Research | October 2020 Hearing Review
The acoustic challenges posed by face coverings for people with hearing loss
By Louise Martin, MSpPathSt
The COVID-19 pandemic and the necessity of wearing masks have made life doubly difficult for people with hearing loss. Here is a literature review from the National Acoustic Laboratories (NAL) on the ways in which face masks and shields have been shown to challenge people with hearing loss.
The COVID-19 pandemic has increased the use of face masks and face shields among health professionals and the general public. The use of face masks is known to adversely impact on aspects of communication, and this has created unique challenges for the hearing-impaired community who may be put at a greater communication disadvantage than those with normal hearing.1 National Acoustic Laboratories (NAL) is aware of these challenges and is working to provide innovative research and solutions. The following aspects of communication may be impacted by the wearing of face masks/face shields:
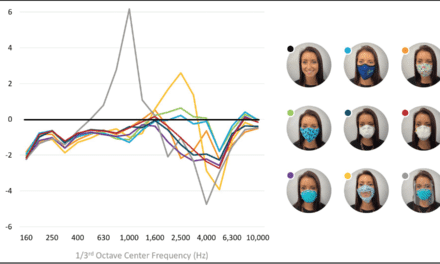
Reduced sound levels at high frequencies; amplification at low frequencies. Medical masks essentially serve as a low-pass filter, attenuating the high frequencies (2000-7000 Hz) spoken by the wearer, with the decibel level of attenuation ranging from 3-4 dB for a simple medical mask and close to 12 dB for the N95 masks.2 Cloth masks have also been found to attenuate higher frequencies by differing amounts (above 1000 Hz) depending on their composition and weave.3 While face shields also attenuate high frequencies, they amplify low frequencies so their overall effect on speech understanding is unclear, and research is ongoing.
Reduced discrimination of speech signal amongst competing noise. Reduced discrimination may occur in an environment with a high level of noise, such as a hospital. Those with hearing loss may suffer more from mask effects than those with normal hearing because of their increased difficulty understanding speech in noise in most situations.
Loss of visual-speech cues. Auditory-visual speech, where both auditory and visual-speech cues (ie, lip, tongue, and face movements) are available, enhances speech perception.4-6 Those with hearing impairment rely more heavily on visual-speech information than those with normal hearing.7,8 Visual-speech cues help to counteract hearing difficulty experienced,6 particularly in a noisy environment.4,7 Cloth and medical masks block access to visual-speech cues including facial expressions and lip-movements. The impact of mask wearing on communication is likely to differ among people with hearing impairment depending on individual speechreading ability and reliance on auditory-visual speech. Individuals with early-onset, severe-to-profound hearing impairments have been found to have enhanced speechreading ability9 and may therefore experience a negative impact. Clearly, individuals who are totally reliant on lip-reading to communicate will experience a negative impact.10 Further research is required to explore the impact of masks on speech perception for people with hearing impairment, investigating factors such as the onset of hearing loss, degree of loss, and the use of hearing aids/cochlear implants.
Small impact on speech production. Mask wearing has been found to have only a small impact on articulation and only minor effects on the airstream.11 Therefore, the ability to use the mouth to articulate appears to be not significantly hindered by the wearing of masks, although further research on this topic could be beneficial.
The combination of the above factors related to mask wearing, including the increased difficulty in understanding speech, room/noise reverberation, and the absence of visual cues can put people with hearing loss at a communication disadvantage in comparison to those with normal hearing.2,10
The various types of facial coverings have differing impacts on communication:
Typical masks (cloth and medical). Both cloth and medical masks perform better acoustically than transparent masks.3 A major drawback of cloth and medical masks is the visual barrier these masks present to those in the hearing-impaired community who depend on nonverbal communication cues on the face.12-14
Transparent face masks (with windows made of plastic). In comparison to opaque cloth masks, masks with plastic windows perform worse acoustically, reducing the high frequency sound cues that are crucial for speech more than opaque masks.3 Despite this, some studies have found that transparent masks improve speech understanding in noise by making the lips and mouth visually accessible.1 The issue of fogging of the clear plastic window (due to exhaled breath) is also a problem that manufacturers of these masks are currently attempting to overcome.
Face shields. It should be noted that a clear face shield is not considered to provide the same level of protection from infection as a face mask.15 In line with transparent face masks, face shields offer the benefit of visual input.3 Further research into the acoustic impact of face shields is needed; however NAL preliminary findings do not indicate a negative impact on speech intelligibility.16
The use of lapel microphones has been recommended to overcome some of the difficulties encountered with the use of masks. Masks tend to attenuate high-frequency sound in front of the talker, whereas microphones placed above and below the mask are less affected. To preserve visual cues without destroying high-frequency sound cues, the use of clear window masks in combination with lapel microphones has been recommended.3
For hearing aid wearers, NAL has provided a face mask program that increases gain to compensate for the reduced speech levels of a talker wearing a mask. This program can be accessed at NAL’s website at: https://www.nal.gov.au/nal-mask-adjust/.

Correspondence can be addressed to Louise Martin at: [email protected].
Citation for this article: Martin L. NAL update: Impact of face masks and face shields on communication. Hearing Review. 2020;27(10):28-29.
References
- Atcherson SR, Mendel LL, Baltimore WJ. The effect of conventional and transparent surgical masks on speech understanding in individuals with and without hearing loss. J Am Acad Audiol. 2017;28(1):58-67.
- Goldin A, Weinstein B, Shiman N. How do medical masks degrade speech reception? Hearing Review. 2020;27(5):8-9.
- Corey RM, Jones U, Singer AC. Acoustic effects of medical, cloth, and transparent face masks on speech signals. Champaign, IL: UUniversity of Illinois at Urbana-Champaign; August 11, 2020.
