter the cochlea, the test-tube shaped outer hair cells shrink, thus pulling the tectorial membrane down, so the stereocilia of the jug-shaped inner hair cells can be bent or sheared.
The jug-shaped inner hair cells send all sound information to the brain; without them we are totally deaf. These hair cells have one fundamental limitation, however: they cannot sense sounds softer than conversational speech.3 More specifically, the inner hair cells cannot sense signals below about 50 dB SPL for the low frequencies and below about 65 dB SPL for the high frequencies.4
The outer hair cells work in the opposite direction; that is, they receive messages from the brain and from within the cochlea telling them to rapidly stretch or shrink. These test-tube shaped outer hair cells are the active mechanism of the cochlea—the moving parts. Their movements help the inner hair cells sense soft sounds.
Sound hitting the eardrum results in a traveling wave of fluid motion inside the cochlea, thus causing a ripple along the floor upon which the hair cells stand (known as the basilar membrane). The stereocilia of the inner hair cells bend or become sheared where the wave peaks. This is what stimulates the hair cells at the cochlea’s wide base (high frequencies) or narrow apex (low frequencies) or at some unique place in between. In short, the wave grows (and slows) as it goes up the spiral-shaped cochlea until it reaches peak amplitude and stops. By the way, the main reason that the wave actually gets a peak in the first place is because it meets impedance along its travels up the spiral. As it is forced to slow down along its spiral route, its energy has to go somewhere; hence, its peak of “vertical” amplitude.
The wave’s peak is even further defined as a result of the action of the outer hair cells. The stretching/shrinking action of the outer hair cells temporarily alters the basilar membrane on either side of the peak. This mechanically forces the peak into a sharper point that, in turn, increases our ability to distinguish between frequencies that are close together. In someone with outer hair cell damage, the traveling wave peak is dull and rounded, and their ability to distinguish frequencies that are close together is diminished (Figure 2). Is it any wonder that those with sensorineural hearing loss (SNHL) and damaged outer hair cells have difficulty separating speech from background noise?

Figure 2. Without the action of the outer hair cells, the traveling wave has a dull and rounded peak. This passive traveling wave stimulates many adjacent frequencies simultaneously. The sharpening of the peak is accomplished with the action of the outer hair cells, and this increases the ability to distinguish between frequencies that are close together.
Why WDRC is Often Recommended
It can safely be said, therefore, that the most common type of damage to the ear is damage to the outer hair cells. This results in the most common type of hearing loss: a moderate SNHL, where soft sounds below conversational speech (50–65 dB HL) are inaudible, yet 90-100 dB HL sounds are perceived as loud as they would be to someone with normal hearing. For this person, hearing aids should amplify the soft sounds significantly and amplify louder sounds by progressively smaller and smaller increments. Wide Dynamic Range Compression (WDRC) hearing aids that accomplish this are specifically intended to imitate what the outer hair cells once did. Outer hair cells begin their work for sounds below 50–65 dB SPL; hence, the knee-point of WDRC is most often found at input levels of around 50 dB, as well.

Figure 3. These idealized, schematic shapes represent three traveling wave envelopes. The top shows a normal traveling wave envelope, resulting from stimulation of two tones different in frequency. The middle shows a traveling wave envelope that is reduced in amplitude. Note also that the peaks are rounded, due to outer hair cell damage. The bottom shows what would happen with amplification. The original traveling wave size or amplitude is restored, but the peaks are still rounded. In other words, the ability to separate speech from background noise has not been restored.
It must be emphasized, however, that no matter how good a hearing aid is, it cannot restore a normal-functioning cochlear traveling wave (Figure 3). When the sharpened peak of a traveling wave becomes dull, it is dull for good. Hearing aids can only amplify and, by so doing, can only enlarge a diminished traveling wave. They cannot restore one’s original sharp frequency resolution or the ability to separate frequencies that are close together. Amplification only increases audibility of sounds, but does not come close to the majesty and wonder of the healthy cochlea.
