The Mediterranean is a sea of cultural, as well as political and social, contradictions. It is where democracy was born and tyranny flourished. If you have ever spent time in southern Europe, you probably found these contradictions to be intense, striking, and at times exciting. Just ask George Clooney why he owns a villa on Lake Como. As you would expect, the Mediterranean way of life finds its way into how hearing care is practiced in this part of the world.
When you talk to medical professionals from the Mediterranean, you soon find they pride themselves on being spontaneous and unstructured in their clinical approach.1 If you thought professionals didn’t follow protocols in North America, just try to get Mediterranean providers to use them. To an American or northern European, this improvisational approach may seem unorganized and impulsive. However, with a little insight, you soon realize that there is something to be learned from “feeling” rather than just methodically following a protocol.
The other thing you realize is this improvisational approach to patient care is a lot like the best jazz music. There is a lot of cacophony on the surface, but underneath all the dissonance is harmony and brilliance. After you’ve taken the time to understand it, you realize it just makes sense. The aim of this article is to provide the North American clinician with a framework for how to incorporate the Mediterranean approach in your own work with patients.
Embracing the Journey
Probably the best way to approach the improvisational way to patient care is to think of your relationship as a journey of discovery. Conducting a consultation appointment with a customer is a lot like planning and preparing for a long journey—it’s important to get organized before you go.
Many Mediterranean dispensing professionals pride themselves on taking the time to get emotionally connected to each patient. To some, this may feel like crossing the line between effective patient care and friendship; however, to the Mediterranean, getting to know someone on a deeper level is extremely important if you want to help them.
Spontaneous free-flowing dialogue with the patient is more important than an accurate audiogram. Many Americans would be uncomfortable with this approach; simply going off on a spontaneous dialogue without controlling the content of the message seems nerve-wracking. That’s where having some structure is preferable.
Therefore, Figure 1 might serve as a road map. It will help you decide where you need to go with your conversation.
Step 1. Get to know the person, not just the hearing loss. This is the part of the conversation where you find out if the customer is motivated to get help and if they are ready to accept it from you.
Sounds simple, but it is not. Customers are not always ready to instantly open up and talk about sensitive topics like hearing impairment. They have to feel comfortable in our presence. It just makes sense to not only take the time to break the ice with some small talk, but to also make sure we provide a warm and nurturing environment.
Think about the last time you had something on your mind that was making you feel uncomfortable. In most cases, it takes a while to feel comfortable enough with someone to actually start talking about it. It’s up to us to make the customer feel comfortable in our presence. This could take a long time, and to some of us, this first stage could seem very inefficient. However, getting to know the person (not just the hearing loss) is absolutely critical.
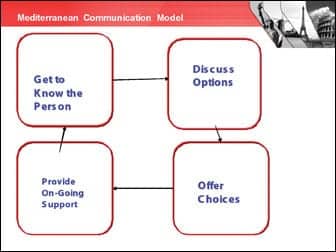
|
| Figure 1. The road map for the Improvisational Counseling Approach discussed in this article. |
TIP Use an open-ended needs assessment tool, like the COSI,2 to list and prioritize as many detailed goals for hearing aid use as you can. These goals should flow naturally out of the conversation. Additionally, a Mediterranean approach requires that you stick with the dialogue and resist the temptation to put the patient in the test booth too soon.
Once we have begun to make the customer feel comfortable and unveil some of the reasons they are in the office, we need to take an even more active role in listening and trying to understand the patient. A good way to improve your listening is to think of each patient as a unique riddle that needs to be solved. Galileo, the great 17th-century Italian scientist, challenged conventional wisdom by proving that the earth rotates around the sun. Your discovery does not have to be quite so monumental; all you need to do is be curious enough to ask good questions and patient enough to listen to the answers.
Step 2. Discuss options. Once you have moved the conversation to the point where you sense the patient is feeling that you understand them, it is time to begin a dialogue about results and treatment options. In Mediterranean countries, providers relish the opportunity to communicate with enthusiasm how much they can help the customer with their treatment options. The Mediterranean hearing care professional tends to value both the fundamental significance of scientific culture and its practical value.1 This means that an audiologist from southern Europe is more likely to give what may seem to be a meandering explanation of results and treatment options to the customer. Many North Americans have been taught that long-winded explanations of results are inefficient and even a waste of time. These long and detailed explanations, however, when viewed from a Mediterranean perspective, indicate to the customer that the professional is extremely knowledgeable and perhaps, more importantly, passionate about their profession.
