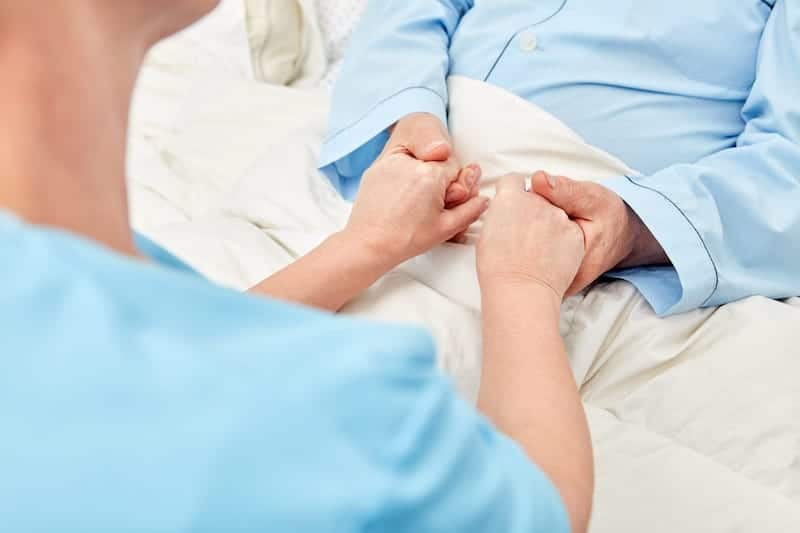
HCPs can dramatically improve the quality of end-of-life care for people with hearing loss by facilitating communication at a vital time.
By Douglas L Beck AuD, F-AAA, CCC-A
It’s no secret that most of our patients are older, often in their 60s, 70s, 80s, and beyond.
Souza1 reports that by 2044, the population of people over age 85 will triple. She says hearing loss is not inevitable but is often a consequence of aging. Souza found that 40% of people over age 65 have hearing loss, 60% of people over 75 years, and 80% of people over age 85. As age increases, so does all-cause hearing loss. This means that a large percentage of older adults who enter hospice for end-of-life care have hearing loss, yet hearing care is seldom available for this population. Let’s delve into the reasons why this is the case and why it is so concerning.
Age-Related Hearing Loss
There are many reasons why hearing loss occurs, secondary to a lengthy life span. In some respects, damage to the auditory system is cumulative, like radiation exposure. It builds up over the years and eventually creates havoc. The effects of noise exposure from concerts, recorded and live music, headsets, radio, TV, industrial and military noise, weapons, air travel, construction, alarms, motorcycles, chainsaws, lawnmowers, and leaf blowers happen daily. After 60, 70, or 80 years of hearing and listening in an industrialized noisy society, hearing loss is not unexpected.
Darrow2 reports that age-related hearing loss (ARHL) is ultimately a multi-factorial progressive neurodegenerative disease. ARHL most often results from a genetic predisposition, oxidative stress, inflammation, and often, a lifetime of auditory insult (noise, acoustic trauma, ototoxic medications, etc.). Darrow states that although ARHL often starts with simple outer hair cell damage, it progressively worsens such that the neural connections between the inner hair cells and auditory nerve are damaged and degraded, ultimately creating havoc as the central nervous system attempts to compensate for an attenuated and distorted auditory input.
Livingston and colleagues3 stated that 60% of the risk factor for dementia is due to age and DNA, neither of which is modifiable! However, 40% of the potentially modifiable risk factors for dementia include untreated hearing loss (the largest of the potentially modifiable risk factors), untreated hypertension, untreated diabetes, social isolation, air pollution, depression, less education, alcohol, drug abuse, and more.
Although many licensed hearing care professionals (HCPs) know and prioritize this information, the public and most other professionals do not. Perhaps the value and impact of hearing and listening with regard to emotional and physical well-being, cognition, brain health, and the ability to understand in difficult listening situations are simply trivialized or ignored by most professionals and the public.