Essential Cochlear Concepts
Cochlear dead spots occur where there is complete destruction to both the inner and outer hair cells. As mentioned earlier, the gain provided by the outer hair cells to very soft input levels is about 50 dB for the low frequencies and about 65 dB for the high frequencies. Moore says that additional inner hair cell damage can only result in another 25-30 dB of hearing loss beyond 50 dB in the lows and 65 dB in the highs.4 This would make the maximum hearing loss possible from only hair cell damage about 75-80 dB in the lows and 95 dB in the highs.
An important fact to keep in mind is that the traveling wave is asymmetrical in shape (Figures 2-4). This concept is essential in understanding Moore’s test for cochlear dead spots. The traveling wave has a long tail towards the cochlea’s wide base (high-frequency region) and a steep front that is facing the cochlea’s low-frequency apex. This is our hearing physiology and explains “the upward spread of masking,” or that low frequencies mask high frequencies better than vice versa (Figure 4).

Figure 4. The traveling wave is asymmetrical in shape. Soft, high-frequency stimulation results in a small traveling wave at the base of the cochlea (right), which would easily be overcome or masked by the wave resulting from intense low-frequency stimulation at the apex (left). The reverse would not be true. Intense, high-frequency stimulation results in a traveling wave confined to the base of the cochlea (right) and, thus, it would not interfere with the wave resulting from soft low-frequency stimulation (left).
TEN Test Procedures
Moore’s TEN test for cochlear dead spots is available on a CD that can be played over a two-channel audiometer (http://hearing.psychol.cam.ac.uk/dead/ dead.html). The CD plays puretones, as well as a single broadband masking noise (noise that includes all audiometric frequencies). This broad-band noise is quite different from the narrow bands of noise used in our audiometers. The puretones and the masking noise have to be directed toward the same ear, and this can only be done with a two-channel audiometer. One can separately adjust the intensity of the tones and the masking noise by way of the intensity controls on the audiometer and send both to either the right or left ear. You begin by testing for thresholds of the puretones from the CD, and then testing the same ear for thresholds while the masking noise is presented into that ear (ie, ipsilateral masking).
When this article was first published in The Hearing Professional, the TEN test puretones and broadband masking noise were all calibrated in dB SPL, not HL. This is important to note when using the CD. If a client has normal hearing, the thresholds on the typical audiogram will look a bit like a barn roof (Figure 5), with best thresholds showing for the mid frequencies and borderline-to-mild hearing loss appearing for the low frequencies and high frequencies. The reason for this audiogram shape is that normal-hearing ears are most sensitive to frequencies between 1-4 kHz. Incidentally, this is why equalizer buttons on some stereo systems are shaped like a smile; we need the artificial boost for the lows and highs in order to hear all of the frequencies at equal loudness levels. To be sure, there are some complicated calibration issues that would need to be addressed in order to accurately translate the TEN test results to the typical audiogram with which we are all familiar. These, however, are beyond the scope of this introductory article. As of late last year, the TEN test5 is available in calibration of dB HL. This makes it easier to relate test results directly to the audiogram.
The procedure for Moore’s TEN is to first test for hearing thresholds for the puretones from the TEN CD in quiet, and then to retest for the same thresholds in the presence of ipsilateral masking. When using the test, be sure to go to a level whereby the better thresholds of the person are affected (ie, made worse by the masking). Compare the unmasked thresholds to the masked thresholds. The TEN should affect the better thresholds because it is audible to the person at these frequencies. The worst thresholds, however, should not be affected because the TEN should not be audible to the person at these frequencies. If they are, then suspect cochlear dead spots at these frequencies.

Figure 5. Moore’s TEN test on someone with normal hearing. Note that the thresholds from the puretones of the TEN CD produce a convex, “barn-roof” shape. This is due to the calibration of the CD tones in dB SPL, whereas the audiogram is measured in terms of dB hearing loss. Note also, however, that the thresholds masked by 30 dB TEN are only those thresholds that can hear it and not, for example, the worst threshold at 8000 Hz.
For a normal-hearing person, for example, 30 dB of the TEN from the CD should affect most thresholds (Figure 5). If the decibels on the audiogram were in dB SPL, all thresholds would be elevated or shifted to show a flat 30 dB hearing loss. On the typical audiogram (where dB HL rather than dB SPL is used), the barn-roof shaped thresholds for the normal-hearing person are still affected by the TEN. Figure 5 shows that, for any frequency where the broadband TEN is audible, thresholds within the TEN are shifted to at least the intensity of the TEN, so they are simply “pushed lower” down on the audiogram.
