Utilizing research that focuses on pulse rate signals and how they can evoke highly synchronized cortical responses, SoundCure’s S-tones are designed to inhibit and reduce perceived tinnitus—and provide a new science-based tool for hearing care professionals.
The idea that external sounds can have a substantial impact on tinnitus is well accepted. There are a variety of sound therapy tools and masking devices (including hearing aids) that work well for tinnitus patients. However, many of these devices are “hit or miss” in their effectiveness and rely on everything from pure-tones to music.
SoundCure has developed an approach that introduces “cortically interesting” sounds designed by researchers to positively alter the abnormal neural activities related to tinnitus in order to reduce tinnitus perception. Different from steady-state sounds, which produce mostly onset and offset responses in the cortex, the temporally patterned sounds used by SoundCure—primarily modulated pulse rate signals—are said by researchers to produce highly synchronized and robust cortical responses that assist in tinnitus remediation.

SoundCure CEO Bill Perry
Recent research reported in the April edition of the Journal of the Association for Research in Otolaryngology (JARO) has supported the SoundCure approach. Consequently, HR recently interviewed SoundCure CEO Bill Perry about the company and its S-tones.
HR: There’s a pretty interesting science story behind the genesis of SoundCure. Can you tell us about it?
Perry: It is an interesting story. It basically starts in 2006 with a patient who was referred from his surgeon to Fan-Gang Zeng, PhD, a professor at the University of California Irvine. This patient, a former musician, had been troubled with chronic tinnitus for such a long time and extent that he resorted to the rather radical step of getting a cochlear implant specifically to deal with his tinnitus [studies have established that CIs can provide tinnitus relief for certain patients]. Unfortunately, the implant did nothing to improve his symptoms.
Although Dr Zeng is now very well known in the field of tinnitus, when this patient showed up at his lab, he had never really focused on tinnitus; rather, he’d had many, many years of clinical experience with cochlear implants. Dr Zeng started working with the patient in multiple sessions involving electrical stimulation with the implant to find some sort of tinnitus relief. Because they really didn’t know what would work, they tried almost everything: high-rate stimulation, stimulation on a range of different electrodes, etc. As Dr Zeng describes it, they essentially threw the kitchen sink at the problem.
Much to their surprise, low rate stimuli [ie, 40 to 100 Hz] at a certain electrode provided dramatic relief for this patient. And it was the kind of relief in which he essentially stopped everyone and said, “Wait. Don’t move. Let me enjoy this moment of not hearing my tinnitus.” The case study is detailed in a peer-reviewed paper that states: “During the first 150 seconds of this low-rate stimulus, nothing happened as the subject perceived both the stimulus and his tinnitus. Surprisingly at the 180 seconds mark, the subject, for the first time in two years, could not hear any of the high-pitched tinnitus. All he heard was a calming, pleasant tone produced by the low-rate stimulus.”1
That was really the “eureka moment” in finding what SoundCure now calls S-tones, and it was completely unexpected. In fact, many researchers had theorized that high-frequency, high-rate stimulation [3000 to 8000 Hz] might be useful in the treatment of tinnitus.
Dr Zeng and his colleagues were understandably surprised by this finding. So they went through an exhaustive review of independent research on the subject of low-rate stimulation and how the brain processes these signals. They found a 2001 paper written by researchers at Johns Hopkins along with a follow-up paper in 2002 involving mammalian brain activity and low-rate stimulation.2,3 It should be emphasized that these papers did not focus on tinnitus. Instead, they were about how low-rate pulse modulation between 40 and 120 Hz can produce sustained, synchronized neural activity in the brain. If the stimulation was lower than 40 Hz or higher than 120 Hz, it was as if the brain didn’t pay attention or couldn’t keep pace with the signals. However, in that kind of “sweet spot” from 40 to 120 Hz, there was synchronized, robust, sustained brain activity. Again, these were studies unrelated to tinnitus, focusing instead on how the mammalian brain responds to stimulation.
Dr Zeng and his team found this pretty interesting. They had one patient who had experienced substantial tinnitus relief from low-rate stimulation, and they had found some very interesting independent research that might explain why this stimulation might positively affect tinnitus. But, obviously, that’s not enough. In scientific research, you need to verify an approach in a series of patients.