An Uninformed Public
Jiang, Mishra, Shrestha, et al.4 reviewed the UK Biobank cohort study of 437,000 adults aged 40–69. Their data was gathered between 2006 and 2010 across 22 centers in the United Kingdom. They reported in The Lancet that for people with hearing loss who use hearing aids, the risk of dementia is similar to that of people without hearing loss. They noted an “urgent need” to address hearing loss to improve cognitive decline.
However, other professionals (non-HCPs) and mainstream news sources are often misaligned or not up to date with the discipline-specific scientific community. This misalignment may lead to incorrect or incomplete information delivered to the public and the resultant (and unfortunately) typical dismissive approach to hearing loss.
For example, one of the most well-known neurosurgeons in the U.S. is Sanjay Gupta, MD. Dr Gupta is CNN’s chief medical correspondent and appears to be a wonderful, compassionate, and caring person. He is soft-spoken, very bright, knowledgeable, and an endearing storyteller. Yet, in his 2021 book “Keep Sharp: Build a Better Brain at Any Age” he neglects (i.e., hardly mentions) the importance of hearing and listening to build and maintain a healthy brain. To me, that otherwise informative and excellent book is typical of the way mainstream “medical” news is delivered to, and received by, the public. Hearing and listening are often ignored despite their monumental importance to brain health, cognition, education, knowledge, language, psychology, and emotional and physical well-being.
Fortunately, other professionals (doctors, audiologists, neuroscientists, neurologists, etc.) do report the importance of hearing and listening to maintain, nourish, and grow a healthy brain. Yet these books, articles, and information remain invisible to most professionals and the public.
For example, Daniel Levitin’s unforgettable 2007 book “This is Your Brain on Music.” Levitin explores and explains how music (in particular), as well as language, emotion, psychology, and more, work cohesively to coordinate human thought.5 He indicates that creating and expressing sounds and hearing and listening to sounds (often percussion and other core/basic sounds) may be the foundation of expressive and receptive language.
Nina Kraus6 wrote that comprehending sound is an extraordinarily difficult task. In her book “Of Sound Mind,” she addresses the partnership of sound and brain and that hearing is “always on.” She states we can generally choose to attend to or ignore sound as we desire. Kraus reports we don’t just “hear” sounds; we engage with them. She addresses how our brain interacts with sound, memories, knowledge, language, vocabulary, emotions, thoughts, movement, and more.
Bryson7 states hearing is a “seriously underrated miracle.” His book “The Body” is simply an extraordinary read for professionals and non-professionals.
Harvard’s Pinker8 addresses how spoken (and perceived) words (i.e., expressive and receptive speech) mold, limit, and lead our thoughts. Pinker argues we may experience linguistic determinism. That is, our language, particularly the words which are most often used and learned via speaking, hearing, and listening, determines, limits, and expands our thoughts. He states that expressive and receptive language is the medium between sound (hearing/listening) and thought.
As such, the importance of hearing and listening regarding brain health remains a vast, outcomes-based, peer-reviewed, and generally untold and unknown story for many/most people. People with hearing loss and listening disorders often experience increased anxiety, depression, and stress, notably because their primary communication ability is compromised. People with hearing and listening disorders are often told by well-meaning and (sorry to say, misinformed) professionals…” it’s just hearing loss” or “we all have it” or “get used to it…it’s normal for your age” and other regrettable, unfortunate, incorrect, and damaging misinformation.
People with hearing loss and listening disorders (sub-clinical hearing loss, functional hearing loss, suprathreshold listening disorders, and more) are likely to misunderstand, require clarification, need repeats, and sometimes, they just “mishear.” Of note, most people with hearing and listening difficulty can significantly benefit from a complete audiometric evaluation* and professional services and recommendations to improve their ability to hear and listen, even in difficult and challenging listening situations, such as cocktail-party noise.
