Newborn hearing screening has grown in the United States over the past decade from about a dozen hospitals providing universal newborn hearing screening (UNHS) programs in 1993 to nearly 95% of newborn infants being screened by March 2004.1 There are approximately 4 million births per year in the United States.2 While the actual percentage of infants with permanent hearing loss is about 0.3% (about 12,000 infants per year),3 the actual number of infants referred for post-screening follow-up (ie, “refer rate”) is much higher.
This is due to false-positives: infants who screen positive for hearing loss but are eventually found to have normal hearing. False positive rates range from 2%-10%, varying from state to state and hospital to hospital.4 Using a conservative figure of 2.1% (2002 statistics, conversation with M. Gafney, Center for Disease Control, April 27, 2004) yields approximately 80,000 infants per year that are in need of post-screening diagnostic follow-up.
The growth in post-screening diagnosis has given rise to an increased demand for objective hearing assessment instrumentation. Prominent among the battery of tests a clinician uses when performing objective post-screening hearing assessment are electro-physiological tests, including otoacoustic emissions (OAEs), auditory evoked potentials (AEPs), and impedance audiometry.
The most widely used types of electro-physiological tests are distortion product OAE (DPOAE), auditory brainstem response (ABR), and more recently auditory steady state response (ASSR) tests. However, while the instrumentation is widely used, no published data are available that the author is aware of quantifying clinicians’ satisfaction (or lack thereof) with the performance of the current range of equipment and technologies.
In this light, a study was conducted in Summer 2004 to identify and quantify issues regarding electro-physiological post-screening hearing assessment in infants, in particular ABR and ASSR.
Study Methods
Respondents. Potential respondents were chosen at random from databases and lists that identify those audiologists specializing in infant diagnosis. Responses were obtained from 60 clinical audiologists from across the United States who provided diagnostic electro-physiological services to infants referred from newborn hearing screening programs. Respondents covered the major population centers in the United States, and all major types of facilities: ENT/Physician offices, private practices, hospitals, universities, and clinics. The number of respondents per geographic region corresponded well to the region’s population, with the exception of Florida, which, although one of the more populous states, only had one respondent.
Survey design. The survey consisted of multiple-choice and open-ended questions covering various aspects of electro-physiological testing. Particularly, the survey asked respondents to indicate what frustrations they may currently be experiencing (if any) with their AEP systems, and to assign a level to each frustration, from 1 to 10, with 1 representing very little, and 10 a very high level of frustration. Other questions asked if their AEP testing requires a shielded and/or sound-proof room; whether they would move to other environments if electromagnetic field noise was not an issue; and whether they see ASSR as replacing or complementing ABR.
Respondents were also presented with a list of instrument features, and asked to suggest any additional features they viewed as being helpful, and then rate them on a 3-point scale: 1) Not important: do not consider this feature when selecting an instrument; 2) Desirable: consider this feature when selecting an instrument, but would consider selecting one without it; and 3) Mandatory: would not consider selecting equipment without this feature. Particularly, as wireless communications are penetrating medical devices, the respondents were asked whether relaying the test data to a computer via a wireless connection in an AEP instrument would be valuable.
Findings
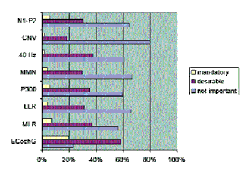
Frustrations and unmet needs. Results concerning frustrations and unmet needs of AEP equipment are shown in Figures 1-2. They show:
0 • A majority (84%) of respondents cited noise as a frustration in AEP testing (Figure 1). Physiologic noise was indicated as the biggest problem in ABR testing, with 75% of respondents citing it as an issue with an average frustration level of 6. Electromagnetic field noise followed physiologic noise, with 52% of respondents citing it as an issue with an average frustration level of 6.

Figure 1. Frustrations with current ABR/ASSR systems. |
• Cumbersome wires and cables were cited by 50% of respondents with an average frustration level of 5.
• Speed (too slow), was cited by 54% of respondents rating it at a frustration level of 6. Figure 2 provides the average reported test times for ABR and ASSR.
Figure 2. Time required for ABR and ASSR testing. |
Not surprisingly, the test times for performing both ABR and ASSR tests are relatively long (see article by Luts & Wouters5 on ABR and ASSR test times). However, test times for ASSR are reported to be longer than those for tone-burst ABR, while the former is typically considered to be faster than the latter.
The need for a shielded and/or sound-proof room. Of the respondents, 53% indicated that they currently test in a shield and/or in a soundproof room. Half (50%) indicated they would conduct testing in other environments if electro-magnetic field noise was not a problem (Figure 3).