HR: And this led to the ATA-funded study and the recent publication in JARO?
Perry: Exactly. They submitted a grant request to the American Tinnitus Association (ATA). As you can imagine—judging from the large number of different proposed tinnitus remedies on the market—the ATA gets a lot of grant proposals, and it therefore has a very rigorous vetting process. But, ultimately, the ATA provided a 2-year grant that Dr Zeng’s team used to study 20 patients with chronic tinnitus. In the study, the patients listened to five types of sound comprising 17 individual external sounds, presented randomly, for a total of 340 trials. So it was a rather laborious process of the patients listening to sounds and rating their subjective tinnitus before, during, and after the sounds were presented during many hours of testing.
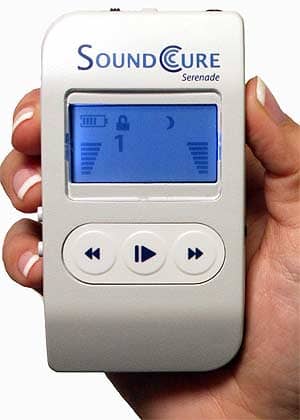
The SoundCure Serenade is a handheld device that is programmed much like a hearing aid using a computer and USB cable. The sound therapy device offers three customizable tones (two S-tones and one narrowband sound), as well as a broadband sound.
The results,4 which were published in the April 2012 edition of JARO, detailed an acute effect of how the patients have the perception of their tinnitus reduced when listening to these treatment sounds. It’s really fascinating work because it finds that the pulse rate sounds were the most effective at reducing tinnitus, but—very importantly—at a lower volume level than the patient’s perceived tinnitus. A total of 90% of the subjects experienced at least some suppression, defined as a reduced loudness with a sound presented at a lower volume than the patient’s tinnitus perception, with at least one of the stimuli. The greatest suppression was achieved with pulse rate tones with frequencies near the tinnitus pitch, or what SoundCure calls S-tones, and these tones were 4 times more likely to provide relief than white noise.
In total, about one-third [35%] of the study participants achieved a 70% or better reduction in their tinnitus, one-third [35%] achieved a 30% to 50% reduction, and one-third [30%] experienced less than a 30% reduction. In the study, no patients reported a worsening of their tinnitus.
HR: So, compared to traditional masking, how do S-tones improve the prospects for tinnitus management?
Perry: I think the way to look at it is maskers often work fairly well; they cover the perceived tinnitus and/or distract the tinnitus patient with another sound like white noise, music, etc. But the concept of masking relies at least partially on signal loudness. For example, if a tinnitus patient perceives the loudness of his/her tinnitus as a 7 on a rating scale of 1 to 10, then depending on how good the signal is at masking their specific tinnitus perception, the masker will generally need to be at a volume level of 7 or more.
With S-tones, research has indicated that the patient can listen to them at a much lower volume level, for example 2 to 4, with substantial reduction in tinnitus perception in many cases down to a 3 or 4 rating—and even better for some “home run” patients. As Dr Zeng has said, the uniqueness of the S-tones is that they reduce the sound burden by not substituting one intrusive sound and sound level for another.
It’s generally accepted that the perception of tinnitus is usually in the high frequencies because that’s the location of the damage in the auditory system. White noise has broadband components. If you can’t hear well at high frequencies, your low frequency perception really picks up on that broadband or white noise—and the white noise can be too loud in the low frequencies (where hearing is better) to be loud enough to mask tinnitus in the higher frequencies (where hearing is worse). So, with traditional masking, patients have to pick their poison: Do they want to hear a loud sound or do they want to hear their tinnitus?
With S-tones, our goal is to play the tones as quietly as possible and still get acute relief and lower the sound burden. We want to make things quieter for the patient and not just cover one sound with another. And you can read about all of this in the research and clinical articles.1-5
HR: And from this research, SoundCure and your Serenade device came into being?
Perry: Correct. Allied Minds is an investment firm that invests in early-stage university technology, and they have about 15 subsidiaries that fall into the life sciences and physical sciences categories. Essentially, the company maintains relationships with universities and finds intellectual properties (IPs), usually in the form of patents or technologies, then licenses and incubates these for a few years. If the technology looks promising, they’ll build a company around it.