* [Please note, I did not say “hearing screenings.” Hearing screenings by HCPs for most adults are (frankly) a waste of time (my opinion) and can often lead to a false conclusion. Of the 335 million Americans, some 38 million will demonstrate hearing loss on an audiogram and will fail a “hearing screening.” Yet, another 26 million will present with hearing difficulty and speech-in-noise problems and normal thresholds and will pass a hearing screening,9,10 as they did not receive a best practice recommended speech-in-noise test and did not complete a listening and communication assessment and more. As such, their “sub-clinical” audiologic difficulties were not quantified, recorded, or discovered. Accurate, correct diagnostic answers can only be determined when all the questions are asked via a comprehensive audiometric evaluation in accordance with AAA, ASHA, and IHS Best Practice guidelines. Other ill-advised tests include whisper tests, watch ticking tests, and the like, as they imply (incorrectly) that if one hears a whisper or a watch tick, that “normal hearing” is present, which is quite often an incorrect and damaging assumption.]
Hospice and Hearing Healthcare
Given the above concerns, facts, and opinions, consider scenarios that occur as people approach the end of life. Unfortunately, the lack of preparation for the end of life is common. Curiously, most people do not have a will.11
In 2015 I wrote an op-ed for The American Academy of Audiology.12 I reported Scientific American (SA) stated that most Americans had not had an end-of-life discussion with their family or physician. SA reported that doctors, nurses, and medical students needed to learn more about these issues and should be more accessible to dying patients, all of which makes sense. However, I wrote that SA missed an essential player in their otherwise excellent article. They missed us. It is rare for HCPs to be involved with hospice or palliative care.
The Rise of Hospice Care
Hospice (as we know it) likely started in the United Kingdom in the 1960s based on the practice and protocols of Dr Dame Cicely Saunders. After Elizabeth Kubler-Ross wrote “On Death and Dying” in the late 1960s, the ideas, concepts, and need for end-of-life care became more widely known and quickly accepted. In 1978, the National Hospice Care Organization (NHO) was founded, and by 1980 Josefina Magno became the first executive director and president of the NHO. In 1982, the US Congress created a Medicare Hospice benefit, and through the mid-1980s multiple insurance plans added hospice care.
While researching this article, I read (and I vaguely recall) that Jack Klugman (he played Oscar on the TV show The Odd Couple) did the first Public Service Announcement (PSA) for hospice in 1982.13
In 1983 the Joint Commission Accreditation Program was implemented, and by 1985 the Hospice Medicare benefit was made permanent. By 1992 the National Hospice Foundation (NHF) was established. In 2004, more than one million people acquired hospice care. These details came from the National Hospice and Palliative Care Organization (NHPCO) website.14
Further reading: Seven Steps to Establishing a Hospice Hearing Program in Your Community
Although solid numbers are hard to establish, my estimate, based on my reading and interpretation of the literature, is that more than 7,500 facilities are managing hospice locations across the USA (in 2023), and probably an additional 10,000 or more home health agencies which provide hospice care. The NHPCO website15 reports 1.5 million Medicare beneficiaries received hospice care in 2018, some 50% of Medicare decedents (people who have died) were enrolled in hospice at the time of death, and the average length of stay in hospice that year was 90 days.
Hospice care might be described as palliative care for those who more than likely have 6 months or less to live. Palliative care is, more or less, pain and symptom management when a cure is not likely, or not possible. When a patient enrolls in hospice, the individual is no longer trying to cure their terminal illness or related conditions, and their doctor has determined those efforts are not working. In the USA, hospice care is regulated by Medicare and is essentially about maintaining comfort for the terminally ill during the end of life and requires a medical doctor to anticipate and sign off on the very probable 6-month (or less) timeline.

How Hearing Loss Affects Communication for Hospice Patients
Notably, the average age of a hospice patient upon admission to hospice was 73 years of age (22 years ago).16 Further, recall that (see above, paragraph one) 40% of people above age 65 have hearing loss, as do 60% of people over age 75 years, as do 80% of people over age 85 years. As such, we expect at least half (probably much more) of hospice patients to have hearing loss.