For someone with hearing loss, the main idea is to provide enough TEN masking so that the better thresholds are shifted, and determine if the worse thresholds are affected. For example, consider someone with a mild hearing loss for the low frequencies and a moderate hearing loss for the highs. The puretones played from the CD will show a similar trend; namely, better hearing for the low frequencies than for the high frequencies (Figure 6). Note that in the presence of ipsilaterally presented TEN, at 30 dB the thresholds for the puretones from the CD are tested again. A shift for the low-frequency thresholds appears, but this does not occur for the high-frequency thresholds. This only makes sense, because the person was not even able to hear the broadband TEN in the high frequencies.

Figure 6. The ipsilateral masking with 30 dB TEN affects the better low-to-mid frequency thresholds of the sloping SNHL, because the TEN is audible to the person at these frequencies. The TEN does not, however, affect the high-frequency thresholds because the TEN is not audible to the person at these frequencies. This would indicate a typical high-frequency SNHL that is due to damaged hair cells at these frequencies, but not due to high-frequency cochlear dead spots.
Similarly, according to Moore,4 if you masked the worst thresholds by their own minimum masking levels with the TEN, these thresholds should theoretically only be shifted to the level of the TEN used to mask them. Consider now that these worst thresholds are caused by cochlear dead spots: in this case, the minimum TEN level would actually shift the worst thresholds at least 10 dB beyond the decibel levels of the TEN itself. This is because these “worst” audiometric thresholds are not real; they are caused by cochlear dead spots and, thus, are actually far worse than the audiogram would suggest!
More “Suspicious” Cases
One type of SNHL that should give rise to suspicion of cochlear dead spots is a moderate degree of reverse hearing loss; another type is a severe degree of precipitous high-frequency hearing loss. For either type, amplification for the worst thresholds might not be the best course of action. For example, excess high-frequency gain can result in feedback for the person with precipitous hearing loss.
Moderate Reverse-Sloping SNHL. Be suspicious of reverse-sloping SNHL, as it could be indicative of low-frequency dead regions. It is very possible that the person could be completely deaf in the low frequencies; however, due to the asymmetric shape of the traveling wave, only a moderate reverse hearing loss may be revealed.
Consider someone who has completely dead inner and outer hair cells for the frequencies below 1000 Hz. In this case, intense low-frequency stimulation results in a traveling wave with a peak at the apical (low-frequency) hair cell region of the cochlea. The long tail of the traveling wave, however, may still extend into the healthy mid-frequency regions (Figure 7). Even though these low-frequency hair cells might be dead, a moderate amount of low-frequency stimulation might still excite living mid-frequency hair cells, thus causing the person to raise a hand, indicating he/she indeed heard a tone. In this case, the person might be “hearing” these low frequencies with their healthy mid-frequency hair cells, and not by means of their dead low-frequency hair cells!

Figure 7. Low-frequency dead spots may reveal only a moderate, low frequency SNHL with a reverse audiogram. Due to the long tail of the traveling wave, intense, low-frequency stimulation may “excite” the healthy mid-frequency hair cell regions (gray area of traveling wave diagram at top of figure). In this case, the person will indicate a response, but it will not truly arise from hearing in the low-frequency hair cell regions.
Severe Precipitous High-Frequency SNHL. Severe precipitous high-frequency SNHL can indicate high-frequency cochlear dead regions. Here, it is possible that the high-frequency thresholds do not truly arise from damaged high-frequency hair cells. On the contrary, these thresholds might result from indirect stimulation of low-frequency hair cells.
High-frequency stimulation would have to be quite intense to enable the steep front of the traveling wave to extend into the living, healthy mid-frequency hair cell regions. The steep slope of the precipitous high-frequency hearing loss thus might reflect the steep front of the traveling wave as it occurs in the cochlea(Figure 8). In this case, even though the high-frequency hair cells might be totally dead, an intense high-frequency tone might stimulate mid-frequency hair cells, causing the person to raise a hand indicating he/she heard something. The high-frequency thresholds are not truly indicative of high-frequency sensitivity; rather, they are a result of indirect stimulation of remote living hair cell regions.