TIP Remember that it is human nature to feel your needs and wishes are being understood. One trap many providers fall into is talking too much and allowing the customer to feel they are not being heard or listened to. While it is important to passionately communicate, take the time to ask the extra questions for clarification.
Step 3. Offer choices. This is another way to summarize or close the appointment. So far, during the conversation, you have discovered the needs of the patient, and discussed some options as they relate to what you have discovered in your needs assessment. Now you need to involve the patient in the final decision to do business with you. Depending on the content of the conversation, you are probably going to offer the patient anywhere between two and three amplification options. Your job is to make sure the choices are understood by the customer. It’s then up to the customer to make a decision that you will support.
TIP If you practice in a clinic that is more retail oriented, it helps to offer choices at distinct price points. Always include a decisive price for each choice you recommend. However, if you have taken the time to really get to know the wishes and desires of the customer, there is a good chance you don’t need to spend much time on this step.
Step 4. Provide ongoing support. Providing ongoing support is akin to saying goodbye to your colleague at the end of the day, knowing you will see them tomorrow. You need to make sure you have told the customer that the initial conversation is the beginning of long-standing occasional conversations you will have together. Providing ongoing support is probably the most effective way to get to know your customer even better.
TIP Be sure to tell the customer at the end of the first visit that you will be there for them if they need any assistance along the way. Offering reassurance is essential and moves the conversation to the next level.
In an age when evidence-based practice is gaining popularity, investing the time and energy into the improvisational journey can add tremendous value for the customer. In fact, using an improvisational approach is a great complement to evidence-based practice.
Taking a more Mediterranean view of how to practice has its rewards. When we improvise in our communication with customers, we are more likely to make the customer feel they are being listened to. We may not be able to measure this value, but the customer can intangibly feel it and will want to do business with us.
References
- Greco P. Towards a “Mediterranean model” of science communication. J Sci Comm. 2004;3(3):1-5.
- Client Oriented Scale of Improvement. Available at: www.nal.gov.au. Accessed November 21, 2007.
Correspondence can be addressed to HR at [email protected] or Brian Taylor at .
Listening to Understand: 5 Tips
You don’t have to be from Palermo or Seville to appreciate the power of effective listening. No matter what part of the world you come from, your success as hearing care professional is largely predicated on your ability to build relationships with patients. In fact, probably the most effective professionals around the world have one unifying feature: The ability to be excellent listeners.
The important question is, what exactly does it means to be an effective listener, and how can I improve this essential skill. When you break it down, there are really just two types of listening. One type is “listening to understand.” The second type is “listening to respond.” Most professionals have been unknowingly trained to “listen to respond.” During the pre-fitting appointment, however, we must “listen to understand.”
When we are sitting face to face with a patient for the five hundredth time, it is easy to anticipate what the patient is going to say. In fact, it is quite common and even expected that we interject our opinions and thoughts throughout the process. In order to improve your ability to “listen to understand”, take the time to occasionally repeat or paraphrase what the patient just said. Regardless of your cultural heritage, these simple 5-steps will improve your ability to build better relationships with your patients. They might appear to be obvious, but many professionals do not consistently implement them.
1. Square up with your shoulders and face the patient. This sends the message that you are focused on what the patient is going to say. Squaring your shoulders also sends the message of respect.
2. Look them in the eyes. When you fail to look the patient in the eyes during the conversation, it sends the message that you are not interested in them. When you are talking with one person, about 70% of the time you should be looking them in the eyes. More than 70% is considered staring. Less than 50% is perceived as disinterest.
3. Smile. This will send the message that you are open minded and pleasant to work with. In short, having a smile will break down barriers.
4. Nod your head. This sends the message that you are following the conversation and trying to have a good relationship with the patient.
5. Take notes. To go one step further, tell the patient that you need to capture as many details as possible and you need to take notes during the conversation. Think about this: People like it (and probably feel more important) when you take notes during a conversation.