V & V can eliminate the need for over 521,000 patient refitting visits annually
The analysis completed from 533 patient responses indicates that the combined use of verification and validation (V & V) will result in an average of 1.2 less visits. It should be apparent—given consumer-related mobility and convenience issues, patient satisfaction issues, and the professional business/labor cost issues—that V & V should be considered a “best practice” or “standard” service for all patients fitted with hearing aids.
We have all heard the old adage “time is money.” In our recent paper,1 it was determined that the number of patient visits to adjust hearing aids was highly correlated with real-world success. In comparing patients who experienced above- or below-average success with their hearing aids, the following was discovered:

Sergei Kochkin, PhD, is executive director of the Better Hearing Institute, Washington, DC.
- 76% of patients with above-average success were fit in 1 or 2 visits compared to 40% of patients who experienced below-average success.
- 47% of patients with below-average success required 4 to 6 visits to fit their hearing aids compared to only 7% of patients who experienced above-average success.
In short, highly successful patients required fewer visits to the clinic. What could explain this difference in number of visits? It is hypothesized that a lack of verification (real-ear measurement) and validation (confirmation of a patient’s performance with their hearing aids) during the hearing aid fitting increased the number of patient visits. For some patients, the result was a less-than-optimum fit, reduced hearing aid utility, and mediocre benefit—each of which accrues to result in rejection and/or the return of the hearing aids for credit.
In this study, we will explore the relationship between verification, validation, and patient visits. Future studies will explore the impact of verification and validation on hearing aid returns.
Methods
We queried the MarkeTrak VIII database for patients fit with hearing aids between January 2008 and January 2009 (the month MarkeTrak was fielded). The reader is referred to earlier publications describing methodology and description of the MarkeTrak VIII database.1-3 Before we explore the relationship between verification, validation, and patient visits, it is important that we rule out extraneous variables explaining above-average patient visits during the hearing aid fitting process; to this point, neither degree of hearing loss in deciles (p<.62) nor age (p<.26) explained significant variance in patient visits.
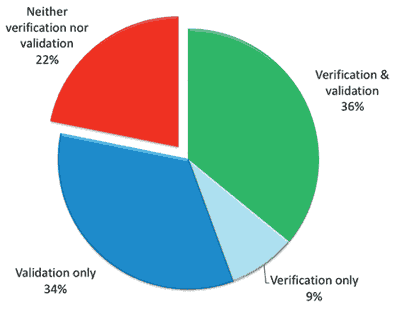
FIGURE 1. Percent of patients reporting that verification (eg, real-ear measurement) and/or validation (eg, benefit/satisfaction survey) was used during the hearing aid fitting process (n=787).
Results
Figure 1 shows the use of verification and validation for 788 subjects fit with hearing aids between 2008 and early 2009. About one-third (36%) of patients reported they were fit with hearing aids using verification and validation (either subjective or objective), another third (34%) had their hearing aid fit validated but not verified, 9% were fit using real-ear measurement (REM) without validation, and 22% reported they received neither verification nor validation during the hearing aid fitting process.
Figure 2 shows average patient visits as a function of whether they were fit with real-ear measurement, validation procedures, or neither (patients who were “not sure” if verification and/or validation was used are excluded). The analysis completed from 533 patient responses (R-Square=.06, F value=11.19, df=3, correlation=.24, p<.0001) indicates that the combined usage of verification (p<.008) and validation (p<.0001) results in an average of 1.2 fewer visits. The interaction of verification and validation was marginally significant (p<.06). The beta weights in this model indicate that validation may possibly reduce patient visits more than REM.
The previous observation confirms that the use of verification and validation in fitting hearing aids decreases the number of visits per hearing aid fitting. As an extension to this analysis, the impact of including these best practices on the US hearing healthcare market was estimated.
In 2010, nearly 2.7 million hearing aids were fit in the US hearing aid market,4 representing over 1.5 million patients (binaural fitting rate of 74.3% in 2008).2 Assuming the same distribution of best practices as noted by patients in Figure 1 and the estimate of reduced patient visits in Figure 2, it is suggested that the systematic utilization of both verification and validation procedures while fitting hearing aids will reduce patient visits by a total of 521,779 visits. This is an opportunity available for every one of the 64% of US practices not utilizing both verification and validation.
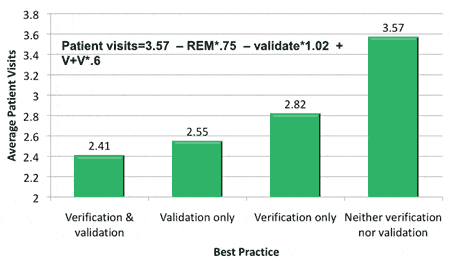
FIGURE 2. Average patient visits to fit hearing aids based on use of verification (REM) and validation procedures (objective or subjective).
Assuming 45 minutes a visit, inclusion of these best practices could reduce the time spent with patients in fitting hearing aids by 391,334 hours in a single year in the United States. This additional time frees the hearing care professional for additional counseling, marketing, community outreach, or fitting new patients with hearing aids. It also represents a significant convenience savings for patients who often have multiple disabilities that can include challenges in mobility, danger from falls, and other potential problems.
Conclusions
The utilization of verification and validation during the hearing aid fitting process was shown to significantly reduce patient visits (1.2 fewer visits), with evidence that utilizing both verification and validation may compound to yield the best results. According to patients, one-third of hearing care professionals in the United States utilize both verification and validation during hearing aid fitting. The MarkeTrak VIII data suggest that wide-scale adoption of verification and validation in the hearing care market will increase patient satisfaction1 and reduce patient visits by more than a half million in the United States. Given the profound implications for the hearing care field, systematic study and verification of these findings in a more robust clinical study is warranted.
Get Your Monthly Copy of Hearing Review

You can now have Hearing Review delivered to your home, workplace, or computer each month! Subscribe now.
If your practice is similar to the 64% highlighted in this study, there is opportunity for growth that could begin today. Simple modification to routine clinical protocol can result in significantly improved patient outcomes. Real-ear measurement is a quick and easy step that should be included in every hearing aid fitting. Validation with a standardized outcome measure is just as easy. An objective pre-post measure is preferred; however, if this is not possible, a brief questionnaire such as the International Outcome Inventory for Hearing Aids (IOI-HA)5—available for free in 21 languages— can provide valuable insight into patient satisfaction and real-world benefit.
It can be argued that time wasted during unnecessary patient visits could be better utilized in improving quality care for existing patients or in the treatment of new patients. After all, time is money!
Acknowledgement
This study was made possible by a special grant from Knowles Electronics, LLC, Itasca, Ill.
References
- Kochkin S, Beck D, Christensen L, Compton-Conley C, Fligor B, Kricos P, McSpaden J, Mueller G, Nilsson M, Northern J, Powers T, Sweetow R, Taylor B, Turner R. MarkeTrak VIII: The impact of the hearing healthcare professional on hearing aid user success. Hearing Review. 2010;17(4):12-34.
- Kochkin S. MarkeTrak VIII: 25-year trends in the hearing health market. Hearing Review. 2009;16(11):12-31.
- Kochkin S. MarkeTrak VIII: Customer satisfaction with hearing aids is slowly increasing. Hear Jour. 2010;63(1):11-19.
- Hearing Industries Association. Quarterly statistics report. Washington, DC: HIA; January 2011.
- Cox RM, Stephens D, Kramer SE. Translations of the International Outcome Inventory for Hearing Aids (IOI-HA). Int J Audiol. 2002;41:3-26. The IOH-HA is also available at: www.memphis.edu/ausp/harl/ioi-ha.htm.