Figure 8. High-frequency dead spots may reveal an audiogram showing a precipitous, pronounced degree of high-frequency SNHL. Due to the steep front of the traveling wave, intense, high-frequency stimulation may “excite” the healthy mid-frequency hair cell regions (gray area of traveling wave diagram at top of figure). In this case, the person will indicate a response, but it will not truly arise from high-frequency hair cell regions.
Reverse and Precipitous High-Frequency SNHL
With cochlear dead regions of hair cells, one actually hears by means of remote, living hair cells. This is called “off-frequency hearing.” A small amount of ipsilaterally presented broad-band TEN masking noise would elevate the normal (or better) thresholds in the living hair cell regions. In the reverse loss, it would make the good mid-to-high-frequency thresholds worse; in the precipitous high-frequency SNHL, it would make the good low-to-mid frequency thresholds worse. If the reverse or precipitous high-frequency hearing loss were due to cochlear dead spots, the TEN would, however, also elevate the thresholds for the worst thresholds, even though the TEN would theoretically be inaudible to the person at these frequencies!
Specifically, in the case of reverse SNHL, the ipsilaterally presented TEN would shift the low-frequency thresholds, even if these thresholds were greater than the intensity of the masking noise. In the case of the precipitous high-frequency SNHL, the TEN would also make the high-frequency thresholds worse, even if they were greater than the intensity of the masking noise.
Using conventional thinking, we would consider this impossible because, at these thresholds, the listener should not even be able to hear the masking noise. The reason why these thresholds are affected, however, is that, when one has dead hair cell regions at any frequency, one hears tones in these dead areas by means of a small piece of the traveling wave that extends into living hair cell regions. If the TEN masking noise does shift the worst thresholds by 10 dB or more, according to Moore, these thresholds are spurious, and do not actually arise from stimulation of damaged hair cells at these frequencies.4 Instead, in these cases, the worst thresholds arise from indirect stimulation of remote, living hair cells at other frequency regions. Therein lies the rub of Moore’s TEN test!
Of course, if the hair cells in question are only damaged and not truly dead, the same ipsilateral TEN masking noise would not shift these worst thresholds. In the case of the reverse SNHL, a small amount of TEN that was enough to shift the better mid-to-high-frequency thresholds would not affect the poorest thresholds at the low frequencies. In the case of the precipitous high-frequency SNHL, a small amount of TEN might indeed shift the good low-frequency thresholds, but would not affect the worst high-frequency thresholds by anywhere near 10 dB. These hearing losses would then, respectively, be a true reverse hearing loss and a true precipitous high-frequency hearing loss.
Figure 9 shows the thresholds for puretones from the TEN CD, followed by the thresholds found in the presence of 50 dB TEN from the CD. The ipsilateral TEN stimulation of 50 dB SPL should not have any effect on the high-frequency thresholds. In fact, the high-frequency thresholds are indeed affected because they show a shift of at least 10 dB. This finding, says Moore, would indicate cochlear dead spots for the high frequencies.4

Figure 9. The ipsilateral masking with 50 dB TEN affects the low-to-mid frequency thresholds of the sloping SNHL because the TEN is audible to the person at these frequencies. However, the TEN also shifts the high-frequency thresholds by at least 10 dB—even though it is not audible to the person at these frequencies. This would indicate a high-frequency SNHL that is due to high-frequency cochlear dead spots. The high-frequency thresholds thus do not truly arise from damaged high-frequency hair cells; rather, they are a result of stimulation of remote hair cells at the low-to-mid frequencies that are responding to intense high-frequency stimulation (ie, what Moore4 refers to as “off-frequency hearing”).
The implications for amplification are important here; namely, don’t focus on amplification in these extreme high-frequency thresholds. It might be best, in this case, to amplify the low-to-mid frequencies as well as the transition of the audiogram where the thresholds drop.
