Contacting existing customers and processing patient data are vital tasks for your office/practice. Here’s how to do it.
| Brian Taylor, AuD, is the professional development manager at Unitron in Plymouth, Minn. | 
|
Once the front office staff (FOS) in your practice has demonstrated a mastery of booking appointments, greeting patients, and managing the opening moments of a challenging situation with a patient,1 the next step is to encourage them to develop these relationship-building skills in a focused direction that will continue to grow your practice. Although there are many ways an effective FOS can help your practice excel, this article will focus on two important, yet underappreciated, tactics. When each of them is methodically executed each day, an improvement in your business is sure to follow. The two tactics addressed in this article are: 1) In-office marketing, and 2) Information gathering.
In-Office Marketing
In comparison to direct marketing, in-office marketing involves any activity in which your practice is engaged in directly communicating with patients who already have a relationship with your practice. Distributing educational literature with your practice’s name and location on it or sending birthday cards to patients in your database are examples of in-office marketing tactics.
Another in-office marketing tactic that can be executed by the FOS is referred to as “pulling charts and making calls.” This in-office marketing tactic involves the FOS systematically reviewing your existing database and actively calling patients to schedule an appointment for a follow-up visit. The purpose of this scheduled visit is to professionally clean and check the hearing instruments, retest hearing thresholds, and further the relationship your practice has fostered with the patient.
The process of pulling charts and making phone calls engages the FOS in one of the central functions of any organization: marketing. Although there are a seemingly endless number of marketing strategies and tactics a practice owner or manager can engage in, they are all designed to serve one important purpose—bring people through your door.
Considering well over half of the business generated in any given year in a typical practice is from existing patients who are purchasing another pair of hearing aids or related services, it simply makes sense for the FOS to spend time each day reminding patients to schedule an appointment to visit your office for a routine follow-up.
|
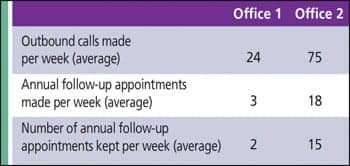
| TABLE 1. An example of comparing two offices and the number of outbound calls and follow-up appointments made over 1 year. |
Requiring the FOS in your practice to systematically pull charts and make phone calls can prove to be an effective tactic, as Table 1 attests. Using examples from two offices with equal-sized patient databases, the importance of proactively contacting your patients is demonstrated. Office 1 has a competent FOS who is not employing any in-office marketing tactics. Although these employees are executing the three essential skills of an effective FOS as reviewed above, Office 1 is not fully engaging the FOS in any in-office marketing tactics. On the other hand, Office 2 not only proactively involves the FOS with in-office marketing, but also carefully tracks all activity. In this particular case, Office 2 is booking 15 more annual follow-up appointments per week on average. Granted, these are relatively short appointments, but each personal contact your practice makes with a patient is an opportunity to educate the patient about new technology, ensure hearing aids are working well, and solidify the patient-provider relationship.
The bottom row of Table 1 shows the number of appointments actually kept. For obvious reasons, this is an important number to track. Because it’s an extension of the proactive nature of trying to schedule annual follow-up appointments, it’s included as part of the tracking process, as FOSs need to routinely confirm all appointments by phone one business day before they are scheduled.
As a general rule, the FOS needs to spend 30 minutes per day pulling charts and making calls. Here is a step-by-step procedure for executing this in-office marketing tactic.
How to Book 1-Year Follow-Up Appointments
Step 1. For 2 to 3 hours per week, review your database and identify patients who have not been seen in your office for 1 year or more. During your search, be sure to include all patients who purchased hearing aids from your office or received a hearing test or other service and didn’t acquire hearing aids from your practice.
Step 2. Call patients who have not been seen in 1 year or more, using the following script as a guideline:
- “Hello. This is _____ calling from [your practice’s name] on [say address] in [say city]. May I speak with Mr/Ms [say last name of patient]?”
- “Hello, Mr/Ms ____ I am calling you today about the hearing aids you purchased from us [say date]. Since it’s been over a year, we wanted to make sure everything was all right with them. How are they working for you?”
- Acknowledge what they just said, then you say: “We recommend that you get your hearing aids cleaned and checked once a year. There is no additional charge for this appointment. We just want to make sure we are doing all we can to keep the hearing aids working at their best for you.”
- “Would you be able to come in next week some time? How about Monday or Tuesday?”
- “If you have any questions, [name of dispensing professional] will be able to address them at your appointment. Do you remember how to get here?” [Give them the address if needed.]
Step 3. For patients who do not schedule an appointment, refile their information back into the database and call the patient again in 3 to 5 weeks. After two attempts to schedule, mail the patient a written reminder on a postcard.
Step 4. For patients who have purchased hearing aids from your practice but are extremely busy and unable to come in for an appointment, offer the opportunity for them to drop off the hearing aids for cleaning and checking.
Managers do not have to limit FOSs to identifying charts and calling patients in need of an annual follow-up appointment. Patients purchasing hearing aids more than 6 months ago clearly benefit from a thorough cleaning and electroacoustical analysis of their devices. Another group FOSs can target with this tactic are patients who were seen in your practice for hearing testing but did not purchase instruments.