Belisomo17 noted relationships at the end of life are among the most important. People at the end of life need to be able to communicate with friends, family, and loved ones, as well as children and grandchildren.
As reported by Smith, Ritchie, & Wallhagen,18 presbycusis can interfere with the patient-professional relationship with specific regard to symptom management, the goals of care, and end-of-life decision-making. They reported the results of 510 responses from 315 MDs, 50 registered nurses, 48 nurse practitioners, 58 social workers, and 39 chaplains. Ninety-one percent said hearing loss impacted the quality of care for older adults, yet 87% reported not screening for hearing loss.
Ironically, 61% of respondents were comfortable with their own communication skills regarding patients with hearing loss. Seventy percent of the 510 respondents reported their management approach included speaking directly into the patient’s ear, while 42% reported speaking to the caregiver, both of which are “non-recommended” strategies. The authors reported, “Knowledge about management approaches and resources is sub-optimal.”
In brief, palliative care and hospice providers believe presbycusis impacts care for patients, yet only 13% screen for hearing loss, despite a high prevalence of hearing loss at the end of life. The authors state hearing loss remains “largely a silent and underappreciated problem.”
In 2019, Wallhagen, Ritchie, & Smith19 reported hearing loss impacts the quality of care provided to people with serious illnesses. They report that undiagnosed and unmanaged hearing loss disrupts the identification, assessment, and treatment of the physical, psychosocial, and spiritual issues the patient is experiencing. The authors report hearing loss should be formally addressed, practitioners should screen for hearing loss, and practitioners should use protocols that facilitate understanding and comprehension, including assistive listening devices and other services and products as needed.
A more recent report by Maidment, Wallhagen, Dowd, and colleagues20 noted that HCPs need to be part of an integrated, multi-disciplinary team to facilitate holistic and person-centered care for older adults. They also reported that healthcare professionals (non-hearing care professionals) should be mindful of their patients’ hearing and listening ability and should refer to HCPs as indicated.
Why HCPs Are Missing from Hospice Care
I have recently had confidential conversations with hospice nurses and others employed in various hospice settings. In those discussions, I informally queried as to the management of people in hospice care with specific regard to their hearing healthcare and communication needs.
I am disappointed to report that, apparently, very few hospice facilities have contracts with or refer to HCPs with regard to the communication (i.e., hearing, listening, amplification) needs of their patients. Although hearing loss is prevalent and, indeed, prominent in most patients served, hearing loss and listening disorders remain generally unaddressed.
Why?
Although hospice providers/locations receive per diem reimbursement based on the needs and location of the patient, hospice care is reimbursed via Medicare under Part A (inpatient services) and through some Medicare Advantage plans. Of note, although hospice is required to provide services such as spiritual care, pre-and post-bereavement care, social worker care, etc., it is not required to provide additional diagnostic (i.e., audiologic) services.
Therefore, if the hospice facility/provider were to recommend comprehensive audiometric evaluations and professional HCP care, the costs for these services would likely be a private pay cost to the patient or the family. Frankly, it seems highly unlikely that the HCP fees would be paid for from the established per diem, as that would lessen the revenue for the hospice facility, many of which struggle to make ends meet.
Let me state clearly, I have the utmost respect for hospice and the professionals who dedicate their careers to making the end of life easier and pain-free for those to whom it is availed. I am 100% onboard, and I remain grateful for and very appreciative of the services they provide. I admire their mission and their impressive and dedicated compassion.
However, my admiration for the work and services they provide does not prevent me from pointing out the obvious: that end-of-life care should absolutely include HCPs to help assess and manage hearing and listening disorders to facilitate maximal communication at this uniquely important time.