Summing Things Up
In ears with cochlear dead spots, tones are processed in the dead areas by means of living hair cells located on surrounding regions of the basilar membrane—what Moore refers to as “off-frequency hearing.” Some patients report that these tones do not sound natural or tonal in quality, or that puretone stimulation in these regions gives them the perception of a scratch or a tickle. These subjective reports, however, are not always consistent from person to person, even though dead areas might be indicated.4
The TEN test on the CD is not, in my opinion, a required part of any new test battery for our patients. On the other hand, the presence of reverse hearing loss or precipitous high-frequency hearing loss should make dispensing professionals suspicious that cochlear dead spots might exist. Furthermore, it is a good idea to ask these patients what their perceptions of audible tones presented to their worst thresholds are like. These two items—initial suspicions and secondary questions—might really help in our consideration of how much amplification to provide for a patient’s poorest thresholds. Should we provide low-frequency gain and output for reverse SNHL? For precipitous high-frequency SNHL, should we focus on amplifying the worst high-frequency thresholds or should we concentrate on amplifying the transition or steep slope itself?
Not to be forgotten, of course, is the education of ourselves; that is, understanding the TEN test for cochlear dead spots requires an appreciation for the fascinating way in which our cochleae function.
| Cochlear Dead Spots: The Fitting Zone
By Ted H. Venema, PhD, and Jay B. McSpaden, PhD, BC-HIS
Venema: Dead regions in the cochlea occur when hair cells are completely gone, missing, or absent in certain rows and/or places in the cochlea. The snail-shaped cochlea has two and a half turns or coils. Imagine the rolled-up cochlea to be “unrolled.” When unrolled, it is over an inch long (33 mm). Inside this unrolled tube is a smaller tube. It is within this smaller tube that the hair cells grow along the entire inch of cochlea from end to end. Now imagine there’s an area about the width of your pinkie fingernail—it could be anywhere on the tube—where there are no living hair cells. That area would be a cochlear dead spot. In a dead spot, there is no hearing sensitivity at all. The person is totally deaf at those particular frequencies. Symmetrical dead spots occur when the area of completely missing hair cells is located in exactly the same place (or frequency) within both cochleas of the individual. Of course, the person’s audiogram would show symmetrical sensorineural hearing loss (SNHL), too. If, on the other hand, the dead regions were located in different locations inside the cochlea, they would be asymmetrical and, accordingly, the person would show SNHL at different frequencies (an asymmetrical audiogram). McSpaden: Are cochlear dead spots always hereditary? Venema: Cochlear dead spots are not necessarily hereditary, but certainly can be passed from one or both parents. Cochlear dead spots can also be congenital, which simply means they existed at the time of birth. Hereditary SNHL can have a large variety of degrees and audiometric shapes. It can be found at any frequency, at various decibel levels, and can be symmetrical or asymmetrical. It can thus be mild to profound—and it can look like a flat loss, a reverse loss, a “cookie bite” loss, or a precipitous high-frequency loss. McSpaden: How does a person get a nongenetic cochlear dead spot? Venema: Nongenetic causes can be labeled as “acquired.” Dead hair cell regions causing complete deafness at specific frequencies can certainly be acquired by various causes encountered along one’s journey through life. Noise induced hearing loss (NIHL) is one example of acquired cochlear dead spots. NIHL first becomes evident as a notch or drop in hearing sensitivity around 4000 Hz. It is interesting to note that NIHL occurs at these frequencies because damage due to noise occurs to hair cells that represent frequencies about one-half an octave above the noise that caused it. In real-ear measurement, we can see that the resonance of the adult outer ear canal stretches from about 1500 Hz to around 4000 Hz, with a 10-20 dB peak at around 2700 Hz. If you move this broad peak of added resonance up a half-octave, you’ll find that the damage to cochlear hair cells occurs right between 3000-6000Hz—exactly where NIHL is seen on the audiogram. Audiometric thresholds with NIHL improve beyond 6000 Hz precisely because the resonance of the outer ear canal, which gives the extra dose of noise in the first place, drops off one-half octave lower, just beyond 4000 Hz. When someone has a prolonged exposure to noise, NIHL can become so severe that it results in completely dead high-frequency hair cells, which in turn cause a severe-to-profound precipitous high-frequency SNHL. NIHL can be symmetrical or