That’s what happened with our company. In 2009, about 3 years after that first patient walked into Dr Zeng’s lab, Allied Minds created SoundCure. I joined the company in 2010, and we’ve built an excellent team with a lot of experience in medical device commercialization. I’m very proud of our staff. We’ve been able to get effectively through the product development and FDA clearance process [in August 2011]. We then did an early pilot-launch in September in a defined region where we determined exactly how we should train and support clinicians.
Our formal launch was at the American Academy of Audiology (AAA) convention during April in Boston where we were absolutely swamped with attendees. I’ve been involved in medical device start-ups since 1992, and I’ve never seen a product launch where we were flooded at a booth with literally hundreds of solid leads. It was wonderful.
HR: To what do you attribute that?
Perry: First, I think it shows that there is a large market need. There are a lot of audiologists and hearing care providers seeking a tinnitus solution. Second, there are literally millions of patients looking for ways to cope with and treat their tinnitus using a long-term solution. Third, I think SoundCure spent a lot of time doing the appropriate scientific research, market research, and ground-work to bring to market a product with the right features and a full clinical support program. We help train professionals for patient evaluations, fitting, and follow-up. Our message is not “Here’s a gizmo for tinnitus.” Clinicians can use our device in their own tinnitus management program, or we can help them from A-to-Z in establishing a program.
Finally, I think most audiologists and hearing professionals are starting to understand that a tinnitus program is increasingly becoming a good way to help build a practice. The economics of it make sense with the way we’ve priced it and created the business model.
HR: Some of the MarkeTrak data6 that HR has published suggest tinnitus remediation could represent the same scale of economic impact as the binaural hearing aid revolution. Would you agree with this?
Perry: I agree completely. I think this is an excellent healthcare opportunity. The ATA and almost everybody in hearing care realizes how widespread tinnitus is. According to the ATA, about 50 million people have tinnitus, of which as many as 20 million adults are at least moderately bothered by it. And a subset of this population—perhaps 1 to 2 million—are so severely impacted by tinnitus that it interferes with their ability to lead a normal life. Tinnitus is the number-one chronic condition of veterans in our military.
These are some pretty eye-opening facts, and I think audiologists and all hearing care professionals are starting to understand that this can be, and should be, a huge healthcare opportunity—as well as a significant economic and marketing opportunity for their businesses.
HR: Can you describe how the hearing care professional programs and prescribes the Serenade device?
Perry: By design, the system is very similar to the hearing aid programming process. Serenade is a handheld device that is about the size of an iPhone. With the USB cable we provide, the clinician connects it to their computer, and the patient is tested through the earphones of the Serenade that he/she will take home.
The session, from beginning to end, takes about 1 hour. About 25 to 30 minutes of that time is used in testing hearing levels, upper loudness limits, loudness growth functions, frequency pitch matching, etc. At the end of this testing, you hit the program button and those parameters are downloaded to the device. The Serenade is not a simple mp3 player or a device that stores recorded music. The clinician places the specific parameters customized for that individual patient on a chip so the device can generate the sounds in real-time for the patient.
The clinician then takes about 5 minutes to explain how the patient uses Serenade. It’s a very simple device to use with very few buttons. It has independent left/right volume control, a sleep-assist timer so it can be programmed to turn off automatically, it has a datalogging function for clinical tracking of use, as well as other functions that will be familiar to most dispensing professionals. We have also created a counseling presentation in a narrated format that allows the clinician to play it and add comments when appropriate or stop whenever the patient might have questions.
HR: For those dispensing professionals who do not have an established tinnitus program, what kind of training do you provide?
Perry: We have developed a resource kit that has everything in one package, and the kit caters to multiple levels of involvement by a practice owner. So, for example, if you’re interested in adding a tinnitus evaluation center to your practice, we can train you on what is needed, how to test, and the procedures involved in billing the proper CPT codes. Of course, we also train in the basics like programming the device, managing patient flow through the practice, conducting a patient triage in deciding how to manage patients relative to audiometric and tinnitus evaluations, talking to patients about sound therapy, offering options from which they can choose, and helping them figure out if they’re a good candidate for sound therapy.
