Hearing loss has been linked to mutations in at least 100 different genes, but up to 16% of genetic hearing loss can be traced to just one gene, STRC, the second most common genetic cause. A first-of-its-kind gene therapy technique developed at Boston Children’s Hospital successfully replaced the mutated protein, stereocilin, in the inner ear and reversed severe hearing loss in mice — sometimes to normal levels of hearing. Findings were published December 15 in the journal Science Advances. An article detailing the research appears on the EurekAlert website.
Related article: TAU Scientists Develop Gene Therapy for Deafness
The technique could also be used in other situations where the therapeutic gene is very large, says Jeffrey Holt, PhD, a scientist in the departments of otolaryngology and neurology at Boston Children’s and the study’s senior investigator.
The team will now test whether the technique works with the human stereocilin gene and test it in a human inner ear cells in a dish, derived from patients with STRC hearing loss. If gene therapy restores auditory function at the tissue level, Holt hopes to apply to the FDA for permission to test it in humans.
Restoring contact
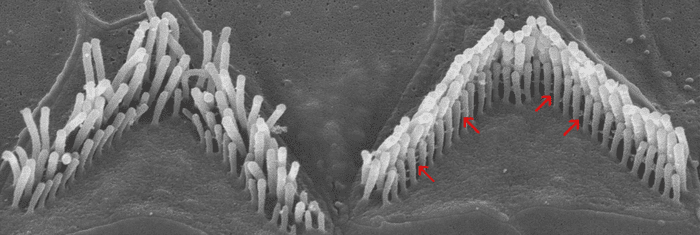
For sounds to be heard, sensory hair cells in the inner ear must make contact with the ear’s tectorial membrane, which vibrates in response to sound, and then convert these vibrations into signals sent to the brain. The stereocilin protein acts as a scaffold, helping the hair cell microvilli stand up together in an organized bundle, so that their tips can touch the membrane.
“If stereocilin is mutated, you don’t have that contact, so the hair cells are not stimulated properly,” said Holt. “But importantly, the hair cells still remain functional, so they are receptive to the gene therapy. We think this will provide a broad window of opportunity for treatment – from babies to adults with hearing loss.”
Creating a new kind of gene therapy
To deliver a healthy stereocilin gene, the team used a synthetic adeno-associated virus (AAV) that is effective in targeting hair cells.
“The challenge we faced was that the gene for stereocilin is too big to fit into the gene therapy vector,” said Holt. “The gene is about 6,200 DNA base pairs long, but the AAV only has a capacity of 4,700 base pairs.”
Olga Shubina-Oleinik, PhD, the study’s first author, came up with a solution: she split the mouse STRC gene in two, and put the two halves in two separate AAVs. She then used an existing technique called protein recombination, where two halves of a protein find each other and hook up. But in this case, it didn’t work.
“We then realized that the beginning of the protein has a short stretch of amino acids that acts like an ‘address,’ directing the protein to its proper place in the cell,” says Shubina-Oleinik. “When we split the protein in half, we realized that one half had the signal, but other half did not, so the halves might not end up in the same location.”
When they added the signal to both halves of the protein, the two halves successfully came together. The researchers found robust restoration of full-length stereocilin protein in the mice and normal-appearing hair bundles that were able to contact the tectorial membrane.
Hearing restoration
The researchers used two types of hearing tests: one similar to hearing tests used in babies, and a test using electrodes on the scalp to measure auditory brainstem responses to a range of sound frequencies and intensities. On testing, the mice were found to be much more sensitive to subtle sounds and showed improved cochlear amplification — the ability to amplify soft sounds, tamp down the response to loud sounds, and discriminate among sounds of different frequencies more precisely. In some mice, hearing was restored to normal levels.
“The results were remarkable and are the first example of hearing restoration using dual-vector gene therapy to target sensory outer hair cells,” said Shubina-Oleinik.
Shubina-Oleinik and Holt have filed a patent application for the gene therapy technology. According to co-author Eliot Shearer, MD, PhD, a clinician-scientist in otolaryngology at Boston Children’s Hospital, approximately 100,000 patients in the US and 2.3 million worldwide carry STRC mutations and could potentially benefit from this therapy.
“It turns out that STRC gene variations are more common than we thought, which makes gene therapy for this disorder so important,” said Shearer, who worked with the Children’s Rare Disease Cohort Initiative to screen a large genomic data set for STRC mutations.
The study was supported by the IDDRC (grant no. 1U54HD090255), the Rare Disease Cohort initiative at Boston Children’s Hospital, the Jeffrey and Kimberly Barber Fund for Gene Therapy Research, the Usher Syndrome Society, and the Foundation Pour l’Audition. Holt is a scientific founder of Audition Therapeutics and an advisor to several biotech companies focused on inner ear therapeutics, and is an inventor on a patent for use of AAV9-PHP.B for gene delivery to the inner ear. The authors declare no other competing interests.
Original Paper: Shubina-Oleinik O, Nist-Lund C, French C, Rockowitz S, Shearer AE, Holt JR. Dual-vector gene therapy restores cochlear amplification and auditory sensitivity in a mouse model of DFNB16 hearing loss. Science Advances. 2021;7(51).
Source: EurekAlert, Boston Children’s Hospital, Science Advances
Image: Carl Nist-Lund, Holt/Géléoc Lab, Boston Children’s Hospital