asymmetrical. Ototoxicity can be another cause of SNHL. In some cases, ototoxicity can result in complete hair cell destruction in certain frequency regions of the cochlea (cochlear dead spots). The most familiar type of ototoxicity is side effects from medications. Some antibiotics known to be toxic to hair cells belong to the family of aminoglycosides. These are drugs that end in the suffix “mycin.” (Note: erythromycin, a common derivative of penicillin, is not ototoxic.) A common ototoxic drug is aspirin; however, it is not known for causing rampant hair cell damage and cochlear dead spots. Aspirin mainly results in tinnitus, and that side effect tends to disappear when the aspirin consumption is stopped. Another cause of cochlear dead spots can be sudden idiopathic deafness (SID). This is almost always unilateral. The prefix “idio” means that the reason for the sudden SNHL is unknown. Usually, in these cases, the only thing we know is that the person experiences a sudden loss of hearing in one ear. Physicians often recommend steroids when patients report SID, but all too often, the hair cell damage is already done by the time treatment is given. Many times, the SID results in almost complete deafness in one ear, with only a bit of residual hearing left at perhaps the very low frequencies. This would be a cochlear dead spot covering a very wide area of the cochlea for which hearing amplification is not very successful. [For detailed information on idiopathic hearing loss, see HR’s special December 2003 edition.] McSpaden: Speaking of amplification, what kind of hearing instrument would you fit on someone with a high-frequency cochlear dead spot? Venema: First let’s look at the challenges that a high-frequency dead spot would present. A high-frequency dead spot manifests itself as a steep, pronounced, precipitous SNHL. The cochlea traveling wave has a long, shallow tail and a steeply sloped front as it moves up the cochlea from the base (where high-frequency hair cells are located) to the apex (where low-frequency hair cells are located). In other words, the steep front of the traveling wave faces the apex or pointed low-frequency end of the cochlea. Consider the person who has dead hair cells in the wide, high-frequency base of the cochlea. If you were to present an intense, high-frequency tone from your audiometer, the peak of the traveling wave would occur in the dead high-frequency area, even though there are no living hair cells there to respond to the tone. The steep slope of that traveling wave front, however, does face the living mid-to-low frequency hair cells, and it will spread slightly into the living mid-frequency hair cells. These hair cells will respond to the high-frequency tone. Thus, the SNHL thresholds in the severe-to-profound high-frequency range do not really come from the traveling wave peak stimulating the high-frequency hair cells because these are dead. Instead, the high-frequency thresholds come indirectly from living mid-frequency hair cells stimulated by the steep front of the traveling wave. We would use the same kind of technology to fit this type of SNHL as we would to fit any other steeply dropping hearing loss. The challenges are the same. How do you fit the severe high-frequency thresholds without, at the same time, providing too much gain and output for the good hearing thresholds in the lower frequencies? Today’s multichannel digital hearing instruments can provide a great start. Even the analog two-channel hearing aids from the mid 1990s can do a good job here. There should be at least two channels—one providing very little gain/output and the other turned way up. The frequency crossover, where the two channels “meet,” should be adjusted to be right at the “corner” of the audiogram, where the hearing thresholds begin to drop off. Another consideration is just how much gain and output one should provide to the severe high-frequency thresholds. Recall that these thresholds may not be real at all, because the high-frequency hair cells are dead! One wonders what these sounds “sound” like (remember, they are hearing them only indirectly) to the individual. Perhaps it is always a good question to ask; if the person reports that the high-frequency tones don’t really sound like tones at all, amplification for these worst high-frequency thresholds may not be a good idea. If you see a person with a steeply dropping audiogram and severe-to-profound high-frequency thresholds, suspect high-frequency cochlear dead spots. Remember, you can “help the dying but you cannot help the dead.” Instead of providing the most gain and output to the worst thresholds, you might want to amplify with less gain and focus on the transition in the hearing loss; that is, amplify along the slope of the hearing loss rather than where it “bottoms out.” In fact, many people in the field advocate this approach for all precipitous high-frequency losses (eg, a glass half-full, rather than glass