- Bernstein JGW, Grant KW. Auditory and auditory-visual intelligibility of speech in fluctuating maskers for normal-hearing and hearing-impaired listeners. J Acoust Soc Am. 2009;125(5):3358.
- Fraser S, Gagné J-P, Alepins M, Dubois P. Evaluating the effort expended to understand speech in noise using a dual-task paradigm: The effects of providing visual speech cues. J Sp Lang Hear Res. 2010;53(1):18-33.
- Frtusova JB, Phillips NA. The auditory-visual speech benefit on working memory in older adults with hearing impairment. Frontiers in Psychol. 2016;7:490.
- Tye-Murray N, Sommers MS, Spehar B. Audiovisual integration and lipreading abilities of older adults with normal and impaired hearing. Ear Hear. 2007;28(5):656-668.
- Fernandez-Lopez A, Martinez O, Sukno FM. Towards estimating the upper bound of visual-speech recognition: The visual lip-reading feasibility database. 2017 12th IEEE International Conference on Automatic Face & Gesture Recognition (FG 2017).May 2017;208-215. Washington, DC.
- Auer ET, Bernstein LE. Enhanced visual speech perception in individuals with early-onset hearing impairment. J Sp Lang Hear Res. 2007;50(5):1157-1165.
- Chodosh J, Weinstein BE, Blustein J. Face masks can be devastating for people with hearing loss. Brit Med Jour. 2020;370:m2683.
- Fecher N, Watt D. Effects of forensically-realistic facial concealment on auditory-visual consonant recognition in quiet and noise conditions. Auditory-Visual Speech Processing (AVSP) 2013. September 2013;81-86. Annecy, France.
- Mendel LL, Gardino JA, Atcherson SR. Speech understanding using surgical masks: A problem in health care? J Am Acad Audiol. 2008;19:686-695.
- Atcherson SR, Finley ET, McDowell BR, Watson C. More speech degradations and considerations in the search for transparent face coverings during the COVID-19 pandemic. Audiology Today.2020.
- Baltimore WJ, Atcherson SR. Helping our clients parse speech through masks during COVID-19. ASHA LeaderLive. https://leader.pubs.asha.org/do/10.1044/leader.MIW.25062020.34/full/. Published June 1, 2020.
- US Centers for Disease Control and Prevention (CDC). Coronavirus Disease 2019 (COVID-19): Considerations for Wearing Masks.. https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/cloth-face-cover-guidance.html#feasibility-adaptations. Published August 7, 2020.
- Mejia J, Galloway J, Cooper J, Monaghan J, Edwards B. On managing the impact of face covers on speech understanding in noise using hearing aids. In press.
Other Resources
Bourguignon M, Baart M, Kapnoula EC, Molinaro N. Lip-reading enables the brain to synthesize auditory features of unknown silent speech. J Neuroscience. 2020;40(5):1053-1065.
Carron C. Soon a transparent surgical mask to keep smiling. Swiss Federal Institute of Technology Lausanne (EPFL) website. https://actu.epfl.ch/news/soon-a-transparent-surgical-mask-to-keep-smiling/. Published September 6, 2020.
Davidson A, Marrone N. A clinically valuable interaction in the midst of COVID-19 and beyond: A viewpoint on the importance of patient-centered outcomes in rehabilitative audiology. Perspectives of the ASHA Special Interest Groups. 2020;5(4):940-945.
Fuller G, Howell M. Can you hear me now? Communicating across the COVID-19 PPE chasm. Texas Medical Association website. https://www.texmed.org/Template.aspx?id=54301. Published August 20, 2020.
Hampton T, Crunkhorn R, Lowe N, et al. The negative impact of wearing personal protective equipment on communication during coronavirus disease 2019. J Laryngol Otol. 2020;134(7):577-581.
Atcherson SR, Mendel LL, Baltimore WJ, et al. The effect of conventional and transparent surgical masks on speech understanding in individuals with and without hearing loss. J Am Acad Audiol. 2017;28(1):58-67.
McKee M, Moran C, Zazove P. Overcoming additional barriers to care for deaf and hard of hearing patients during Covid-19. JAMA Otolaryngol-Head Neck Surg. 2020;146(9):781-782.
Miller CW, Stewart EK, Wu Y-H, Bishop C, Bentler RA, Tremblay K. Working memory and speech recognition in noise under ecologically relevant listening conditions: Effects of visual cues and noise type among adults with hearing loss. J Sp Lang Hear Res. 2017;60(8):2310-2320.
Park J. Unraveling the invisible but harmful impact of Covid-19 on deaf older adults and older adults with hearing loss. J Gerontolog Social Work. 2020. DOI: https://doi.org/10.1080/01634372.2020.1799282.
Rosemann S, Thiel CM. Audio-visual speech processing in age-related hearing loss: Stronger integration and increased frontal lobe recruitment. NeuroImage. 2018;175:425-437.
Sriwijitalai W, Wiwanitkit V. Hearing loss and COVID-19: A note. Am J Otolaryngol. 2020;41(3):102473.
Trecca EMC, Gelardi M, Cassano M. COVID-19 and hearing difficulties. Am J Otolaryngol. 2020;41(4):102496.
West JS, Franck KH, Welling DB. Providing health care to patients with hearing loss during Covid-19 and physical distancing. Laryngoscope Investigative Otolaryngol. 2020;5(3):396-398.
Wittum KJ, Feth L, Hoglund E. The effects of surgical masks on speech perception in noise. Proceedings of Meetings on Acoustics. 2013;19(1):060125.
World Health Organization (WHO). Advice on the use of masks in the context of COVID-19: Interim guidance. https://apps.who.int/iris/bitstream/handle/10665/332293/WHO-2019-nCov-IPC_Masks-2020.4-eng.pdf. Published June 5, 2020.