We also cover counseling and follow-up. We do much of this through intensive primary care training that usually lasts about 4 hours in the clinician’s office, as well as follow-up training and consultation during first fitting. We’ve learned that everybody wins when the support is there and there’s a complete approach.
HR: What about for professionals with an established tinnitus program or who are currently using other tinnitus-related products?
Perry: We view our product as a tool to be used in any tinnitus management program. The Serenade has four tracks of treatment sounds on it, with three types of customizable sounds: two customized S-tones, one customized narrowband sound, and a broadband sound.
Our goal is to offer a more complete sound therapy device that either can be used as another tool in clinician’s armamentarium, or we can provide a full management program that includes training. Our device has gone to experienced clinics that might use several tinnitus devices and are looking for another option—and Serenade functions very well that way.
We have an approach for short-term relief, and importantly, we have an approach for long-term relief. In this way, we offer a “standard habituation model” that we train our sites on, with guidelines on how to achieve habituation for patients. Ultimately, we believe that you need to address the neural component of tinnitus with sound therapy, and you need to address the perceptual component with long-term counseling and habituation.
So, if someone is running an experienced tinnitus clinic, we have a great tool that they can use within their existing program. Alternatively, if they are inexperienced in tinnitus management, we also have the ability to teach them from A to Z. Serenade represents both a tool or a full-service approach.
HR: There is a minority of tinnitus patients who have more problems and issues than the typical dispensing professional may be able to handle. What do you recommend when encountering such a patient?
Perry: One of the things we cover in our training are the different factors that indicate when you should refer the patient somewhere else. Clearly, there are patients who need to be seen by an ENT or other professionals for some cases of severe tinnitus. There may also be some broader psychological indicators, such as severe depression, that you want to identify.
We recommend that every provider has a comfort level and a care level that is realistic for their own practice, and that they be able to refer patients to specialty clinics if they’re uncomfortable with the level of care that can be provided or if some of these warning flags surface. So, we train on identifying patients with moderate to severe tinnitus who do not have the warning flags [and would make good candidates for SoundCure]. There are also some very good tools to screen some these factors like the Beck’s Depression Index and other similar questionnaires. So, in summary, we certainly do recommend that some patients be referred to specialty clinics when necessary.
But these certainly are not the majority of tinnitus patients. Yes, you do have to be trained, you do have to provide support, and you have to manage a suitable tinnitus program. And, yes, there are patients you may need to refer occasionally—there is an excellent and vital role for specialty clinics.
But those patients are the exception and not the rule. Unfortunately, we also realize that the exceptions are often the cases that get talked about most. It’s the “war stories” that get attention at conventions or over a cup of coffee with a colleague, and this can lead to mistaken conclusions. In fact, the vast majority of tinnitus patients can be treated with the full-service approach on which we provide training…And, if you do that, you will provide a great service to a large number of people who need help with their tinnitus. Hearing care professionals are the professionals who should be, and need to be, doing this work. — KES
References
- Zeng et al. Tinnitus suppression by low-rate electric stimulation and its electrophysiological mechanisms. Hear Res. 2011;Jul;2007(1-2):61-6.
- Lu T, Liang L, Wang X. Temporal and rate representations of time-varying signals in the auditory cortex of awake primates. Nat Neurosci. 2001;4(11):1131-1138.
- Liang L, Lu T, Wang X. Neural representations of sinusoidal amplitude and frequency modulations in the primary auditory cortex of awake primates. J Neurophysiol. 2002;87(5):237-261.
- Reavis KM, Rothholtz VS, Tang O, Carroll JA, Djalilian H, Zeng FG. Temporary suppression of tinnitus by modulated sounds. JARO. 2012;13(4):561-571. Available at: www.springerlink.com/content/fk1126x5l228051h
- Reavis KM, Chang JE, Zeng FG. Patterned sound therapy for the treatment of tinnitus. Hear Jour. 2010;60(11):21-24.
- Kochkin S, Tyler R. Tinnitus treatment and the effectiveness of hearing aids: hearing care professional perceptions. Hearing Review. 2008;15(13):14-18.
Citation for this article:
Strom KE. Novel Sound Therapy: SoundCure Harnesses Research on Brain Science in Fighting Tinnitus Hearing Review. 2012;19(08):52-54.