half-empty approach to amplification), particularly when the sloping section of the audiogram still allows for the amplification of extremely important speech cues (eg, 1000-2500 Hz region). McSpaden: It is difficult to fit someone with a low-frequency rising audiogram such as a “reverse” hearing loss? Is this also true when the low-frequency hearing loss is due to cochlear dead spots? Venema: Fitting a low-frequency rising (or reverse) hearing loss has indeed always been a challenge. The fact that these reverse hearing losses can sometimes be due to cochlear dead spots in the low-frequency region (apex) of the cochlea, however, can actually help shed some light on the situation. If the mid-to-high frequency hearing is normal, even a moderate degree of low-frequency SNHL can be indicative of low-frequency cochlear dead spots. In other words, in the presence of normal mid-to-high frequency hearing, total deafness in the low frequencies can masquerade as a moderate degree of low-frequency SNHL. For reasons why reverse SNHL can indicate cochlear dead spots, imagine the traveling wave shape again; the steeply sloped front faces the apex or low-frequency region of the cochlea and the longer, shallow “tail” faces the base or high-frequency region of the cochlea. Now envision presenting a 250 Hz or 500 Hz tone from the audiometer, so that the peak of the traveling wave is made to occur in the dead low-frequency region of the cochlea. The dead low-frequency hair cells cannot respond, but the long, shallow tail of the wave still stimulates the healthy mid-frequency hair cells. In absence of a true response from the low-frequency hair cells, these healthy mid-to-high frequency hair cells respond in their place, and the person raises his/her hand telling you that the low-frequency tone was heard. As with the earlier case of the steep high-frequency hearing loss, the thresholds do not come from the hair cells that are supposed to represent these thresholds; instead, they arise from remote, living hair cells in another frequency region. In contrast to the case where high-frequency cochlear dead spots cause a steep, precipitous high-frequency hearing loss, low-frequency cochlear dead spots do not have to result in a steeply rising audiogram; reverse SNHL can rise suddenly but it can also rise more gently, like a mirror reflection of the longer, more shallowly sloped tail of the traveling wave. McSpaden: Does everyone with a reverse SNHL have low-frequency cochlear dead spots? What about endolymphatic hydrops (Ménière’s disease)? Venema: One should consider that not all reverse SNHL is due to cochlear dead spots. It is very possible that the person could have a true reverse SNHL due to Ménière’s disease. For that matter, one could also simply have an honest-to-goodness hereditary moderate degree of low-frequency SNHL. Here, the person might indeed benefit from some low-frequency amplification. McSpaden: How would you fit these people? Venema: I would be very careful to provide no more gain than is necessary. Due to the asymmetrical shape of the traveling wave, we know that low frequencies mask high frequencies better than highs mask lows. In the case of true reverse SNHL, it might be a good idea to err on the side of less low-frequency amplification. As in the case of high-frequency dead spots, the person with true reverse SNHL will most likely do best with at least a two-channel hearing aid, either analog or digital. Again, adjust the frequency crossover control so that it is as close to the corner of the audiogram as possible. If the rise in thresholds is gentle and there really is no corner, position the crossover so it is at the middle of the rise in thresholds or generally placed at the middle of the change in thresholds. McSpaden: How do you achieve binaural balance in a patient with symmetrical dead spots using hearing instruments? Venema: I presume that symmetrical cochlear dead spots would result in a symmetrical SNHL. I’d try to achieve binaural balance by providing similar gain and output at similar frequencies, just like I would with anyone else who had symmetrical hearing loss. With multichannel analog or digital hearing aids, I’d adjust the frequency crossover between the channels to the same position. McSpaden: How would you verify that success had been achieved? Venema: I’d use real-ear measurement. It can be done quickly and provides good information. McSpaden: How do you achieve binaural balance in a patient with asymmetrical dead spots that you fit with hearing instruments? Venema: I’d try to accomplish this just like I would when fitting anyone else with an asymmetrical reverse SNHL, or an asymmetrical NIHL—or any other asymmetrical precipitous high-frequency hearing loss. Again, I always try to fit difficult hearing loss shapes with multichannel hearing instruments because I can mold the frequency response of the hearing aid to best fit around the corner in the audiogram. In the case of