Figure 3. The need for testing in electromagnetically shielded rooms. |
ASSR acceptance. About one-quarter (27%) of respondents already owned an ASSR device. The vast majority of audiologists saw ABR and ASSR as complementary rather than competitive methodologies. Only 19% of respondents felt that ASSR would replace ABR, either partially or completely. Of those indicating they have no plans to purchase an ASSR instrument, only 3% cited the lack of clinical data as a reason, while 45% cited budgetary constraints (Figure 4). This suggests that the industry has quickly embraced ASSR as a tool, and its limitations in providing certain data is not an impediment to its adoption, which is corraborated by Hall.6

Figure 4. Reasons for not having ASSR. |
Desired instrument features. The features that were sited as the most valuable are summarized in Figures 5-9. The most prominent desirable feature was the ability to function in electromagnetically and physiologically noisy environments which was indicated by 96% of respondents as either desirable or mandatory (Figure 5).
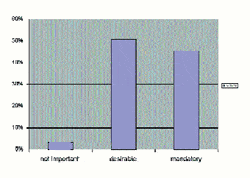
Figure 5. Ability to function in “noisy” environments (ie, electromagnetic and physiological). |
Among other AEP modalities, Electrocochleography (ECochG) was indicated as the most desirable or mandatory (Figure 6). Interestingly, most respondents (97%) indicated wireless communications, which is new to audiology and unavailable in current AEP systems, as a desirable or mandatory feature.
Discussion
According to the survey findings, the main issue facing diagnostic audiologists today in ABR/ASSR testing is physiological and electromagnetic noise, with 97% of respondents rating the need to test in “noisy” environments very high. These noises often restrict an clinician as to where AEP testing can be performed and increase the time it takes to obtain accurate readings. Indeed, half of those audiologists surveyed who currently conduct ABR/ASSR testing in a shielded room would no longer do so if electromagnetic noise was not an issue. Additionally, many do not always have the luxury of testing in shielded environments, as they often need to test in the operating room or NICU.
Over half of survey respondents felt that the wires and cables that connect the patient to the AEP instrument were cumbersome, while almost all respondents rated the advent of a wireless connection between the patient and the AEP instrument as important to very important. Most clinicians want the convenience of having OAE, ABR, and ASSR on a single unit (83%), but only EcochG is strongly desired among other AEP tests (77%).
Less than one-third of facilities reported owning an ASSR unit, with budgetary constraints (not the lack of clinical data) being the limiting factor. Most audiologists see ASSR as complementing, rather than replacing ABR. A majority (89%) felt that multi-frequency ASSR testing on both ears simultaneously was desirable.
Conclusions
While electro-physiological testing is a major part of infant post-screening assessment, and ASSR has become largely accepted as a clinical tool, the ABR/ASSR instrumentation that audiologists currently use still has areas that can be addressed. Physiologic and electromagnetic noise continues to be the largest concern, increasing the time required to obtain accurate readings. Wireless communication is also seen as a way of eliminating the nuisance of cables and providing greater mobility for both patients and audiologists.
Acknowledgement
The author conducted this survey as an independent consultant during Summer 2004, but now serves as product marketing manager for Vivosonic, Inc. He thanks all the clinicians who took part in the survey.
| This article was submitted to HR by Sidney Tannenbaum, MBA, product marketing manager for Vivosonic Inc, Toronto. Correspondence can be addressed to Sidney Tannenbaum, Vivosonic Inc, 620-56 Aberfoyle Cres, Toronto, ON, M8X 2W4, Canada; email: [email protected]. |
References
1. Foust T, White K. Medicaid and private insurance reimbursement for pediatric audiology services. Paper presented at: American Academy of Audiology annual convention; Salt Lake City; April 2004.
2. National Center for Hearing Assessment and Management. Available at: www.infanthearing.org/status/unhsstate.html; Logan, Utah: Utah State University; Accessed December 10, 2004.
3. National Center for Hearing Assessment and Management. Available at: www.infanthearing.org/resources/fact.pdf; Logan, Utah: Utah State University; Accessed December 10, 2004.
4. National Center for Hearing Assessment and Management. Sound Ideas. 2003;5(3). Available at: www.infanthearing.org /newsletter/v5n3/followup.html; Logan, Utah: Utah State University; Accessed December 10, 2004.
5. Luts X, Wouters Y. Comparison of Master and Audera for measurement of auditory steady state responses. Intl J Audiol. In press.
6. Hall, JW III. ABRs or ASSRs? The application of tone-burst ABRs in the era of ASSRs. Hearing Review. 2004;11(9):22-30,60-62.