Information Gathering: Taking Some of the Burden Off You
The second tactic important to the long-term effectiveness of any FOS is information gathering. The involvement of the FOS in the information-gathering process stems from the need to incorporate evidence-based practice (EBP) guidelines into our business. Although the execution of evidence-based practice guidelines is beyond the scope of this article, it’s important to note that EBP relies on self-reports or questionnaires as the gold standard for gauging the effectiveness of hearing aids and other treatment recommendations. In a world in which professionals are pressed for time, employing a well-trained FOS in the information-gathering process—at least on a cursory level—contributes to the success of your practice.
There are several dimensions of hearing aid outcome that the FOS can help begin to capture using a questionnaire during the pre-fitting appointment, including hearing handicap, personality, and self-efficacy (self-confidence). Although it’s never a good idea for the FOS to participate in the case history and communication assessment, the FOS can contribute to the pre-fitting appointment by handing out and scoring a standardized self-report.
One example of how the FOS contributes to the information-gathering process is the use of a pre-fitting questionnaire like the Hearing Handicap Inventory for Elderly-Screening (HHIE-S)2 during the pre-fitting appointment. The HHIE-S is a 5-minute, 10-question self-report that measures the social and emotional impact of hearing loss. The higher the score, the greater the perceived handicapping effect of hearing loss. A further advantage of the HHIE-S is that it can be administered to both the patient and the companion.
One of the practical aspects of the HHIE-S is that the clinician can be cued to cases of denial or a disconnect between the patient and spouse before the fitting, which are all excellent points of discussion with the hearing care professional during the actual pre-fitting appointment. The role of the FOS is simply gathering the information and scoring the self-report in order to save the hearing care professional time during the pre-fitting appointment.
Most dispensing professionals recognize that objective audiometric measures do not offer a complete understanding or description of a patient’s communication status, as the relationship between traditional audiometric measures and real-world hearing aid success is weak. Furthermore, self-reports—which systematically capture the patient’s perspective regarding hearing aid results—are considered the gold standard in the ever-popular evidence-based practice model. For these reasons, it is logical to consider administering self-reports that evaluate many of the non-audiological dimensions of hearing aid outcome.
|
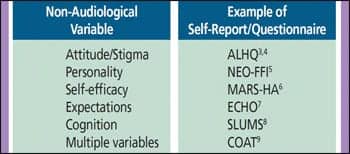
| TABLE 2. The various non-audiological dimensions of hearing aid outcome, along with self-reports used to measure each dimension. All of these self-reports could be administered by the FOS while the patient is waiting to see the provider. |
Unfortunately, one of the drawbacks of administering self-reports is their time-consuming nature. One way to reduce this burden on clinical time is to involve the FOS.
Some of the reliable and valid self-reports that need to be considered by the practice manager and are administered and scored by the FOS during the pre-fitting appointment are summarized in Table 2.3-8 One or two of these self-reports can be administered while the patient is waiting in the reception area prior to their first appointment with the provider. All of the questionnaires listed have been reported in the literature to be both valid and reliable measures of the non-audiological variables of hearing aid outcomes.
In practical terms, the Characteristics of Amplification Tool (COAT)9 may be the best choice for the busy clinician because it captures several of the non-audiological dimensions of hearing aid outcome. The COAT questionnaire, developed by researchers at the Cleveland Clinic, can be downloaded and customized to your liking. One of the advantages of the COAT is that patient responses can be used to have a more focused discussion about many of these important non-audiological variables during the pre-fitting appointment.
Summary
Gathering pre-fitting information using questionnaires and working your existing database to schedule routine follow-up appointments are straightforward tactics that, when faithfully executed by the FOS, can have a profound impact on the overall productivity of your practice. In order to put these ideas into action, managers must formally train their staff, provide feedback, measure results, and look for opportunities to continually improve.
References
- Taylor B, Black K. Three essential skills for TOP performance. Hearing Review. 2008;15(9)38-42.
- Ventry I, Weinstein B. The hearing handicap inventory for the elderly a new tool. Ear Hear. 1982;3(3)128-134.
- Saunders G, Cienkowski K. Refinement and psychometric evaluation of the attitudes toward loss of hearing questionnaire. Ear Hear. 1996;17(6)505-519.
- Cienkowski K, Saunders G. Client-attitude questionnaire provides data that can help shape counseling strategies. Hear Jour. 2000;53(9)42-49.
- Costa P, McCrae R. Longitudinal stability in adult personality. In Hogan R, Johnson JA, Briggs SR, eds. Handbook of Personality Psychology. San Diego Academic Press; 1997269-290.
- West R, Smith S. Development of a hearing aid self-efficacy questionnaire. Int J Audiol. 2007;46759-771.
- Cox R, Alexander G. Expectations about hearing aids and their relationship to fitting outcomes. J Am Acad Audiol. 2000;11(7)368-382.
- Banks W, Morley J. Memories are made of this recent advances in understanding cognitive impairment and dementia. J Gerontol A Biol Sci Med Sci. 2003;58314-321.
- Sandridge SA, Newman CW. Improving the efficiency and accountability of the hearing aid selection process. Available at www.audiologyonline.comarticlesarticle_detail.asparticle_id=1541. Accessed July 28, 2009.
Correspondence can be addressed to HR or Brian Taylor, AuD, at .
Citation for this article:
Taylor B. Two Proven Ways to Engage Front Office Staffers in Your Practice Hearing Review. 2009;16(8):34-37.