asymmetrical SNHL resulting from asymmetrical cochlear dead spots, I’d adjust the frequency crossover between the channels at different positions for each ear. I’d adjust the crossover to occur at the specific frequencies where the hearing loss suddenly changed. If the degree of loss was different between ears, of course, one would have to provide different gain and outputs too. McSpaden: How would you verify the outcomes? Venema: I’d use both objective real-ear measures and subjective comments from the person being fit. McSpaden: Are cookie-bite hearing losses due to mid-frequency cochlear dead spots? If so, how would you these? Venema: Cookie-bite SNHL is often a genetic, hereditary type of hearing loss and, yes, it is often due to mid-frequency cochlear dead spots. As we all know, there are people who have a moderate SNHL for the mid frequencies, even though their low- and high-frequency thresholds are normal or near-normal. The moderate degree of mid-frequency thresholds can actually indicate cochlear dead spots in the mid frequencies. Fitting this type of hearing loss is trickier because it requires at least three channels—one for the low frequencies, one for the mid frequencies, and one for the high frequencies. In a three-channel hearing instrument you’d see two frequency crossovers—one between the low- and mid-frequency channels and the other between the mid- and high-frequency channels. If the cookie bite SNHL dropped and rose suddenly, making it look like there were two corners in the audiogram, I’d set the two frequency crossovers right at the corners and go from there. If the loss dropped and rose gradually, I’d adjust the crossover settings to occur around the centers of each of the two slopes. McSpaden: The literature says that peripheral, tonal tinnitus usually occurs in these patients near the “edge” frequency of the cochlear dead spot. Why there? Venema: No one knows for sure, but it might be related to the “tuning curves” of the hair cells in the cochlea. We know these people always “recruit” loudness at this frequency and that this recruitment may well involve the mitochondria of the hair cells, but we don’t know if these things are related. McSpaden: Tell me about “compression” for these patients. Venema: If the hearing loss is moderate in degree, as is often found in reverse SNHL, I would use WDRC. If the loss is severe, as in the case of some pronounced precipitous high-frequency hearing losses, I would still use WDRC because I’m not providing tons of gain to fit the severe high-frequency thresholds. Fitting the slope is the main thing, and the slope is not as severe as the worst degree of the hearing loss. Along with considerations of compression, I’d really try to use directional microphones. They have been shown again and again to improve speech understanding in background noise. McSpaden: I can think of a number of patients that had a precipitous SNHL who might well have had a dead spot. Can we always tell? And where do you get Moore’s TEN Test? Venema: It’s quite hard to tell because we don’t routinely check inside people’s cochleas to determine whether or not the hair cells along certain frequency areas are dead. It’s best to use your clinical acumen, experience, and ability to listen to the person’s observations about tonal quality in the suspected dead spot. Take a look at the audiometric shape to see if you should be suspicious in the first place. Does the SNHL take a precipitous drop in the mid-to-high frequencies and then bottom out at a severe dB level? Does it look like a reverse rising audiogram? Does it have the cookie-bite shape? Encountering any of these shapes should raise one’s eyebrows. Next, ask the person if tones presented into the suspected “dead zones” truly sound like “tones.” If they don’t, you should back off from providing amplification to those areas. I wouldn’t necessarily shut things off and provide no amplification; rather, I’d simply turn the focus of the transition frequencies along the slope or the rise of the hearing loss. Brian Moore’s TEN CD enables one to test for the presence of cochlear dead spots (visit http://hearing.psychol.cam.ac.uk/dead/ dead.html). You can plug a CD player into the tape inputs of a 2-channel clinical audiometer. Conclusion Correspondence can be addressed to HR or Ted Venema, PhD, at [email protected], or Jay B. McSpaden, PhD, at [email protected]. |

|
References
1. Venema TH. Identifying cochlear dead spots. The Hearing Professional. 2003;52(4):15-20.
2. Venema TH, McSpaden JB. Cochlear dead spots. The Hearing Professional. 2004;53(2):19-22.
3. Venema TH. Compression for Clinicians. San Diego: Singular Publishing Group Inc; 1998.
4. Moore BCJ. Dead regions in the cochlea: Diagnosis, perceptual consequences and amplification for the fitting of hearing aids. Trends in Amplif. 2001;5(1),1–34.
5. Moore Brian CJ, Glasberg BR, Stone MA. Dead regions in the cochlea. Ear and Hearing 2004;25(5):478-487.