As such, I encourage and urge all HCPs to contact their local hospice facilities to see if they might arrange a mutually beneficial, consultative, professional relationship. Unfortunately, as noted above, it appears such a relationship would need to be financially managed directly by the patient or their family. This is a very difficult situation and not one with a clear or easy answer.
Nonetheless, I can assure HCPs who seek and establish these relationships that working in collaboration with hospice will be rewarding, intense, and among the most gratifying professional experiences they will participate in.
Douglas L. Beck, AuD, F-AAA, CCC-A, is an audiologist and consultant who serves on the Hearing Review editorial advisory board as the senior editor of clinical research and writes for multiple audiology, science, medical, and health-related professional organizations globally. He retired as vice president of clinical sciences at Cognivue Inc in June 2023. To learn more: www.douglaslbeck.com
Photos: Dreamstime
References:
- Souza, P. Hearing loss and aging implications for audiologists. ASHA. 2014:(11). https://www.asha.org/articles/hearing-loss-and-aging-implications-for-audiologists/ Accessed June 18, 2023
- Darrow, K. Keith Darrow AuD, PhD. personal correspondence. 2020.
- Livingston et al. Dementia prevention, intervention, and care: 2020 report of the Lancet Commission. The Lancet. 2020;Aug 8:396(10248):413-446. doi: 10.1016/S0140-6736(20)30367-6.
- Jiang, Mishra, Shrestha, et al. Association between hearing aid use and all-cause and cause-specific dementia: an analysis of the UK Biobank cohort. The Lancet. April 13, 2023
- Levitin, DJ. This is Your Brain on Music. The Science of a Human Obsession. Plume;2006.
- Kraus, N. Of Sound Mind. How Our Brain Constructs a Meaningful Sonic World. The MIT Press;2022.
- Bryson B. The Body. Penguin Random House;2021.
- Pinker S. The Stuff of Thought: Language as a Window Into Human Nature. Penguin Books;2007.
- Beck DL, & Danhauer. Amplification for adults with hearing difficulty, speech in noise problems – and normal thresholds. J. Otolaryngology-ENT Research. January 2019.
- Beck DL. Beyond the audiogram: whole-brain hearing and listening. The ASHA Leader https://leader.pubs.asha.org/do/10.1044/leader.FTR2.27112022.aud-assessment-sin.44/full/ November 15, 2021.
- Jones J. How many Americans have a will? June 23, 2021. Gallup www.News.Gallup.com/poll/351500 Accessed Jun 20, 2023.
- Beck DL. Considerations for dying patients. 2015. available at www.douglaslbeck.com.
- National Hospice Organization PSA with Jack Klugman. 1982.https://youtu.be/L1wiqv8wo1s
- National Hospice and Palliative Care Organization (NHPCO). History of hospice care. www.nhpco.org/hospice-care-overview/history-of-hospice/ Accessed June 20, 2023.
- National Hospice and Palliative Care Organization. New facts and figures report on hospice care in America. https://www.nhpco.org/hospice-facts-figures. August 17, 2020. Accessed June 20, 2023.
- Vitetta L, Kenner D, Kissane D, & Sali A. Clinical outcomes in terminally ill patients admitted to hospice care: Diagnostic and therapeutic interventions. J. Palliat. Care. Summer 2001;17(2). 69-77.
- Belisomo R. Hearing loss an oft-overlooked problem for hospice patients. Reuters. February 4, 2015. Accessed June 20, 2023.
- Smith, AK. Ritchie, CS. & Wallhagen, ML. Hearing loss in hospice and palliative care: a national survey of providers. Journal of Pain Symptom Manage. 2016;(2):852, 254-258.
- Wallhagen ML, Ritchie CS, & Smith AK. Hearing loss effect on hospice and palliative care through the eyes of practitioners. J. Pain Symptom Manage. 2019;(4):57;724-730.
- Maidment DW, Wallhagen ML, Dowd K, Mick P, Piker E, Spankovich C, & Urry W. (2023). Age Ageing. 2023;(2);52: doi:10.1093/ageing/afad020.